Cardiovascular disease (CVD) is the leading cause of death in the United States. One-third of these deaths may be preventable through healthy lifestyle choices including diet and physical activity. The Mediterranean diet is associated with reduced cardiovascular mortality, whereas the Dietary Approaches to Stop Hypertension (DASH) eating plan is associated with a reduced risk of coronary artery disease. Substituting dietary saturated fat with polyunsaturated fatty acids is associated with improved cardiovascular outcomes, although exogenous supplementation with omega-3 fatty acids does not improve cardiovascular outcomes. There is an association between increased sodium intake and cardiovascular risk, but reducing dietary sodium has not consistently shown a reduction in cardiovascular risk. Physical activity recommendations for adults are at least 150 minutes of moderate-intensity aerobic activity per week, 75 minutes of vigorous-intensity aerobic activity per week, or an equivalent combination. Increases in physical activity by any level are associated with reduced cardiovascular risk. Introducing muscle-strengthening activities at least twice per week in previously inactive adults is associated with improved cardiovascular outcomes. Inactive adults without known CVD can gradually increase activity to a moderate-intensity level without consulting a physician. The U.S. Preventive Services Task Force recommends behavioral counseling to promote healthy diet and physical activity in adults at high risk of CVD. Evidence of benefit for counseling patients at average risk is less established.
Cardiovascular disease (CVD) is the leading cause of death in the United States.1 From 2008 to 2010, CVD accounted for 272,668 deaths annually in persons younger than 80 years. Nearly one-third of deaths from CVD are considered potentially preventable.1 The American Heart Association (AHA) has published recommendations defining ideal cardiovascular health. Recommendations for physical activity in adults are at least 150 minutes of moderate-intensity aerobic activity or at least 75 minutes of vigorous-intensity aerobic activity per week.2 Ideal cardiovascular health also includes adhering to at least four of five components of a diet consistent with the Dietary Approaches to Stop Hypertension (DASH) eating plan (Table 1).2
WHAT IS NEW ON THIS TOPIC: CARDIOVASCULAR DISEASE PREVENTION
Benefits of combined lifestyle interventions to reduce cardiovascular disease risk may be more pronounced in groups at higher risk, such as patients with diabetes mellitus or hypertension.
Any physical activity is associated with lower cardiovascular risk, and the benefit increases with increasing amounts of weekly physical activity.
Although increased sodium intake has been associated with stroke and cardiovascular disease, a 2014 Cochrane review evaluating dietary sodium restriction in normotensive and hypertensive patients showed no effect on cardiovascular outcomes or all-cause mortality.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Adults should follow an eating plan consistent with the Dietary Approaches to Stop Hypertension diet or the Mediterranean diet. | A | 11, 13, 14 |
| Substituting dietary saturated fat with polyunsaturated fat is recommended to reduce cardiovascular risk. | B | 18 |
| Adults healthy enough to exercise should engage in at least 150 minutes of moderate-intensity aerobic activity, 75 minutes of vigorous-intensity aerobic activity, or an equivalent combination, each week. | A | 27, 28 |
| Physically inactive adults should be counseled that any increase in physical activity is associated with a reduction in cardiovascular risk. | A | 27, 28 |
| Muscle-strengthening activity at least twice per week in previously inactive adults is associated with improved cardiovascular outcomes. | B | 29 |
| Adults without a significant history of cardiovascular disease can gradually increase their activity level to moderate intensity safely without consulting a physician. | C | 27 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Table 1. Dietary Approaches to Stop Hypertension (DASH) Eating Plan

| ≥ 4.5 cups of fruits and vegetables per day |
| ≥ 2 3.5-oz servings of fish, preferably oily fish, per week |
| ≥ 3 1-oz-equivalent servings of fiber-rich whole grains per day (defined as at least 1.1 g of fiber per 10 g of carbohydrate) |
| < 1,500 mg of sodium per day |
| < 450 calories (36 oz) of sugar-sweetened beverages per week |
Information from reference 2.
Adherence to these recommendations is low. Only 5% of adults achieve the recommended amount of moderate-intensity physical activity when objectively measured,3 and only 18% meet the AHA goals for daily fruit and vegetable consumption.4 Additionally, nearly 35% of adults in the United States were obese in 2011 and 2012.5 Family physicians can make an important contribution by counseling patients on the health benefits of adhering to healthy diet and physical activity recommendations.
