Premenstrual disorders affect up to 12% of women. The subspecialties of psychiatry and gynecology have developed overlapping but distinct diagnoses that qualify as a premenstrual disorder; these include premenstrual syndrome and premenstrual dysphoric disorder. These conditions encompass psychological and physical symptoms that cause significant impairment during the luteal phase of the menstrual cycle, but resolve shortly after menstruation. Patient-directed prospective recording of symptoms is helpful to establish the cyclical nature of symptoms that differentiate premenstrual syndrome and premenstrual dysphoric disorder from other psychiatric and physical disorders. Physicians should tailor therapy to achieve the greatest functional improvement possible for their patients. Select serotonergic antidepressants are first-line treatments. They can be used continuously or only during the luteal phase. Oral contraceptives and calcium supplements may also be used. There is insufficient evidence to recommend treatment with vitamin D, herbal remedies, or acupuncture, but there are data to suggest benefit from cognitive behavior therapy.
Premenstrual disorders consist of psychiatric or somatic symptoms that develop within the luteal phase of the menstrual cycle, affect the patient's normal daily functioning, and resolve shortly after menstruation. The luteal phase begins after ovulation and ends with the start of menstruation. The subspecialties of psychiatry and gynecology have developed overlapping but distinct diagnoses that qualify as a premenstrual disorder.1 The American Congress of Obstetricians and Gynecologists (ACOG) includes psychiatric and physical symptoms in describing premenstrual syndrome (PMS; Table 1).2 The American Psychiatric Association (APA) focuses predominantly on psychiatric symptoms in its diagnostic criteria for premenstrual dysphoric disorder (PMDD; Table 2).3 Symptoms can occur anytime between menarche and menopause. The burden of disease can be high; women with PMS have higher rates of work absences, higher medical expenses, and lower health-related quality of life.4
WHAT IS NEW ON THIS TOPIC: PREMENSTRUAL SYNDROME AND PREMENSTRUAL DYSPHORIC DISORDER
