Summary of Recommendation and Evidence
The USPSTF recommends against screening for chronic obstructive pulmonary disease (COPD) in asymptomatic adults (Table 1). D recommendation.
Table 1. Screening for Chronic Obstructive Pulmonary Disease: Clinical Summary of the USPSTF Recommendation
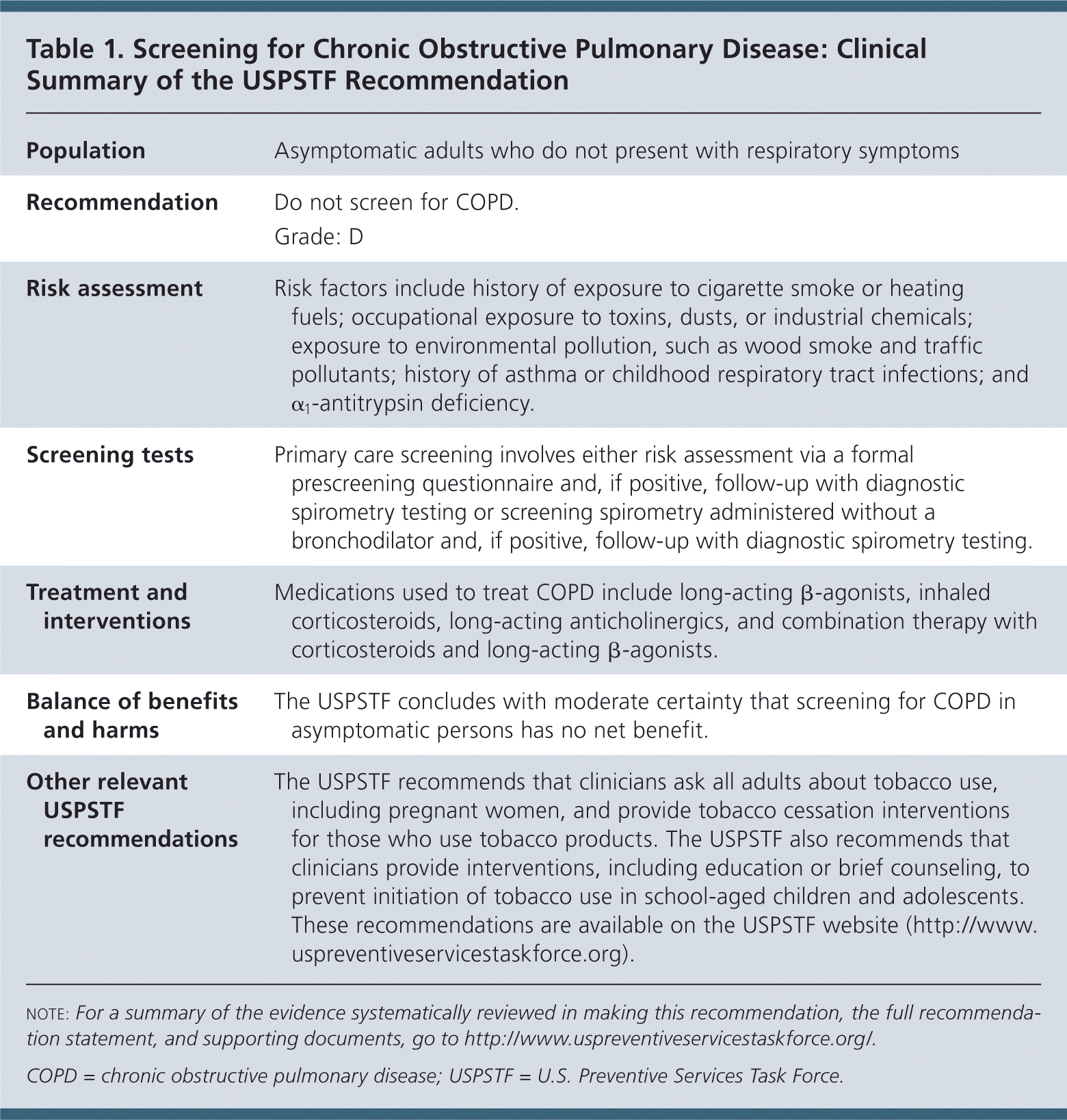
| Population | Asymptomatic adults who do not present with respiratory symptoms |
| Recommendation | Do not screen for COPD. |
| Grade: D | |
| Risk assessment | Risk factors include history of exposure to cigarette smoke or heating fuels; occupational exposure to toxins, dusts, or industrial chemicals; exposure to environmental pollution, such as wood smoke and traffic pollutants; history of asthma or childhood respiratory tract infections; and α1-antitrypsin deficiency. |
| Screening tests | Primary care screening involves either risk assessment via a formal prescreening questionnaire and, if positive, follow-up with diagnostic spirometry testing or screening spirometry administered without a bronchodilator and, if positive, follow-up with diagnostic spirometry testing. |
| Treatment and interventions | Medications used to treat COPD include long-acting β-agonists, inhaled corticosteroids, long-acting anticholinergics, and combination therapy with corticosteroids and long-acting β-agonists. |
| Balance of benefits and harms | The USPSTF concludes with moderate certainty that screening for COPD in asymptomatic persons has no net benefit. |
| Other relevant USPSTF recommendations | The USPSTF recommends that clinicians ask all adults about tobacco use, including pregnant women, and provide tobacco cessation interventions for those who use tobacco products. The USPSTF also recommends that clinicians provide interventions, including education or brief counseling, to prevent initiation of tobacco use in school-aged children and adolescents. These recommendations are available on the USPSTF website ( http://www.uspreventiveservicestaskforce.org). |
note: For a summary of the evidence systematically reviewed in making this recommendation, the full recommendation statement, and supporting documents, go to http://www.uspreventiveservicestaskforce.org/.
