Case Scenario
A 45-year-old woman presented to my practice's free health clinic with spinal pain that had been radiating down her left arm and leg for four months. She is a refugee from Cuba and lives in a crowded apartment with her adult son, her brother, her husband, and her husband's parents. Upon arriving in the United States two years ago, the family was provided with temporary Medicaid assistance for seven months, but is now entirely uninsured.
The patient's situation is complicated by job insecurity; she and her son are the only two family members who have found steady work. For the past six months, she has been employed at an automotive plant as an assembly line worker, which involves long hours of repetitive heavy lifting. She says the pain is worse while she is at work, and she feels that there is nothing she can do about it. I suspect this labor is the cause of her back pain, but I know she cannot quit her job. Given her limited options, how should I approach pain management for this patient?
Commentary
In addition to providing direct medical care, the physician can help this patient by obtaining an occupational history, formulating hypotheses about the cause of the pain and potential interventions, and establishing a therapeutic relationship. The physician should also provide a complete musculoskeletal examination to evaluate symptoms and rule out sensory or motor impairment; a depression screening; and assurances that the patient will not be abandoned and that her care will continue.
ADDRESSING WORKPLACE CONDITIONS
The concern that work-related biomechanical stressors have caused or contributed to the patient's back pain may provide an opportunity for positive intervention. Although repetitive motion, heavy lifting, and awkward postures present clear ergonomic hazards, workplace modifications to reduce these hazards can be straightforward, affordable, and provide a tangible return on investment, particularly if other workers have been injured, which is likely. To the extent that the physician or others in the practice who provide social assistance or patient advocacy may be able to help this patient negotiate worksite modifications, she may be able to continue to work. Both the Occupational Safety and Health Administration (OSHA) and its sister agency, the Centers for Disease Control and Prevention's National Institute for Occupational Safety and Health, provide user-friendly guidelines for reducing ergonomic hazards (Table 1). Large manufacturers may have in-house capabilities for addressing these hazards. Smaller companies are also eligible for free assessment and guidance through the small business consultation programs that OSHA funds in each state. Whether the patient is willing to raise these options with her supervisor or have the physician raise them will depend in part on her fear of losing her job, as well as the severity of her condition.
Table 1. Occupational Health Resources for Workers and Physicians
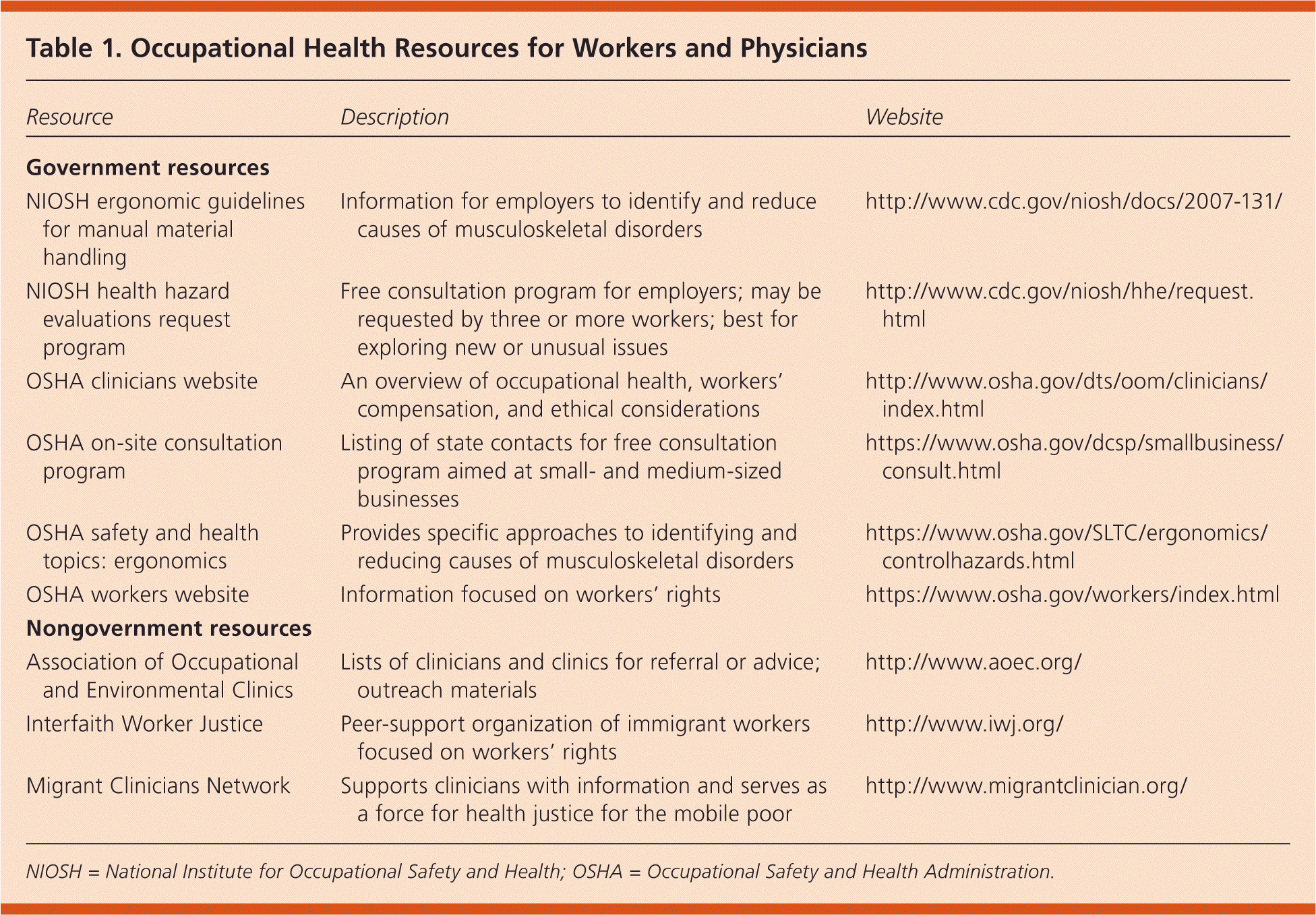
| Resource | Description | Website |
|---|---|---|
| Government resources | ||
| NIOSH ergonomic guidelines for manual material handling | Information for employers to identify and reduce causes of musculoskeletal disorders | http://www.cdc.gov/niosh/docs/2007-131/ |
| NIOSH health hazard evaluations request program | Free consultation program for employers; may be requested by three or more workers; best for exploring new or unusual issues | http://www.cdc.gov/niosh/hhe/request.html |
| OSHA clinicians website | An overview of occupational health, workers' compensation, and ethical considerations | http://www.osha.gov/dts/oom/clinicians/index.html |
| OSHA on-site consultation program | Listing of state contacts for free consultation program aimed at small- and medium-sized businesses | https://www.osha.gov/dcsp/smallbusiness/consult.html |
| OSHA safety and health topics: ergonomics | Provides specific approaches to identifying and reducing causes of musculoskeletal disorders | https://www.osha.gov/SLTC/ergonomics/controlhazards.html |
| OSHA workers website | Information focused on workers' rights | https://www.osha.gov/workers/index.html |
| Nongovernment resources | ||
| Association of Occupational and Environmental Clinics | Lists of clinicians and clinics for referral or advice; outreach materials | http://www.aoec.org/ |
| Interfaith Worker Justice | Peer-support organization of immigrant workers focused on workers' rights | http://www.iwj.org/ |
| Migrant Clinicians Network | Supports clinicians with information and serves as a force for health justice for the mobile poor | http://www.migrantclinician.org/ |
NIOSH = National Institute for Occupational Safety and Health; OSHA = Occupational Safety and Health Administration.
