Psychosis is a symptom complex that may include hallucinations, delusions, disorders of thought, and disorganized speech or behavior. Acute psychosis is primary if it is symptomatic of a psychiatric disorder, or secondary if caused by a specific medical condition. Patients with primary psychiatric disorders are likely to have auditory hallucinations, prominent cognitive disorders, and complicated delusions. If psychosis is caused by a medical condition, the patient may exhibit cognitive changes and abnormal vital signs, and may have visual hallucinations. Illicit drug use is the most common medical cause of acute psychosis. Clinicians should ask about recent head injury or trauma, seizures, cerebrovascular disease, or new or worsening headaches. A subacute onset of psychosis should raise suspicion for an oncologic cause. Collateral history from family members is helpful in establishing the presentation and course of the illness. The physical examination should include complete neurologic and mental status assessments. Tachycardia or severe hypertension may indicate drug toxicity or thyrotoxicosis; fever may suggest encephalitis or porphyria. Suggested initial laboratory tests include a complete blood count, metabolic profile, thyroid function tests, urine toxicology, and measurement of parathyroid hormone, calcium, vitamin B12, folate, and niacin. Testing for human immunodeficiency virus infection and syphilis should also be considered. Prompt recognition of the etiology of psychosis may improve treatment, consultation, and prognosis.
Psychosis is a symptom complex that may include hallucinations, delusions, disorders of thought, and disorganized speech or behavior. Primary care is often the point of first contact for patients exhibiting psychotic symptoms, and family physicians must be alert to the distinguishing features that point to a psychiatric or medical etiology.1–3
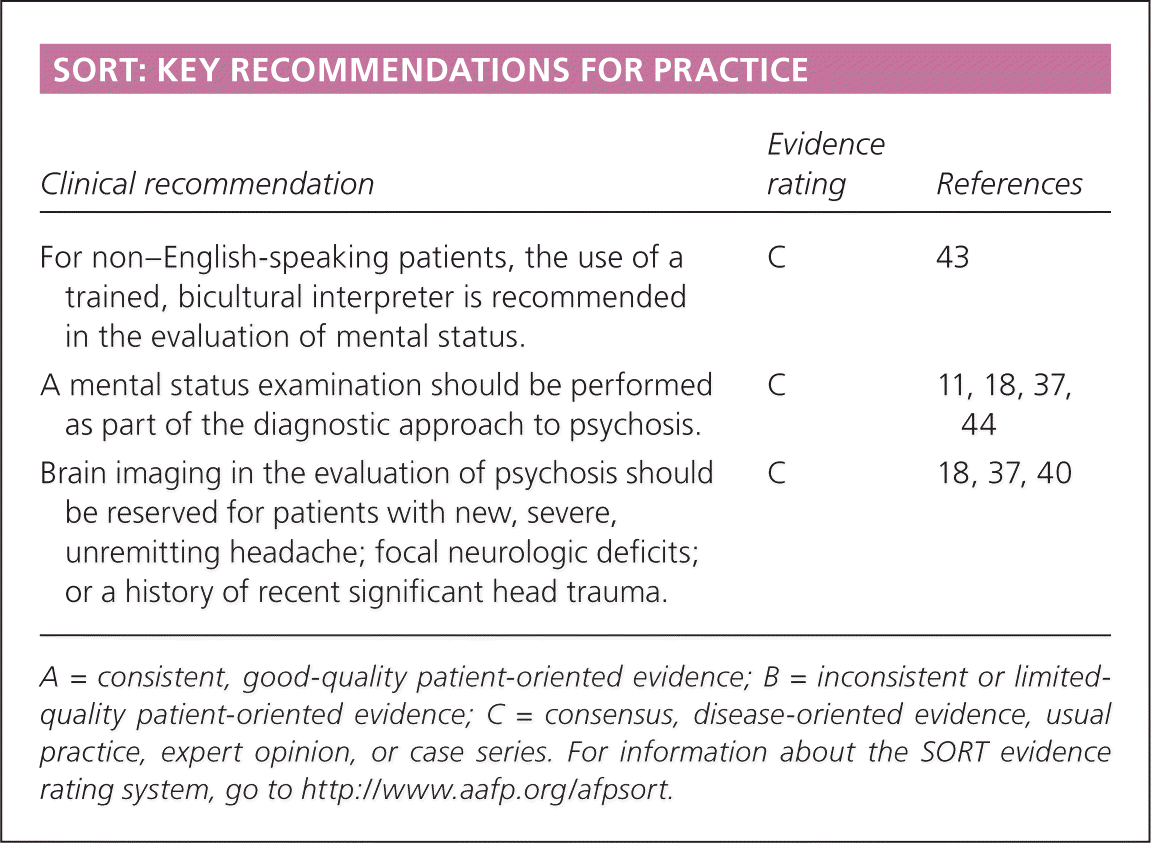
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| For non–English-speaking patients, the use of a trained, bicultural interpreter is recommended in the evaluation of mental status. | C | 43 |
| A mental status examination should be performed as part of the diagnostic approach to psychosis. | C | 11, 18, 37, 44 |
| Brain imaging in the evaluation of psychosis should be reserved for patients with new, severe, unremitting headache; focal neurologic deficits; or a history of recent significant head trauma. | C | 18, 37, 40 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN PSYCHIATRY: RECOMMENDATIONS FROM THE CHOOSING WISELY CAMPAIGN

| Recommendation | Sponsoring organization |
|---|---|
| Do not prescribe antipsychotics to patients for any indication without appropriate initial evaluation and appropriate ongoing monitoring. | American Psychiatric Association |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Epidemiology
