The authors applied a novel method to identify recent clinical studies that showed results consistent with the principles of the Choosing Wisely campaign. The method, based on crowdsourcing studies known as POEMs (patient-oriented evidence that matters), involved analyzing POEM ratings submitted by physician members of the Canadian Medical Association in the context of their continuing medical education. In the 251 unique POEMs delivered to these physicians in 2015, an average of 1,284 physician ratings were received per POEM. The authors then identified the POEMs that ranked highest on a single item in the rating questionnaire—namely, whether the POEM helps reduce overdiagnosis or overtreatment, which is the focus of the Choosing Wisely campaign. The result is a set of POEMs of original research that describe interventions that are not superior to other options, are sometimes more expensive, or place patients at increased risk of harm. Knowing the bottom line of these studies could help physicians and patients engage in better conversations when making decisions about clinical care.
Choosing Wisely is an initiative that asks medical specialty societies to identify at least five things their members should no longer do because they represent low-value patient care.1 This article highlights the top research studies from 2015 that are consistent with this philosophy.
An annual series in American Family Physician summarizes the top original research studies of the year for primary care.2–6 The studies are selected for their relevance to practice and assessed for validity by independent experts in primary care and research methodology. Approximately 250 articles meet these criteria each year, and they are evaluated in the POEMs continuing medical education (CME) program in Canada.7 The top research studies are then identified based on ratings of clinical relevance submitted by Canadian physicians. POEMs stands for patient-oriented evidence that matters,8 which relates to changes in a patient's morbidity, mortality, or quality of life. It differs from disease-oriented evidence, which relates to changes in physiologic or surrogate markers of health, such as blood pressure, serum creatinine level, hemoglobin level, or neurotransmitters. These markers may or may not directly affect a patient's morbidity, mortality, or quality of life.
A 2015 article described how data from the same POEMs CME program could help the Choosing Wisely campaign systematically identify new recommendations for consideration by expert panels from specialty societies.9 For this article, a novel method of crowdsourcing was used to identify the most primary care–relevant studies of 2015 consistent with the principles of Choosing Wisely. This involved analyzing ratings of POEMs submitted by thousands of physician members of the Canadian Medical Association, using a validated questionnaire.10 For 251 unique POEMs delivered during the calendar year of 2015, an average of 1,284 physician ratings per POEM were received. The POEMs that ranked highest on one item in the rating questionnaire, namely “this information will help to avoid unnecessary treatment, diagnostic procedures, preventive interventions, or a referral for this patient,” were identified. This questionnaire item was chosen because of its direct link to the objective of the Choosing Wisely campaign: reducing overdiagnosis or overtreatment.
The POEMs in this article identify opportunities for physicians to engage in conversation with their patients about low-value care in a way that is consistent with the principles of Choosing Wisely. Many of these POEMs describe interventions that are not superior to other options, are sometimes more expensive, or place patients at increased risk of harm. To maintain a focus on research studies, POEMs about guidelines, such as those produced by the U.S. Preventive Services Task Force, were excluded. We also excluded 12 of the most relevant POEMs of 2015 that were discussed in a previous article.6 However, to highlight their relevance to the Choosing Wisely philosophy, these 12 POEMs are available online (eTable A).
