Antibiotic resistance is one of the world's most pressing public health problems. Antibiotic-resistant infections account for an estimated 2 million illnesses and 23,000 deaths annually in the United States.1 Antibiotic use is a major driver of resistance,1 and most antibiotics are used in outpatient settings.2 Nationally, population-based rates of antibiotic prescribing for children decreased from 2000 to 2010, but did not change among adults 18 to 64 years of age and increased for adults 65 years and older.3 Additionally, broad-spectrum antibiotic prescribing increased for all age groups from 2000 to 2010,3 and antibiotic prescribing for acute respiratory tract infections remained common in children and adults.3,4 In 2011, U.S. clinicians prescribed 262.5 million outpatient courses of antibiotics; of these, family physicians prescribed one-fourth, more than any other subspecialty.5 Thus, family physicians are critical partners in the effort to avoid antibiotic overuse.
Being a good antibiotic steward means protecting patients and the public from antibiotic resistance and adverse events by prescribing antibiotics only when needed, and prescribing the right drug at the right dosage for the right duration. Antibiotic use in childhood has been linked to increased risks of autoimmune diseases and obesity, which are likely mediated via disruptions in the microbiome.6 Clinicians should carefully weigh the risks and benefits when prescribing these drugs. In focus groups, messages about the risks associated with antibiotic use resonated with parents, who stated that they want to be informed about possible adverse drug events.7 However, adult patients seemed to be less concerned about the possibility of adverse drug events.7
Why do clinicians prescribe antibiotics inappropriately? They generally know—but do not always follow—established clinical guidelines for appropriate antibiotic use.8 Clinicians cite patient pressure and customer satisfaction as major reasons for inappropriate antibiotic prescriptions.8–10 Clinicians are more likely to prescribe antibiotics if they perceive that the parent wants them to, but studies have shown that they do not accurately predict parental expectations.11 Studies suggest that parents are often seeking reassurance that their child's condition is not serious and want to know how to help relieve their child's symptoms, but the clinician perceives them as expecting antibiotics based on things that they say.11,12 For example, clinicians are significantly more likely to think a parent wants antibiotics if the parent asks questions about the treatment plan (e.g., stating that over-the-counter treatment is not working, questioning whether the clinician thinks the child needs antibiotics), but parents are actually no more likely to do so if they expect to receive antibiotics.12 Misunderstandings such as these are likely contributing to antibiotic overuse.
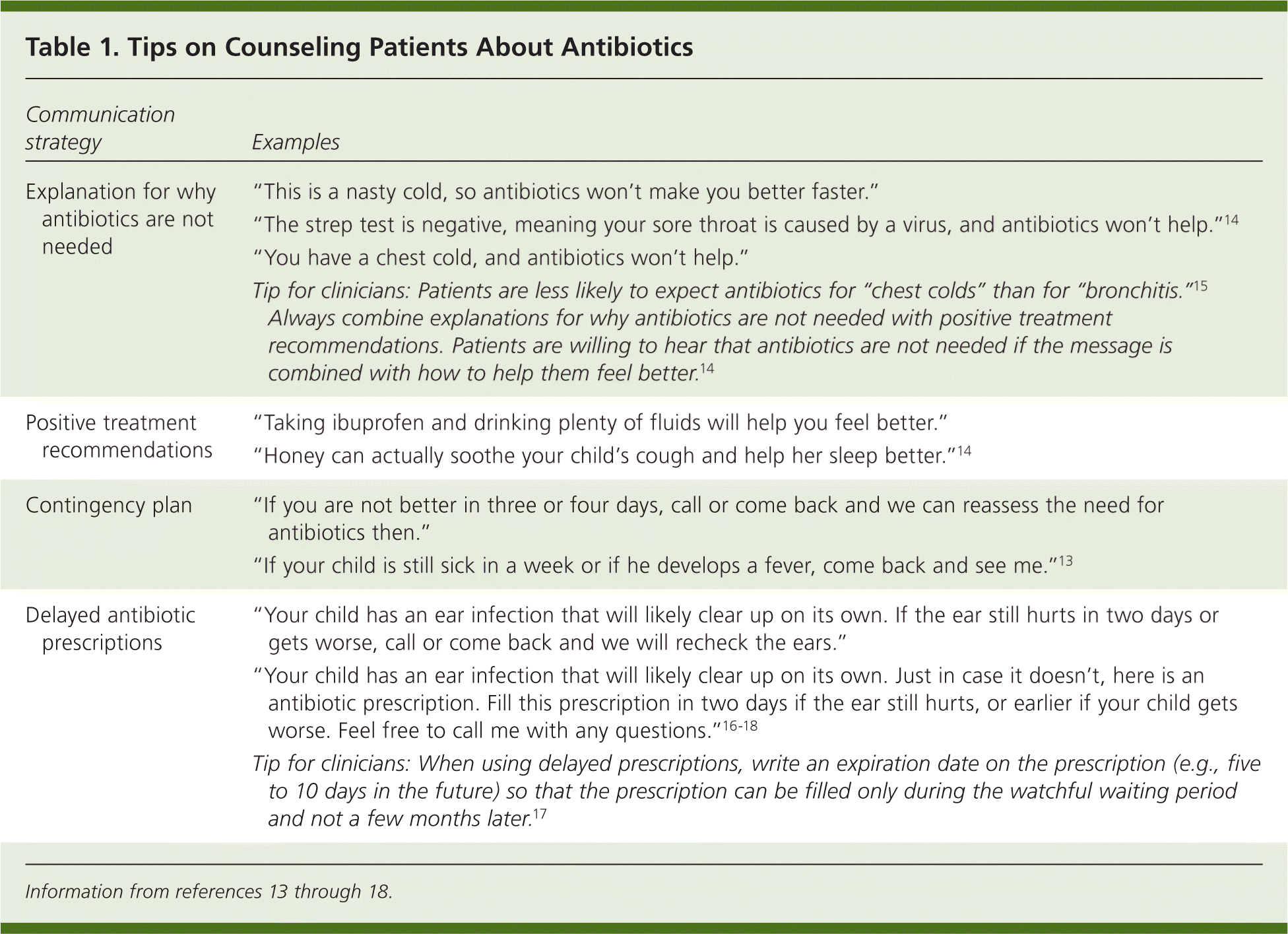
Although not all patients and families expect antibiotics, some do. In these cases, how can clinicians prescribe antibiotics appropriately and keep patients and families satisfied? Studies have shown that even if patients expect antibiotics, they are willing to forego them if clinicians explain why antibiotics are not needed, provide positive treatment recommendations, and suggest contingency plans13,14 (Table 113–18 ). Furthermore, labels are important: patients are less likely to expect antibiotics if they are told they have a “chest cold” rather than “bronchitis.”15 In the Netherlands, communications training for family physicians led to reduced antibiotic prescriptions for acute respiratory infections in patients of all ages, and the effect of this training was sustained over 3.5 years.19 This communications training focused on teaching the clinician to elicit the patient's baseline knowledge and expectations, discuss the benefits and harms of antibiotics, provide a contingency plan for the illness, and assess the patient's understanding at the end of the visit.20
