Cardiac rehabilitation is a comprehensive multidisciplinary program individually tailored to the needs of patients with cardiovascular disease. The overall goals focus on improving daily function and reducing cardiovascular risk factors. Cardiac rehabilitation includes interventions aimed at lowering blood pressure and improving lipid and diabetes mellitus control, with tobacco cessation, behavioral counseling, and graded physical activity. The physical activity component typically involves 36 sessions over 12 weeks, during which patients participate in supervised exercise under cardiac monitoring. There are also intensive programs that include up to 72 sessions lasting up to 18 weeks, although these programs are not widely available. Additional components of cardiac rehabilitation include counseling on nutrition, screening for and managing depression, and assuring up-to-date immunizations. Cardiac rehabilitation is covered by Medicare and recommended for patients following myocardial infarction, bypass surgery, and stent placement, and for patients with heart failure, stable angina, and several other conditions. Despite proven benefits in mortality rates, depression, functional capacity, and medication adherence, rates of referral for cardiac rehabilitation are suboptimal. Groups less likely to be referred are older adults, women, patients who do not speak English, and persons living in areas where cardiac rehabilitation is not locally available. Additionally, primary care physicians refer patients less often than cardiologists and cardiothoracic surgeons.
Cardiac rehabilitation was initially developed in the 1950s. Through the 1970s, programs consisted mainly of structured exercise after myocardial infarction (MI). In 1995, the U.S. Department of Health and Human Services published a clinical practice guideline on cardiac rehabilitation, which prompted a transition from an exercise program to a holistic combination of exercise training, lifestyle modification, and behavioral therapy.1
WHAT IS NEW ON THIS TOPIC: CARDIAC REHABILITATION
Home-based exercise programs result in clinical improvements that are at least comparable with those from center-based programs. Home-based cardiac rehabilitation participants also had improved adherence to program recommendations.
In a study of patients with heart failure undergoing cardiac rehabilitation, completion of an exercise training program was associated with a 40% decrease in the presence of depression. Only small improvements in functional capacity appear to be needed to decrease depression.
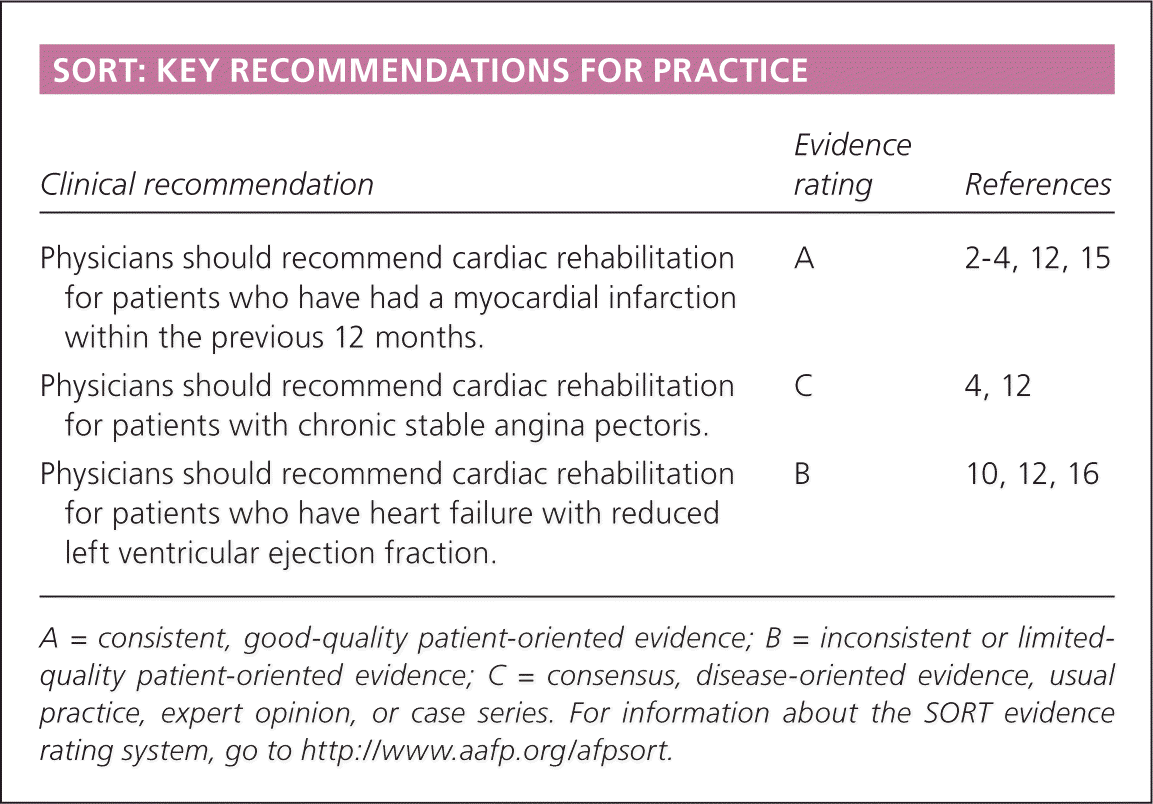
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Physicians should recommend cardiac rehabilitation for patients who have had a myocardial infarction within the previous 12 months. | A | 2–4, 12, 15 |