Diet
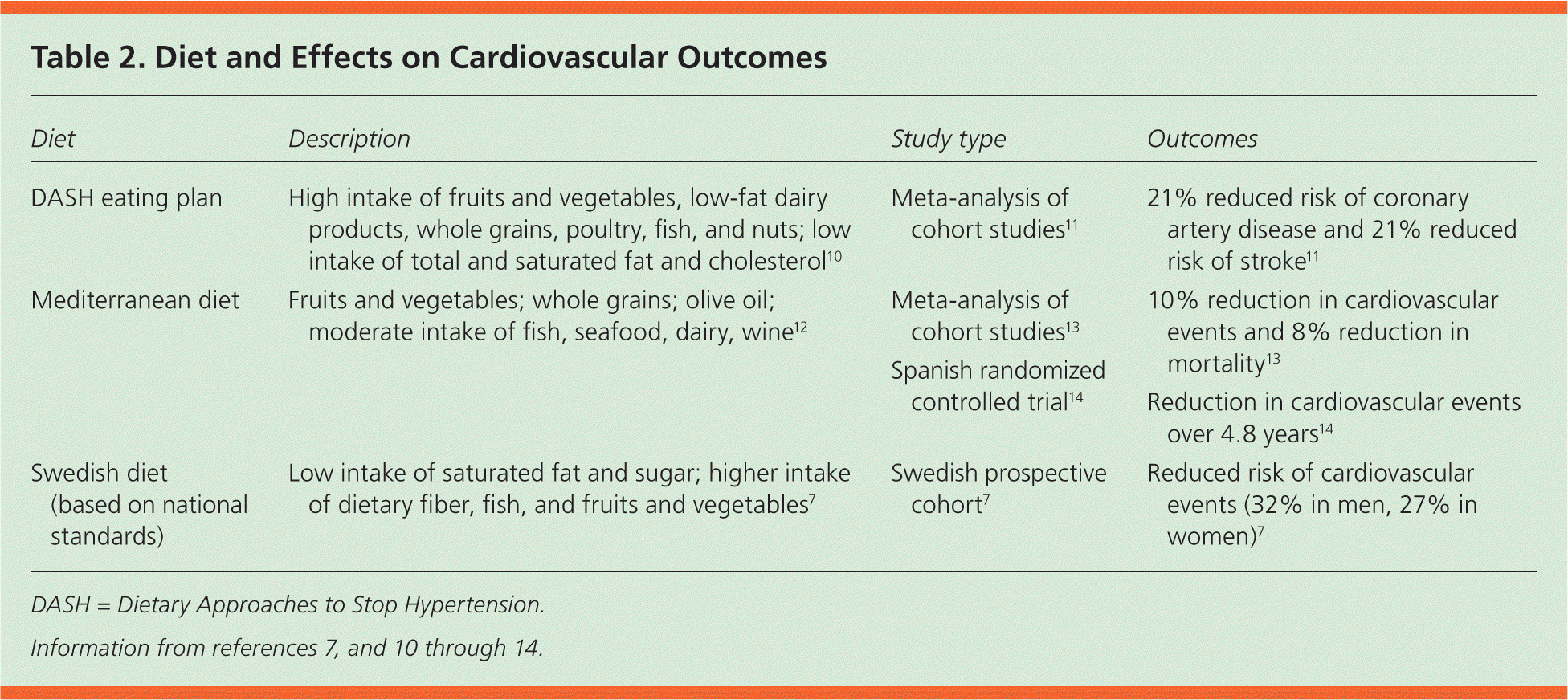
It is difficult to isolate the effects of individual nutrients on health benefits. Current research suggests the greater importance of viewing diet as a whole rather than focusing on specific nutrients.6,7 Several dietary approaches have been studied for their effects on CVD. Low-fat diets and high-fat, low-carbohydrate diets are popular and effective for weight loss, but there is insufficient evidence to recommend them for primary CVD prevention.8,9 There are several dietary strategies that have been evaluated for patient-oriented outcomes, such as cardiovascular events, cardiovascular mortality, and all-cause mortality. A summary of different dietary strategies is shown in Table 2.7,10–14
Table 2. Diet and Effects on Cardiovascular Outcomes
| Diet | Description | Study type | Outcomes |
|---|---|---|---|
| DASH eating plan | High intake of fruits and vegetables, low-fat dairy products, whole grains, poultry, fish, and nuts; low intake of total and saturated fat and cholesterol10 | Meta-analysis of cohort studies11 | 21% reduced risk of coronary artery disease and 21% reduced risk of stroke11 |
| Mediterranean diet | Fruits and vegetables; whole grains; olive oil; moderate intake of fish, seafood, dairy, wine12 | Meta-analysis of cohort studies13 | 10% reduction in cardiovascular events and 8% reduction in mortality13 |
| Spanish randomized controlled trial14 | Reduction in cardiovascular events over 4.8 years14 | ||
| Swedish diet (based on national standards) | Low intake of saturated fat and sugar; higher intake of dietary fiber, fish, and fruits and vegetables7 | Swedish prospective cohort7 | Reduced risk of cardiovascular events (32% in men, 27% in women)7 |
DASH = Dietary Approaches to Stop Hypertension.
