Clinical Question
Can gout be diagnosed with clinical and laboratory data, without performing joint aspiration?
Evidence Summary
Gout is a metabolic disorder of hyperuricemia in which excessive extracellular uric acid crystalizes and precipitates, causing end-organ damage, most commonly in joints. It is estimated that gout affects more than 8 million Americans and accounts for 7 million ambulatory visits in the United States annually.1 Gout is ideally diagnosed through identification of characteristic negatively birefringent crystals under polarized light microscopy in fluid aspirated from end-organ deposits, typically from a joint.2 However, fewer than 10% of patients with gout see a rheumatologist, and most cases of gout are diagnosed in the primary care setting based on signs, symptoms, and serum uric acid level.3 But how accurate is a clinical diagnosis, and can it be done better?
One study recruited 93 primary care physicians in the Netherlands who identified and referred 381 consecutive patients with acute monoarthritis.4 The researchers collected the physician's diagnostic impression of gout or nongout, a variety of signs and symptoms, and the serum uric acid level. They also obtained synovial fluid from each patient for monosodium urate crystal analysis. If the diagnosis was unclear, the patient was followed for a year and reevaluated using history, physical examination, and reaspiration. Gout was diagnosed in the 216 patients with monosodium urate crystals; 165 patients did not have gout, and instead had other arthropathies, such as rheumatoid arthritis, psoriatic arthritis, poststreptococcal reactive arthritis, Lyme arthritis, and osteoarthritis. Compared with the preferred diagnostic test, clinical diagnosis by a primary care physician demonstrated limited accuracy (sensitivity = 0.97; specificity = 0.28; positive predictive value = 0.64; negative predictive value = 0.87; positive and negative likelihood ratios = 1.3 and 0.1, respectively). Thus, a primary care physician's overall clinical impression is good at ruling out gout, but not at ruling it in.
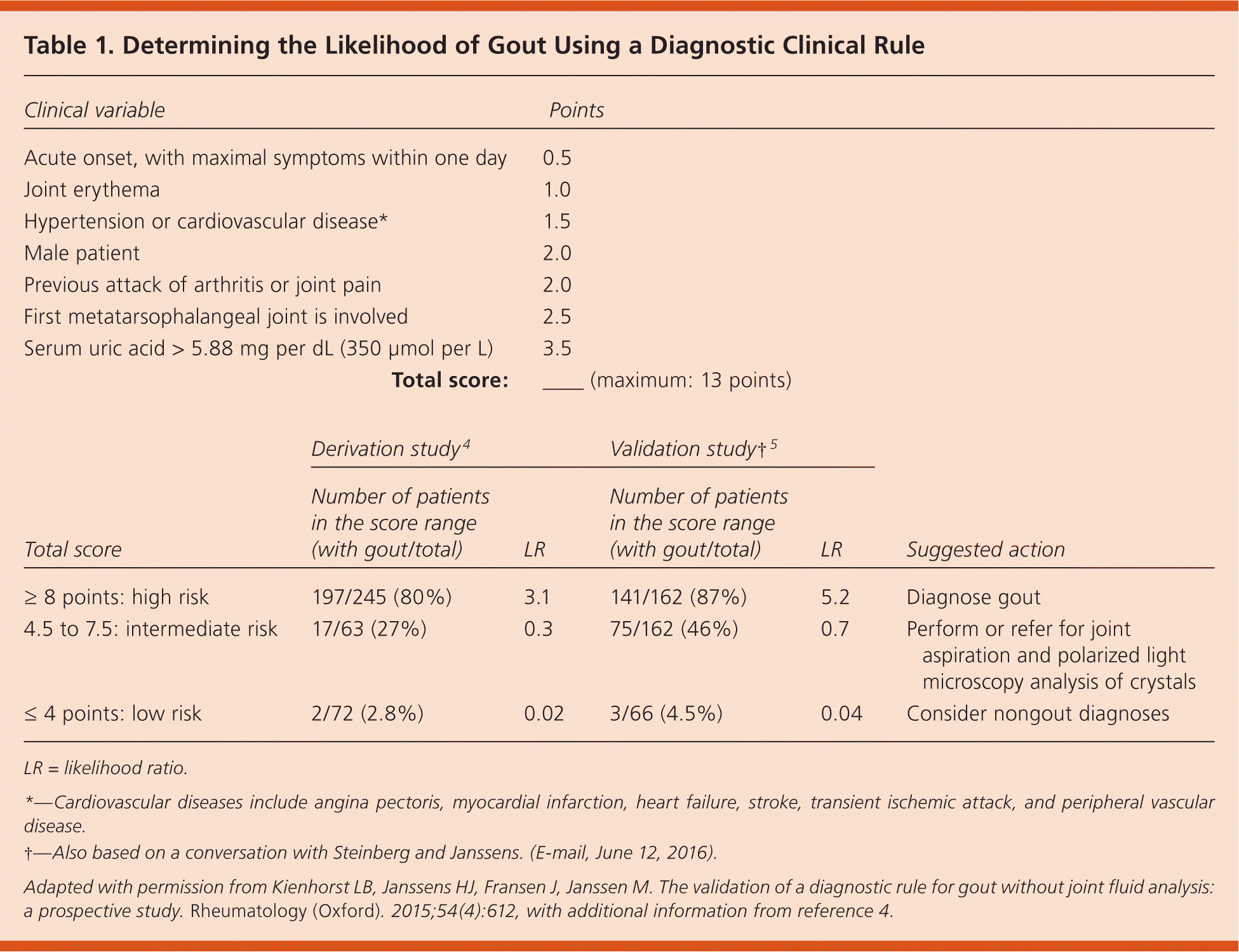
The researchers then used logistic regression to identify the seven best independent predictors of gout.4 Each was assigned a point value according to how strongly it contributed to the diagnosis of gout (Table 1).4,5 Based on cutoffs of 4 points or less, 4.5 to 7.5 points, and 8 points or more, high and low scores had better positive and negative predictive values than the physician's overall impression: the positive predictive value was 80% with a high score vs. 64% with physician impression; the negative predictive value was 97% with a low score vs. 87% with physician impression.4
Table 1. Determining the Likelihood of Gout Using a Diagnostic Clinical Rule
| Clinical variable | Points | ||||
| Acute onset, with maximal symptoms within one day | 0.5 | ||||
| Joint erythema | 1.0 | ||||