Prospective questionnaires are the most accurate way to diagnose premenstrual syndrome and premenstrual dysphoric disorder because patients have been found to greatly overestimate the cyclical nature of symptoms, when realistically, they are erratic or simply exacerbated during the luteal cycle.
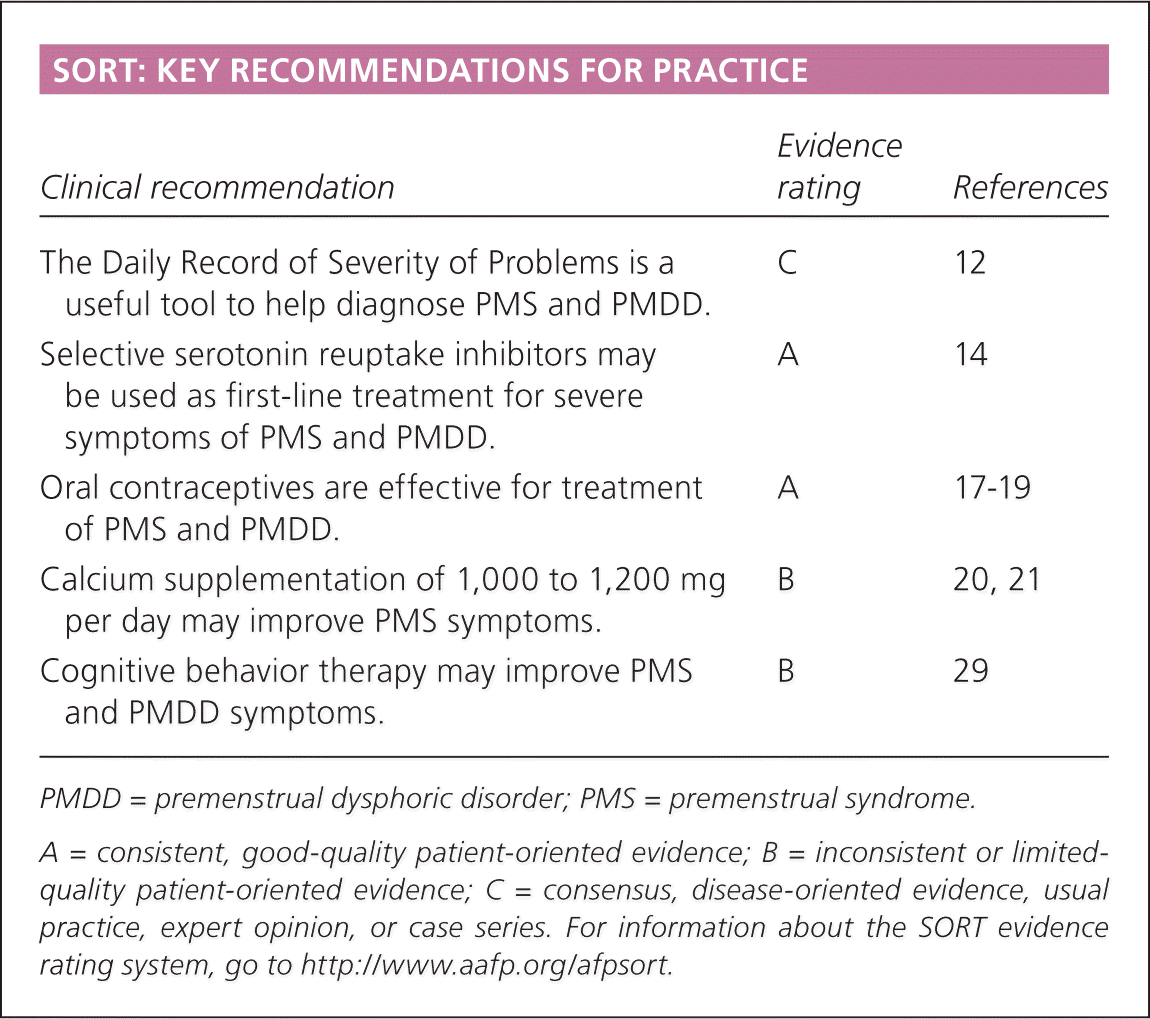
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The Daily Record of Severity of Problems is a useful tool to help diagnose PMS and PMDD. | C | 12 |
| Selective serotonin reuptake inhibitors may be used as first-line treatment for severe symptoms of PMS and PMDD. | A | 14 |
| Oral contraceptives are effective for treatment of PMS and PMDD. | A | 17–19 |
| Calcium supplementation of 1,000 to 1,200 mg per day may improve PMS symptoms. | B | 20, 21 |
| Cognitive behavior therapy may improve PMS and PMDD symptoms. | B | 29 |
PMDD = premenstrual dysphoric disorder; PMS = premenstrual syndrome.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Table 1. Diagnostic Criteria for Premenstrual Syndrome

| Premenstrual syndrome can be diagnosed if the patient reports at least one of the following affective and somatic symptoms during the five days before menses in each of the three previous menstrual cycles* | |
|---|---|
| Affective symptoms | Somatic symptoms |
| Angry outbursts | Abdominal bloating |
| Anxiety | Breast tenderness or swelling |
| Confusion | Headache |
| Depression | Joint or muscle pain |
| Irritability | Swelling of extremities |
| Social withdrawal | Weight gain |
*—These symptoms must be relieved within four days of the onset of menses, without recurrence until at least day 13 of the cycle, and must be present in the absence of any pharmacologic therapy, hormone ingestion, or drug or alcohol use. The symptoms must occur reproducibly during two cycles of prospective recording. The patient must exhibit identifiable dysfunction in social, academic, or work performance.
Adapted with permission from American College of Obstetricians and Gynecologists. Guidelines for Women's Health Care: A Resource Manual. 4th ed. Washington, DC: American College of Obstetricians and Gynecologists; 2014:608.
