The Institute of Medicine, the Healthy People 2020 initiative, and the U.S. Surgeon General agree that oral health directly affects overall health.1–3 Fluoride is an important aspect of good oral care. It is inexpensive, easy to deliver, and effective. With 181 million Americans not visiting the dentist annually,4 family physicians have an essential role in oral health care.
Fluoride is used in three formats: systemic ingestion, personal topical application, and professional topical application. When used systemically, fluoride is incorporated into teeth to reduce enamel solubility and is also excreted in saliva, producing a topical effect. Topical fluoride application has the greatest impact, slowing demineralization (tooth breakdown), enhancing remineralization (tooth strengthening), and inhibiting bacterial metabolism.
Systemic Fluoride
The Centers for Disease Control and Prevention (CDC) has called water fluoridation one of 10 great public health achievements of the 20th century. The CDC estimates that for every dollar spent on fluoridation, $38 is saved in dental treatment costs.5 The U.S. Department of Health and Human Services has set the optimal fluoride concentration at 0.7 ppm.6 The Environmental Protection Agency has set the maximum safety level at 4 ppm.7 Water fluoridation status can be checked on the CDC website (http://nccd.cdc.gov/DOH_MWF/Default/Default.aspx) or by calling the local water company. States and counties have testing centers for well water.
It is important to ask patients about their sources of drinking and cooking water. Physicians should ask about use of water filters; reverse osmosis filters (located on faucet taps) remove fluoride, whereas other water filters (e.g., Brita filters) do not. Additionally, the consumption of bottled water has increased to 29 gallons per person annually.8 Bottled-water drinkers have lower fluoride intake. The fluoride content of bottled water is not required on the label. Only about 5% of bottled water lists fluoride content on the label, and 80% contains suboptimal levels.9 Consuming even a small amount of fluoridated water daily is deemed beneficial (e.g., using fluoridated water only for cooking).
One issue with systemic fluoride is exposure in children younger than six months through formula consumption. Only 19% of mothers in the United States are exclusively breastfeeding by the time their infant is six months of age.10 Approximately 90% of parents who give their child formula use powdered formula, and about 75% mix it with tap water.11 The American Dental Association suggests that powdered formula can be reconstituted with fluoridated drinking water; however, it may lead to mild fluorosis.12 Strictly a cosmetic issue, fluorosis is the white mottling of permanent teeth from excessive exposure to fluoride during tooth development. Alternatives to fluoridated drinking water include ready-to-feed formula or reconstituting formula with fluoride-free water (e.g., purified, distilled, or reverse-osmosis water). A benefit to exclusive breastfeeding is less fluoride exposure during this period. Fluoride can be introduced at six months of age, as cereal and food are introduced.
The American Academy of Pediatrics, the American Academy of Family Physicians, and the U.S. Preventive Services Task Force (USPSTF) recommend fluoride supplementation for children six months or older who do not have optimally fluoridated drinking water.13–15 Fluoride supplementation should be prescribed only after determining the fluoride content of the child's local water supply. Dosing is based on the child's age and the concentration of fluoride in the water (Table 1).16 Fluoride supplementation should continue until 16 years of age.
Table 1. Dietary Fluoride Dosing According to Fluoride Content of Drinking Water

| Age | < 0.3 ppm | 0.3 to 0.6 ppm | > 0.6 ppm |
|---|---|---|---|
| 6 months to 3 years | 0.25 mg | None | None |
| 3 to 6 years | 0.5 mg | 0.25 mg | None |
| 6 to at least 16 years | 1.0 mg | 0.5 mg | None |
Adapted with permission from American Academy of Pediatric Dentistry. Guideline on fluoride therapy. http://www.aapd.org/media/Policies_Guidelines/G_fluoridetherapy.pdf. Accessed May 19, 2015.
Personal Application of Topical Fluoride
Everyone, regardless of age or risk factors, should brush their teeth twice daily with a fluoride-containing toothpaste. Appropriate amounts of toothpaste include a smear for children up to three years of age and a pea-sized amount for children three to six years of age.13,17 Parents or caregivers should brush children's teeth for them until seven to eight years of age.