| Physicians should recommend cardiac rehabilitation for patients with chronic stable angina pectoris. | C | 4, 12 |
| Physicians should recommend cardiac rehabilitation for patients who have heart failure with reduced left ventricular ejection fraction. | B | 10, 12, 16 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
What Is Cardiac Rehabilitation?
Cardiac rehabilitation is a comprehensive multidisciplinary approach to care that is systematically applied and individually tailored to the needs of patients with cardiovascular disease (CVD). The American Association of Cardiovascular and Pulmonary Rehabilitation and the American Heart Association (AHA) emphasize that cardiac rehabilitation is designed to optimize physical, psychological, vocational, and social functioning while slowing or reversing the CVD process.2,3 Standard of care for cardiac rehabilitation programs includes requirements for a medical director and an on-site emergency response team.4
Cardiac rehabilitation typically begins in an inpatient setting, followed by outpatient sessions after discharge. Components typically include an exercise program, nutrition counseling, behavioral counseling, immunizations, and smoking cessation programs, as well as medical care aimed at controlling blood pressure, lipid levels, and diabetes mellitus. Several of these components are discussed in this article. Programs also focus on adherence to appropriate medication regimens.2,3
ASSESSMENT
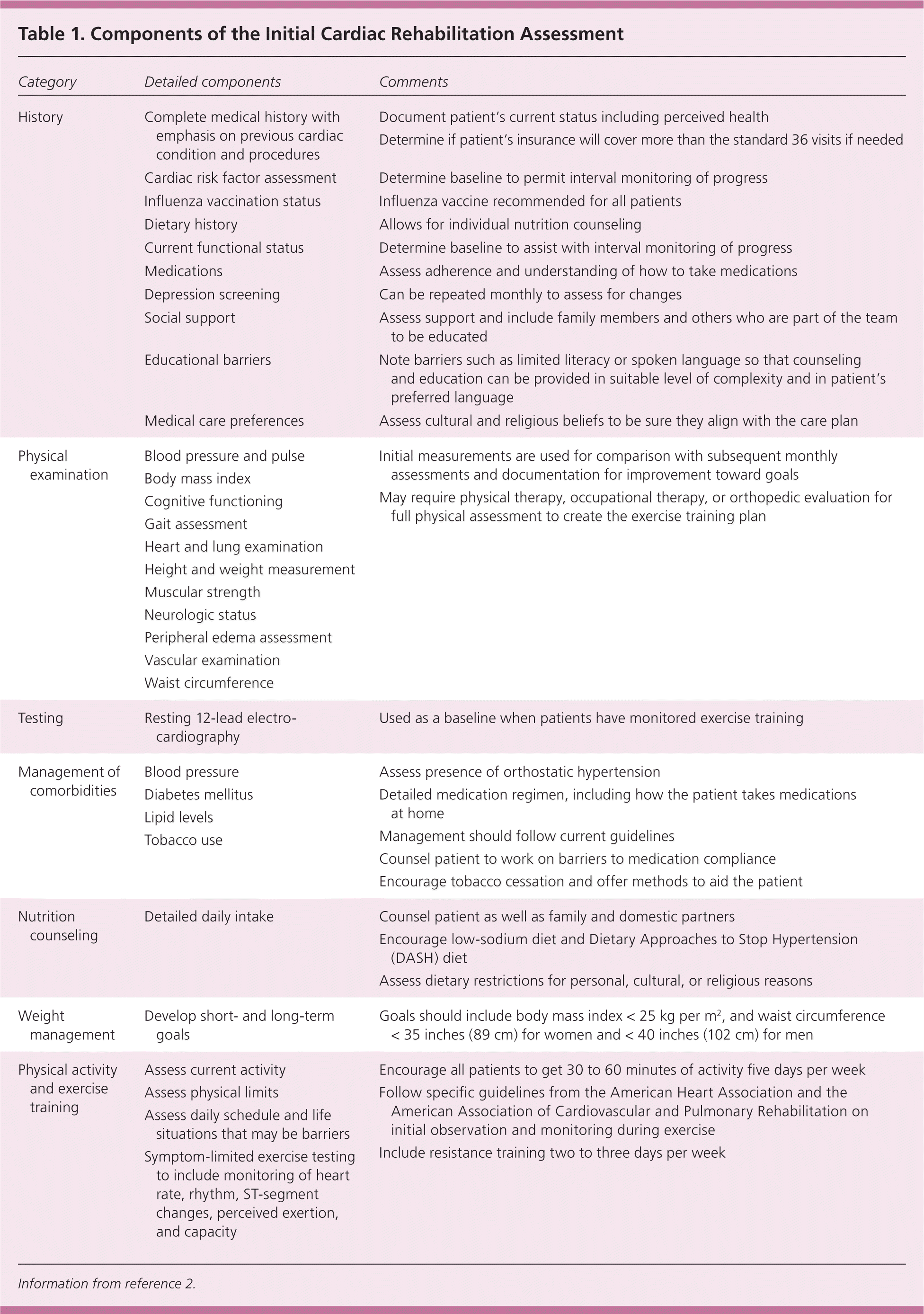
The first step in cardiac rehabilitation is an initial assessment, with subsequent assessments typically performed monthly.2,4,5 These assessments are completed by a team of professionals who evaluate a patient's symptoms, lifestyle habits (e.g., diet, exercise, tobacco use), comorbidities, and other parameters4,5 (Table 12 ).
Table 1. Components of the Initial Cardiac Rehabilitation Assessment
| Category | Detailed components | Comments |
|---|---|---|
| History | Complete medical history with emphasis on previous cardiac condition and procedures | Document patient's current status including perceived health |
| Determine if patient's insurance will cover more than the standard 36 visits if needed | ||
| Cardiac risk factor assessment | Determine baseline to permit interval monitoring of progress | |
| Influenza vaccination status | Influenza vaccine recommended for all patients | |
| Dietary history | Allows for individual nutrition counseling | |
| Current functional status | Determine baseline to assist with interval monitoring of progress | |
| Medications | Assess adherence and understanding of how to take medications | |
| Depression screening | Can be repeated monthly to assess for changes | |
