Key components of the pretravel consultation include intake questions regarding the traveler's anticipated itinerary and medical history; immunizations; malaria prophylaxis; and personal protection measures against arthropod bites, traveler's diarrhea, and injury. Most vaccinations that are appropriate for international travelers are included in the routine domestic immunization schedule; only a few travel-specific vaccines must also be discussed. The most common vaccine-preventable illnesses in international travelers are influenza and hepatitis A. Malaria prophylaxis should be offered to travelers to endemic regions. Personal protection measures, such as applying an effective insect repellent to exposed skin and permethrin to clothing and using a permethrin-impregnated bed net, should be advised for travelers to the tropics. Clinicians should offer an antibiotic prescription that travelers can take with them in case of traveler's diarrhea. Additional topics to address during the pretravel consultation include the risk of injury from motor vehicle crashes and travel-specific risks such as altitude sickness, safe sex practices, and emergency medical evacuation insurance.
Data show that 1.1 billion persons crossed an international border in 2014, and this number is projected to increase to 1.8 billion persons in 2025.1 Tourism is increasing in both high- and low-income destinations, and is the first- or second-largest source of revenue in 20 of the 48 least developed countries.2
WHAT'S NEW ON THIS TOPIC: THE PRETRAVEL CONSULTATION
Pregnant women and women of childbearing age who are trying to conceive should postpone travel to Zika-endemic areas. If they do visit these areas, they should be vigilant about arthropod avoidance measures. Because Zika is also transmitted by sex, men who visit Zika-endemic areas should use condoms with pregnant sex partners.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| International travelers should receive routine domestic immunizations as well as travel-specific immunizations to reduce the risk of illness and death from vaccine-preventable diseases. | A | 15, 16 |
| Use of personal protection measures, including applying DEET or picaridin on exposed skin and permethrin on clothing, and using a permethrin-impregnated bed net, reduces risk from arthropod-borne illnesses (e.g., malaria, dengue fever) in travelers. | C | 18, 19, 22 |
| Travelers to endemic regions should receive malaria prophylaxis. | A | 24, 25 |
| A short course of antibiotics reduces the duration of traveler's diarrhea. | A | 34, 35 |
