Breast cancer is one of the most common malignancies among women, with approximately 3% of women dying from the disease and approximately 12% of those who live to 80 years of age being diagnosed with it at some point during their lifetime.1 Although screening mammography reduces breast cancer–specific mortality, women may overestimate its benefit.2
Biennial mammography is recommended for all women between 50 and 74 years of age by the U.S. Preventive Services Task Force (USPSTF).3 The American Cancer Society (ACS) updated its guidelines in 2015, increasing the age at which all women should receive regular mammography from 40 to 45 years.4 The USPSTF identifies biennial mammography as the interval with the best balance of benefits and harms. The ACS recommends shared decision making regarding when to start mammography for women 40 to 44 years of age, annual mammography for women 45 to 54 years of age, and biennial mammography after that.
For women 40 to 49 years of age, in whom the net benefit of screening mammography is smaller than in older women, the USPSTF recommends that physicians discuss the risks and benefits of screening and let the patient decide when to begin. The task force notes that women who have a first-degree relative diagnosed with breast cancer should be screened starting at 40 years of age, and that the balance of benefits and harms becomes more favorable as women advance through their 40s.
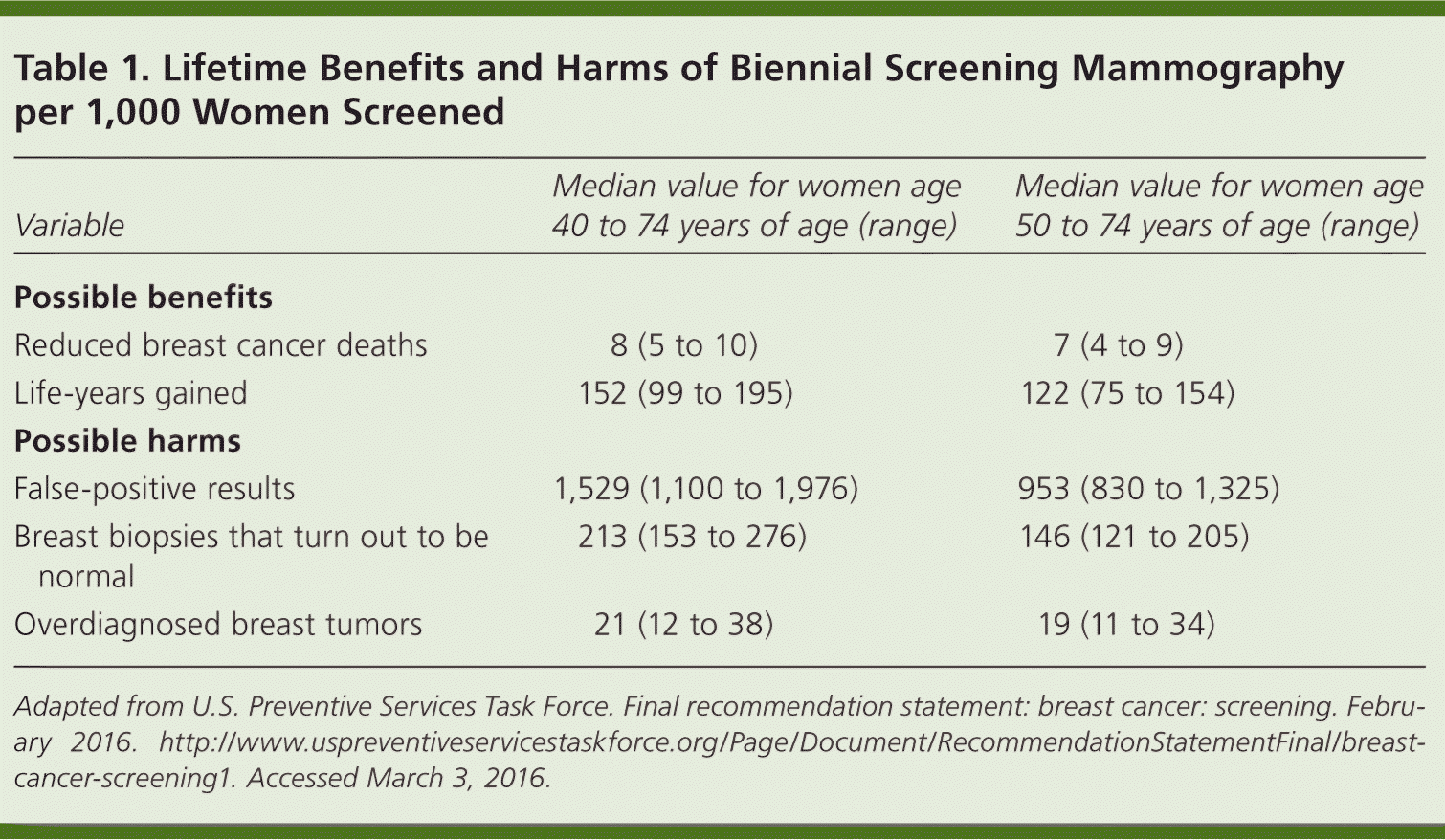
What are the data regarding potential benefits and harms of starting mammography at 40 vs. 50 years of age? Table 1 summarizes the results of a lifetime program of screening mammography in 1,000 women, ending at 75 years, and outlines the key benefits and harms associated with starting mammography at 40 vs. 50 years of age.5 For every 1,000 women who start screening mammography at 40 instead of 50 years, approximately one woman will live about 30 years longer, whereas about 600 women will have a false-positive test result, about 70 will have a biopsy that ends up being normal, and two will be treated for a cancer that never would have caused any symptoms or problems.