The history and physical examination provide a record of the work-related nature of the patient's condition, and if she requires additional medical care or is unable to work, this documentation will be needed to support her if she decides to file a claim. Workers' compensation programs are specific to each state, but they generally cover medical expenses, such as physical therapy referrals, and a portion of salary—usually once a minimum number of days of work have been missed. Unfortunately, workers may realistically fear retaliation and job loss for reporting injuries. They may be reprimanded for causing the injury or be required to undergo mandatory drug screening. Workers' compensation carriers may contest the work-relatedness of back pain or other conditions that could arise from non-occupational activities. Fewer than one-half of workers who are injured file workers' compensation claims, and only one-half of those are awarded benefits.1,2 The decision to file a claim rests with the patient. Legal aid referral may be helpful.
FEAR OF JOB LOSS
Addressing chronic pain is challenging, and this patient presents the additional concern that she may lose her job, which she needs to support her family. The combination of financial stress, fear of job loss, and physically demanding working conditions may contribute to a cycle of chronic pain and depression.3,4
Two approaches may help this patient, and both likely require referrals. The first is to identify social services for which she may be eligible; the second is to direct her toward workers' centers, unions, and other labor or community associations that may help provide a sense of self-efficacy, particularly if her employer fails to reduce the hazards and she decides to file an OSHA complaint.5
Although her family's Medicaid coverage had a finite duration, as a legal U.S. resident, she may take advantage of other public health programs and services that are available to refugees and authorized immigrants. Most importantly, because she can become a U.S. citizen in the future, she can look forward to accessing public health services that are not available to immigrants who do not have documentation or are not citizens, such as the Supplemental Nutrition Assistance Program and Temporary Assistance for Needy Families. Additionally, she may currently be eligible for these programs because they both make a provision for Cuban entrants within the first few years of their arrival. If she resides in a state that has implemented expanded Medicaid, she may be able to receive coverage based on income. If her state has not expanded Medicaid, her limited family income coupled with her qualified immigration status allows her to purchase private health insurance and to be eligible for premium tax credits and other savings. However, the high deductibles in many of these plans are a barrier to care for many low-wage workers. As a last resort, if she were to become too incapacitated to work, she may be entitled to Supplemental Security Income assistance.6
The free clinic where the patient is receiving care can help her navigate the health care system, particularly if she faces language or transportation barriers. Alternatively, the clinic may refer her to a Federally Qualified Health Center, or to a look-alike center, both of which can receive payments from the Centers for Medicare and Medicaid Services. Currently, 1,380 of these organizations receive partial funding to provide primary care and additional support services to the most vulnerable members of society, without regard for immigration status.7
It is worth emphasizing that an undocumented immigrant in a similar situation would face additional burdens, such as retaliatory deportation, permanent job loss, and family separation. Although most states require employers to provide workers' compensation to employees who are injured on the job regardless of immigration status, a handful expressly exclude unauthorized workers.8 Immigrants in this circumstance often continue to work through the pain and pay for all follow-up care out of pocket.
RECOMMENDATIONS
For the patient in this case scenario, the physician should document the work-relatedness of the pain; explore options for worksite interventions and for filing workers' compensation; offer information about additional resources; and, finally, respect her decisions.
This concerned physician is uniquely positioned to discuss the occupational origins of the patient's back pain, offering both palliative interventions and potential work accommodations. Table 1 provides resources on identifying and reducing worksite hazards, occupational medicine information, and resources for workers.