MEDITERRANEAN DIET
Mediterranean diets emphasize diversity and seasonality, fruits and vegetables, whole grains, and olive oil, with moderate intake of fish, seafood, dairy, and wine.12 A 2010 meta-analysis of prospective cohort studies showed that increased adherence to a Mediterranean diet reduced cardiovascular events such as myocardial infarction (MI) and stroke, and lowered cardiovascular mortality (relative risk [RR] = 0.90; 95% confidence interval [CI], 0.87 to 0.93) and all-cause mortality (RR = 0.92; 95% CI, 0.90 to 0.94).13 A 2013 randomized controlled trial (RCT) of 7,447 patients in Spain with type 2 diabetes mellitus or three other cardiovascular risk factors showed that a Mediterranean diet was associated with a five-year reduction in a composite end point of MI, stroke, and cardiovascular mortality. The diet was supplemented with extra virgin olive oil (absolute risk reduction = 0.6%; number needed to treat = 167) or nuts (absolute risk reduction = 1%; number needed to treat = 100).14
SWEDISH DIET
A population-based prospective cohort study of 17,216 men in Sweden evaluated diet quality as measured by adherence to the 2005 Swedish dietary guidelines, emphasizing low intake of saturated fat and sugar, and higher intake of dietary fiber, fish, and fruits and vegetables. The primary composite outcome after 16 years was cardiovascular events including MI, ischemic stroke, or death from ischemic heart disease. Participants with a high-quality diet had a lower risk of cardiovascular events (hazard ratio [HR] = 0.68; 95% CI, 0.49 to 0.73 for men; HR = 0.73; 95% CI, 0.59 to 0.91 for women).7
DASH EATING PLAN
The DASH eating plan emphasizes a diet with high intake of fruits and vegetables, low-fat dairy products, whole grains, poultry, fish, and nuts, and low intake of total and saturated fat and cholesterol.10 A 2013 meta-analysis of six cohort studies evaluated the association of adherence to the DASH diet and the incidence of cardiovascular outcomes. Adherence decreased the risk of coronary artery disease (RR = 0.79; 95% CI, 0.71 to 0.88) and stroke (RR = 0.81; 95% CI, 0.72 to 0.92).11
POLYUNSATURATED FATTY ACIDS
There is significant debate about polyunsaturated fatty acids (PUFAs) and their role in the primary prevention of cardiovascular events. Several meta-analyses of RCTs have shown varying degrees of benefit for omega-3 fatty acids.15 Several of these analyses, however, pooled the effect of increased dietary intake and exogenous supplementation of omega-3 fatty acids. A 2012 meta-analysis of 21 prospective cohort studies involving more than 675,000 participants evaluated fish consumption and cerebrovascular disease over a mean of 15.1 years. The authors found that eating two to four servings of fish weekly was associated with a reduced risk of cerebrovascular disease (RR = 0.94; 95% CI, 0.90 to 0.98). An increase of two servings of any fish per week was associated with a 4% risk reduction of cerebrovascular disease.16 However, a 2014 RCT of more than 4,200 patients 50 to 85 years of age taking omega-3 fatty acids for macular degeneration showed that supplementation did not decrease the risk of cardiovascular events.17
A 2010 meta-analysis of eight RCTs with more than 13,000 patients evaluated an increase in total or omega-6 PUFA intake as a substitute for saturated fat intake. The primary outcome was a composite of cardiovascular events including MI, cardiovascular mortality, or sudden death. In aggregate, participants in the intervention group consumed 15% of daily calories from PUFAs vs. 5% in the control group. Increased PUFA consumption was associated with an RR of 0.81 (95% CI, 0.70 to 0.95) for the primary outcome.18
The U.S. Food and Drug Administration recommends that saturated fats account for no more than 5% to 6% of daily caloric intake.10 Evidence shows that a diet high in PUFAs is associated with a reduction in cardiovascular events, but current evidence does not conclusively support the use of omega-3 fatty acid supplements for CVD prevention.
