Summary of Recommendation and Evidence
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of screening for impaired visual acuity in older adults (Table 1). I statement.
See the Clinical Considerations for suggestions for practice regarding the I statement.
Table 1. Screening for Impaired Visual Acuity in Older Adults: Clinical Summary of the USPSTF Recommendation
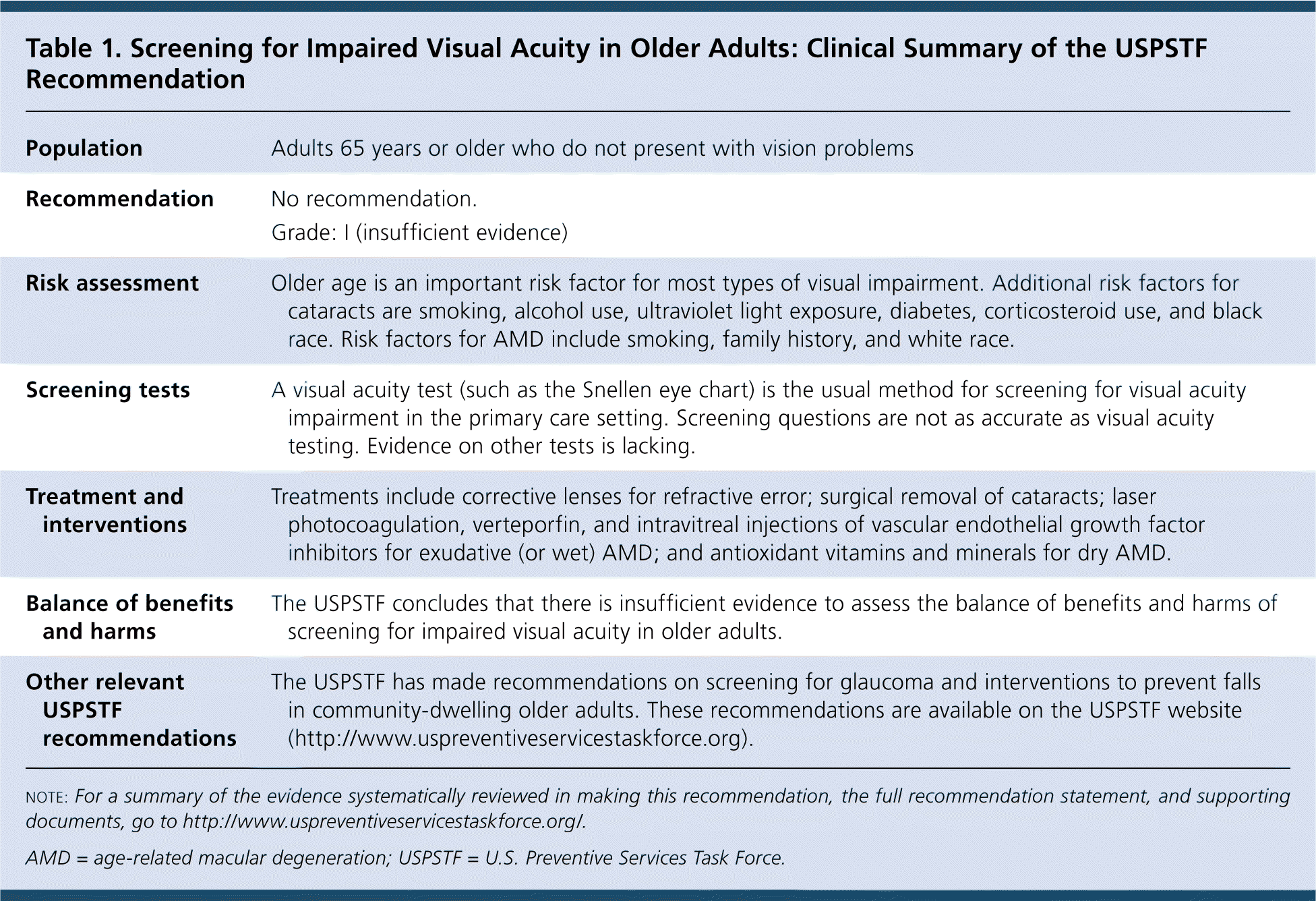
| Population | Adults 65 years or older who do not present with vision problems |
| Recommendation | No recommendation. |
| Grade: I (insufficient evidence) | |
| Risk assessment | Older age is an important risk factor for most types of visual impairment. Additional risk factors for cataracts are smoking, alcohol use, ultraviolet light exposure, diabetes, corticosteroid use, and black race. Risk factors for AMD include smoking, family history, and white race. |
| Screening tests | A visual acuity test (such as the Snellen eye chart) is the usual method for screening for visual acuity impairment in the primary care setting. Screening questions are not as accurate as visual acuity testing. Evidence on other tests is lacking. |
| Treatment and interventions | Treatments include corrective lenses for refractive error; surgical removal of cataracts; laser photocoagulation, verteporfin, and intravitreal injections of vascular endothelial growth factor inhibitors for exudative (or wet) AMD; and antioxidant vitamins and minerals for dry AMD. |
| Balance of benefits and harms | The USPSTF concludes that there is insufficient evidence to assess the balance of benefits and harms of screening for impaired visual acuity in older adults. |
| Other relevant USPSTF recommendations | The USPSTF has made recommendations on screening for glaucoma and interventions to prevent falls in community-dwelling older adults. These recommendations are available on the USPSTF website (http://www.uspreventiveservicestaskforce.org). |
note: For a summary of the evidence systematically reviewed in making this recommendation, the full recommendation statement, and supporting documents, go to http://www.uspreventiveservicestaskforce.org/.
