A 30-year-old white man reported a 10-year history of itchy, scaly fingernails that chipped and fell off easily. The nails were pitted but not painful. All of his fingernails, but none of his toenails, were affected. He also had patches of dry, scaly skin on his scalp, low back, and genitals. He was otherwise healthy. He had been employed as a handyman. His family history was unremarkable.
On physical examination, most of the nails were intact but had some proximal erosion. The distal nails were clipped close, but some had separation from the nail bed, with scaling and yellowing distally. Most of the nails displayed pitting, with the periungual area unaffected (Figure 1). The patient had one pink patch with scale on the right temporal scalp, and additional patches on his back and scrotum.
Figure 1.
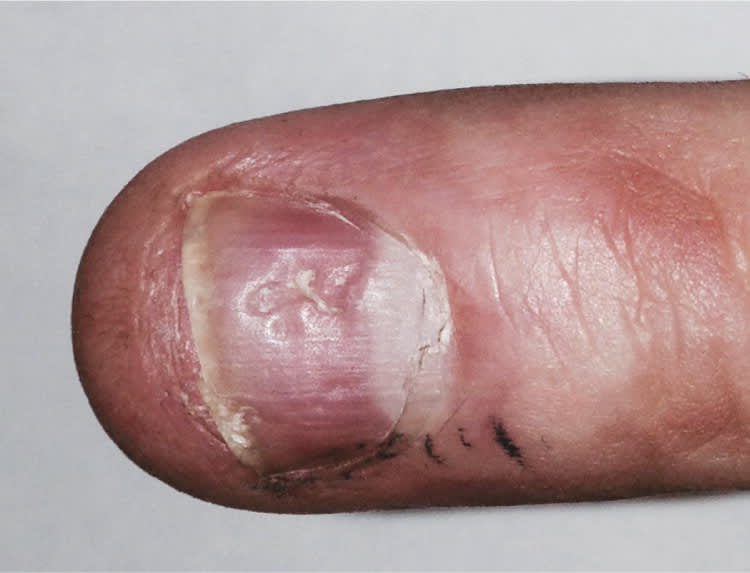
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Alopecia areata.
B. Chronic paronychia.
C. Iron deficiency.
D. Psoriasis.
E. Sarcoidosis.
Discussion
The answer is D: psoriasis. The patient has the classic pitting, scaling, and nail bed separation of psoriasis of the nails. Leukonychia (white nails) and trachyonychia (rough, sandpaper-like nails) are also present.1 The scaly patches on his body, his age, and his race also point to psoriasis.2 The nail pitting results from focal areas of abnormal keratinization in the nail matrix. The diagnosis of nail changes caused by psoriasis is clinical, and biopsy is not necessary.
Although psoriasis of the nail typically does not respond to topical treatments,3 topical corticosteroid with a vitamin D analogue can be tried for mild disease. Subungual glucocorticoid injections have also been used before systemic therapy.4 Nail psoriasis has shown improvement with oral infliximab (Remicade) and adalimumab (Humira). Oral retinoids (e.g., acitretin [Soriatane]), photochemotherapy, and pulsed dye laser therapy are not as effective.5 The benefits and adverse effects of these treatments should be discussed with the patient. Hand hygiene and use of moisturizers are important in the continued management of nail psoriasis.
Alopecia areata involves focal, nonscarring hair loss in areas of normal scalp. Within the patch of hair loss, there may be exclamation point hairs, which are thinner at the base.6 Patients with alopecia areata sometimes have nail pitting.
