A 43-year-old man presented with a one-week history of multiple weeping papules on his penis and scrotum. The lesions were not painful, and he had no other symptoms. He had no relevant medical history, including human immunodeficiency virus infection, but he had had unprotected sexual encounters with multiple women over the previous three months.
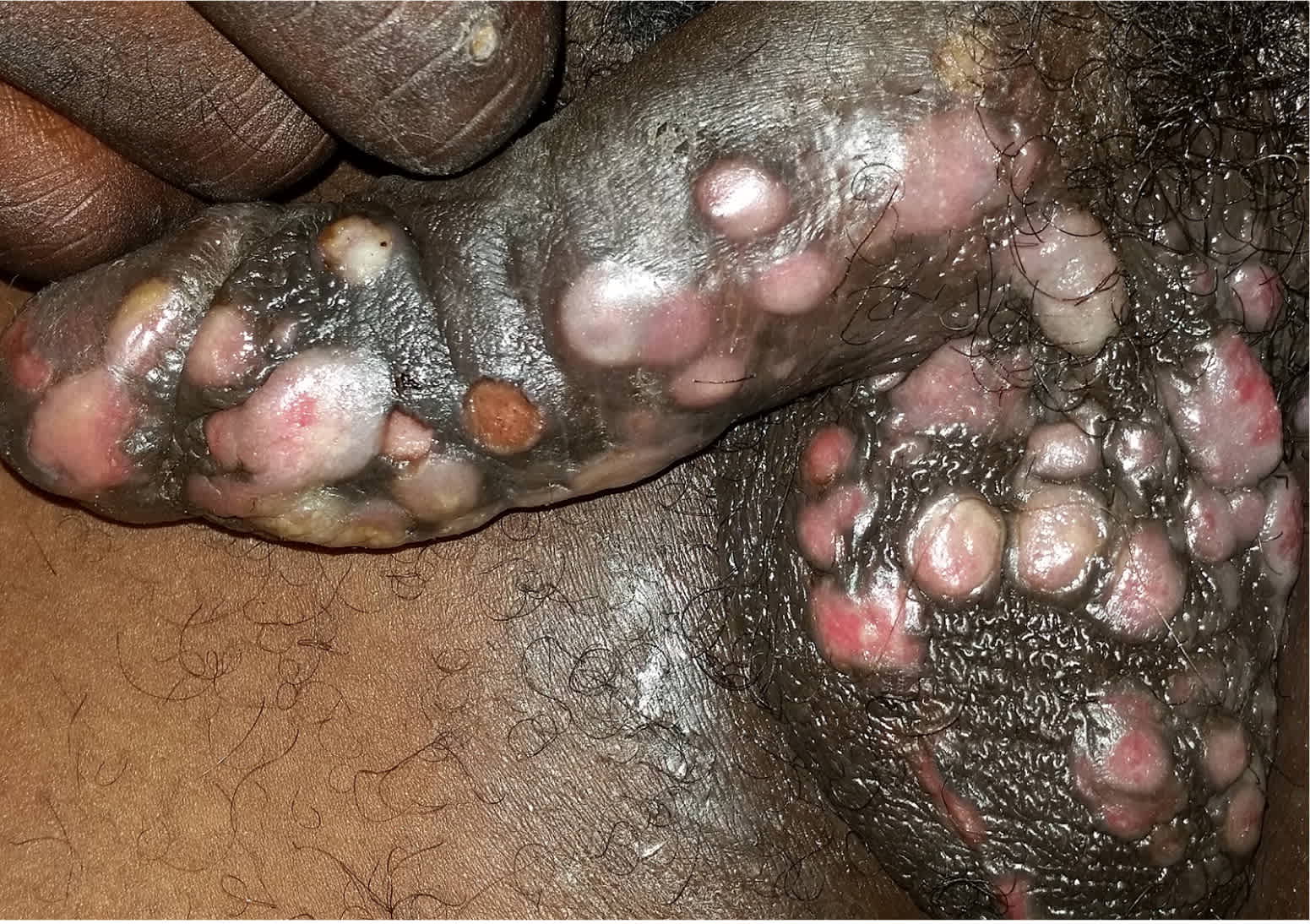
Physical examination revealed more than 50 firm, moist, pink papules on the scrotum and penile shaft (Figure 1). The lesions were nontender, smooth, and flat-topped. The patient had bilateral inguinal lymphadenopathy. The remainder of the examination was normal. A rapid human immunodeficiency virus infection test was negative. A biopsy was performed for further evaluation.