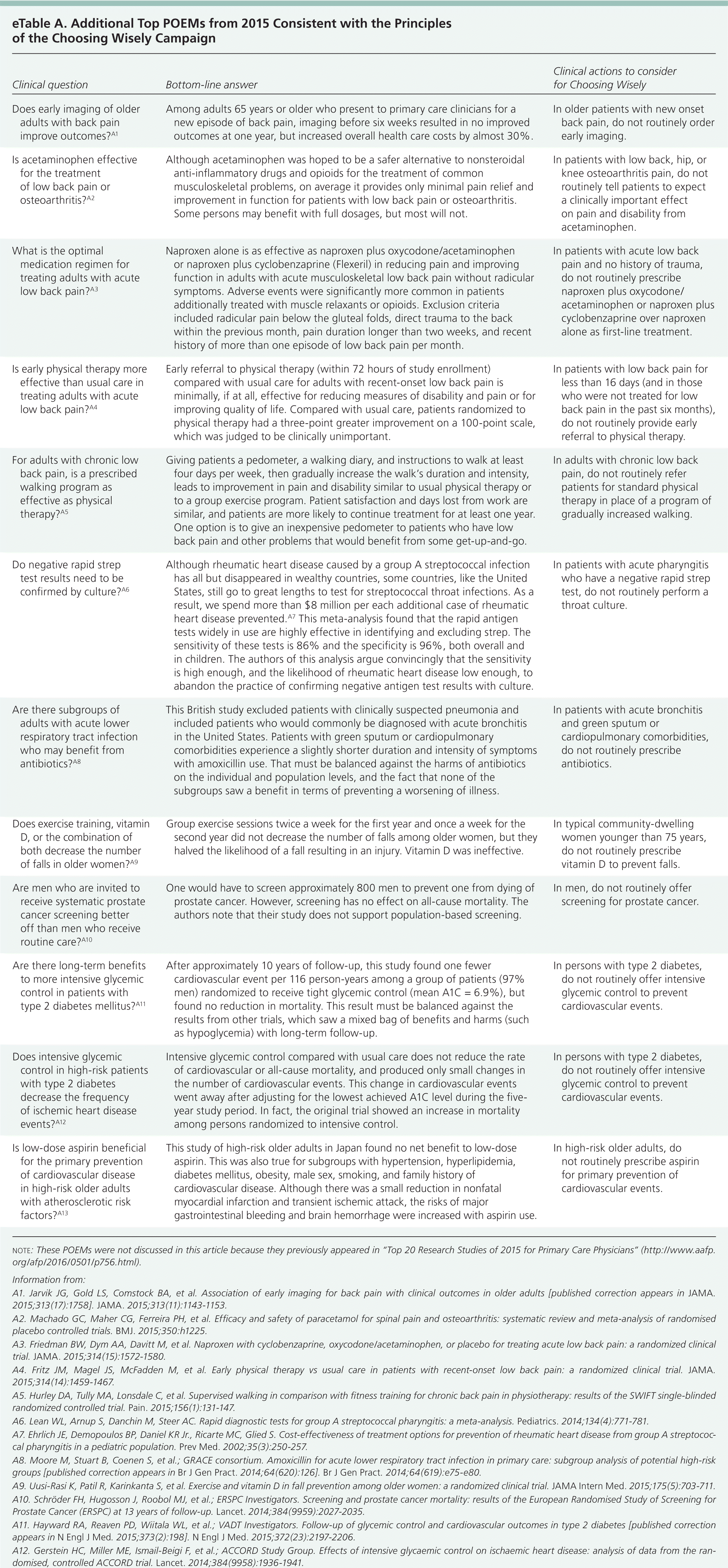
eTable A. Additional Top POEMs from 2015 Consistent with the Principles of the Choosing Wisely Campaign
| Clinical question | Bottom-line answer | Clinical actions to consider for Choosing Wisely |
|---|---|---|
| Does early imaging of older adults with back pain improve outcomes?A1 | Among adults 65 years or older who present to primary care clinicians for a new episode of back pain, imaging before six weeks resulted in no improved outcomes at one year, but increased overall health care costs by almost 30%. | In older patients with new onset back pain, do not routinely order early imaging. |
| Is acetaminophen effective for the treatment of low back pain or osteoarthritis?A2 | Although acetaminophen was hoped to be a safer alternative to nonsteroidal anti-inflammatory drugs and opioids for the treatment of common musculoskeletal problems, on average it provides only minimal pain relief and improvement in function for patients with low back pain or osteoarthritis. Some persons may benefit with full dosages, but most will not. | In patients with low back, hip, or knee osteoarthritis pain, do not routinely tell patients to expect a clinically important effect on pain and disability from acetaminophen. |
| What is the optimal medication regimen for treating adults with acute low back pain?A3 | Naproxen alone is as effective as naproxen plus oxycodone/acetaminophen or naproxen plus cyclobenzaprine (Flexeril) in reducing pain and improving function in adults with acute musculoskeletal low back pain without radicular symptoms. Adverse events were significantly more common in patients additionally treated with muscle relaxants or opioids. Exclusion criteria included radicular pain below the gluteal folds, direct trauma to the back within the previous month, pain duration longer than two weeks, and recent history of more than one episode of low back pain per month. | In patients with acute low back pain and no history of trauma, do not routinely prescribe naproxen plus oxycodone/acetaminophen or naproxen plus cyclobenzaprine over naproxen alone as first-line treatment. |
| Is early physical therapy more effective than usual care in treating adults with acute low back pain?A4 | Early referral to physical therapy (within 72 hours of study enrollment) compared with usual care for adults with recent-onset low back pain is minimally, if at all, effective for reducing measures of disability and pain or for improving quality of life. Compared with usual care, patients randomized to physical therapy had a three-point greater improvement on a 100-point scale, which was judged to be clinically unimportant. | In patients with low back pain for less than 16 days (and in those who were not treated for low back pain in the past six months), do not routinely provide early referral to physical therapy. |
| For adults with chronic low back pain, is a prescribed walking program as effective as physical therapy?A5 | Giving patients a pedometer, a walking diary, and instructions to walk at least four days per week, then gradually increase the walk's duration and intensity, leads to improvement in pain and disability similar to usual physical therapy or to a group exercise program. Patient satisfaction and days lost from work are similar, and patients are more likely to continue treatment for at least one year. One option is to give an inexpensive pedometer to patients who have low back pain and other problems that would benefit from some get-up-and-go. | In adults with chronic low back pain, do not routinely refer patients for standard physical therapy in place of a program of gradually increased walking. |