Table 2. Diagnostic Criteria for Premenstrual Dysphoric Disorder

| A. In the majority of menstrual cycles, at least five symptoms must be present in the final week before the onset of menses, start to improve within a few days after the onset of menses, and become minimal or absent in the week postmenses. | |
| B. One (or more) of the following symptoms must be present: | |
| 1. Marked affective lability (e.g., mood swings; feeling suddenly sad or tearful, or increased sensitivity to rejection). | |
| 2. Marked irritability or anger or increased interpersonal conflicts. | |
| 3. Marked depressed mood, feelings of hopelessness, or self-deprecating thoughts. | |
| 4. Marked anxiety, tension, and/or feelings of being keyed up or on edge. | |
| C. One (or more) of the following symptoms must additionally be present, to reach a total of five symptoms when combined with symptoms from Criterion B above. | |
| 1. Decreased interest in usual activities (e.g., work, school, friends, hobbies). | |
| 2. Subjective difficulty in concentration. | |
| 3. Lethargy, easy fatigability, or marked lack of energy. | |
| 4. Marked change in appetite; overeating; or specific food cravings. | |
| 5. Hypersomnia or insomnia. | |
| 6. A sense of being overwhelmed or out of control. | |
| 7. Physical symptoms such as breast tenderness or swelling, joint or muscle pain, a sensation of “bloating,” or weight gain. | |
| D. The symptoms are associated with clinically significant distress or interference with work, school, usual social activities, or relationships with others (e.g., avoidance of social activities; decreased productivity and efficiency at work, school, or home). | |
| E. The disturbance is not merely an exacerbation of the symptoms of another disorder, such as major depressive disorder, panic disorder, persistent depressive disorder (dysthymia), or a personality disorder (although it may co-occur with any of these disorders). | |
| F. Criterion A should be confirmed by prospective daily ratings during at least two symptomatic cycles. ( | |
| G. The symptoms are not attributable to the physiologic effects of a substance (e.g., a drug of abuse, a medication, other treatment) or another medical condition (e.g., hyperthyroidism). | |
Reprinted with permission from the American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 5th ed. Washington, DC: American Psychiatric Association; 2013:171–172.
Epidemiology
About 80% of women report at least one physical or psychiatric symptom during the luteal phase of their menstrual cycle; however, most do not report significant impairment in their daily life.5 In a study of 2,800 French women, about 12% met the diagnostic criteria for PMS, and 4% reported severe symptoms.6 The prevalence of PMS is not associated with age, educational achievement, or employment status.6 Symptom persistence and severity tend to fluctuate. One study found that only 36% of women who were diagnosed with PMS continued to meet the diagnostic criteria one year later.6 Women who gained weight or had a stressful event in the past year are more likely to be diagnosed with PMS.6 Fewer patients meet the more rigorous diagnostic criteria for PMDD; its prevalence is 1.3% to 5.3%.5
Etiology
There is a poor understanding of the etiology of premenstrual disorders. Several studies suggest that cyclical changes in estrogen and progesterone levels trigger the symptoms.7–9 Postmenopausal women who had previously been diagnosed with PMS had recurrent psychiatric and physical symptoms when they received cyclical progestogen therapy.7 Furthermore, the suppression of estrogen with gonadotropin-releasing hormone analogues has been shown to significantly improve PMS symptoms.8 Changes in mood may be attributable to the effect estrogen and progesterone have on the serotonin, γ-aminobutyric acid, and dopamine systems.9 These can also alter the renin-angiotensin-aldosterone system, which could explain some of the bloating and swelling that occur during the luteal phase.9 Sex hormone levels alone cannot fully explain premenstrual disorders. Studies show that women diagnosed with a premenstrual disorder do not have higher levels of estrogen or progesterone than the general population, and accepted explanations as to why some women could be more sensitive to fluctuations in these sex hormones are lacking.6 Monozygotic twin studies suggest a possible genetic component to premenstrual disorders; however, no genes have been identified.10
Diagnosis
Establishing the timing of symptoms is essential when evaluating for PMS and PMDD. Symptoms must occur during the luteal phase and resolve shortly after the onset of menstruation. Other conditions, such as depression or anxiety, may worsen during the luteal phase, but these can be distinguished from PMS because they persist throughout the menstrual cycle. Migraines, anemia, endometriosis, and hypothyroidism may produce symptoms similar to PMS or PMDD and should also be considered. Diagnostic laboratory testing or imaging should be directed at ruling out alternative medical diagnoses.