Figure 1.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Chancroid.
B. Condyloma acuminatum.
C. Condyloma latum.
D. Granuloma inguinale.
E. Lymphogranuloma venereum.
Discussion
The answer is C: condyloma latum. Condyloma latum is a highly contagious cutaneous form of secondary syphilis caused by the spirochete Treponema pallidum. The hypopigmented lesions are painless, firm, moist, flat-topped, smooth, pink-to-reddish papules. They generally appear on mucocutaneous sites but may also occur in moist intertriginous regions.
Secondary syphilis presents three to 12 weeks after the primary chancre and usually resolves in two to 12 weeks. The primary chancre is still present in up to one-third of patients with secondary syphilis.1 Other features of secondary syphilis include a generalized papulosquamous rash involving the palms and soles, patchy (“moth-eaten”) alopecia of the scalp, mucous patches, and generalized lymphadenopathy with associated fever, headache, and malaise.2
Serologic testing is the mainstay of syphilis diagnosis. Initial testing includes nontreponemal tests, such as the Venereal Disease Research Laboratories and rapid plasma reagin tests.3 Because of the 1% to 2% false-positive rate with initial testing, the diagnosis is confirmed with the fluorescent treponemal antibody absorption test, which has high sensitivity and very high specificity for syphilis. Lesional skin biopsy may be particularly helpful in cases of primary and secondary syphilis because of the availability of the T. pallidum immunostain. Penicillin G benzathine is the treatment of choice for all stages of syphilis, except for neurosyphilis.4
Chancroid is a sexually transmitted infection caused by Haemophilus ducreyi bacteria. It presents as one or more painful, nonindurated genital ulcers with a friable base and sharp undermined borders, as well as associated painful inguinal lymphadenopathy.5