Table 1. Tips on Counseling Patients About Antibiotics
| Communication strategy | Examples |
|---|---|
|
|
|
|
|
|
|
|
Beyond effective communication, making a public commitment to prescribe antibiotics appropriately and using delayed antibiotic prescribing (i.e., watchful waiting) are evidence-based interventions (Table 2).16,18–21 One study found that displaying posters in examination rooms with the clinician's photograph, signature, and commitment to use antibiotics appropriately led to a 20% reduction in inappropriate prescribing for acute respiratory infections.21 Delayed prescriptions can be used for patients with nonsevere infections that are likely to resolve spontaneously but may require antibiotics if they do not improve, such as otitis media or sinusitis. In delayed antibiotic prescribing, patients are given a prescription but instructed not to fill it unless symptoms do not improve or worsen within a certain time. Alternatively, the patient can return for an antibiotic prescription.
Table 2. Evidence-Based Interventions to Reduce Inappropriate Antibiotic Prescribing

| Intervention | Example | Results |
|---|---|---|
| Delayed antibiotic prescriptions | Patients are given a prescription or instructed to return to get a prescription if they do not feel better in a specified time or if they feel substantially worse | 62% of children with acute otitis media and delayed prescriptions did not fill them; 13% of children with acute otitis media and immediate prescriptions did not fill them.18 |
| 91% of adults with acute respiratory infections and immediate antibiotic prescriptions used antibiotics; 33% of patients with delayed antibiotic prescriptions did not use antibiotics; 23% of patients who were instructed to return to get a prescription used antibiotics; 12% of patients with no antibiotic prescriptions used antibiotics. Patient satisfaction was similar in all groups.16 | ||
| Effective communication | Training on how to elicit the patient's baseline knowledge and expectations, discussing the benefits and harms of antibiotic use, providing a contingency plan, and assessing the patient's understanding20 | Antibiotics were prescribed in 26% of visits for respiratory infections to family physicians who had communications training compared with 39% of visits to physicians in the control group.19 |
| Public commitments to use antibiotics appropriately | Posters displayed in examination rooms with the clinician's photograph, signature, and commitment to use antibiotics appropriately | 20% reduction in inappropriate antibiotic prescribing for adults with acute respiratory tract infections compared with control group.21 |
Appropriate antibiotic prescribing is a quality-of-care issue; all clinicians have the responsibility to provide the right treatments to their patients while minimizing harm. Effective communication, public commitments, and delayed antibiotic prescriptions are evidence-based tools that family physicians can institute in any office setting. With these interventions, we can continue to improve antibiotic prescribing for children and extend these improvements to patients of all ages.