In the general population, there is an approximate 3% lifetime prevalence of psychotic disorders, with 0.21% accounting for psychosis due to a general medical condition.4 A recent review found a prevalence of 0.5% to 4.3% for bipolar disorder in primary care populations, and approximately 9% for bipolar spectrum illnesses.5 In one urban primary care population, the prevalence of psychotic symptoms was most commonly associated with depressive, anxiety, and panic disorders (42.4%, 38.6%, and 24.8%, respectively), followed by substance use disorders (13.8%).6
Childhood-onset schizophrenia (12 years or younger) is uncommon, with a prevalence of 0.2 to 0.4 per 10,000.7 However, children may exhibit psychotic symptoms secondary to medication adverse effects, drug toxicity or poisons, metabolic defects, autoimmune disorders, or other psychiatric disorders.8 In a 10-year cohort study, adolescent use of marijuana increased the occurrence of incident psychosis and, with ongoing use, the risk of persistent psychotic episodes.9
The prevalence of depression in pregnancy has been estimated to be 13.6% at 32 weeks' gestation to 17% at approximately 36 weeks' gestation.10 Postpartum psychosis occurs after one in 500 to 1,000 births; risk factors include a history of premorbid depression or bipolar disorder, prior peripartum mood disorder, or a previous episode of postpartum psychosis.11,12
Etiology
The role of dopamine in the pathophysiology of psychosis is supported by the effectiveness of dopamine receptor antagonists in treating symptoms, and from evidence that psychosis-producing drugs such as methamphetamine, cocaine, and levodopa enhance dopamine secretion. Hypofunction of the N-methyl-d-aspartate glutamate receptor may cause schizophrenia.13,14 Psychotic presentations associated with autoimmune disorders raise the possibility of shared genetic features or common exposures to etiologic factors, such as infections.15
Differential Diagnosis
Acute psychosis is primary if it is symptomatic of a psychiatric disorder, or secondary if caused by a specific medical condition. A key diagnostic distinction must be made between psychotic symptoms caused by delirium, a psychiatric disorder, or a defined medical condition (Table 1).11,16 For example, if substance use or withdrawal is suspected, it may be difficult to differentiate delirium from psychosis.17 Delirium, an often reversible or temporary state of confusion with a rapid onset from altered brain function, is most often diagnosed in older or hospitalized populations, but it must be ruled out before reaching a definitive diagnosis of psychosis.11 Patients with existing cognitive deficits may present with mixed delirium and psychosis. In these cases, it is helpful to ask about the temporal course of their symptoms, signs of systemic illness, or recent environmental change, and to obtain collateral information from caregivers. These patients may be taking multiple medications with psychoactive effects.