AMD = age-related macular degeneration; USPSTF = U.S. Preventive Services Task Force.
Rationale
IMPORTANCE
Impairment of visual acuity is a serious public health problem in older adults. In 2011, about 12% of U.S. adults aged 65 to 74 years and 15% of those 75 years or older reported having problems seeing, even with glasses or contact lenses.
DETECTION
The USPSTF found convincing evidence that screening with a visual acuity test can identify persons with a refractive error. The USPSTF found convincing evidence that screening questions are not as accurate as visual acuity testing for assessing visual acuity. The USPSTF found adequate evidence that visual acuity testing alone does not accurately identify early age-related macular degeneration (AMD) or cataracts.
BENEFITS OF DETECTION AND EARLY TREATMENT
The USPSTF found inadequate overall evidence on the benefits of screening, early detection, and treatment to provide a coherent assessment of the overall benefits. Several studies evaluated the direct benefit of screening and reported no reductions in vision disorders or vision-related function in screened populations; however, these studies had limitations, including differing control interventions, high loss to follow-up, and low uptake of treatment. The USPSTF found adequate evidence that early treatment of refractive error, cataracts, and AMD improves or prevents loss of visual acuity.
HARMS OF DETECTION AND EARLY TREATMENT
The USPSTF found inadequate evidence on the harms of screening. The USPSTF found adequate evidence that early treatment of refractive error, cataracts, and AMD may lead to harms that are small to none.
USPSTF ASSESSMENT
The USPSTF concludes that the evidence is insufficient to assess the balance of benefits and harms of screening for impaired visual acuity in older adults. The evidence is lacking to provide a coherent assessment, and the balance of benefits and harms cannot be determined.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to asymptomatic adults 65 years or older who do not present to their primary care clinician with vision problems.