SODIUM RESTRICTION
Observational data have linked increased sodium intake in overweight patients to an increased risk of stroke, CVD mortality, and all-cause mortality.19 Increased sodium intake is associated with higher rates of stroke and CVD. Based largely on observational data, the AHA published an updated recommendation in 2012 reaffirming that dietary sodium intake should not exceed 1,500 mg per day.20 However, a 2014 Cochrane review of eight RCTs evaluating dietary sodium restriction in normotensive and hypertensive patients showed no effect on cardiovascular outcomes and all-cause mortality.21 Current evidence suggests a J-shaped association between sodium intake and CVD, with the lowest risk occurring with consumption of 3 to 5 g of sodium per day.22 Prospective evidence currently does not support sodium restriction.
Physical Activity
Physical activity is routinely recommended to promote optimal cardiovascular health. Physical inactivity and a less active lifestyle have been linked to significant increases in CVD risk.23 Elimination of a sedentary lifestyle may reduce CVD by 15% to 39% and stroke by 33%.23 A meta-analysis of prospective cohort studies estimated that reducing the time spent sitting to less than three hours per day would result in a two-year increase in average life expectancy.24 Observational studies consistently show an association between increased physical activity and reduction of CVD. A study of 9,181 men and women 50 years and older used self-reports of physical activity to categorize participants into low, moderate, and high levels of activity.25 The primary outcome was incident or fatal CVD. When adjusted for age, sex, and other comorbid conditions, a high level of physical activity was associated with a reduction in incident CVD (HR = 0.77; 95% CI, 0.68 to 0.89) and cardiovascular mortality in patients with baseline CVD (HR = 0.77; 95% CI, 0.65 to 0.89). Additionally, high (HR = 0.68; 95% CI, 0.56 to 0.84) and moderate (HR = 0.78; 95% CI, 0.64 to 0.94) levels of physical activity were associated with a reduction in cardiovascular mortality in patients without baseline CVD.25
Objective parameters of exercise tolerance also show that increased exercise capacity is associated with lower mortality. In one observational study, 6,213 men (mean age = 59 years) were referred for treadmill stress testing and followed for a mean of 6.2 years. Among the men without CVD, there was a significantly increased risk of all-cause mortality (RR = 4.5; 95% CI, 3.0 to 6.8) for those with an exercise capacity of less than six metabolic equivalents compared with those achieving a capacity of at least 13 metabolic equivalents. Additionally, the age-adjusted RR of death incrementally increased with decreasing exercise capacity, both among otherwise healthy participants and those with CVD.26