| Do negative rapid strep test results need to be confirmed by culture?A6 | Although rheumatic heart disease caused by a group A streptococcal infection has all but disappeared in wealthy countries, some countries, like the United States, still go to great lengths to test for streptococcal throat infections. As a result, we spend more than $8 million per each additional case of rheumatic heart disease prevented.A7 This meta-analysis found that the rapid antigen tests widely in use are highly effective in identifying and excluding strep. The sensitivity of these tests is 86% and the specificity is 96%, both overall and in children. The authors of this analysis argue convincingly that the sensitivity is high enough, and the likelihood of rheumatic heart disease low enough, to abandon the practice of confirming negative antigen test results with culture. | In patients with acute pharyngitis who have a negative rapid strep test, do not routinely perform a throat culture. |
| Are there subgroups of adults with acute lower respiratory tract infection who may benefit from antibiotics?A8 | This British study excluded patients with clinically suspected pneumonia and included patients who would commonly be diagnosed with acute bronchitis in the United States. Patients with green sputum or cardiopulmonary comorbidities experience a slightly shorter duration and intensity of symptoms with amoxicillin use. That must be balanced against the harms of antibiotics on the individual and population levels, and the fact that none of the subgroups saw a benefit in terms of preventing a worsening of illness. | In patients with acute bronchitis and green sputum or cardiopulmonary comorbidities, do not routinely prescribe antibiotics. |
| Does exercise training, vitamin D, or the combination of both decrease the number of falls in older women?A9 | Group exercise sessions twice a week for the first year and once a week for the second year did not decrease the number of falls among older women, but they halved the likelihood of a fall resulting in an injury. Vitamin D was ineffective. | In typical community-dwelling women younger than 75 years, do not routinely prescribe vitamin D to prevent falls. |
| Are men who are invited to receive systematic prostate cancer screening better off than men who receive routine care?A10 | One would have to screen approximately 800 men to prevent one from dying of prostate cancer. However, screening has no effect on all-cause mortality. The authors note that their study does not support population-based screening. | In men, do not routinely offer screening for prostate cancer. |
| Are there long-term benefits to more intensive glycemic control in patients with type 2 diabetes mellitus?A11 | After approximately 10 years of follow-up, this study found one fewer cardiovascular event per 116 person-years among a group of patients (97% men) randomized to receive tight glycemic control (mean A1C = 6.9%), but found no reduction in mortality. This result must be balanced against the results from other trials, which saw a mixed bag of benefits and harms (such as hypoglycemia) with long-term follow-up. | In persons with type 2 diabetes, do not routinely offer intensive glycemic control to prevent cardiovascular events. |