DEET = diethyltoluamide.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Only a minority of international travelers—36% in one study—seek pretravel counseling; of those, 60% see a primary care clinician, 10% see a travel subspecialist, and 30% turn to friends and family.3 Although research supports some portions of the pretravel encounter (e.g., malaria prophylaxis, immunizations), the benefit of counseling on other topics (e.g., motor vehicle crashes, safe sex) has not yet been demonstrated.4
Although consulting a clinician is beneficial to patients at any time before international travel, pretravel visits should ideally occur at least six weeks before departure to maximize benefit of immunizations and other preventive measures. The pretravel consultation is likely to be particularly useful in those visiting low-income nations.
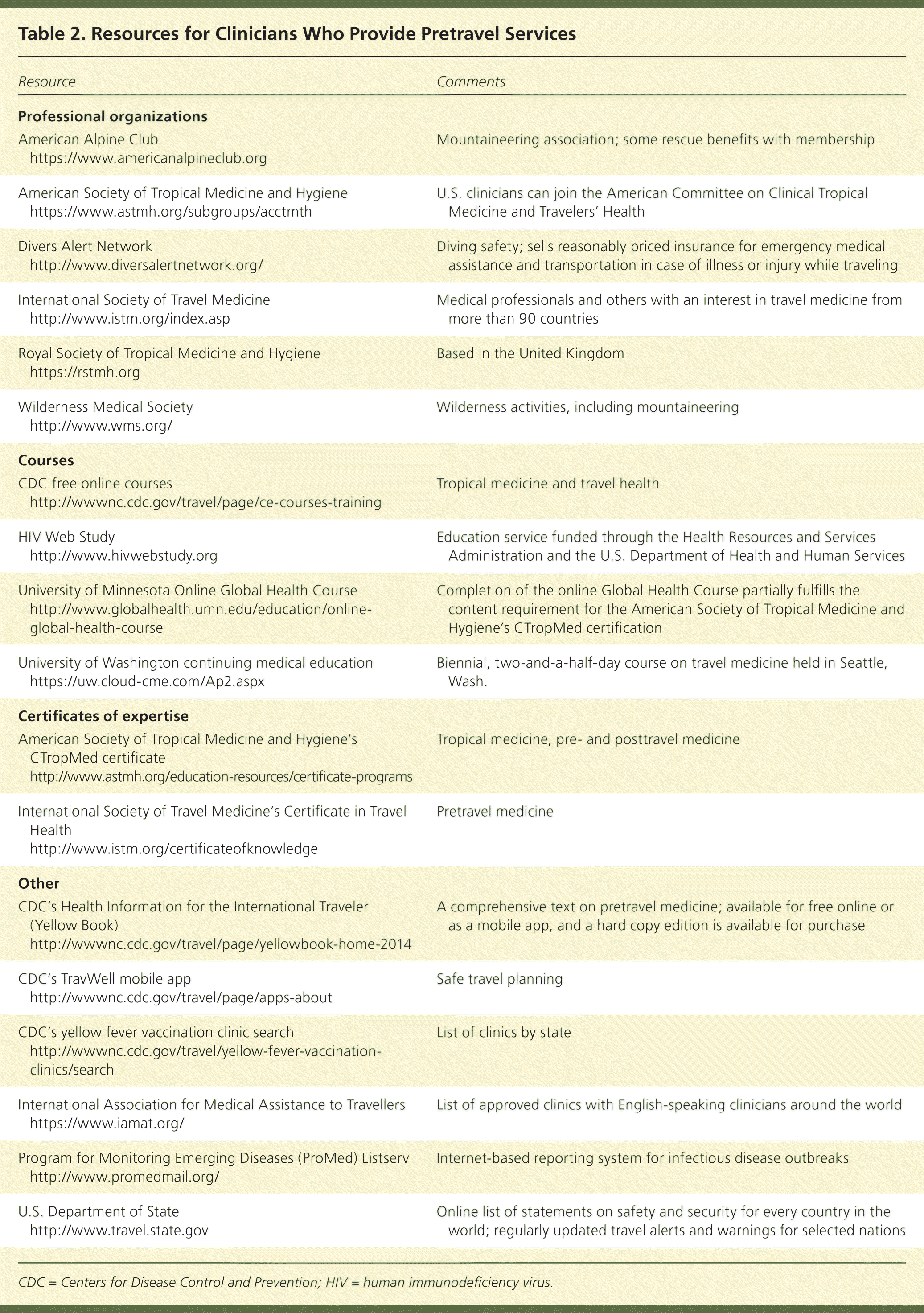
Table 1 outlines the recommended components of the pretravel consultation,5,6 and Table 2 provides resources for clinicians who provide pretravel services. Physicians who perform pretravel consultations only occasionally or who have minimal training in travel medicine may want to refer complex cases to a clinician experienced in travel medicine.
Table 1. Recommended Components of the Pretravel Consultation

| Assessment |
| Upcoming trip: dates, itinerary, reason for trip, travel style, special activities (e.g., mountain climbing, diving, rafting) |
| Medical history: medications, allergies, surgeries, hospitalizations, special conditions (e.g., pregnancy, breastfeeding, recent myocardial infarction or cerebrovascular accident, immunocompromise, psychiatric condition), immunizations, prior experience with malaria prophylaxis, illnesses related to travel |
| Immunizations |
| Routine (eTable A) |
| Travel-specific (e.g., typhoid fever, yellow fever, Japanese encephalitis, rabies, cholera) |
| Arthropod-borne disease risk reduction |
| Personal protection measures (applying insect repellent, such as DEET or picaridin, to exposed skin and permethrin to clothing; sleeping under a permethrin-impregnated bed net) |
| Malaria prophylaxis |
| Traveler's diarrhea |
| Risk reduction (e.g., hand washing, cautious food and drink selection) |
| Carry-along medication, such as an antibiotic and antimotility agent (e.g., loperamide [Imodium]), for as-needed self-treatment |
| Counseling for further risk reduction |
| Avoidance of motor vehicle crashes, deep venous thrombosis, high-altitude illness, drowning |
| Crime, security |
| Emergency evacuation insurance |
| Safe sex practices |
| Sun protection |
| Traveler resources |
DEET = diethyltoluamide.