Chronic paronychia is a painful inflammation of the periungual area caused by an infection. It occurs in occupations in which the fingers are kept moist, such as fishmongers, aquarists, and hair stylists. There is no pitting of the nails.7
Iron deficiency can occur in patients with chronic blood loss or nutritional deficiency. It can cause nail abnormalities, such as brittle and thin nails and koilonychia (spooning of the nails).8
Sarcoidosis is a systemic granulomatous disease that primarily affects the lungs, eyes, and skin in adults. Nail changes, such as pitting, ridges, thinning, and brittleness, can occur with sarcoidosis but are rare.9
Summary Table
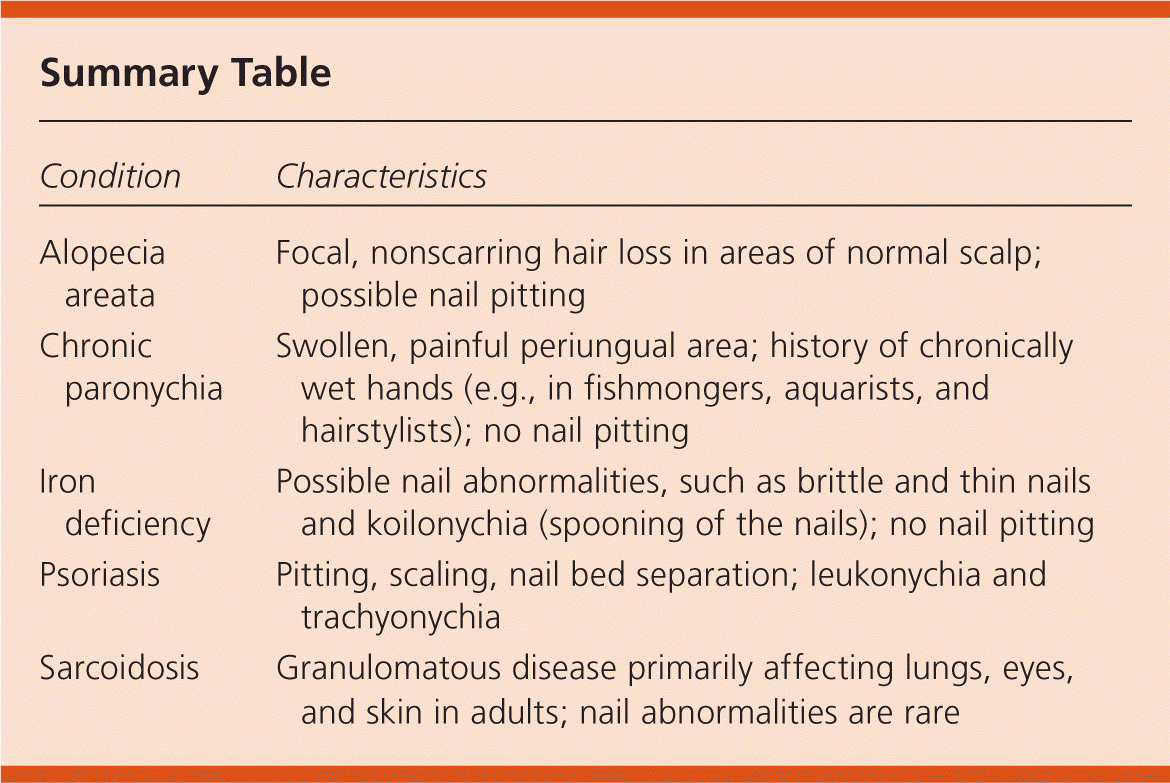
| Condition | Characteristics |
|---|---|
| Alopecia areata | Focal, nonscarring hair loss in areas of normal scalp; possible nail pitting |
| Chronic paronychia | Swollen, painful periungual area; history of chronically wet hands (e.g., in fishmongers, aquarists, and hairstylists); no nail pitting |
| Iron deficiency | Possible nail abnormalities, such as brittle and thin nails and koilonychia (spooning of the nails); no nail pitting |
| Psoriasis | Pitting, scaling, nail bed separation; leukonychia and trachyonychia |
| Sarcoidosis | Granulomatous disease primarily affecting lungs, eyes, and skin in adults; nail abnormalities are rare |
The views expressed are those of the author and do not reflect the official policy of Manet Community Health Center.

