One in five Americans reports no usual source of health care, and the number of Americans reporting that they have a personal relationship with a usual source of care has declined steadily over the past 15 years. Given the positive association between having a usual source of care and the nation's Triple Aim initiative of lower health care costs, improved population health outcomes, and better patient experience, this trend is worthy of further exploration and policy-maker attention.
Having a usual source of health care has been associated with improved health outcomes, fewer health disparities, and lower health system costs.1 Additionally, individuals with a usual source of care and health insurance are more likely to access care when needed and to seek preventive care services.2 We used data from the nationally representative Medical Expenditure Panel Survey collected between 1996 to 2012 to identify trends in the types of usual sources of care reported by individuals (Figure 1). We noted the percentage of people who reported having a usual source of care, and whether that source was a person or facility. To smooth the trends, a three-year moving average for each measure was calculated.
Figure 1.
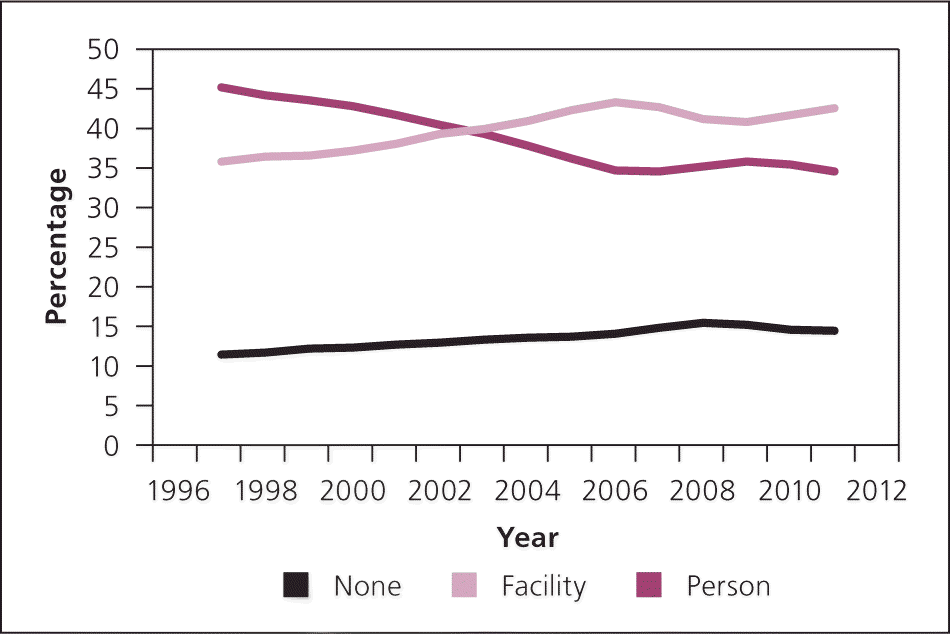
Types of usual sources of health care.
Data from the Medical Expenditure Survey (consolidated data files: 1996–2012).
Although the percentage of all persons who reported a usual source of care across the study period declined slightly, a more striking divergence was apparent in those who had a usual source of care. Declines in the percentage of people reporting an individual clinician as their usual source of care was countered by a nearly equivalent rise in those reporting a facility. These trends persisted even after controlling for age, race, insurance status, and poverty status. Previous studies have shown that most Americans (82%) have a usual source of care. For 56% of these people, their usual source is an individual as opposed to a facility, mostly family physicians (62%), followed by internists (16%), pediatricians (15%), and other clinicians (8%).3
It is unclear whether identifying a facility rather than a clinician as a usual source of care impacts the delivery of the primary care functions deemed essential to improving health system costs and quality—first contact, coordination, continuity, and comprehensiveness.4,5 It is also unknown whether the favorable effects of having a usual source of care hold true for people who shift from an individual to a facility as their usual source of care. The advent of patient-centered medical homes, broader primary care teams, and increased virtual contact may help to explain these findings and represent opportunities for improved outcomes. This important topic deserves further research and the attention of health care stakeholders.
The information and opinions contained in research from the Graham Center do not necessarily reflect the views or the policy of the AAFP.
This series is coordinated by Kenny Lin, MD, MPH, Associate Deputy Editor for AFP Online.

