A 52-year-old male smoker presented with a mildly pruritic rash that began three months earlier on his back and spread to his scalp, trunk, and extremities, including the palms and soles. He had a history of alcoholic cirrhosis. He had no recent new exposures, including medications.
Physical examination revealed numerous well-circumscribed, erythematous, non-blanching plaques with adherent white scale involving approximately 70% of his body (Figures 1 and 2). His palms and soles displayed thick scale with fissures, and he had oil spots and onycholysis affecting several fingernails.
Figure 1.
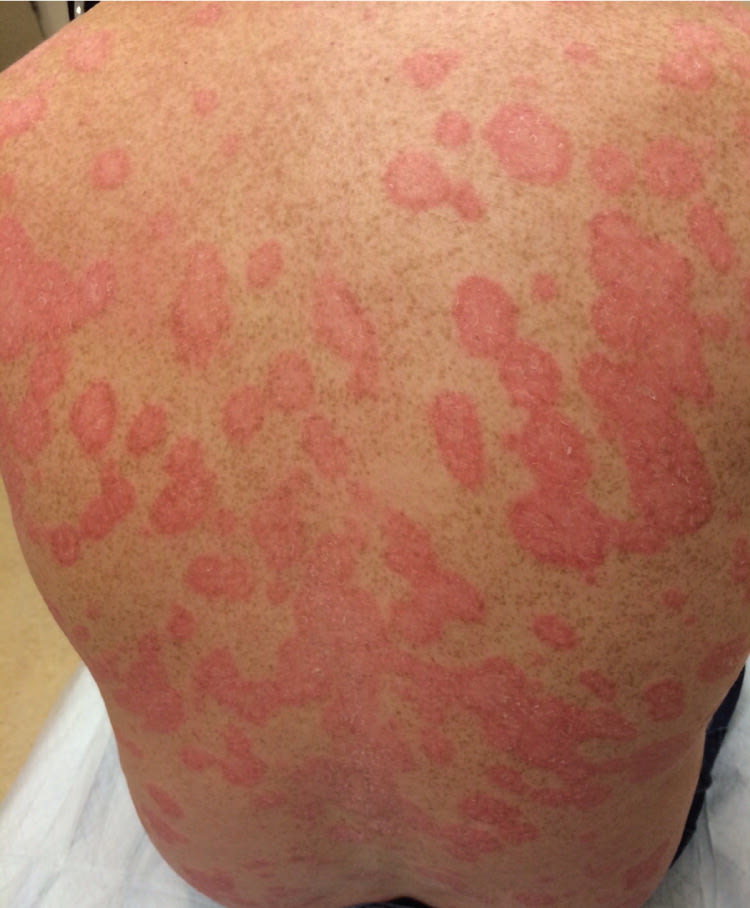
Figure 2.
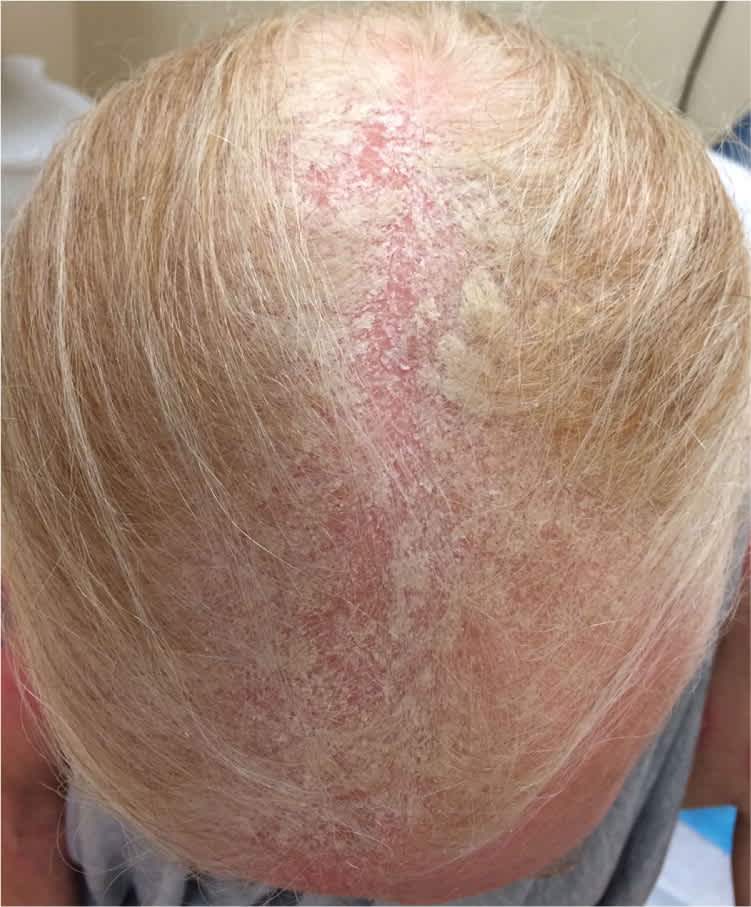
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Cutaneous sarcoidosis.
