A 31-year-old man presented with a lesion on his tongue that he first noticed six months earlier as small red dots. His dentist thought it was caused by irritation from his dental bridge. It was painless, but he had some bleeding after brushing his teeth and tongue. He had not received any medical care for the lesion.
His medical history was significant for hypertension treated with hydrochlorothiazide, and a recent clavicle fracture after a motorcycle accident. He never smoked, but he used one can per week of chewing tobacco for one year. He quit five years before presentation. He drank less than three alcoholic beverages per week. A review of systems was negative. He was not using any new toothpastes or mouthwashes.
On physical examination, he was well appearing and afebrile, but overweight. His tongue had a large lateral fungating, whitish, exophytic lesion with anterior fissuring of the entire left side of the tongue (Figure 1). There was no tenderness or ulceration. He had a slight speech impediment secondary to mouth fullness but no difficulty swallowing. There were no palpable cervical lymph nodes.
Figure 1.
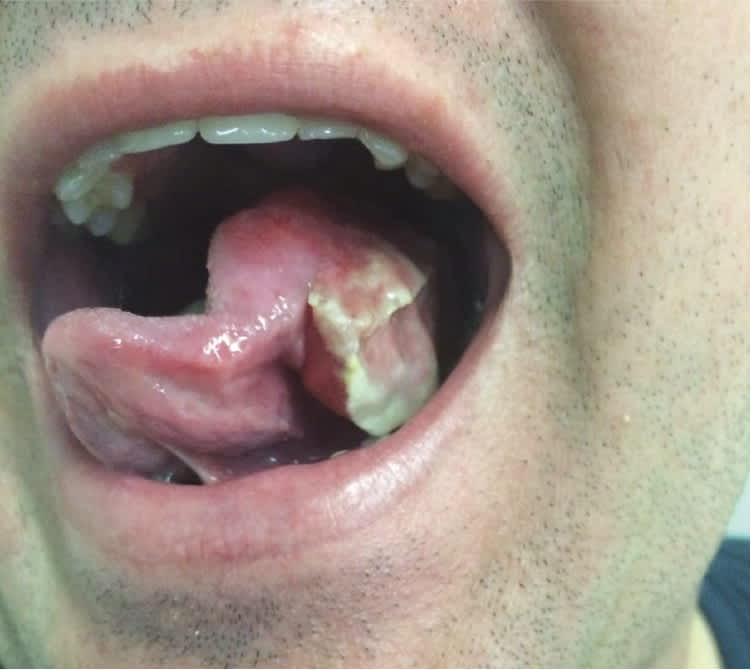
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Mucosal candidiasis.
B. Oral leukoplakia.
C. Oral pyogenic granuloma.
D. Squamous cell carcinoma.
Discussion
The answer is D: squamous cell carcinoma, which required urgent biopsy and surgical excision. The characteristic features of oral squamous cell carcinoma include lateral location, fungating appearance, whitish color, and central ulceration. The history of tobacco use lasting for one year also makes cancer more likely. The history suggests that the lesion began as erythroplakia, which was thought to be related to his dental work. He never received follow-up because of an overseas deployment.
After the biopsy confirmed squamous cell carcinoma, he underwent subtotal left glossectomy, bilateral radical neck dissection, tracheotomy, and radical forearm free flap reconstruction. The patient was treated with adjuvant chemotherapy. Oral squamous cell carcinomas are often preceded by potentially malignant disorders. Patients may have erythroplakia, an ulcer with fissuring or exophytic margins, a speckled (red/white) leukoplakia, a lump with abnormal blood vessels, an indurated lump or ulcer, or a nonhealing socket after tooth extraction.1–3 Diagnosis may be delayed for up to six months. Early detection and treatment are the key to significantly decreased morbidity and mortality.
Approximately 90% of oral cancers are squamous. Squamous cell carcinoma is common in men, with an average age of onset of 50 years. The etiology is multifactorial and related to lifestyle, including use of tobacco, betel nut, and alcohol.4–6 This patient had never received the human papillomavirus (HPV) vaccine, and HPV infection has a potential role in the transformation of cells into precancerous and cancerous oral lesions.7
Mucosal candidiasis, or thrush, is less common in adults. It typically occurs with immune suppression, such as in those with human immunodeficiency virus infection or AIDS, those who have had an organ transplant, and those taking immunosuppressants or antimicrobials. Mucosal candidiasis presents as multiple white patches resembling milk curds. The patches can be wiped off, revealing a raw erythematous base. Irritation and pain are common.