| Does intensive glycemic control in high-risk patients with type 2 diabetes decrease the frequency of ischemic heart disease events?A12 | Intensive glycemic control compared with usual care does not reduce the rate of cardiovascular or all-cause mortality, and produced only small changes in the number of cardiovascular events. This change in cardiovascular events went away after adjusting for the lowest achieved A1C level during the five-year study period. In fact, the original trial showed an increase in mortality among persons randomized to intensive control. | In persons with type 2 diabetes, do not routinely offer intensive glycemic control to prevent cardiovascular events. |
| Is low-dose aspirin beneficial for the primary prevention of cardiovascular disease in high-risk older adults with atherosclerotic risk factors?A13 | This study of high-risk older adults in Japan found no net benefit to low-dose aspirin. This was also true for subgroups with hypertension, hyperlipidemia, diabetes mellitus, obesity, male sex, smoking, and family history of cardiovascular disease. Although there was a small reduction in nonfatal myocardial infarction and transient ischemic attack, the risks of major gastrointestinal bleeding and brain hemorrhage were increased with aspirin use. | In high-risk older adults, do not routinely prescribe aspirin for primary prevention of cardiovascular events. |
note: These POEMs were not discussed in this article because they previously appeared in “Top 20 Research Studies of 2015 for Primary Care Physicians” (https://www.aafp.org/afp/2016/0501/p756.html).
Information from: A1. Jarvik JG, Gold LS, Comstock BA, et al. Association of early imaging for back pain with clinical outcomes in older adults [published correction appears in JAMA. 2015;313(17):1758]. JAMA. 2015;313(11):1143–1153.
A2. Machado GC, Maher CG, Ferreira PH, et al. Efficacy and safety of paracetamol for spinal pain and osteoarthritis: systematic review and meta-analysis of randomised placebo controlled trials. BMJ. 2015;350:h1225.
A3. Friedman BW, Dym AA, Davitt M, et al. Naproxen with cyclobenzaprine, oxycodone/acetaminophen, or placebo for treating acute low back pain: a randomized clinical trial. JAMA. 2015;314(15):1572–1580.
A4. Fritz JM, Magel JS, McFadden M, et al. Early physical therapy vs usual care in patients with recent-onset low back pain: a randomized clinical trial. JAMA. 2015;314(14):1459–1467.
A5. Hurley DA, Tully MA, Lonsdale C, et al. Supervised walking in comparison with fitness training for chronic back pain in physiotherapy: results of the SWIFT single-blinded randomized controlled trial. Pain. 2015;156(1):131–147.
A6. Lean WL, Arnup S, Danchin M, Steer AC. Rapid diagnostic tests for group A streptococcal pharyngitis: a meta-analysis. Pediatrics. 2014;134(4):771–781.
A7. Ehrlich JE, Demopoulos BP, Daniel KR Jr., Ricarte MC, Glied S. Cost-effectiveness of treatment options for prevention of rheumatic heart disease from group A streptococcal pharyngitis in a pediatric population. Prev Med. 2002;35(3):250–257.
A8. Moore M, Stuart B, Coenen S, et al.; GRACE consortium. Amoxicillin for acute lower respiratory tract infection in primary care: subgroup analysis of potential high-risk groups [published correction appears in Br J Gen Pract. 2014;64(620):126]. Br J Gen Pract. 2014;64(619):e75–e80.
A9. Uusi-Rasi K, Patil R, Karinkanta S, et al. Exercise and vitamin D in fall prevention among older women: a randomized clinical trial. JAMA Intern Med. 2015;175(5):703–711.
A10. Schröder FH, Hugosson J, Roobol MJ, et al.; ERSPC Investigators. Screening and prostate cancer mortality: results of the European Randomised Study of Screening for Prostate Cancer (ERSPC) at 13 years of follow-up. Lancet. 2014;384(9959):2027–2035.