COPD = chronic obstructive pulmonary disease; USPSTF = U.S. Preventive Services Task Force.
Rationale
IMPORTANCE
About 14% of U.S. adults aged 40 to 79 years have COPD, and it is the third leading cause of death in the United States.1,2 Persons with severe COPD are often unable to participate in normal physical activity due to deterioration of lung function.
DETECTION
COPD is defined as airflow limitation that is not fully reversible. COPD is associated with an abnormal inflammatory response of the lung to harmful particles or gases. Diagnosis is based on postbronchodilator spirometry, which detects fixed airway obstruction; a forced expiratory volume in 1 second to forced vital capacity (FEV1/FVC) ratio of less than 0.70 is the current criterion for a positive COPD diagnosis. Persons with COPD often, but not always, have symptoms such as dyspnea (difficulty breathing or shortness of breath), chronic cough, and chronic sputum production. Patients often have a history of exposure to risk factors such as cigarette smoke or heating fuels or occupational exposure to dusts or chemicals. Although postbronchodilator spirometry is required to make a definitive diagnosis, prescreening questionnaires can elicit current symptoms and previous exposures to harmful particles or gases.
BENEFITS OF DETECTION AND EARLY TREATMENT
The USPSTF found inadequate evidence that screening for COPD in asymptomatic persons using questionnaires or spirometry improves health outcomes.
HARMS OF DETECTION AND EARLY TREATMENT
The USPSTF found inadequate evidence on the harms of screening. However, given the lack of benefit of early detection and treatment, the opportunity cost associated with screening asymptomatic persons may be large. The amount of time and effort required to screen for COPD in asymptomatic persons (using screening spirometry with or without prescreening questionnaires) is not trivial.
USPSTF ASSESSMENT
The USPSTF determined that early detection of COPD, before the development of symptoms, does not alter the course of the disease or improve patient outcomes. The USPSTF concludes with moderate certainty that screening for COPD in asymptomatic persons has no net benefit. Thus, screening is not recommended in persons who do not have symptoms suggestive of COPD. The USPSTF recommends against screening for COPD in asymptomatic adults.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation statement applies to asymptomatic adults who do not recognize or report respiratory symptoms. It does not apply to at-risk persons who present to clinicians with symptoms such as chronic cough, sputum production, dyspnea, or wheezing. It also does not apply to persons with a family history of α1-antitrypsin deficiency.
RISK ASSESSMENT
Exposure to cigarette smoke or toxic fumes increases the risk for COPD. Epidemiological studies have found that 15% to 50% of smokers develop COPD.3 More than 70% of all COPD cases occur in current or former smokers. Occupational exposure to toxins, dusts, or industrial chemicals contributes an estimated 15% of all COPD cases. Environmental pollution, including wood smoke and traffic pollutants, is also associated with increased risk for COPD. Nonmodifiable risk factors for COPD include history of asthma or childhood respiratory tract infections and α1-antitrypsin deficiency.
SCREENING TESTS
Screening adults in primary care involves either risk assessment via a formal prescreening questionnaire and, if positive, follow-up with diagnostic spirometry testing or screening spirometry administered without a bronchodilator and, if positive, follow-up with diagnostic spirometry testing. Patients identified as high risk by a prescreening questionnaire or screening spirometry are referred for diagnostic spirometry testing. Diagnosis by spirometry requires persistent airway obstruction after administration of an inhaled bronchodilator, such as albuterol (i.e., post-bronchodilator spirometry). COPD is diagnosed if the patient has a postbronchodilator FEV1/FVC ratio of less than 0.70. Severity is defined by the percentage of predicted post-bronchodilator FEV1; 80% or more is mild, 50% to 79% is moderate, 30% to 49% is severe, and less than 30% is very severe.
OTHER APPROACHES TO PREVENTION
Prevention of exposure to cigarette smoke and other toxic fumes is the best way to prevent COPD. Interventions to prevent the initiation of tobacco use are an effective way to prevent exposure to cigarette smoke. Current smokers should receive cessation counseling and be offered behavioral and pharmacological therapies to stop smoking.
USEFUL RESOURCES
The USPSTF recommends that clinicians ask all adults, including pregnant women, about tobacco use and provide tobacco cessation interventions for those who use tobacco products. The USPSTF also recommends that clinicians provide interventions, including education or brief counseling, to prevent initiation of tobacco use in school-aged children and adolescents. These recommendations and their supporting evidence are available on the USPSTF website ( http://www.uspreventiveservicestaskforce.org).