The 2008 Physical Activity Guidelines for Americans provide recommendations for physical activity (Table 3).27 Adults healthy enough to exercise should engage in a total of 150 minutes of moderate-intensity aerobic activity or 75 minutes of vigorous-intensity aerobic activity per week. A systematic review of 33 studies evaluated different levels of physical activity on the risk of coronary heart disease.28 Adults who were physically active at half of the level suggested by the 2008 guidelines had reduced risks of coronary heart disease (RR = 0.86; 95% CI, 0.77 to 0.96), similar to the degree of risk reduction observed in those who met the recommended physical activity targets. Those who met the standard for additional health benefits had an additional risk reduction (RR = 0.80; 95% CI, 0.74 to 0.88).28 These data suggest that any physical activity is associated with lower cardiovascular risk, and the benefit increases as the amount of weekly physical activity increases. Analysis of data from the 1999 to 2004 National Health and Nutrition Examination Survey showed that the adjusted HR for all-cause mortality was 44% lower among previously insufficiently active adults who engaged in muscle-strengthening activity at least twice per week.29
Table 3. 2008 Physical Activity Guidelines for Americans
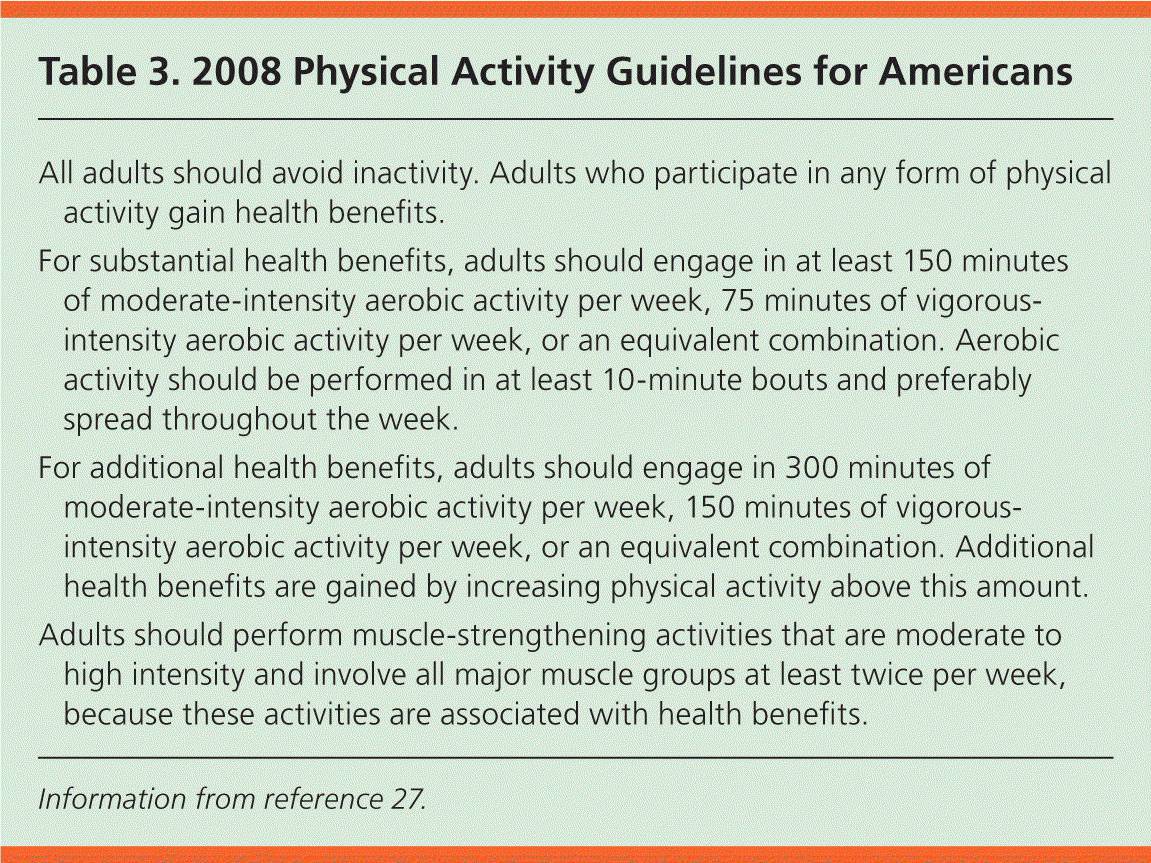
| All adults should avoid inactivity. Adults who participate in any form of physical activity gain health benefits. |
| For substantial health benefits, adults should engage in at least 150 minutes of moderate-intensity aerobic activity per week, 75 minutes of vigorous-intensity aerobic activity per week, or an equivalent combination. Aerobic activity should be performed in at least 10-minute bouts and preferably spread throughout the week. |
| For additional health benefits, adults should engage in 300 minutes of moderate-intensity aerobic activity per week, 150 minutes of vigorous-intensity aerobic activity per week, or an equivalent combination. Additional health benefits are gained by increasing physical activity above this amount. |
| Adults should perform muscle-strengthening activities that are moderate to high intensity and involve all major muscle groups at least twice per week, because these activities are associated with health benefits. |
Information from reference 27.
The benefits of physical activity on reducing cardiovascular events and mortality have also been demonstrated in men with diabetes. A subset of 2,803 men in the Health Professionals Follow-up Study with self-reported type 2 diabetes at 30 years or older were grouped into quintiles of physical activity and followed for 14 years. Compared with those in the lowest quintile, men who performed in the second quintile of physical activity had a lower risk of fatal CVD (RR = 0.55; 95% CI, 0.32 to 0.96), and continued risk reduction was demonstrated to the highest quintile of physical activity (RR = 0.45; 95% CI, 0.24 to 0.84).30 Data on the effects of physical activity on mortality and cardiovascular events in other high-risk populations are limited.