| Social support | Assess support and include family members and others who are part of the team to be educated | |
| Educational barriers | Note barriers such as limited literacy or spoken language so that counseling and education can be provided in suitable level of complexity and in patient's preferred language | |
| Medical care preferences | Assess cultural and religious beliefs to be sure they align with the care plan | |
| Physical examination | Blood pressure and pulse | Initial measurements are used for comparison with subsequent monthly assessments and documentation for improvement toward goals |
| Body mass index | May require physical therapy, occupational therapy, or orthopedic evaluation for full physical assessment to create the exercise training plan | |
| Cognitive functioning | ||
| Gait assessment | ||
| Heart and lung examination | ||
| Height and weight measurement | ||
| Muscular strength | ||
| Neurologic status | ||
| Peripheral edema assessment | ||
| Vascular examination | ||
| Waist circumference | ||
| Testing | Resting 12-lead electrocardiography | Used as a baseline when patients have monitored exercise training |
| Management of comorbidities | Blood pressure | Assess presence of orthostatic hypertension |
| Diabetes mellitus | Detailed medication regimen, including how the patient takes medications at home | |
| Lipid levels | Management should follow current guidelines | |
| Tobacco use | Counsel patient to work on barriers to medication compliance | |
| Encourage tobacco cessation and offer methods to aid the patient | ||
| Nutrition counseling | Detailed daily intake | Counsel patient as well as family and domestic partners |
| Encourage low-sodium diet and Dietary Approaches to Stop Hypertension (DASH) diet | ||
| Assess dietary restrictions for personal, cultural, or religious reasons | ||
| Weight management | Develop short- and long-term goals | Goals should include body mass index < 25 kg per m2, and waist circumference < 35 inches (89 cm) for women and < 40 inches (102 cm) for men |
| Physical activity and exercise training | Assess current activity | Encourage all patients to get 30 to 60 minutes of activity five days per week |
| Assess physical limits | Follow specific guidelines from the American Heart Association and the American Association of Cardiovascular and Pulmonary Rehabilitation on initial observation and monitoring during exercise | |
| Assess daily schedule and life situations that may be barriers | ||
| Symptom-limited exercise testing to include monitoring of heart rate, rhythm, ST-segment changes, perceived exertion, and capacity | Include resistance training two to three days per week |
Information from reference 2.