Table 1. Selected Medical and Psychiatric Causes of Psychosis

| Medical causes | |
| Delirium (acute, transient disturbance in mental function) | |
| Hypo- or hyperglycemia | |
| Hypoxia | |
| “ICU psychosis” | |
| Medication interactions or withdrawal | |
| Sepsis | |
| Serum electrolyte or metabolic abnormalities | |
| Sleep deprivation | |
| Other medical causes (chronic disturbance in mental function) | |
| Autoimmune disorders (e.g., multiple sclerosis, systemic lupus erythematosus) | |
| Endocrine disorders (e.g., Cushing disease, diabetes mellitus, thyroid disease) | |
| Genetic, heritable conditions | |
| Neurologic conditions (e.g., dementia, encephalitis, epilepsy, Parkinson disease) | |
| Nutritional conditions (e.g., vitamin B deficiency) | |
| Oncologic conditions (e.g., ovarian teratoma, small cell lung cancer) | |
| Pharmacologic causes (e.g., medication adverse effect, substance abuse or withdrawal) | |
| Psychiatric causes11,16 | |
| Bipolar I disorder | |
| Depression with psychotic features | |
| Psychotic disorder (brief), with or without marked stressors* | |
| Schizoaffective disorder | |
| Schizophrenia | |
ICU = intensive care unit.
*—Classified as peripartum, if during pregnancy or within four weeks of delivery.
Patients with primary psychiatric disorders are more likely to have auditory hallucinations, prominent cognitive disorders, and complicated delusions.18 Schizophrenia, bipolar disorder, major depression, schizoaffective disorder, and brief psychotic disorder are the most common psychiatric illnesses that present in primary care with psychotic features. Level of consciousness and awareness are usually—but not always—intact. Overall appearance may be normal, or disheveled and unkempt. According to the Diagnostic and Statistical Manual of Mental Disorders, 5th ed. (DSM-5), diagnostic criteria for schizophrenia include symptoms persisting for at least six months and significant difficulty in one or more major functional capacities.11 However, during a prodromal phase in schizophrenia, patients may relate unusual perceptions or odd thoughts, and may report that sounds seem louder or colors more intense; the clinician should recognize that these symptoms may be early features of schizophrenia.16
In the manic phase of bipolar I disorder, the patient may present with at least a seven-day history of elevated or expansive mood, hallucinations or delusions, extreme goal-directed activity, and decreased need for sleep.11 In schizoaffective disorder, patients may have characteristics of both mania (bipolar type) and major mood disturbance (depressive type). With psychotic depression, a patient is likely to have decreased energy and delusions or hallucinations consistent with major depression, such as voices reinforcing the patient's feeling of guilt or worthlessness. Alternatively, patients with major depressive disorder may present with prominent symptoms of anxiety or even panic. Patients experiencing a brief psychotic episode display the cardinal symptoms of delusions, hallucinations, and disorganized speech, but for a shorter period of time and with eventual recovery. Postpartum psychosis is classified in DSM-5 as a brief psychotic disorder if it occurs during pregnancy or within four weeks after delivery. During a peripartum episode of psychosis, women have delusions, hallucinations, or disorganized speech, and may have hallucinations telling them to hurt or kill their baby.