Table 1. Lifetime Benefits and Harms of Biennial Screening Mammography per 1,000 Women Screened
| Variable | Median value for women age 40 to 74 years of age (range) | Median value for women age 50 to 74 years of age (range) |
|---|---|---|
| Possible benefits | ||
| Reduced breast cancer deaths | 8 (5 to 10) | 7 (4 to 9) |
| Life-years gained | 152 (99 to 195) | 122 (75 to 154) |
| Possible harms | ||
| False-positive results | 1,529 (1,100 to 1,976) | 953 (830 to 1,325) |
| Breast biopsies that turn out to be normal | 213 (153 to 276) | 146 (121 to 205) |
| Overdiagnosed breast tumors | 21 (12 to 38) | 19 (11 to 34) |
Adapted from U.S. Preventive Services Task Force. Final recommendation statement: breast cancer: screening. February 2016. http://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/breast-cancer-screening1. Accessed March 3, 2016.
What about screening women older than 75 years? Although the USPSTF concluded that evidence for this age group was insufficient because randomized trials have not included any women older than 75 years, modeling studies commissioned by the USPSTF suggest that the benefit of mammography may extend to healthy older women in this age group.6 The ACS supports continuing screening until women have a life expectancy of 10 years or less.4
In the context of a busy office visit, how can we do conversations about breast cancer screening justice? It is important that we initiate the conversation with our patients, who may not know that they have a decision to make, by asking, “Are you ready to talk about when you want to start getting mammograms?” This question could be posed by the nurse or medical assistant, and if the patient answers in the affirmative, a handout with easy-to-understand information about the potential benefits and harms of starting mammography at 40 years of age could be given (Table 2).
Table 2. Information for Patients Deciding When to Start Getting Mammograms

| Summary | |
| Women in their 40s and their physicians should discuss the pros and cons of starting mammography before 50 years of age. Based on the best scientific evidence, here are the potential benefits and harms for 1,000 women who start mammography at 40 years compared with 50 years: | |
| • One woman diagnosed with breast cancer will not die | |
| • 576 more women will have a false-positive test result | |
| • 67 more women will have breast biopsies with normal results | |
| • Two women will be diagnosed and treated for breast tumors that would never have caused symptoms or problems or needed treatment | |
| Important Terms | |
| False-positive result: A false positive is sometimes called a false alarm or cancer scare. In these cases, patients are called back for more imaging because something unusual was seen on the first mammogram, but it turns out to not be a cancer. | |
| Breast biopsy: Sometimes, additional imaging cannot sort out whether a finding is or is not a cancer. About one out of 10 times, a doctor has to do a biopsy to confirm if a patient has cancer, which involves numbing the tissue in the breast and using a needle to gather tissue for examination under the microscope. | |
| Overdiagnosed breast tumor: Some cancers (about one out of five) grow very slowly, to the point where they would never have caused symptoms or problems, and the patient would have eventually died of something else. Finding and treating these tumors in women who get mammograms lead to unneeded worry and treatment. | |
If the physician's practice uses a patient portal or contacts patients by e-mail before visits, women could be referred to a site that helps them make an informed decision before their visit, such as http://breastscreeningdecisions.org. These practical strategies can help family physicians and women in their 40s make more informed decisions about breast cancer screening.
editor's note: Dr. Ebell is AFP's deputy editor for evidence-based medicine. He is a member of the USPSTF. This article is his own work and does not necessarily represent the views and policies of the USPSTF. Dr. Lin is associate deputy editor for AFP online.