Table 2. Resources for Clinicians Who Provide Pretravel Services
| Resource | Comments | |
|---|---|---|
| Professional organizations | ||
| American Alpine Club | Mountaineering association; some rescue benefits with membership | |
| https://www.americanalpineclub.org | ||
| American Society of Tropical Medicine and Hygiene | U.S. clinicians can join the American Committee on Clinical Tropical Medicine and Travelers' Health | |
| https://www.astmh.org/subgroups/acctmth | ||
| Divers Alert Network | Diving safety; sells reasonably priced insurance for emergency medical assistance and transportation in case of illness or injury while traveling | |
| http://www.diversalertnetwork.org/ | ||
| International Society of Travel Medicine | Medical professionals and others with an interest in travel medicine from more than 90 countries | |
| http://www.istm.org/index.asp | ||
| Royal Society of Tropical Medicine and Hygiene | Based in the United Kingdom | |
| https://rstmh.org | ||
| Wilderness Medical Society | Wilderness activities, including mountaineering | |
| http://www.wms.org/ | ||
| Courses | ||
| CDC free online courses | Tropical medicine and travel health | |
| http://wwwnc.cdc.gov/travel/page/ce-courses-training | ||
| HIV Web Study | Education service funded through the Health Resources and Services Administration and the U.S. Department of Health and Human Services | |
| http://www.hivwebstudy.org | ||
| University of Minnesota Online Global Health Course | Completion of the online Global Health Course partially fulfills the content requirement for the American Society of Tropical Medicine and Hygiene's CTropMed certification | |
| http://www.globalhealth.umn.edu/education/online-global-health-course | ||
| University of Washington continuing medical education | Biennial, two-and-a-half-day course on travel medicine held in Seattle, Wash. | |
| https://uw.cloud-cme.com/Ap2.aspx | ||
| Certificates of expertise | ||
| American Society of Tropical Medicine and Hygiene's CTropMed certificate | Tropical medicine, pre- and posttravel medicine | |
| http://www.astmh.org/education-resources/certificate-programs | ||
| International Society of Travel Medicine's Certificate in Travel Health | Pretravel medicine | |
| http://www.istm.org/certificateofknowledge | ||
| Other | ||
| CDC's Health Information for the International Traveler (Yellow Book) | A comprehensive text on pretravel medicine; available for free online or as a mobile app, and a hard copy edition is available for purchase | |
| http://wwwnc.cdc.gov/travel/page/yellowbook-home-2014 | ||
| CDC's TravWell mobile app | Safe travel planning | |
| http://wwwnc.cdc.gov/travel/page/apps-about | ||
| CDC's yellow fever vaccination clinic search | List of clinics by state | |
| http://wwwnc.cdc.gov/travel/yellow-fever-vaccination-clinics/search | ||
| International Association for Medical Assistance to Travellers | List of approved clinics with English-speaking clinicians around the world | |
| https://www.iamat.org/ | ||
| Program for Monitoring Emerging Diseases (ProMed) Listserv | Internet-based reporting system for infectious disease outbreaks | |
| http://www.promedmail.org/ | ||
| U.S. Department of State | Online list of statements on safety and security for every country in the world; regularly updated travel alerts and warnings for selected nations | |
| http://www.travel.state.gov | ||
CDC = Centers for Disease Control and Prevention; HIV = human immunodeficiency virus.
Assessment
The assessment should include dates of travel, anticipated itinerary, planned activities, mode of travel, and reason for travel. Additionally, clinicians should inquire about the traveler's acceptance level for health risks and budget for health care expenditures.
A full medical history should be elicited from the traveler, including immunization records, medications, allergies, and medical conditions. Certain conditions, if uncontrolled, may increase health risks in travelers and include congestive heart failure, hypertension, seizures, diabetes mellitus, and mental illness. Clinicians may recommend against particular trips or activities if they exceed the traveler's physical abilities or if there is a specific contraindication. Persons who have had a myocardial infarction or coronary artery bypass within the previous two weeks, or a complicated myocardial infarction within the previous six weeks,7 are thought to be at higher risk of cardiovascular events when flying. Prior use of antimalarials and any adverse effects experienced should be recorded. Physicians should ask women about pregnancy status and birth control method, if applicable.