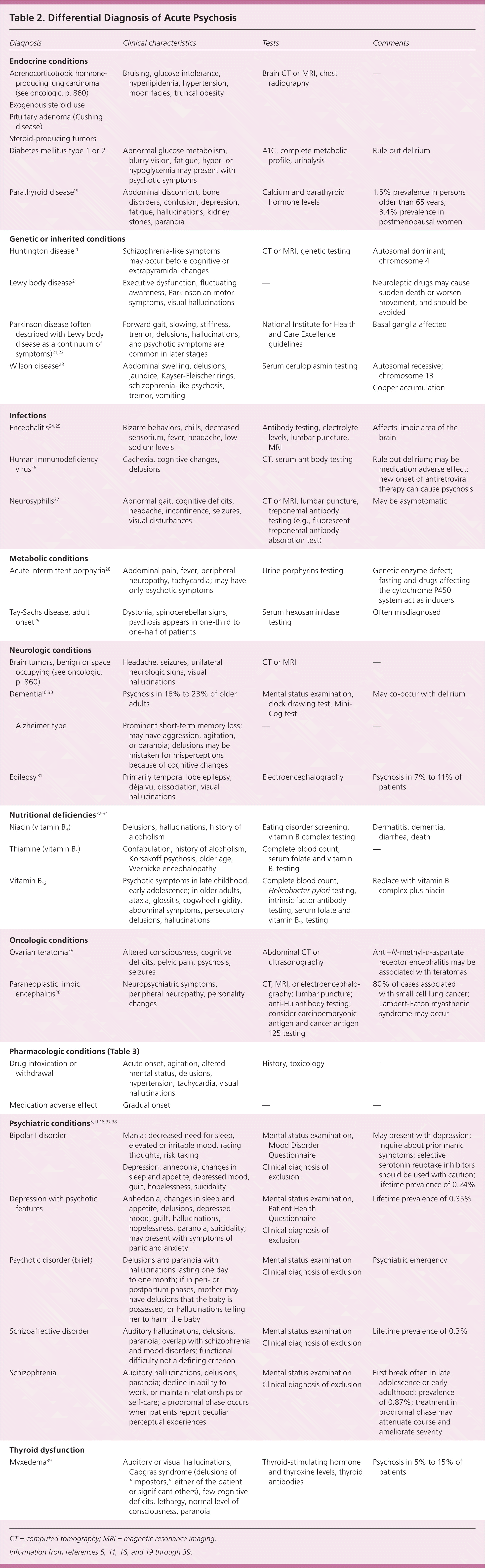
In secondary psychosis, there may be cognitive difficulties, abnormal vital signs, and visual hallucinations. Several medical conditions may initially present with psychosis; thus, a systematic approach to diagnosis is required to identify the cause (Table 2).5,11,16,19–39 Illicit drug use is the most common medical cause of acute psychosis.40
Table 2. Differential Diagnosis of Acute Psychosis
| Diagnosis | Clinical characteristics | Tests | Comments | |
|---|---|---|---|---|
| Endocrine conditions | ||||
| Adrenocorticotropic hormone-producing lung carcinoma (see oncologic, p. 860) | Bruising, glucose intolerance, hyperlipidemia, hypertension, moon facies, truncal obesity | Brain CT or MRI, chest radiography | — | |
| Exogenous steroid use | ||||
| Pituitary adenoma (Cushing disease) | ||||
| Steroid-producing tumors | ||||
| Diabetes mellitus type 1 or 2 | Abnormal glucose metabolism, blurry vision, fatigue; hyper- or hypoglycemia may present with psychotic symptoms | A1C, complete metabolic profile, urinalysis | Rule out delirium | |
| Parathyroid disease19 | Abdominal discomfort, bone disorders, confusion, depression, fatigue, hallucinations, kidney stones, paranoia | Calcium and parathyroid hormone levels | 1.5% prevalence in persons older than 65 years; 3.4% prevalence in postmenopausal women | |
| Genetic or inherited conditions | ||||
| Huntington disease20 | Schizophrenia-like symptoms may occur before cognitive or extrapyramidal changes | CT or MRI, genetic testing | Autosomal dominant; chromosome 4 | |
| Lewy body disease21 | Executive dysfunction, fluctuating awareness, Parkinsonian motor symptoms, visual hallucinations | — | Neuroleptic drugs may cause sudden death or worsen movement, and should be avoided | |
| Parkinson disease (often described with Lewy body disease as a continuum of symptoms)21,22 | Forward gait, slowing, stiffness, tremor; delusions, hallucinations, and psychotic symptoms are common in later stages | National Institute for Health and Care Excellence guidelines | Basal ganglia affected | |
| Wilson disease23 | Abdominal swelling, delusions, jaundice, Kayser-Fleischer rings, schizophrenia-like psychosis, tremor, vomiting | Serum ceruloplasmin testing | Autosomal recessive; chromosome 13 | |
| Copper accumulation | ||||
| Infections | ||||
| Encephalitis24,25 | Bizarre behaviors, chills, decreased sensorium, fever, headache, low sodium levels | Antibody testing, electrolyte levels, lumbar puncture, MRI | Affects limbic area of the brain | |
| Human immunodeficiency virus26 | Cachexia, cognitive changes, delusions | CT, serum antibody testing | Rule out delirium; may be medication adverse effect; new onset of antiretroviral therapy can cause psychosis | |
| Neurosyphilis27 | Abnormal gait, cognitive deficits, headache, incontinence, seizures, visual disturbances | CT or MRI, lumbar puncture, treponemal antibody testing (e.g., fluorescent treponemal antibody absorption test) | May be asymptomatic | |