A11. Hayward RA, Reaven PD, Wiitala WL, et al.; VADT Investigators. Follow-up of glycemic control and cardiovascular outcomes in type 2 diabetes [published correction appears in N Engl J Med. 2015;373(2):198]. N Engl J Med. 2015;372(23):2197–2206.
A12. Gerstein HC, Miller ME, Ismail-Beigi F, et al.; ACCORD Study Group. Effects of intensive glycaemic control on ischaemic heart disease: analysis of data from the randomised, controlled ACCORD trial. Lancet. 2014;384(9958):1936–1941.
A13. Ikeda Y, Shimada K, Teramoto T, et al. Low-dose aspirin for primary prevention of cardiovascular events in Japanese patients 60 years or older with atherosclerotic risk factors: a randomized clinical trial. JAMA. 2014;312(23):2510–2520.
Musculoskeletal Disease
Table 1 summarizes clinical actions to consider for the treatment of musculoskeletal disease, including meniscal tears, spinal stenosis, and knee degenerative joint disease.11–17
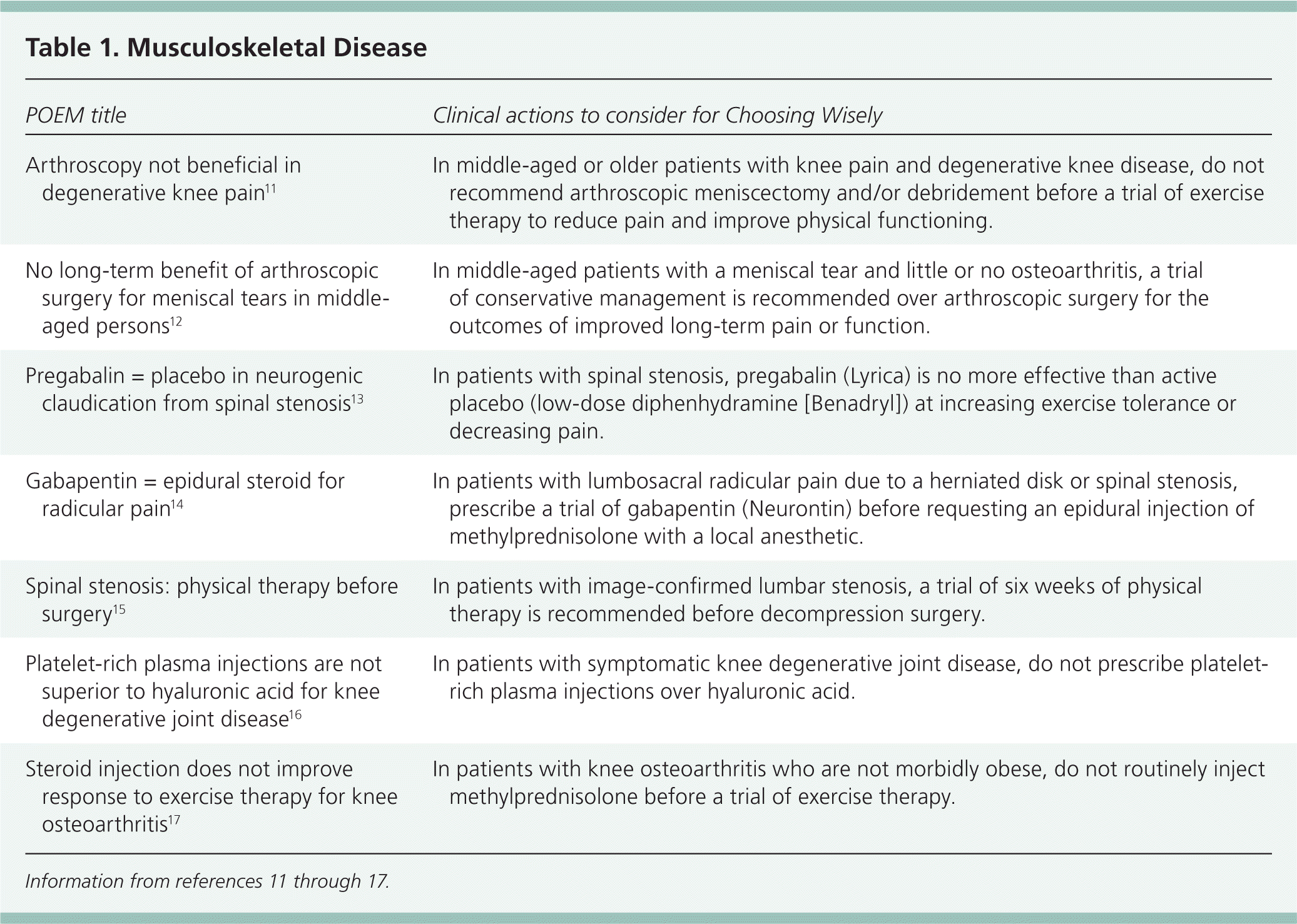
Table 1. Musculoskeletal Disease
| POEM title | Clinical actions to consider for Choosing Wisely |
|---|---|
| Arthroscopy not beneficial in degenerative knee pain11 | In middle-aged or older patients with knee pain and degenerative knee disease, do not recommend arthroscopic meniscectomy and/or debridement before a trial of exercise therapy to reduce pain and improve physical functioning. |
| No long-term benefit of arthroscopic surgery for meniscal tears in middle-aged persons12 | In middle-aged patients with a meniscal tear and little or no osteoarthritis, a trial of conservative management is recommended over arthroscopic surgery for the outcomes of improved long-term pain or function. |