Recommendations for physical activity should be tailored to individual patients' long-term goals. Various examples of physical activity and their associated levels of intensity are provided in Table 4.23,27 These are general associations; individual effort in each of these activities will determine the intensity of the activity. Inactive adults who are otherwise healthy can gradually increase their activity to moderate intensity without consulting a physician.27 Likewise, adults with a baseline regimen of regular moderate-intensity activity can safely advance to vigorous-intensity activities without consultation.27
Table 4. Intensity Levels for Various Forms of Physical Activity
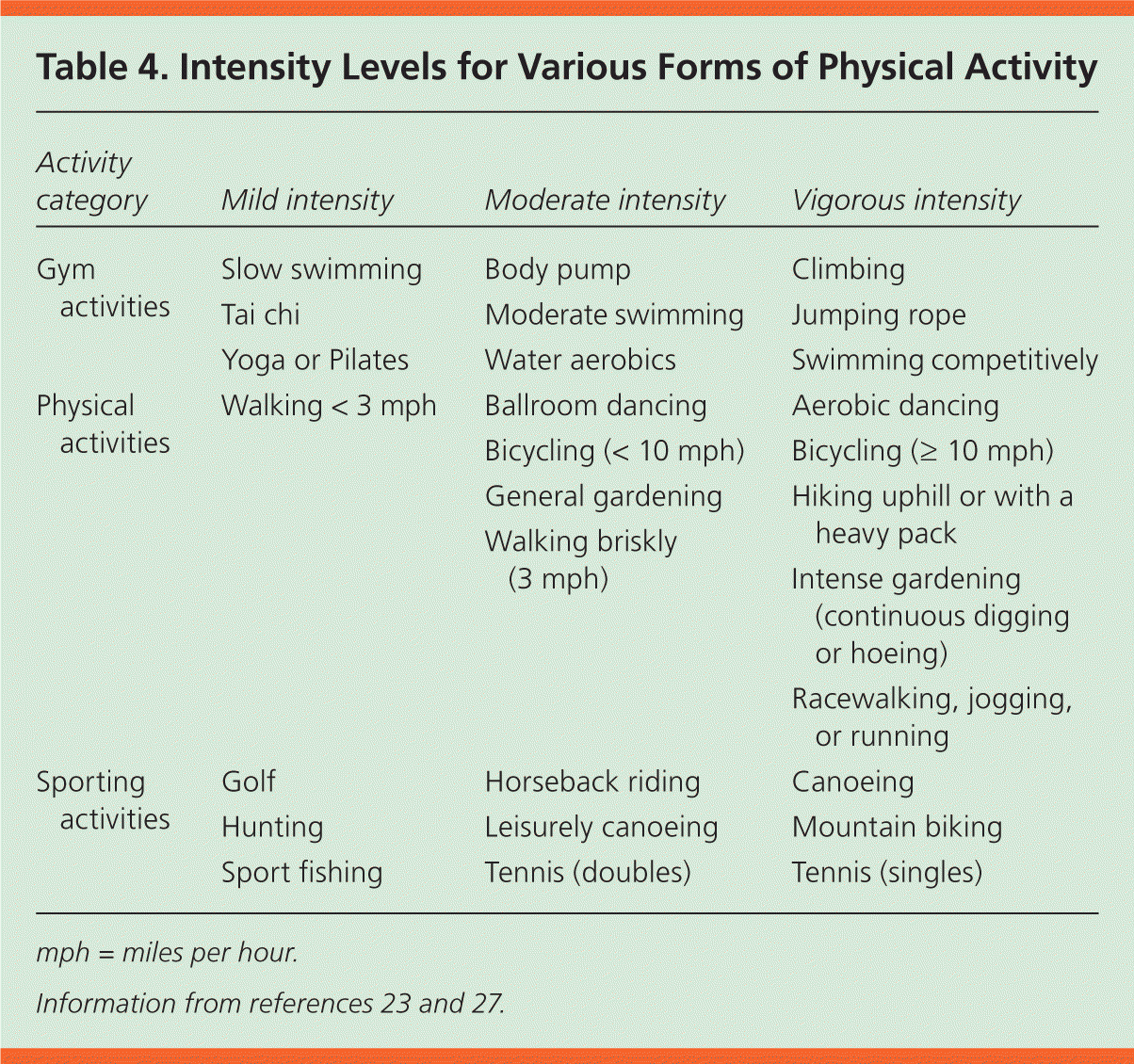
| Activity category | Mild intensity | Moderate intensity | Vigorous intensity |
|---|---|---|---|
| Gym activities | Slow swimming | Body pump | Climbing |
| Tai chi | Moderate swimming | Jumping rope | |
| Yoga or Pilates | Water aerobics | Swimming competitively | |
| Physical activities | Walking < 3 mph | Ballroom dancing | Aerobic dancing |
| Bicycling (< 10 mph) | Bicycling (≥ 10 mph) | ||
| General gardening | Hiking uphill or with a heavy pack | ||
| Walking briskly (3 mph) | Intense gardening (continuous digging or hoeing) | ||
| Racewalking, jogging, or running | |||
| Sporting activities | Golf | Horseback riding | Canoeing |
| Hunting | Leisurely canoeing | Mountain biking | |
| Sport fishing | Tennis (doubles) | Tennis (singles) |
mph = miles per hour.