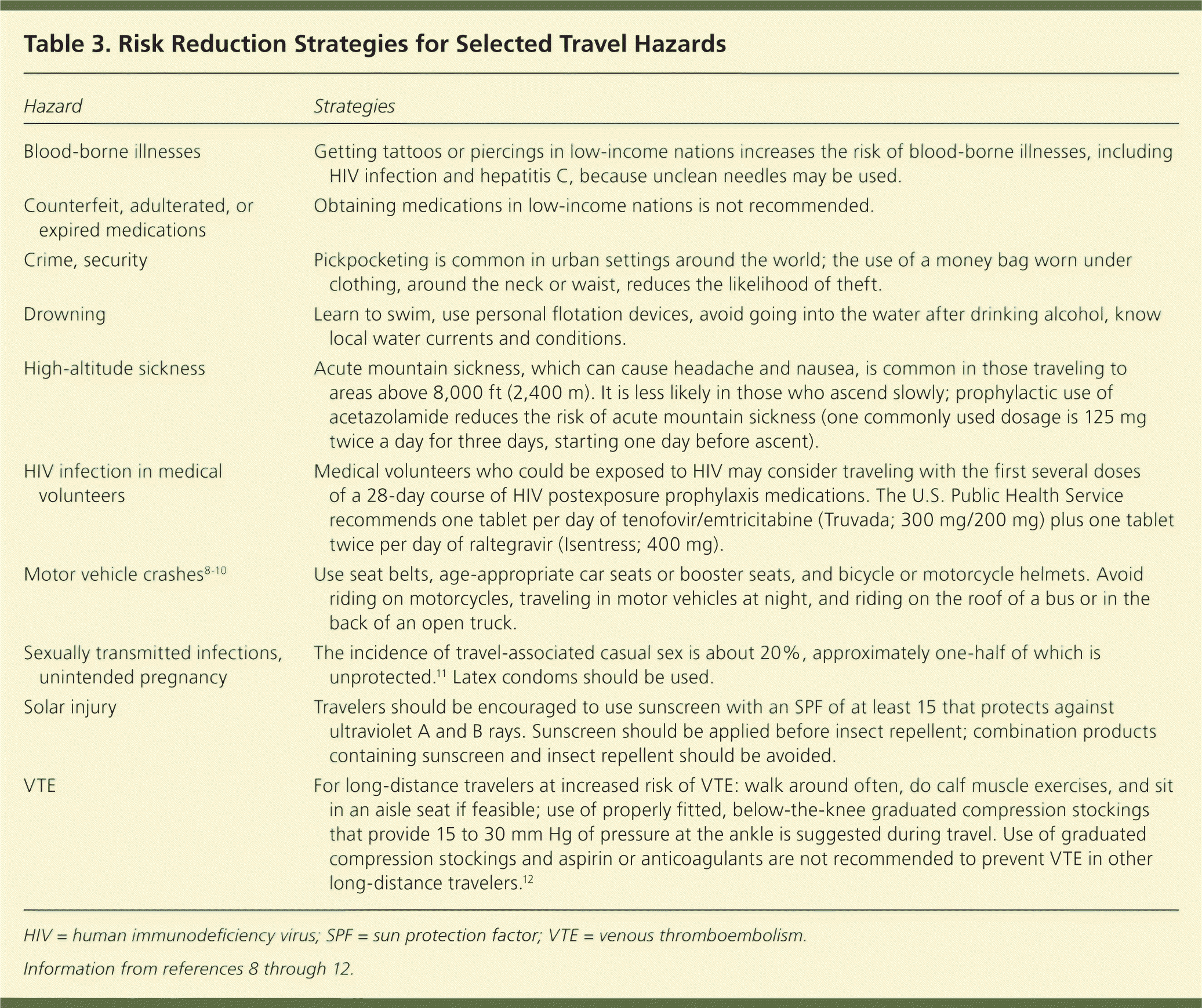
Table 3. Risk Reduction Strategies for Selected Travel Hazards
| Hazard | Strategies |
|---|---|
| Blood-borne illnesses | Getting tattoos or piercings in low-income nations increases the risk of blood-borne illnesses, including HIV infection and hepatitis C, because unclean needles may be used. |
| Counterfeit, adulterated, or expired medications | Obtaining medications in low-income nations is not recommended. |
| Crime, security | Pickpocketing is common in urban settings around the world; the use of a money bag worn under clothing, around the neck or waist, reduces the likelihood of theft. |
| Drowning | Learn to swim, use personal flotation devices, avoid going into the water after drinking alcohol, know local water currents and conditions. |
| High-altitude sickness | Acute mountain sickness, which can cause headache and nausea, is common in those traveling to areas above 8,000 ft (2,400 m). It is less likely in those who ascend slowly; prophylactic use of acetazolamide reduces the risk of acute mountain sickness (one commonly used dosage is 125 mg twice a day for three days, starting one day before ascent). |
| HIV infection in medical volunteers | Medical volunteers who could be exposed to HIV may consider traveling with the first several doses of a 28-day course of HIV postexposure prophylaxis medications. The U.S. Public Health Service recommends one tablet per day of tenofovir/emtricitabine (Truvada; 300 mg/200 mg) plus one tablet twice per day of raltegravir (Isentress; 400 mg). |
| Motor vehicle crashes8–10 | Use seat belts, age-appropriate car seats or booster seats, and bicycle or motorcycle helmets. Avoid riding on motorcycles, traveling in motor vehicles at night, and riding on the roof of a bus or in the back of an open truck. |