| Pregabalin = placebo in neurogenic claudication from spinal stenosis13 | In patients with spinal stenosis, pregabalin (Lyrica) is no more effective than active placebo (low-dose diphenhydramine [Benadryl]) at increasing exercise tolerance or decreasing pain. |
| Gabapentin = epidural steroid for radicular pain14 | In patients with lumbosacral radicular pain due to a herniated disk or spinal stenosis, prescribe a trial of gabapentin (Neurontin) before requesting an epidural injection of methylprednisolone with a local anesthetic. |
| Spinal stenosis: physical therapy before surgery15 | In patients with image-confirmed lumbar stenosis, a trial of six weeks of physical therapy is recommended before decompression surgery. |
| Platelet-rich plasma injections are not superior to hyaluronic acid for knee degenerative joint disease16 | In patients with symptomatic knee degenerative joint disease, do not prescribe platelet-rich plasma injections over hyaluronic acid. |
| Steroid injection does not improve response to exercise therapy for knee osteoarthritis17 | In patients with knee osteoarthritis who are not morbidly obese, do not routinely inject methylprednisolone before a trial of exercise therapy. |
MENISCAL TEARS
Findings from the top POEMs of 2015 raise doubt about the value of surgical intervention for nontraumatic meniscal tear in middle-aged persons. In two separate meta-analyses of randomized trials, meniscectomy was reported to be ineffective for the long-term outcomes of pain or function, regardless of whether the patient had radiographic evidence of osteoarthritis.11,12 Therefore, arthroscopic meniscectomy and debridement should not be recommended before an adequate trial of exercise therapy, reserving surgery only for patients with persistent pain or functional limitations, such as limited range of motion.