| Metabolic conditions | ||||
| Acute intermittent porphyria28 | Abdominal pain, fever, peripheral neuropathy, tachycardia; may have only psychotic symptoms | Urine porphyrins testing | Genetic enzyme defect; fasting and drugs affecting the cytochrome P450 system act as inducers | |
| Tay-Sachs disease, adult onset29 | Dystonia, spinocerebellar signs; psychosis appears in one-third to one-half of patients | Serum hexosaminidase testing | Often misdiagnosed | |
| Neurologic conditions | ||||
| Brain tumors, benign or space occupying (see oncologic, p. 860) | Headache, seizures, unilateral neurologic signs, visual hallucinations | CT or MRI | — | |
| Dementia16,30 | Psychosis in 16% to 23% of older adults | Mental status examination, clock drawing test, Mini-Cog test | May co-occur with delirium | |
| Alzheimer type | Prominent short-term memory loss; may have aggression, agitation, or paranoia; delusions may be mistaken for misperceptions because of cognitive changes | — | — | |
| Epilepsy 31 | Primarily temporal lobe epilepsy; déjà vu, dissociation, visual hallucinations | Electroencephalography | Psychosis in 7% to 11% of patients | |
| Nutritional deficiencies32–34 | ||||
| Niacin (vitamin B3) | Delusions, hallucinations, history of alcoholism | Eating disorder screening, vitamin B complex testing | Dermatitis, dementia, diarrhea, death | |
| Thiamine (vitamin B1) | Confabulation, history of alcoholism, Korsakoff psychosis, older age, Wernicke encephalopathy | Complete blood count, serum folate and vitamin B1 testing | — | |
| Vitamin B12 | Psychotic symptoms in late childhood, early adolescence; in older adults, ataxia, glossitis, cogwheel rigidity, abdominal symptoms, persecutory delusions, hallucinations | Complete blood count, Helicobacter pylori testing, intrinsic factor antibody testing, serum folate and vitamin B12 testing | Replace with vitamin B complex plus niacin | |
| Oncologic conditions | ||||
| Ovarian teratoma35 | Altered consciousness, cognitive deficits, pelvic pain, psychosis, seizures | Abdominal CT or ultrasonography | Anti–N-methyl- | |
| Paraneoplastic limbic encephalitis36 | Neuropsychiatric symptoms, peripheral neuropathy, personality changes | CT, MRI, or electroencephalography; lumbar puncture; anti-Hu antibody testing; consider carcinoembryonic antigen and cancer antigen 125 testing | 80% of cases associated with small cell lung cancer; Lambert-Eaton myasthenic syndrome may occur | |
| Pharmacologic conditions (Table 3) | ||||
| Drug intoxication or withdrawal | Acute onset, agitation, altered mental status, delusions, hypertension, tachycardia, visual hallucinations | History, toxicology | — | |
| Medication adverse effect | Gradual onset | — | — | |
| Psychiatric conditions5,11,16,37,38 | ||||