EXERCISE PROGRAM
The exercise training program is typically a 36-session supervised program lasting 12 weeks. The sessions are led by a trained nurse, physical therapist, exercise physiologist, or physician, and are typically conducted with the patient under continuous cardiac monitoring. Exercise training sessions occur one to three times per week, depending on a patient's individual functional capabilities, with the goal being 30 minutes of moderate aerobic exercise occurring five days per week.4,5
NUTRITION EDUCATION
During cardiac rehabilitation sessions, patients meet for intensive education about nutrition. Besides counseling on appropriate diet, sessions on cooking and grocery shopping with the patient's family may be included.
BEHAVIORAL COUNSELING
There is a high prevalence of depression among patients with CVD,6 and research has shown that depression increases the mortality risk in these patients.7,8 As a result, cardiac rehabilitation programs have added behavioral health specialists to help patients manage the psychosocial aspects of CVD, including sexual health, mood disorders, and fear of recurrence.2,4,5
IMMUNIZATIONS
Assuring appropriate immunizations is another component of cardiac rehabilitation. Specifically, the Advisory Council on Immunization Practices recommends annual influenza vaccination for patients with CVD.9
What Are Intensive Programs?
In addition to the standard programs, there are intensive cardiac rehabilitation programs that include up to 72 sessions and can last up to 18 weeks.5,10 However, intensive programs are not widely available. Programs that involve 12 to 36 sessions and last 12 to 52 months have demonstrated benefits, including better lipid and blood pressure control, improved medication adherence, decreased depression, reduced emotional stress, and enhanced exercise tolerance.5
Who Is Eligible for Cardiac Rehabilitation?
The AHA gives cardiac rehabilitation a class-1 recommendation for patients with a number of cardiovascular disorders4,11,12 (Table 24,11–14 ). Cardiac rehabilitation is recommended for patients following MI, bypass surgery, and stent placement beginning in an inpatient setting. It is also recommended for outpatients with MI in the previous 12 months,2–4,12,15 chronic stable angina pectoris,4,12 and heart failure with reduced left ventricular ejection fraction.10,12,16 The AHA and European guidelines also include patients who have pacemakers or implantable cardioverter-defibrillator devices as possibly benefiting from rehabilitation.13,17
Table 2. AHA Recommendations for Cardiac Rehabilitation

| AHA class-1 recommendation and covered by Medicare |
| Coronary artery bypass surgery |
| Coronary revascularization via percutaneous intervention |
| Current stable angina pectoris |
| Heart or heart-lung transplantation |
| Heart valve repair or replacement |
| Myocardial infarction in the previous 12 months |
| Recent cerebrovascular accident (women only) |
| Stable chronic heart failure with reduced left ventricular ejection fraction |
| Recommended by AHA but not class 1 or covered by Medicare |
| Implantable cardioverter-defibrillator |
| Pacemaker |
AHA = American Heart Association.
Recent performance measures state that patients should begin cardiac rehabilitation immediately after an inpatient stay for any of the conditions with class-1 recommendations. If not hospitalized, patients should be referred for rehabilitation by their outpatient physician within 12 months of the applicable diagnoses or procedures.12 The only patients who are not considered candidates for rehabilitation are those with a medically unstable, life-threatening condition or those who do not have a program available within 60 minutes of their home.12
Is Cardiac Rehabilitation Covered by Medicare?