SUGGESTIONS FOR PRACTICE REGARDING THE I STATEMENT
Potential Preventable Burden. In 2011, about 12% of U.S. adults aged 65 to 74 years and 15% of those 75 years or older reported having problems seeing, even with glasses or contact lenses.1 The prevalence of AMD is 6.5% in adults older than 40 years and increases with age (2.8% in those aged 40 to 59 years and 13.4% in those aged ≥ 60 years).2 About half of all cases of bilateral low vision (i.e., best-corrected visual acuity of < 20/40) in adults 40 years and older are caused by cataracts. The prevalence of cataracts increases sharply with age; an estimated 50% of U.S. adults 80 years or older have cataracts.1 The prevalence of hyperopia requiring a correction of +3.0 diopters or more ranges from about 5.9% in U.S. adults aged 50 to 54 years, to 15.2% in adults aged 65 to 69 years, to 20.4% in adults 80 years or older.1
Older age is an important risk factor for most types of visual impairment. Additional risk factors for cataracts are smoking, alcohol use, ultraviolet light exposure, diabetes, corticosteroid use, and black race. Risk factors for AMD include smoking, family history, and white race.1
Potential Harms. The harms of screening in a primary care setting have not been adequately studied. Overall, the potential for harms from treatment are small to none. Harms of treatment of refractive error include a potential for increased falls with the use of multifocal lenses; infectious keratitis with the use of contact lenses, laser-assisted in situ keratomileusis (LASIK), or laser-assisted subepithelial keratectomy (LASEK); and corneal ectasia with LASIK. Harms of cataract surgery include posterior lens opacification and endophthalmitis. Treatment of AMD with antioxidant vitamins and mineral supplements is not associated with increased risk of most serious adverse events.
Although there appears to be benefit in longer-term outcomes, a systematic review found that treatment of AMD with laser photocoagulation was associated with greater risk of acute loss of 6 or more lines of visual acuity vs. no treatment at 3 months (relative risk [RR] = 1.41 [95% CI, 1.08 to 1.82]).3 Pooled estimates report a non–statistically significant association between photodynamic therapy and risk of acute loss of 20 or more letters of visual acuity vs. placebo at 7 days (RR = 3.75 [95% CI, 0.87 to 16]; 3 trials).4,5 One of 2 trials found that treatment of wet AMD with intravitreal vascular endothelial growth factor (VEGF) inhibitor therapy was associated with greater likelihood of withdrawal vs. sham therapy; there were no differences in serious or other adverse events, but estimates were imprecise.1,4,6,7
Current Practice. About half of U.S. adults older than 65 years reported having an eye examination within the last 12 months in a 2007 study.8
SCREENING TESTS
A visual acuity test (e.g., the Snellen eye chart) is the usual method for screening for visual acuity impairment in the primary care setting. Screening questions are not as accurate as visual acuity testing for identifying visual acuity impairment. Evidence on the use of other tests for vision screening in primary care, such as the pinhole test (a test for refractive error), the Amsler grid (a test of central vision to detect AMD), genetic testing, or funduscopy (visual inspection of the interior of the eye), is lacking.
TREATMENT
Several types of treatment are effective for improving visual acuity. Corrective lenses improve visual acuity in patients with a refractive error. Treatment of cataracts through surgical removal of the cataract is effective for improving visual acuity. Treatment of exudative (or wet) AMD includes laser photocoagulation, verteporfin, and intravitreal injections of VEGF inhibitors. Antioxidant vitamins and minerals are an effective treatment for dry AMD.
OTHER APPROACHES TO PREVENTION
This recommendation statement does not include screening for glaucoma. The USPSTF's recommendations on screening for glaucoma and falls prevention are available on its website (http://www.uspreventiveservicestaskforce.org).
This recommendation statement was first published in JAMA. 2016;315(9):908–914.
The “Other Considerations,” “Discussion,” “Update of Previous USPSTF Recommendation,” and “Recommendations of Others” sections of this recommendation statement are available at http://www.uspreventiveservicestaskforce.org/Page/Document/UpdateSummaryFinal/impaired-visual-acuity-in-older-adults-screening.
The USPSTF recommendations are independent of the U.S. government. They do not represent the views of the Agency for Healthcare Research and Quality, the U.S. Department of Health and Human Services, or the U.S. Public Health Service.