| Bipolar I disorder | Mania: decreased need for sleep, elevated or irritable mood, racing thoughts, risk taking | Mental status examination, Mood Disorder Questionnaire | May present with depression; inquire about prior manic symptoms; selective serotonin reuptake inhibitors should be used with caution; lifetime prevalence of 0.24% | |
| Depression: anhedonia, changes in sleep and appetite, depressed mood, guilt, hopelessness, suicidality | Clinical diagnosis of exclusion | |||
| Depression with psychotic features | Anhedonia, changes in sleep and appetite, delusions, depressed mood, guilt, hallucinations, hopelessness, paranoia, suicidality; may present with symptoms of panic and anxiety | Mental status examination, Patient Health Questionnaire | Lifetime prevalence of 0.35% | |
| Clinical diagnosis of exclusion | ||||
| Psychotic disorder (brief) | Delusions and paranoia with hallucinations lasting one day to one month; if in peri- or postpartum phases, mother may have delusions that the baby is possessed, or hallucinations telling her to harm the baby | Mental status examination | Psychiatric emergency | |
| Clinical diagnosis of exclusion | ||||
| Schizoaffective disorder | Auditory hallucinations, delusions, paranoia; overlap with schizophrenia and mood disorders; functional difficulty not a defining criterion | Mental status examination | Lifetime prevalence of 0.3% | |
| Clinical diagnosis of exclusion | ||||
| Schizophrenia | Auditory hallucinations, delusions, paranoia; decline in ability to work, or maintain relationships or self-care; a prodromal phase occurs when patients report peculiar perceptual experiences | Mental status examination | First break often in late adolescence or early adulthood; prevalence of 0.87%; treatment in prodromal phase may attenuate course and ameliorate severity | |
| Clinical diagnosis of exclusion | ||||
| Thyroid dysfunction | ||||
| Myxedema39 | Auditory or visual hallucinations, Capgras syndrome (delusions of “impostors,” either of the patient or significant others), few cognitive deficits, lethargy, normal level of consciousness, paranoia | Thyroid-stimulating hormone and thyroxine levels, thyroid antibodies | Psychosis in 5% to 15% of patients | |
CT = computed tomography; MRI = magnetic resonance imaging.
Medical conditions associated with psychosis include autoimmune, endocrine, neurologic, and nutritional disorders.37 Suspected endocrine conditions include thyroid and parathyroid dysfunction. Hallmark neurologic conditions include temporal lobe epilepsy, Parkinson disease, and Lewy body disease. A subacute onset of psychosis should raise suspicion for an oncologic cause, such as a steroid-producing tumor, space-occupying brain lesion, or paraneoplastic etiology. Genetic or heritable diseases should be considered; for example, Huntington disease may first present with a psychotic episode.20
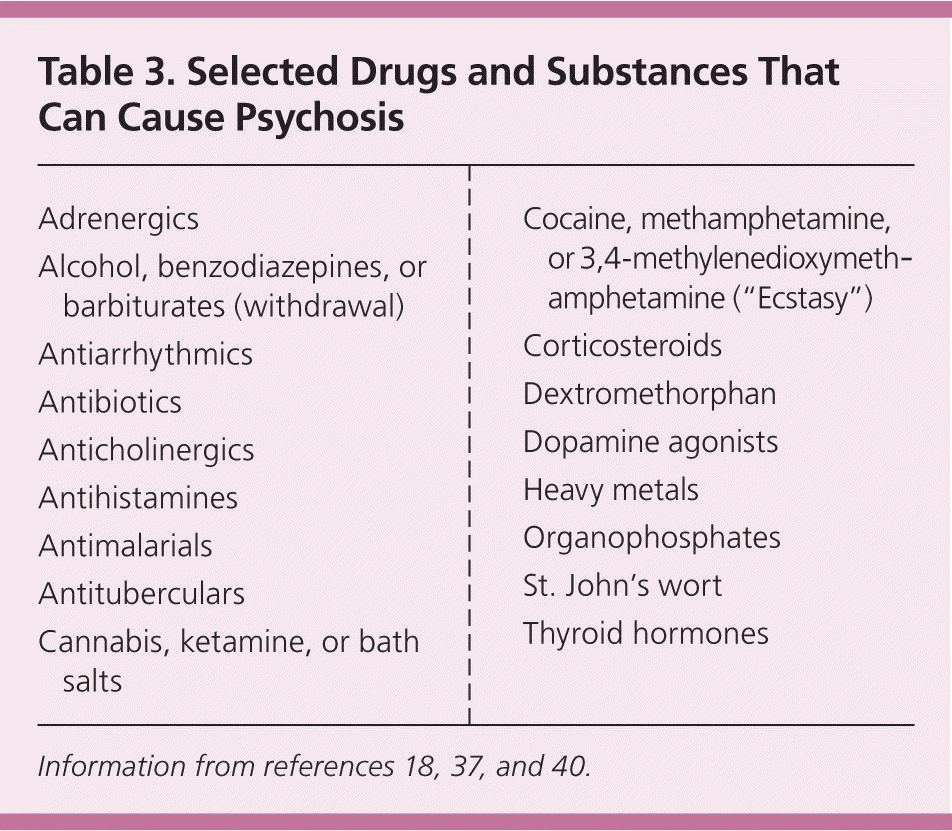
Information on medication interactions and use of herbal, over-the-counter, and recreational drugs should be elicited, because drug toxicity is a common cause of acute psychotic reactions18,37 (Table 318,37,40 ).