| Sexually transmitted infections, unintended pregnancy | The incidence of travel-associated casual sex is about 20%, approximately one-half of which is unprotected.11 Latex condoms should be used. |
| Solar injury | Travelers should be encouraged to use sunscreen with an SPF of at least 15 that protects against ultraviolet A and B rays. Sunscreen should be applied before insect repellent; combination products containing sunscreen and insect repellent should be avoided. |
| VTE | For long-distance travelers at increased risk of VTE: walk around often, do calf muscle exercises, and sit in an aisle seat if feasible; use of properly fitted, below-the-knee graduated compression stockings that provide 15 to 30 mm Hg of pressure at the ankle is suggested during travel. Use of graduated compression stockings and aspirin or anticoagulants are not recommended to prevent VTE in other long-distance travelers.12 |
HIV = human immunodeficiency virus; SPF = sun protection factor; VTE = venous thromboembolism.
Noninfectious Risks
The most common cause of death in nonelderly international travelers is motor vehicle crashes, which account for 18% to 24% of deaths in all travelers. Deaths from motor vehicle crashes are markedly more common in low-income nations. Other common causes of death in travelers include violence (e.g., homicide, suicide) and drowning.13,14
Immunization-Preventable Diseases
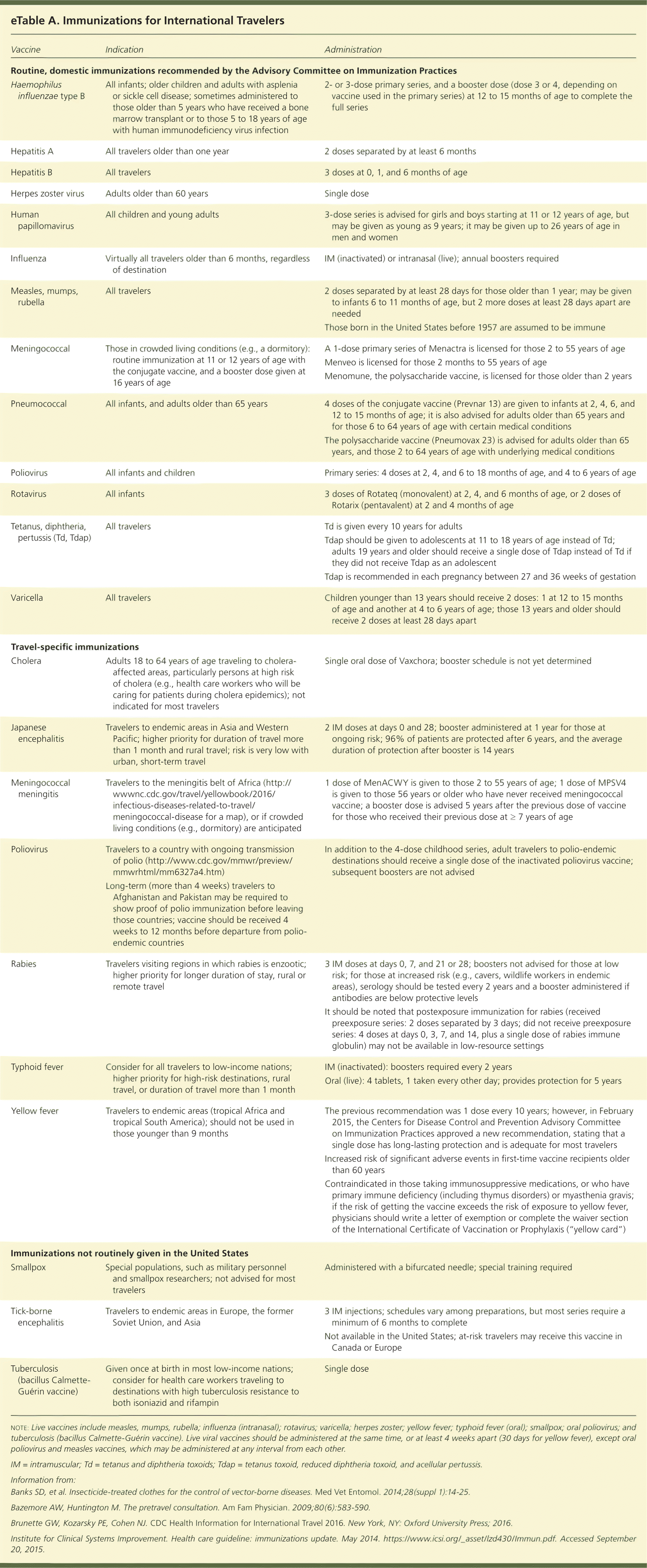
eTable A summarizes immunizations recommended for international travelers. Live vaccines should be avoided in travelers who are pregnant or immunocompromised.