B. Nummular eczema.
C. Plaque psoriasis.
D. Subacute cutaneous lupus erythematosus.
E. Tinea corporis.
Discussion
The answer is C: plaque psoriasis. Psoriasis is a common autoimmune condition with a strong genetic component that affects 2% to 5% of the population.1 There is a bimodal distribution for onset of disease, with about 75% of cases occurring between 15 and 20 years of age; there is a second peak from 50 to 60 years of age.2 Behavioral factors associated with psoriasis include smoking, alcohol abuse, and obesity.2 After controlling for these factors, patients with psoriasis have an increased risk of cardiovascular disease and metabolic syndrome.3
Psoriasis is a clinical diagnosis that encompasses a wide spectrum of presentations often categorized by morphology.4 Plaque psoriasis is the most common pattern, characterizing 90% of cases.3,4 As demonstrated in this case, it is generally symmetric, and begins as scaly, erythematous macules that spread peripherally and coalesce to form plaques that may become confluent. Fissuring can occur when lesions extend to palms, soles, or joint lines. One-half of patients with psoriasis display nail involvement, including oil spots, onycholysis, subungual hyperkeratosis, or pitting.3 About 30% of patients also develop arthritis.1
Treatment of psoriasis depends on comorbidities and extent of disease. Topical treatments include tar, corticosteroids, and retinoids. Phototherapy is also effective.3,5 Systemic treatments include methotrexate, cyclosporine (Sandimmune), acitretin (Soriatane), and biologics such as T-cell and tumor necrosis factor inhibitors.3 Systemic corticosteroids should be avoided because they can significantly worsen disease when withdrawn.3,4 Patients should also be counseled about smoking and alcohol cessation, as well as weight loss.3
Approximately 25% of patients with sarcoidosis have skin involvement, which can have different manifestations. One form is plaque sarcoidosis, which appears as round, flat-topped, erythematous plaques that may be scaly. The plaques usually occur in a symmetric distribution on the face, extremities, or trunk.5,6
Nummular eczema typically begins on the extremities, often after trauma or allergic exposure, as a highly pruritic, coin-shaped, erythematous, vesicular, and crusted plaque.5 Small papulovesicular satellite lesions form around the primary lesion and coalesce into a larger plaque.5
Subacute cutaneous lupus erythematosus occurs primarily on sun-exposed skin, beginning with small, scaly, erythematous papules or plaques that expand into one of two forms: an annular lesion or a larger plaque in the psoriasiform/papulosquamous variant. One-half of these patients meet criteria for systemic lupus erythematosus.5,6
Tinea corporis is a superficial dermatophyte infection characterized by well-circumscribed, circular patches with central clearing and a scaly, raised, advancing edge. It begins on the trunk but may spread to the extremities. The diagnosis can be confirmed by demonstration of fungi on a potassium hydroxide examination of a skin scraping.5,6
Summary Table

| Condition | Characteristics |
|---|---|
| Cutaneous sarcoidosis | Round, flat-topped, erythematous plaques that may be scaly; other findings of sarcoidosis; symmetric distribution on the face, extremities, or trunk |
| Nummular eczema | Highly pruritic, coin-shaped, erythematous, vesicular, crusted plaques; often occurs after trauma or allergic exposure; typically begins on the extremities |
| Plaque psoriasis | Scaly, erythematous macules that coalesce to form plaques; symmetric, spreads peripherally |
| Subacute cutaneous lupus erythematosus | Small, scaly, erythematous papules or plaques that expand to form an annular lesion or a larger plaque; one-half of patients meet criteria for systemic lupus erythematosus; occurs primarily on sun-exposed skin |
| Tinea corporis | Well-circumscribed, circular patches with central clearing; scaly, raised, advancing edge; begins on the trunk, but may spread to extremities |