Professional Application of Topical Fluoride
The USPSTF recommends that primary care physicians apply fluoride varnish to all children periodically (two to four times per year, depending on risk) for preventing and controlling dental caries from the time of primary tooth eruption through five years of age; this is associated with a 37% to 63% reduction in caries.15 The USPSTF targeted nondental primary care clinicians because they are more likely than dentists to have contact with children younger than six years. Fluoride varnish is easily applied, comes in many flavors, and is well tolerated by children, making it ideal for integration into medical practice. The varnish remains on the teeth for one to seven days before dissolving. During that time, it remineralizes enamel, repairs early defects and decay, and strengthens teeth. There are no absolute contraindications to varnish, and it does not cause fluorosis. Medicaid reimburses clinicians in 47 states and the District of Columbia for varnish application.18
Incorporating Fluoride into Medical Practice
Fluoride, like all medical interventions, has small risks, the most prevalent being fluorosis. However, most cases of fluorosis in the United States are considered mild. Because most fluoride ingestion is from toothpaste (80%),19 it is important to counsel patients about the correct amount of toothpaste for young children.
For physicians who want further training in fluoride varnish application and other pediatric or adult oral health issues, visit the AAFP-endorsed Smiles For Life website at http://www.smilesforlifeoralhealth.org. Additional resources for clinicians are provided in Table 2.
Table 2. Fluoride Resources for Clinicians and Patients
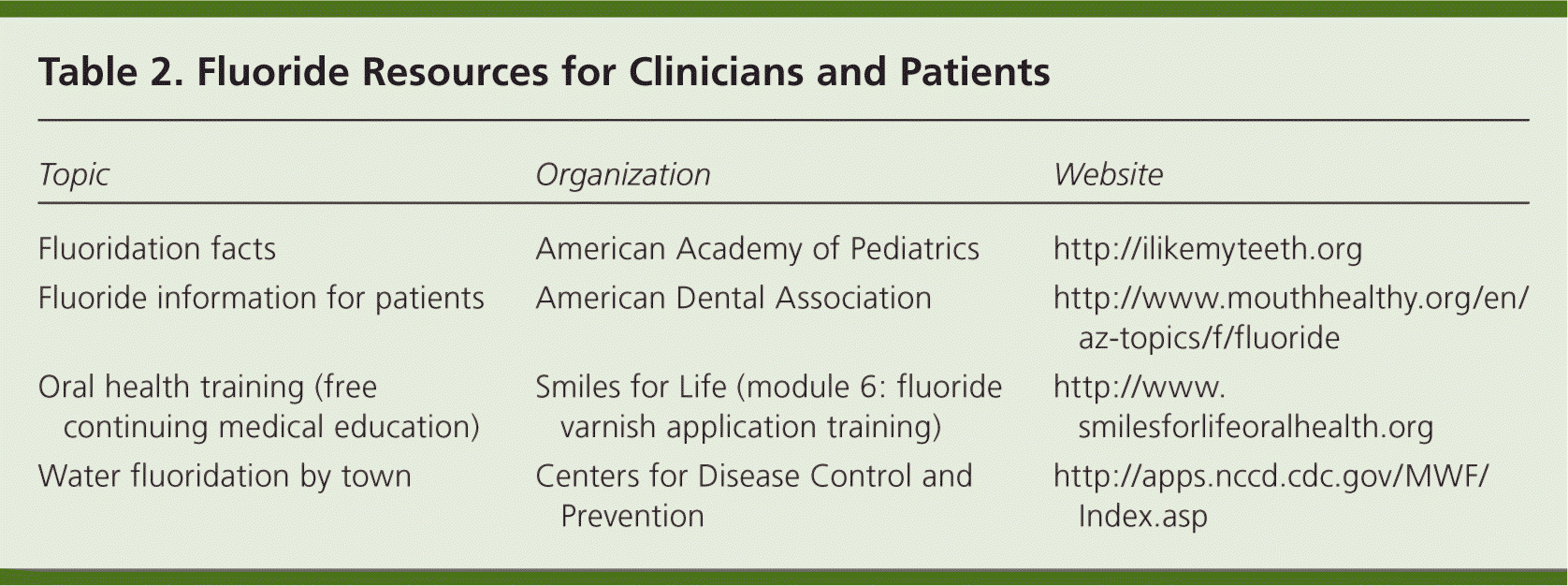
| Topic | Organization | Website |
|---|---|---|
| Fluoridation facts | American Academy of Pediatrics | http://ilikemyteeth.org |
| Fluoride information for patients | American Dental Association | http://www.mouthhealthy.org/en/az-topics/f/fluoride |
| Oral health training (free continuing medical education) | Smiles for Life (module 6: fluoride varnish application training) | http://www.smilesforlifeoralhealth.org |
| Water fluoridation by town | Centers for Disease Control and Prevention | http://nccd.cdc.gov/DOH_MWF/Default/Default.aspx |