ACOG has defined PMS as a condition in which a woman experiences at least one affective symptom and one somatic symptom that cause dysfunction in social, academic, or work performance. These symptoms must be cyclical, beginning after ovulation and resolving shortly after the onset of menstruation (Table 1).2 To meet the diagnostic criteria for PMDD, a patient must have at least five of the symptoms listed in Table 2 in the week before menses, and these symptoms must improve within a few days after the onset of menses.3
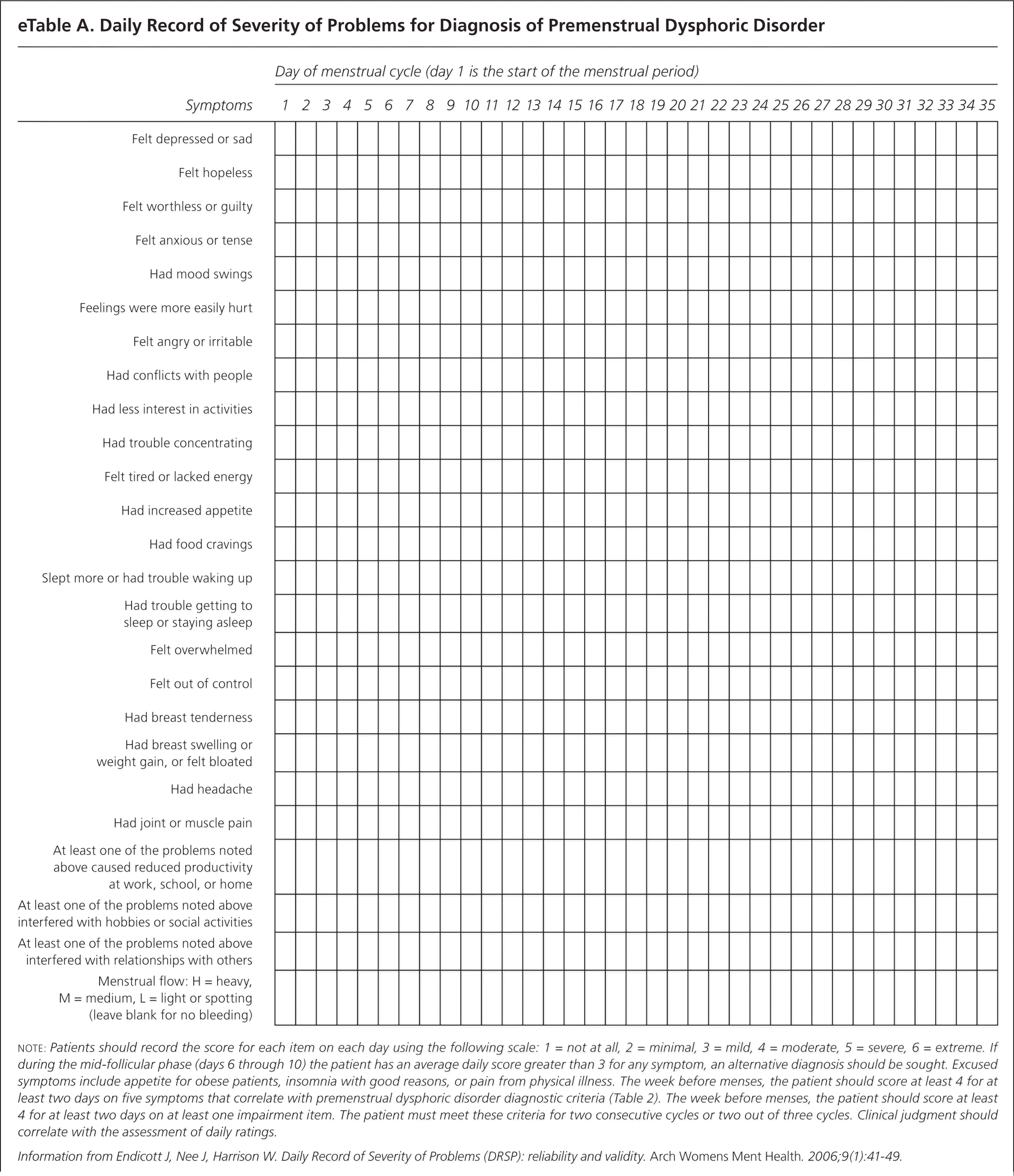
Prospective questionnaires are the most accurate way to diagnose PMS and PMDD because patients greatly overestimate the cyclical nature of symptoms, when in fact they are erratic or simply exacerbated during their luteal phase.2,3,11 The Daily Record of Severity of Problems (DRSP) is a valid and reliable tool that can be used to diagnose PMS or PMDD12 (eTable A). It is a daily log of symptoms that correlate with the diagnostic criteria for PMS and PMDD. Patients rate their symptoms through at least two menstrual cycles, which requires a significant investment of time and effort. Administering the DRSP on the first day of menses may be an acceptable way to screen for premenstrual disorders. A cutoff value of 50 provides a positive predictive value of 63.4% and a negative predictive value of 90%.13
eTable A. Daily Record of Severity of Problems for Diagnosis of Premenstrual Dysphoric Disorder
| Symptoms | Day of menstrual cycle (day 1 is the start of the menstrual period) | ||||||||||||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 | 13 | 14 | 15 | 16 | 17 | 18 | 19 | 20 | 21 | 22 | 23 | 24 | 25 | 26 | 27 | 28 | 29 | 30 | 31 | 32 | 33 | 34 | 35 | |
| Felt depressed or sad | |||||||||||||||||||||||||||||||||||
| Felt hopeless | |||||||||||||||||||||||||||||||||||
| Felt worthless or guilty | |||||||||||||||||||||||||||||||||||
| Felt anxious or tense | |||||||||||||||||||||||||||||||||||
| Had mood swings | |||||||||||||||||||||||||||||||||||
| Feelings were more easily hurt | |||||||||||||||||||||||||||||||||||
| Felt angry or irritable | |||||||||||||||||||||||||||||||||||
| Had conflicts with people | |||||||||||||||||||||||||||||||||||