eTable A. Immunizations for International Travelers
| Vaccine | Indication | Administration |
|---|---|---|
| Routine, domestic immunizations recommended by the Advisory Committee on Immunization Practices | ||
| Haemophilus influenzae type B | All infants; older children and adults with asplenia or sickle cell disease; sometimes administered to those older than 5 years who have received a bone marrow transplant or to those 5 to 18 years of age with human immunodeficiency virus infection | 2- or 3-dose primary series, and a booster dose (dose 3 or 4, depending on vaccine used in the primary series) at 12 to 15 months of age to complete the full series |
| Hepatitis A | All travelers older than one year | 2 doses separated by at least 6 months |
| Hepatitis B | All travelers | 3 doses at 0, 1, and 6 months of age |
| Herpes zoster virus | Adults older than 60 years | Single dose |
| Human papillomavirus | All children and young adults | 3-dose series is advised for girls and boys starting at 11 or 12 years of age, but may be given as young as 9 years; it may be given up to 26 years of age in men and women |
| Influenza | Virtually all travelers older than 6 months, regardless of destination | IM (inactivated) or intranasal (live); annual boosters required |
| Measles, mumps, rubella | All travelers | 2 doses separated by at least 28 days for those older than 1 year; may be given to infants 6 to 11 months of age, but 2 more doses at least 28 days apart are needed |
| Those born in the United States before 1957 are assumed to be immune | ||
| Meningococcal | Those in crowded living conditions (e.g., a dormitory): routine immunization at 11 or 12 years of age with the conjugate vaccine, and a booster dose given at 16 years of age | A 1-dose primary series of Menactra is licensed for those 2 to 55 years of age |
| Menveo is licensed for those 2 months to 55 years of age | ||
| Menomune, the polysaccharide vaccine, is licensed for those older than 2 years | ||
| Pneumococcal | All infants, and adults older than 65 years | 4 doses of the conjugate vaccine (Prevnar 13) are given to infants at 2, 4, 6, and 12 to 15 months of age; it is also advised for adults older than 65 years and for those 6 to 64 years of age with certain medical conditions |
| The polysaccharide vaccine (Pneumovax 23) is advised for adults older than 65 years, and those 2 to 64 years of age with underlying medical conditions | ||
| Poliovirus | All infants and children | Primary series: 4 doses at 2, 4, and 6 to 18 months of age, and 4 to 6 years of age |
| Rotavirus | All infants | 3 doses of Rotateq (monovalent) at 2, 4, and 6 months of age, or 2 doses of Rotarix (pentavalent) at 2 and 4 months of age |
| Tetanus, diphtheria, pertussis (Td, Tdap) | All travelers | Td is given every 10 years for adults |
| Tdap should be given to adolescents at 11 to 18 years of age instead of Td; adults 19 years and older should receive a single dose of Tdap instead of Td if they did not receive Tdap as an adolescent | ||
| Tdap is recommended in each pregnancy between 27 and 36 weeks of gestation | ||
| Varicella | All travelers | Children younger than 13 years should receive 2 doses: 1 at 12 to 15 months of age and another at 4 to 6 years of age; those 13 years and older should receive 2 doses at least 28 days apart |
| Travel-specific immunizations | ||
| Cholera | Adults 18 to 64 years of age traveling to cholera-affected areas, particularly persons at high risk of cholera (e.g., health care workers who will be caring for patients during cholera epidemics); not indicated for most travelers | Single oral dose of Vaxchora; booster schedule is not yet determined |
| Japanese encephalitis | Travelers to endemic areas in Asia and Western Pacific; higher priority for duration of travel more than 1 month and rural travel; risk is very low with urban, short-term travel | 2 IM doses at days 0 and 28; booster administered at 1 year for those at ongoing risk; 96% of patients are protected after 6 years, and the average duration of protection after booster is 14 years |