Condyloma acuminatum (genital warts) is caused by human papillomavirus infection. It is the most common viral sexually transmitted infection. The lesions are painless, cauliflower-like or polypoid, skin-colored papules of varying sizes. Condyloma latum can mimic condyloma acuminatum, but the lesions of condyloma latum tend to be more flat-topped and smooth.6
Granuloma inguinale is a genitoulcerative disease endemic in tropical and subtropical regions of the world. It is caused by Klebsiella granulomatis bacteria and begins as a slow-growing nodule or papule at the site of inoculation that develops into a painless, beefy-red genital ulcer. Inguinal lymphadenopathy is not commonly present.7
Lymphogranuloma venereum is caused by the L1, L2, and L3 serovars of Chlamydia trachomatis. It most commonly occurs in tropical and subtropical regions, although outbreaks have occurred in developed countries among those with human immunodeficiency virus infection. After an incubation period of three to 12 days, a small, painless, spontaneously resolving papule or shallow ulcer appears. Within two to six weeks, infection spreads to the deep and superficial inguinal lymph nodes, resulting in painful unilateral inguinal or femoral lymphadenopathy (buboes), which may suppurate.8
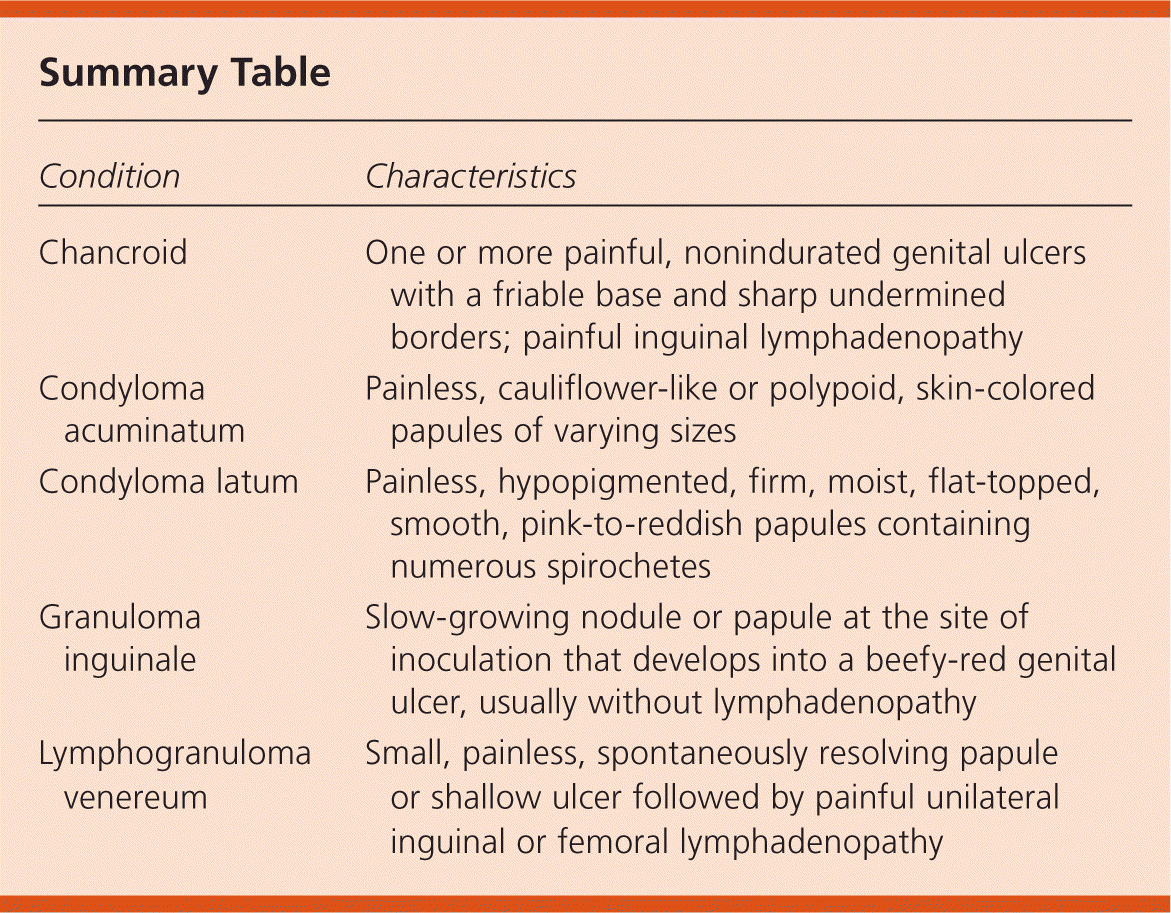
Summary Table
| Condition | Characteristics |
|---|---|
| Chancroid | One or more painful, nonindurated genital ulcers with a friable base and sharp undermined borders; painful inguinal lymphadenopathy |
| Condyloma acuminatum | Painless, cauliflower-like or polypoid, skin-colored papules of varying sizes |
| Condyloma latum | Painless, hypopigmented, firm, moist, flat-topped, smooth, pink-to-reddish papules containing numerous spirochetes |
| Granuloma inguinale | Slow-growing nodule or papule at the site of inoculation that develops into a beefy-red genital ulcer, usually without lymphadenopathy |
| Lymphogranuloma venereum | Small, painless, spontaneously resolving papule or shallow ulcer followed by painful unilateral inguinal or femoral lymphadenopathy |