Medicare guidelines cover standard and intensive cardiac rehabilitation. However, to be eligible for Medicare coverage, programs must include physician-prescribed exercise, cardiac risk factor modification, a psychosocial assessment of mental and emotional functioning, an outcomes assessment, and an individualized treatment plan reviewed and signed by a physician every 30 days.10
Medicare coverage of standard cardiac rehabilitation includes a maximum of two one-hour sessions per day, covering up to 36 total sessions, with the option to renew for an additional 36 sessions when deemed to be medically necessary. Coverage for intensive cardiac rehabilitation is limited to 72 one-hour sessions (up to six sessions per week) for up to 18 weeks.10 There are only three types of intensive cardiac rehabilitation approved by Medicare: Dr. Dean Ornish Program for Reversing Heart Disease, Pritikin Intensive Cardiac Rehab program, and Benson-Henry Institute Cardiac Wellness Program.14 It is important to note that these programs are not widely available; locations can be found by searching program websites.
Benefits of Cardiac Rehabilitation
The benefits of cardiac rehabilitation have been repeatedly demonstrated over the past three decades, and include reduction in cardiovascular risk, enhanced emotional well-being, and improvement in several other outcomes.
REDUCED CARDIOVASCULAR RISK
In a study of more than 600,000 Medicare beneficiaries hospitalized for acute coronary syndromes, stable ischemic heart disease, or revascularization procedures, there was a reduction in mortality rates among patients attending cardiac rehabilitation programs vs. those not attending. Patients were compared based on the number of sessions attended (one to 24 sessions vs. 25 sessions or more). At one year and five years, the mortality rates were lower for those who attended 25 or more cardiac rehabilitation sessions (2.2% vs. 5.3% at one year, and 16.3% vs. 24.6% at five years). Additionally, among patients attending 25 or more sessions, subgroup analyses showed that women, nonwhites, and older adults had greater benefit.18
Another study further defined the inverse relationship between number of sessions attended and mortality. Compared with patients who attended 12 to 24 sessions, patients who attended all 36 exercise training sessions had decreased risks of death (14% vs. 22%) and MI (12% vs. 23%) over the four-year study.19 Another study found reductions in cardiac-specific and all-cause mortality rates among patients participating in cardiac rehabilitation after percutaneous coronary interventions.20
IMPROVEMENTS IN DEPRESSION
A 2007 study examining the effect of cardiac rehabilitation on depression compared 522 patients who completed a rehabilitation program with 179 patients who dropped out within two weeks of program entry. Using a 92-question validated questionnaire, the rate of depression decreased from 17% at entry into cardiac rehabilitation to 6% after completion. Data on mortality rates were available for both groups after follow-up for an average of 3.5 years. Patients with depression who completed rehabilitation had a lower mortality rate than those who did not complete the program (8% vs. 30%).21
In a more recent study on exercise training and depression in patients with heart failure, completion of the exercise training program was associated with a 40% decrease in the presence of depression.16 Improvements in depression were most notable among those who experienced an improvement in functional capacity, but only small improvements in functional capacity were needed to decrease depression.
OTHER BENEFITS
Cardiac rehabilitation has been shown to increase functional capacity as measured by exercise tolerance and peak oxygen consumption.15 Other parameters that demonstrate improvement include weight loss, lipid control, and management of comorbidities.22 It is not possible, however, to definitively attribute these improvements to cardiac rehabilitation because conditions such as diabetes, hypertension, and hyperlipidemia may be managed pharmacologically by a primary care physician outside of the rehabilitation program.