| Had less interest in activities | |||||||||||||||||||||||||||||||||||
| Had trouble concentrating | |||||||||||||||||||||||||||||||||||
| Felt tired or lacked energy | |||||||||||||||||||||||||||||||||||
| Had increased appetite | |||||||||||||||||||||||||||||||||||
| Had food cravings | |||||||||||||||||||||||||||||||||||
| Slept more or had trouble waking up | |||||||||||||||||||||||||||||||||||
| Had trouble getting to sleep or staying asleep | |||||||||||||||||||||||||||||||||||
| Felt overwhelmed | |||||||||||||||||||||||||||||||||||
| Felt out of control | |||||||||||||||||||||||||||||||||||
| Had breast tenderness | |||||||||||||||||||||||||||||||||||
| Had breast swelling or weight gain, or felt bloated | |||||||||||||||||||||||||||||||||||
| Had headache | |||||||||||||||||||||||||||||||||||
| Had joint or muscle pain | |||||||||||||||||||||||||||||||||||
| At least one of the problems noted above caused reduced productivity at work, school, or home | |||||||||||||||||||||||||||||||||||
| At least one of the problems noted above interfered with hobbies or social activities | |||||||||||||||||||||||||||||||||||
| At least one of the problems noted above interfered with relationships with others | |||||||||||||||||||||||||||||||||||
| Menstrual flow: H = heavy, M = medium, L = light or spotting (leave blank for no bleeding) | |||||||||||||||||||||||||||||||||||
note: Patients should record the score for each item on each day using the following scale: 1 = not at all, 2 = minimal, 3 = mild, 4 = moderate, 5 = severe, 6 = extreme. If during the mid-follicular phase (days 6 through 10) the patient has an average daily score greater than 3 for any symptom, an alternative diagnosis should be sought. Excused symptoms include appetite for obese patients, insomnia with good reasons, or pain from physical illness. The week before menses, the patient should score at least 4 for at least two days on five symptoms that correlate with premenstrual dysphoric disorder diagnostic criteria (Table 2). The week before menses, the patient should score at least 4 for at least two days on at least one impairment item. The patient must meet these criteria for two consecutive cycles or two out of three cycles. Clinical judgment should correlate with the assessment of daily ratings.