Table 3. Selected Drugs and Substances That Can Cause Psychosis
| Adrenergics | |
| Alcohol, benzodiazepines, or barbiturates (withdrawal) | |
| Antiarrhythmics | |
| Antibiotics | |
| Anticholinergics | |
| Antihistamines | |
| Antimalarials | |
| Antituberculars | |
| Cannabis, ketamine, or bath salts | |
| Cocaine, methamphetamine, or 3,4-methylenedioxymeth-amphetamine (“Ecstasy”) | |
| Corticosteroids | |
| Dextromethorphan | |
| Dopamine agonists | |
| Heavy metals | |
| Organophosphates | |
| St. John's wort | |
| Thyroid hormones | |
Diagnostic Strategy
HISTORY
Obtaining a history from a patient with psychotic symptoms may be challenging.41 Although the differential diagnosis of primary and secondary psychoses is broad, sensitive inquiry about the patient's recent illness can help to focus diagnostic thinking.38 Clinicians should ask about recent head injury or trauma to rule out subdural hematoma and obtain other relevant neurologic history, such as seizures, cerebrovascular disease, or new or worsening headaches.42
Recognition of psychosis by the primary care physician is facilitated by prior knowledge of a patient's family, medical, and cultural history. Individual cultures reflect a set of beliefs, values, and practices shared by members of a particular group. Delusional thinking and hallucinations should be considered within the patient's specific cultural context. What may appear delusional in one culture may be normal in another. Hallucinations relating to religious expressions may be accepted in certain groups.11 If the patient is not proficient in English, a bicultural interpreter is essential to assess whether the patient's thought processes and use of language are culturally consistent.43
The temporal relationship and course of psychotic symptoms, as well as the patient's age, background, and general medical condition, may provide diagnostic clues.16 For example, a first major break in schizophrenia usually occurs in late adolescence or early adulthood, although earlier signs may have been present for years. An onset of psychosis may occur acutely after recreational drug use or as a later presentation in multiple sclerosis. Whenever possible, collateral information should be collected from family members.
The social history should include recent stressors or significant changes in the patient's life, such as job loss, death of a significant other, educational stress, or other traumatic event. Family history may provide clues to suggest a psychiatric diagnosis or heritable condition. Travel history may suggest exposure to infection, such as malaria. A history of multiple sex partners may suggest human immunodeficiency virus infection or syphilis. A dietary history is important to identify potential nutritional deficits, which are common in frail older persons. Niacin deficiency can be a consequence of severe eating disorders. Occupational or environmental exposures should be noted.