A recent Cochrane review of 63 studies demonstrated a reduction in hospital admissions and increases in overall quality of life with cardiac rehabilitation. Although it showed a reduction in overall mortality, as in previous studies, there was no reduction in MI or revascularization rates.23
Underutilization and Disparities
PATIENT DEMOGRAPHIC FACTORS
Despite the known benefits of cardiac rehabilitation, there continue to be disparities in referral and participation rates. Research indicates that being a non–English speaker is the strongest predictor of not receiving a referral for cardiac rehabilitation, with English speakers almost 10 times more likely to be referred (relative risk = 9.56; 95% confidence interval, 2.5 to 42).24
Older adults also have a lower rate of referral. Older age should not preclude participation in cardiac rehabilitation; patients in this age group experience benefits from these programs. In particular, research demonstrates improvements in exercise capacity and quality of life, as well as a reduction in overall mortality rates.25–27
A recent systematic review also demonstrated a significant difference in referral rates based on sex, with 45% of men vs. 38.5% of women being referred for cardiac rehabilitation.28 Individuals of lower socioeconomic status are also less likely to participate because of less flexible work schedules, less health insurance coverage, and less education.29
Individuals living in rural areas are less likely to participate in cardiac rehabilitation, even if they are referred to a program. One study of 254 rural residents referred for cardiac rehabilitation found that only 28% attended any part of the program and only 17% completed a full 36-week program. Distance from home was the most common reason cited for not completing the program.30
SYSTEM, CLINICAL, AND PHYSICIAN FACTORS
Physician and system factors also contribute to below-optimal rates of referral for cardiac rehabilitation. A key system-related factor is whether the hospital to which a patient is admitted has an existing cardiac rehabilitation program.24
A key clinical factor for participation in rehabilitation is the patient's underlying cardiac condition. A study conducted at 56 hospitals that discharged 172,817 patients after MI, percutaneous intervention, or bypass surgery found that only 56% of patients who were candidates for cardiac rehabilitation were actually referred to a program. Despite evidence that cardiac rehabilitation is of benefit in all three conditions, patients were more likely to be referred if they had undergone bypass surgery (74% referral rate) than if they underwent percutaneous intervention (58%) or had an MI without those interventions (53%).31
Physician specialty also influences referral rates. Cardiologists and cardiothoracic surgeons refer eligible patients to cardiac rehabilitation more often than do primary care physicians.32
Other factors influencing referral rates include lack of knowledge of programs in the area, lack of understanding of the benefits of cardiac rehabilitation, lack of standardized referral forms, inconvenience, and perceived poor program quality.33 Nonetheless, patient participation in cardiac rehabilitation is improved when recommended by a physician and if specific oral and written information is given with additional phone follow-up.34,35 Physicians can identify resources in their community at https://www.aacvpr.org/Resources/Program-Directory, and find an information sheet at https://www.aacvpr.org/Portals/0/Resources/CR%20Fact%20Sheet%201.12.doc. They can also refer patients to information from the AHA at http://www.heart.org/HEARTORG/Conditions/More/CardiacRehab/What-is-Cardiac-Rehabilitation_UCM_307049_Article.jsp or the National Heart, Lung, and Blood Institute at http://www.nhlbi.nih.gov/health/health-topics/topics/rehab.
New Approaches
Other cardiac rehabilitation program formats have been proposed and are being studied. Home-based programs could potentially improve participation and outcomes, especially for patients living far from supervised programs. Multiple small studies suggest that home-based exercise programs result in clinical improvements that are comparable with outcomes from center-based programs.35–37 A Cochrane review of home-based rehabilitation vs. rehabilitation in specialized centers showed that all outcomes, including exercise capacity, systolic blood pressure, lipoprotein levels, and mortality rates, were equivalent. Participants in home-based cardiac rehabilitation also had improved adherence to program recommendations.38 The authors suggest that expansion of standardized home-based cardiac rehabilitation may bridge the gap in the availability for all eligible patients.
Telephone support and other social media support for patients in cardiac rehabilitation programs are new areas of interest. One systematic review showed fewer hospitalizations, improved tobacco cessation rates, lower depression scores, lower anxiety scores, and a lower systolic blood pressure in a group receiving telephone support.39 Computer mentoring and mobile texting support are being studied as ways to support patients in cardiac rehabilitation.40
Data Sources: A PubMed search was completed in Clinical Queries using the key terms cardiac rehabilitations, components, indications, and benefits. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. Databases searched include the Cochrane database, the National Guideline Clearinghouse database, and DynaMed. Search dates: April 2014, June 2015, and March 2016.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the Uniformed Services University of the Health Sciences, the U.S. Air Force, or the Department of Defense.