Information from Endicott J, Nee J, Harrison W. Daily Record of Severity of Problems (DRSP): reliability and validity. Arch Womens Ment Health. 2006;9(1):41–49.
Treatment
Treatment of PMS and PMDD focuses on relieving physical and psychiatric symptoms. Many of the medications used address the body's hormonal activity through suppression of ovulation, whereas others affect the concentration of neurotransmitters such as serotonin, norepinephrine, or dopamine in the brain. A third group of complementary or alternative agents with varying mechanisms of action are also used. In the United States, selective serotonin reuptake inhibitors (SSRIs) are approved for primary treatment. Although SSRIs are considered psychiatric medications, when used to treat premenstrual disorders they improve physical and psychiatric symptoms in most patients.14 Physicians should tailor therapy based on patient tolerance and response to each medication.
PHARMACOLOGIC TREATMENTS
Serotonergic Antidepressants. SSRIs are first-line treatment for severe symptoms of PMS and PMDD. Sertraline (Zoloft), paroxetine (Paxil), fluoxetine (Prozac), citalopram (Celexa), and escitalopram (Lexapro) can be used to treat the psychiatric symptoms of PMS and PMDD and have been shown to relieve some of the physical symptoms.14 A 2013 Cochrane review analyzed 31 randomized controlled trials that compared SSRIs with placebo for symptom relief of PMS.14 Each of the five SSRIs studied had statistically significant benefits on patient-reported symptoms when taken continuously or only during the luteal phase, but more direct studies comparing luteal phase administration with continuous administration are needed.14 Adverse effects include nausea, asthenia, fatigue, and sexual dysfunction.14 All SSRI doses seemed to be effective for psychiatric symptoms, and ultimately could be titrated to the patient's tolerability.14 Higher doses are needed for relief of physical symptoms. Bupropion (Wellbutrin) was not effective for symptom relief of PMS or PMDD.14
Serotonin-Norepinephrine Reuptake Inhibitors (SNRIs). SNRIs such as venlafaxine have been used off-label to treat PMDD in women with predominantly psychological symptoms.15 The effect is achieved over a relatively short period, three to four weeks, and sustained throughout subsequent menstrual cycles.15
Quetiapine (Seroquel). This antipsychotic has been studied as an adjunctive treatment with an SSRI or SNRI in patients with PMS or PMDD. The goal was to improve luteal phase mood in women who did not respond to SSRI or SNRI therapy alone.16 In a small study, 20 women were started on 25 mg of quetiapine and followed for three menstrual cycles.16 Luteal phase mood lability, anxiety, and irritability were reduced in the quetiapine group.16
Oral Contraceptives. Studies have suggested that oral contraceptives provide benefit when treating physical and psychiatric symptoms of PMS or PMDD. Researchers analyzed four moderate-quality trials of continuous oral contraceptive use (90 mcg levonorgestrel/20 mcg ethinyl estradiol) in women who tracked their symptoms on the DRSP.17 Although results were somewhat inconsistent, an improvement in depressive and physical symptoms (from 30% to 59%) was identified. A higher placebo response occurred in women with PMDD, which suggests that a greater improvement occurred in women with predominantly psychiatric, placebo-responsive symptoms at baseline.17,18 A separate PMDD trial found that continuous treatment for 112 days resulted in the most improvement in DRSP scores.18
A 2012 Cochrane review of oral contraceptives containing drospirenone evaluated five trials with 1,920 women.19 High drop-out rates were noted in all but one trial. Results showed that the drospirenone combination pill reduced impairments in productivity and social functioning in women with PMDD, but there was insufficient evidence of benefit for those with PMS.19 Oral contraceptives with and without drospirenone seem to be effective at relieving abdominal bloating, mastalgia, headache, weight gain, and swelling of extremities. Trials that extend beyond three months are needed for further analysis.19