| Hypertension or cardiovascular disease* | 1.5 | ||||
| Male patient | 2.0 | ||||
| Previous attack of arthritis or joint pain | 2.0 | ||||
| First metatarsophalangeal joint is involved | 2.5 | ||||
| Serum uric acid > 5.88 mg per dL (350 μmol per L) | 3.5 | ||||
| Total score: | _____ (maximum: 13 points) | ||||
| Derivation study4 | Validation study†5 | ||||
| Total score | Number of patients in the score range (with gout/total) | LR | Number of patients in the score range (with gout/total) | LR | Suggested action |
| ≥ 8 points: high risk | 197/245 (80%) | 3.1 | 141/162 (87%) | 5.2 | Diagnose gout |
| 4.5 to 7.5: intermediate risk | 17/63 (27%) | 0.3 | 75/162 (46%) | 0.7 | Perform or refer for joint aspiration and polarized light microscopy analysis of crystals |
| ≤ 4 points: low risk | 2/72 (2.8%) | 0.02 | 3/66 (4.5%) | 0.04 | Consider nongout diagnoses |
LR = likelihood ratio.
*—Cardiovascular diseases include angina pectoris, myocardial infarction, heart failure, stroke, transient ischemic attack, and peripheral vascular disease.
†—Also based on a conversation with Steinberg and Janssens. (E-mail, June 12, 2016).
Adapted with permission from Kienhorst LB, Janssens HJ, Fransen J, Janssen M. The validation of a diagnostic rule for gout without joint fluid analysis: a prospective study. Rheumatology (Oxford). 2015;54(4):612, with additional information from reference4.
In a validation study of a new group of 390 Dutch primary care patients with acute monoarthritis, the diagnostic clinical rule again outperformed physician diagnosis and performed as well as in the derivation study.5 Physicians should feel comfortable ruling out gout if the score is 4 points or less, and diagnosing it if the score is 8 points or more. Referral to a rheumatologist should be considered for diagnostic confirmation if the score is in the intermediate range. If referral is not an option, nongout diagnoses, reevaluation in three to six months, and/or a trial of empiric therapy can be considered.
Applying the Evidence
A 37-year-old man presents for the second time in 15 months with acute onset of seemingly atraumatic pain, redness, and swelling of the metatarsophalangeal joint in his great toe. He does not have hypertension or cardiovascular disease. His uric acid level was 6.9 mg per dL (410 μmol per L) during the first episode. At the first visit, you suspected unappreciated trauma. But with a second episode, your suspicion shifts toward gout. Because you are not skilled in performing polarization microscopy or small joint aspiration, it is unlikely that you can make the diagnosis using the preferred method of analyzing joint aspirate crystals.
Using the clinical diagnostic rule, you determine that the patient has a score of 11.5 points. Although the unimpressive uric acid level originally dissuaded you from diagnosing gout, this score is strongly suggestive of gout. You make the diagnosis and initiate therapy.