Putting It Together
Research on the effect of combined dietary and physical activity interventions on cardiovascular events suggests that there may be more benefit than with either intervention alone. A 2014 population-based cohort study of Swedish men 45 to 79 years of age followed for 12 years showed that the combination of high-quality diet (the highest quintile of adherence to a diet high in fruits and vegetables, legumes, nuts, reduced-fat dairy products, whole grains, and fish) and physically active lifestyle (at least 40 minutes of walking or biking per day and one hour of additional physical activity per week), when added to moderate alcohol consumption and tobacco cessation, was associated with a reduced risk of MI (RR = 0.24; 95% CI, 0.12 to 0.47) compared with those who adopted none of the healthy lifestyle behaviors.31
The U.S. Preventive Services Task Force (USPSTF) currently recommends that physicians consider initiating behavioral counseling in adults without preexisting CVD or CVD risk factors to promote adherence to a healthy diet and physical activity on an individual basis. In addition to CVD risk, they should consider other factors, such as a patient's readiness to change, social support, and community resources that can provide support. The USPSTF did not find high-quality evidence that behavioral counseling interventions in adults at average risk of CVD reduces CVD events or mortality.32 The USPSTF is currently in the process of updating this recommendation.
Benefits of counseling interventions may be more pronounced in groups at higher cardiovascular risk. A 2011 Cochrane review of 55 RCTs reporting on pooled data for multiple counseling and educational methods showed no effect on primary prevention of all-cause or cardiovascular mortality or cardiovascular events. However, all-cause mortality was reduced when including only studies recruiting patients with diabetes or hypertension (RR = 0.78) or in patients taking antihypertensives or lipid-lowering therapy at baseline (RR = 0.86).33 Specific counseling strategies promoting dietary compliance and increased physical activity were not recommended based on this review.
The USPSTF found four good-quality trials involving more than 3,900 patients with cardiovascular risk factors that evaluated combined lifestyle-counseling interventions promoting healthy diet and physical activity. None of the trials showed a reduction in mortality or cardiovascular events. One trial that did show benefit had high baseline rates of CVD and allowed for pharmacologic therapy in patients who did not respond to counseling.34 For adults who are overweight (body mass index greater than 25 kg per m2) or obese (body mass index greater than 30 kg per m2) with CVD risk factors (e.g., hypertension, dyslipidemia, impaired glucose tolerance, metabolic syndrome), the USPSTF recommends providing intensive behavioral health counseling to promote a healthy diet and physical activity or referring patients for such services. Effective counseling strategies have involved face-to-face sessions with information on diet and physical activity and behavioral change strategies, typically delivered by dietitians or health educators.35
Data Sources: We reviewed ClinicalKey, Contemporary Clinical Trials, EBSCO, Essential Evidence Plus, ProQuest Hospital Collection, and PubMed, searching for cohort studies, randomized controlled trials, meta-analyses, and systematic reviews. Search terms included sports medicine, cardiovascular disease diet treatment, cardiovascular disease exercise treatment, and prevention cardiovascular disease exercise. We searched updated clinical recommendations from the American Heart Association and the U.S. Preventive Services Task Force. We also performed bibliographic searches of practice recommendations to identify additional primary literature sources. Search dates: March 30 and December 15, 2014, and October 27, 2015.
The authors thank Mrs. O'Dell McGuire, MLIS, hospital librarian at Martin Army Community Hospital, for her assistance performing literature searches.
The opinions and assertions contained in this article are strictly those of the authors and are not to be construed as representing official policy of the U.S. Army, the Department of Defense, or the U.S. government.