SPINAL STENOSIS
There is little evidence to support the use of pregabalin (Lyrica) for the neuropathic pain of spinal stenosis. In a trial of 29 patients with spinal stenosis and radicular or walking-induced pain, pregabalin was no more effective than low-dose diphenhydramine (Benadryl; an active placebo).13 In a separate trial, gabapentin (Neurontin) titrated to between 1,800 and 3,600 mg per day was as effective as an epidural steroid injection in the short-term (three months).14 These results could indicate that steroid injections and gabapentin are modestly effective but short-lived, that neither are effective and provide a placebo effect, or that the study lacked power to demonstrate that epidural injections are superior to gabapentin. Given the similarities between pregabalin and gabapentin, one wonders if both drugs reduce the neuropathic pain of spinal stenosis via a placebo effect. Until we have more data on the best conservative therapies for spinal stenosis, the most reasonable option may be a trial of gabapentin, physical therapy, or both before requesting an epidural injection.15
KNEE DEGENERATIVE JOINT DISEASE
In symptomatic patients with knee degenerative joint disease, those who received platelet-rich plasma injections were no better off in terms of symptoms and function score compared with those who received hyaluronic acid.16 Although the study concluded that both treatments are effective, previous studies question the benefit of hyaluronic acid injections.18 Another study found that injections of methylprednisolone cannot be routinely recommended to enhance patients' ability to participate in exercise therapy.17
Cardiovascular Disease
Table 2 summarizes clinical actions to consider for the treatment of cardiovascular disease, including beta-blocker therapy, dual antiplatelet therapy, and screening for coronary artery disease in patients with diabetes mellitus.19–22
Table 2. Cardiovascular Disease

| POEM title | Clinical actions to consider for Choosing Wisely |
|---|---|
| Post-MI beta blockers do not decrease mortality19 | In patients receiving optimal chronic treatment after an MI, do not prescribe a beta blocker to improve overall survival beyond 30 days. |
| More than one year of dual antiplatelet therapy after stent more harmful than beneficial20 | In patients with drug-eluting stents who did not experience a coronary event during the first year, do not prescribe dual antiplatelet therapy beyond one year. |
| No benefit to screening with CT angiography for asymptomatic CAD in adults with diabetes21 | In adults with type 1 or type 2 diabetes mellitus and no indication of existing CAD, do not request coronary CT angiography to screen for this condition. |
| Adding sitagliptin does not reduce or increase the risk of cardiovascular outcomes22 | In patients with type 2 diabetes, do not prescribe sitagliptin (Januvia) to reduce the risk of cardiovascular events. |
CAD = coronary artery disease; CT = computed tomography; MI = myocardial infarction.
BETA BLOCKERS AFTER MYOCARDIAL INFARCTION
Although recommended by guidelines and used as a quality indicator of hospital care, the use of beta blockers after myocardial infarction, when combined with optimal contemporary acute and chronic treatment, does not provide a further survival benefit. In a meta-analysis, the early use of beta blockers reduced subsequent reinfarction and angina symptoms, but these benefits began to wane within 30 days.19 Thus, in the era of statins, anti-platelet agents, and stents, beta blockers do not appear to confer a benefit beyond 30 days.
DUAL ANTIPLATELET THERAPY AFTER DRUG-ELUTING STENTS
Among patients treated with drug-eluting stents who do not experience a coronary event during the first year, continuing dual antiplatelet therapy beyond one year provides no additional benefit. When the data from this study are pooled with those from other studies, they not only show a lack of benefit but also demonstrate more frequent serious bleeding.20
CORONARY ARTERY DISEASE
Diabetes is an important risk factor for cardiovascular events and mortality. However, screening for coronary artery disease in asymptomatic adults with diabetes (types 1 or 2) using coronary computed tomography (CT) angiography does not improve outcomes vs. standard care.21 A study evaluating the safety of sitagliptin (Januvia) added to the drug regimen of patients with a mean A1C level of 7.2% revealed that sitagliptin did not increase cardiovascular events, but, more importantly, it did not decrease their risk of such events either.22
Anticoagulation and Venous Thromboembolism
Table 3 summarizes clinical actions to consider for managing bridging anticoagulation and screening for occult malignancy in patients with venous thromboembolism.23–26
Table 3. Anticoagulant Therapy/Venous Thromboembolism

| POEM title | Clinical actions to consider for Choosing Wisely |
|---|---|
| More harm than good with bridge therapy in low-risk venous thromboembolism patients23 | In patients with venous thromboembolism, especially those already at low risk of recurrence, do not prescribe bridge anticoagulant therapy during the warfarin (Coumadin) interruption period. |
| Bridging anticoagulation in patients with atrial fibrillation associated with more cardiovascular events and bleeding24 | In patients with atrial fibrillation who are receiving anticoagulation therapy and are undergoing a surgical procedure, do not provide bridging anticoagulation. |
| Perioperative bridging anticoagulation unhelpful for invasive procedures25 | In patients with atrial fibrillation who undergo an elective invasive procedure, do not prescribe bridging anticoagulation. |
| Routine CT scans for occult malignancy not useful in patients with unprovoked venous thromboembolism26 | In patients with unprovoked venous thromboembolism, do not request CT of the abdomen and pelvis to detect occult malignancy. |
CT = computed tomography.
