A 33-year-old man presented with asymptomatic blue-gray lesions on both feet. The lesions started developing six months earlier, getting darker and larger over time. He was using naproxen, tretinoin cream (Retin-A), and oral minocycline (Minocin).
Physical examination revealed coalescing, blue-gray, pinpoint papules and plaques on the distal dorsal, medial, and lateral surfaces of the feet (Figures 1 and 2). The lesions were nonblanching and nontender to palpation. Biopsy of the papules showed diffuse pigmentation of the dermis with distinct dark granules within macrophages.
Figure 1.
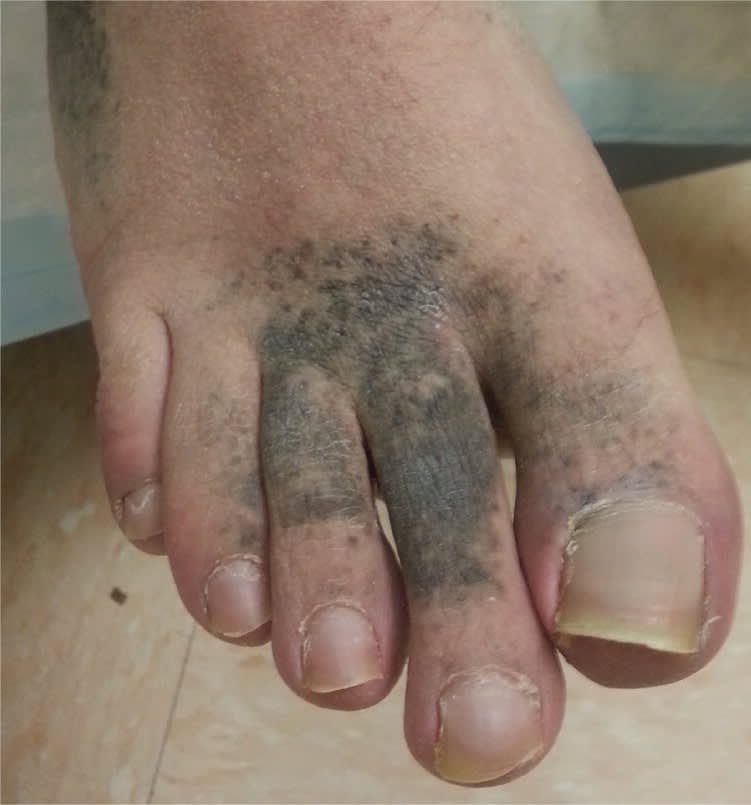
Figure 2.
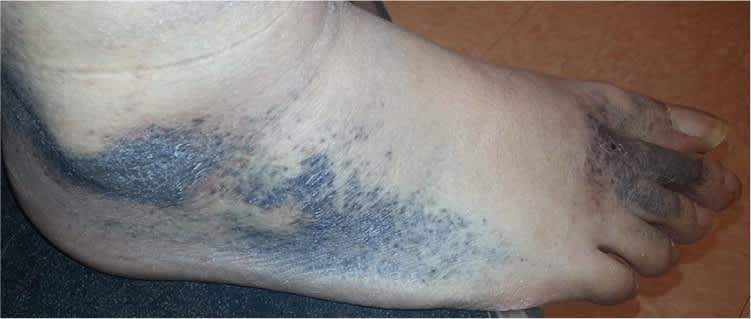
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Acanthosis nigricans.
B. Capillaritis.
C. Drug-induced hyperpigmentation.
D. Fixed drug eruption.
E. Lichen simplex chronicus.
Discussion
The answer is C: drug-induced hyperpigmentation. Hyperpigmentation is a well-known adverse effect of minocycline, an antibiotic used to treat acne vulgaris and rosacea. Hyperpigmentation can occur on cutaneous and mucosal surfaces, bone and teeth, and internal organs such as the thyroid.1 Although benign, it can lead to cosmetic concerns.2 One year prior to presentation, the patient had switched from oral doxycycline to minocycline for treatment of acne vulgaris because of a national shortage of doxycycline.
Hyperpigmentation from minocycline can be divided into three subtypes according to clinical and histopathologic findings.3 Two stains are used to distinguish the subtypes: Prussian blue stain (detects iron) and Fontana-Masson stain (detects melanin).
Type I is the most common subtype. It appears as black-blue pigmentation in areas of active inflammation or scarring. In patients taking minocycline to treat moderate to severe inflammatory facial acne, the hyperpigmentation primarily affects the face. Histologically, type-I lesions will stain positive for iron.4 Type II affects normal skin, most commonly on the arms and legs, and appears blue-gray. This type can be confused with persistent ecchymosis. Type-II lesions stain positive for iron and melanin. Type III is the least common form. It appears muddy brown and occurs on sun-exposed areas. It is associated with the dose and duration of minocycline treatment. This subtype stains positive for only melanin.5
Acanthosis nigricans presents as hyperpigmented velvety plaques and thickening of the skin in the flexural or intertriginous areas. It is common in patients with diabetes mellitus and obesity.
Capillaritis is caused by red blood cells leaking from superficial postcapillary venules. It appears clinically as brown-red macules, generally on the lower legs. The shade of pigment varies, representing different stages of hemosiderin reabsorption. Histologically, there are extravasated red blood cells within the papillary dermis and minimal epidermal changes.
A fixed drug eruption is an adverse drug reaction that produces a sharply demarcated pigmented patch at the same location with each exposure to the drug. It is common on the genitals, although it can occur anywhere. Histologically, changes may include a band-like lichenoid lymphocytic infiltrate, Civatte bodies, and abundant melanophages.
Lichen simplex chronicus is a consequence of chronic scratching or rubbing of the skin. Lesions are lichenified, well-demarcated plaques with occasional scaling and occur on the scalp, neck, wrists, lower legs, and genitals. They are typically pruritic.
Summary Table

| Condition | Physical examination | Location |
|---|---|---|
| Acanthosis nigricans | Hyperpigmented velvety plaques and thickening of the skin | Axillae, body folds (neck, inguinal areas) |
| Capillaritis | Brown-red macules; shades of pigment may vary, representing different stages of hemosiderin reabsorption | Generally the lower legs |
| Fixed drug eruption | Sharply demarcated pigmented patch appearing at the same location with each exposure to the drug | Anywhere, but commonly on the genitals |
| Lichen simplex chronicus | Lichenified, well-defined plaques with occasional scaling; typically pruritic | Scalp, neck, wrists, lower legs, genitals |
| Minocycline-induced hyperpigmentation | Skin discoloration: black-blue (type I), blue-gray (type II), muddy brown (type III) | Area of inflammation or scarring; commonly affects the face (type I), arms and lower legs (type II), and sun-exposed skin (type III) |