PHYSICAL EXAMINATION
The physical examination should include a complete medical and mental status examination. Tachycardia or severe hypertension may indicate drug toxicity or thyrotoxicosis; fever may suggest encephalitis or porphyria.18 Physical signs suggestive of underlying diagnoses include cushingoid appearance in certain endocrinopathies, arthritic deformities in autoimmune disorders, or movement and gait disturbances in conditions such as multiple sclerosis and Parkinson disease.37 The neurologic examination should assess for focal signs, sensory deficits, myoclonus, or tremors. Tendon reflexes, cranial nerve testing, and ophthalmologic examination are important if a brain lesion, infection, or metabolic disease is suspected.
The mental status examination was reviewed in a previous article in American Family Physician.44 It combines elements of the history, direct observation, and assessment of the patient's general behavior, mood, affect, speech, and thought processes—particularly hallucinations.11 For example, frequency and features of auditory hallucinations may clarify their diagnostic significance. The patient's insight and judgment should be assessed; does the patient think he or she is ill? Has the patient noticed changes in thinking? If yes, what changes? Direct inquiry about suicidal or homicidal thoughts and plans is essential to determine whether immediate referral or hospitalization is indicated.
LABORATORY TESTING
When diagnostic signs and symptoms suggest a medical condition, targeted laboratory tests can be obtained.18,37 Suggested initial tests include a complete blood count to assess for anemia, elevated white blood cell count, or increased eosinophils; a metabolic profile to evaluate renal and hepatic function and electrolyte and glucose levels; thyroid function tests; urine toxicology testing; and measurement of parathyroid hormone, calcium, vitamin B12, folate, and niacin. Testing for human immunodeficiency virus infection and syphilis should also be considered. If there is concern for an autoimmune cause, antinuclear antibody testing and determination of the erythrocyte sedimentation rate can be useful. Rare conditions, such as acute intermittent porphyria or adult Tay-Sachs disease, may be identified by urine testing for porphyrins, or serum testing for hexosaminidase A.
Emergency brain imaging is usually not required unless the patient presents with new, severe, unremitting headache; focal neurologic deficits; or a history of recent significant head trauma.18,37,40,42
Subsequent Management
Psychotic symptoms are debilitating and can be terrifying to patients and their families. Prompt recognition of the etiology may improve treatment, consultation, and prognosis. The patient and family members can be given therapeutic support in the office, and provided with appropriate educational literature.
If the patient expresses suicidal ideation or intent, or manifests symptoms of mania, immediate referral to emergency care is warranted.
If the psychosis is secondary, the family physician has an opportunity to deliver timely intervention and management for acute causes, and to ameliorate symptoms by providing long-term patient- and family-centered support for more chronic conditions.
Any patient with a primary diagnosis of a psychotic disorder will benefit from close collaboration between behavioral health specialists and the primary care physician.3,45,46 The early use of antipsychotics, particularly clozapine (Clozaril), can decrease the risk of suicide in patients with schizophrenia, which may be as high as 15%, particularly in the initial phase of the illness.41,46,47 Other treatments for schizophrenia were reviewed in a previous article in American Family Physician.48
Despite optimal treatment, patients with schizophrenia and other psychotic disorders often have deficits in social functioning, are unable to maintain employment, and lack appropriate housing. The stigma of mental illness and poor mental health literacy compounds the challenges that patients face.49 Patients may lack insight into medical comorbidities and complex drug regimens, and the course of illness may be complicated by tobacco or other substance use.50 New and developing models are providing promising approaches toward integrated, patient-centered care for individuals with primary psychotic disorders.51,52
Data Sources: PubMed, Agency for Healthcare Research and Quality reports, Essential Evidence Plus, the Cochrane database, and the National Guideline Clearinghouse were searched using the terms psychosis, primary care presentations, psychosis in children, postpartum psychosis, early psychosis, treatment of early psychosis, and specific medical conditions crossed with psychosis (e.g., multiple sclerosis, seizures, endocrine disorders, medications, substances). Search dates: February 2014 through July 2014.