BRIDGING ANTICOAGULATION
Does the inconvenience of complicated bridging anticoagulation regimens really improve outcomes? An increasing body of literature questions the value of bridging or finds net harm. In 2015, two observational studies reported associations between bridging therapy and an increased risk of bleeding and cardiovascular events. Moreover, withholding bridging therapy is not associated with an increased risk of recurrent venous thromboembolism, suggesting that bridging anticoagulation should not be routinely recommended for patients with venous thromboembolism, especially those at low risk of recurrence.23 In patients with nonvalvular atrial fibrillation, bridging anticoagulation was associated with a higher risk of bleeding complications and cardiovascular events.24
Observational studies such as these do not allow for causal inference. For this reason, the best evidence to date comes from a trial of adults with chronic atrial fibrillation and at least one CHADS2 risk factor (congestive heart failure, hypertension, age 75 years or older, diabetes, and stroke or transient ischemic attack).25 Patients who underwent an elective invasive procedure were randomized to bridging anticoagulation with dalteparin (Fragmin) or placebo. Patients with a mechanical heart valve, recent stroke or embolism, impaired renal function, or thrombocytopenia were excluded. Bridging anticoagulation worsened outcomes for patients, resulting in more episodes of major bleeding and no difference in the rate of stroke or venous thromboembolism. Of note, the patients were largely undergoing minor surgical procedures with low bleeding risk; patients at very high risk of thromboembolism or stroke were not represented in this study.
SCREENING FOR OCCULT MALIGNANCY IN THE CONTEXT OF VENOUS THROMBOEMBOLISM
An example of overtesting comes from a trial of adults with an initial diagnosis of deep venous thrombosis or pulmonary embolism. At each of nine centers, patients were randomized to receive a basic evaluation for occult malignancy (history and physical examination, basic blood tests, chest radiography, mammography for women older than 50 years, Papanicolaou test for sexually active women 18 to 70 years of age, and prostate cancer screening for men older than 40 years) or the same evaluation plus a comprehensive CT of the abdomen and pelvis. Overall, 33 patients (3.9%) had a new diagnosis of cancer during the first year of follow-up, with no significant difference between groups: 14 in the basic screening group and 19 in the group that also received a CT scan. The mean time to a new cancer diagnosis was 4.2 months for the patients who received basic screening and four months for those who also received CT. Therefore, there is no advantage to adding CT of the abdomen and pelvis to a basic screening protocol for occult malignancy in patients with unprovoked venous thromboembolism.26
Miscellaneous
VITAMIN D
In postmenopausal women (average age of 61 years) at low risk of falls, vitamin D supplementation—even in those with low levels of the vitamin—did not improve bone mineral density, muscle mass, or strength, and did not reduce the risk of falls (Table 4).27 Of note, the women took daily (800 IU) or twice-monthly (50,000 IU) vitamin D3 supplements. Not routinely screening for low vitamin D levels will make it easier to avoid ineffective supplementation.
Table 4. Miscellaneous

| POEM title | Clinical actions to consider for Choosing Wisely |
|---|---|
| Treating low vitamin D levels is ineffective in postmenopausal women27 | In typical community-dwelling postmenopausal women younger than 75 years, do not prescribe vitamin D to improve bone mineral density, muscle strength, functional status, or risk of falls. |
Information from reference 27.
editor's note: This article was cowritten by Dr. Mark Ebell, Deputy Editor for AFP and cofounder and Editor-in-Chief of Essential Evidence Plus, published by Wiley-Blackwell, Inc. Because of Dr. Ebell's dual roles and ties to Essential Evidence Plus, the article underwent peer review and editing by four of AFP's medical editors. Dr. Ebell was not involved in the editorial decision-making process.—Jay Siwek, MD, Editor, American Family Physician