Oral leukoplakia is a bright white, sharply defined patch or plaque that cannot be wiped off. It is a diagnosis of exclusion pending appropriate histologic workup. Oral leukoplakia is thought to be a premalignant condition and does not typically cause symptoms.
Oral pyogenic granulomas have a rapid growth pattern (over one to two weeks) and are nodular and erythematous in appearance. They can undergo fibrous maturation, appearing more whitish, or transform completely to fibromas. They often occur on the buccal gingiva between the teeth and typically bleed spontaneously without irritation.
Summary Table
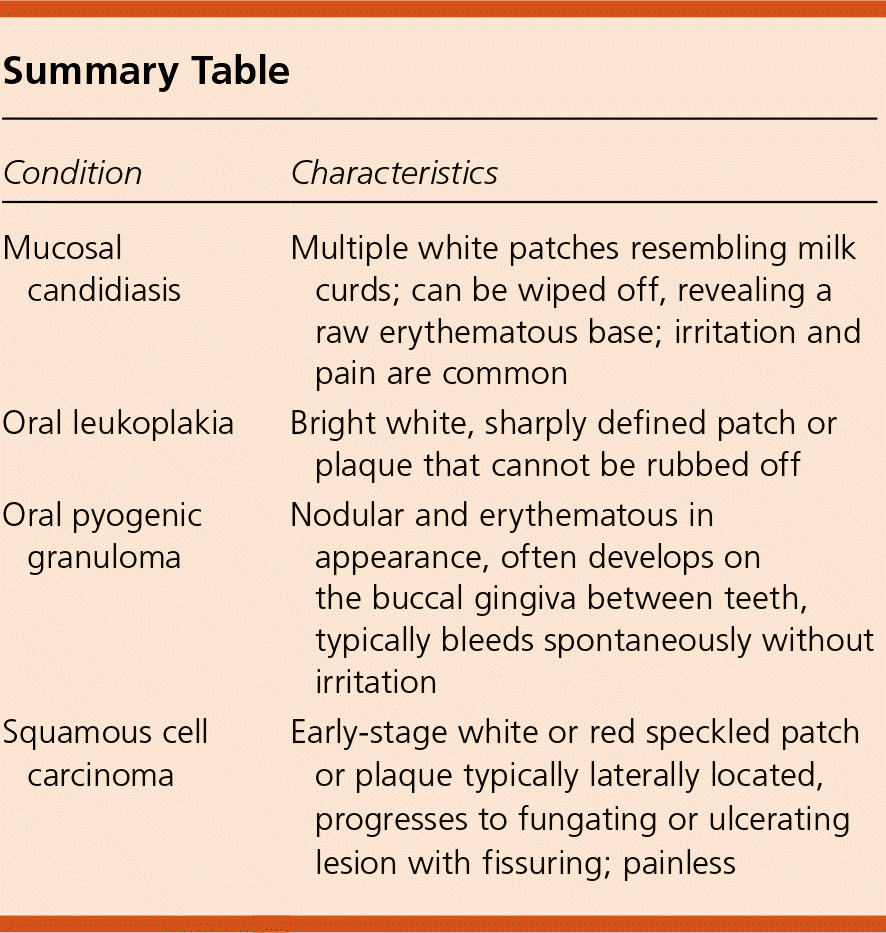
| Condition | Characteristics |
|---|---|
| Mucosal candidiasis | Multiple white patches resembling milk curds; can be wiped off, revealing a raw erythematous base; irritation and pain are common |
| Oral leukoplakia | Bright white, sharply defined patch or plaque that cannot be rubbed off |
| Oral pyogenic granuloma | Nodular and erythematous in appearance, often develops on the buccal gingiva between teeth, typically bleeds spontaneously without irritation |
| Squamous cell carcinoma | Early-stage white or red speckled patch or plaque typically laterally located, progresses to fungating or ulcerating lesion with fissuring; painless |
The opinions and assertions contained herein are the private views of the author and are not to be construed as official or as reflecting the views of the U.S. Navy Medical Department or the U.S. Navy at large.