Other Medications. Calcium supplementation has been evaluated as treatment for PMS. Women with PMS and mood instability have been noted to have associated cyclic changes in their calcium levels; the exact mechanism of action is unknown.20 A randomized controlled trial of 179 Tehran University students who met criteria for PMS without another psychiatric diagnosis found a 50% reduction in depression, appetite, and fatigue in women who received 500 mg of supplemental calcium carbonate twice daily for three months.21 This result was also demonstrated in a U.S. study of more than 400 women who supplemented with 1,200 mg of calcium carbonate daily.20
Vitamin D supplementation for treatment of PMS and PMDD symptoms was reviewed in a cross-sectional analysis of a large study.22 The cross-section analyzed was too small to make strong conclusions about the benefit of vitamin D.22 A separate study followed 401 women for 16 years and compared those who developed PMS with those who did not.23 The analysis concluded that low vitamin D levels were not associated with an increased risk of PMS.23 Further studies are needed to support the use of vitamin D as a treatment for symptoms of PMS and PMDD. Vitamin B6 at a dosage of 80 mg per day has also been studied and recommended as treatment for primarily psychological symptoms of PMS, but these studies are small and more data is needed to recommend it as first-line treatment.24
Guidelines from the International Society of Premenstrual Disorders addressed gonadotropin-releasing hormone agonists as potential treatment of PMS and PMDD by eliminating luteal phase symptoms.25 Although these medications have been used since the 1980s and are effective, they are not practical for long-term use because of the increased cardiovascular and osteoporosis risks associated with extended use.25 Long-term users often need hormone add-back therapy to counteract many of their hypoestrogenic effects, which may cause a return of PMS symptoms.26
COMPLEMENTARY AND NONPHARMACOLOGIC TREATMENTS
Herbal Preparations and Acupuncture. Many small, poorly conducted studies have reviewed the effectiveness of Chinese herbal supplements and acupuncture in the treatment of premenstrual symptoms.27 This evidence is too limited and study quality is too poor to suggest benefit.27 A 2010 Cochrane review of Chinese herbal supplements for PMS also did not find evidence that was strong enough to support their use.28 The studies evaluated use of saffron, St. John's wort, ginkgo, vitex agnus-castus, peppermint, angelica root, dragon's teeth, turmeric, tangerine leaf, and bitter orange, among others.27,28 Larger, more extensive trials are needed to support the use of these agents as first-line treatment.
Cognitive Behavior Therapy. A 2009 meta-analysis analyzed seven trials, three of which were randomized controlled trials, and showed improvement in functioning and depression scores for patients with PMS or PMDD.29 The frequency and duration of therapy were not defined. However, the results suggest that mindfulness-based exercises and acceptance-based cognitive behavior therapy may be helpful for reducing symptoms. Further studies are needed to support the use of cognitive behavior therapy as first-line therapy.
Data Sources: Research was conducted in the PubMed and Cochrane databases using the terms PMS and PMDD, PMS and PMDD treatment, and PMS and PMDD definition. We also used articles located in an Essential Evidence Plus report on the topic premenstrual dysphoric disorder, topic 248. External sources such as the Diagnostic and Statistical Manual of Mental Disorders, 5th ed., and publications from the American Congress of Obstetricians and Gynecologists were accessed separately and directly through our institutional licensing agreement at the Medical College of Wisconsin. Search date: August 1, 2015.