| Meningococcal meningitis | Travelers to the meningitis belt of Africa ( http://wwwnc.cdc.gov/travel/yellowbook/2016/infectious-diseases-related-to-travel/meningococcal-disease for a map), or if crowded living conditions (e.g., dormitory) are anticipated | 1 dose of MenACWY is given to those 2 to 55 years of age; 1 dose of MPSV4 is given to those 56 years or older who have never received meningococcal vaccine; a booster dose is advised 5 years after the previous dose of vaccine for those who received their previous dose at ≥ 7 years of age |
| Poliovirus | Travelers to a country with ongoing transmission of polio ( http://www.cdc.gov/mmwr/preview/mmwrhtml/mm6327a4.htm) | In addition to the 4-dose childhood series, adult travelers to polio-endemic destinations should receive a single dose of the inactivated poliovirus vaccine; subsequent boosters are not advised |
| Long-term (more than 4 weeks) travelers to Afghanistan and Pakistan may be required to show proof of polio immunization before leaving those countries; vaccine should be received 4 weeks to 12 months before departure from polio-endemic countries | ||
| Rabies | Travelers visiting regions in which rabies is enzootic; higher priority for longer duration of stay, rural or remote travel | 3 IM doses at days 0, 7, and 21 or 28; boosters not advised for those at low risk; for those at increased risk (e.g., cavers, wildlife workers in endemic areas), serology should be tested every 2 years and a booster administered if antibodies are below protective levels |
| It should be noted that postexposure immunization for rabies (received preexposure series: 2 doses separated by 3 days; did not receive preexposure series: 4 doses at days 0, 3, 7, and 14, plus a single dose of rabies immune globulin) may not be available in low-resource settings | ||
| Typhoid fever | Consider for all travelers to low-income nations; higher priority for high-risk destinations, rural travel, or duration of travel more than 1 month | IM (inactivated): boosters required every 2 years |
| Oral (live): 4 tablets, 1 taken every other day; provides protection for 5 years | ||
| Yellow fever | Travelers to endemic areas (tropical Africa and tropical South America); should not be used in those younger than 9 months | The previous recommendation was 1 dose every 10 years; however, in February 2015, the Centers for Disease Control and Prevention Advisory Committee on Immunization Practices approved a new recommendation, stating that a single dose has long-lasting protection and is adequate for most travelers |
| Increased risk of significant adverse events in first-time vaccine recipients older than 60 years | ||
| Contraindicated in those taking immunosuppressive medications, or who have primary immune deficiency (including thymus disorders) or myasthenia gravis; if the risk of getting the vaccine exceeds the risk of exposure to yellow fever, physicians should write a letter of exemption or complete the waiver section of the International Certificate of Vaccination or Prophylaxis (“yellow card”) | ||
| Immunizations not routinely given in the United States | ||
| Smallpox | Special populations, such as military personnel and smallpox researchers; not advised for most travelers | Administered with a bifurcated needle; special training required |
| Tick-borne encephalitis | Travelers to endemic areas in Europe, the former Soviet Union, and Asia | 3 IM injections; schedules vary among preparations, but most series require a minimum of 6 months to complete |
| Not available in the United States; at-risk travelers may receive this vaccine in Canada or Europe | ||
| Tuberculosis (bacillus Calmette-Guérin vaccine) | Given once at birth in most low-income nations; consider for health care workers traveling to destinations with high tuberculosis resistance to both isoniazid and rifampin | Single dose |
note: Live vaccines include measles, mumps, rubella; influenza (intranasal); rotavirus; varicella; herpes zoster; yellow fever; typhoid fever (oral); smallpox; oral poliovirus; and tuberculosis (bacillus Calmette-Guérin vaccine). Live viral vaccines should be administered at the same time, or at least 4 weeks apart (30 days for yellow fever), except oral poliovirus and measles vaccines, which may be administered at any interval from each other.
IM = intramuscular; Td = tetanus and diphtheria toxoids; Tdap = tetanus toxoid, reduced diphtheria toxoid, and acellular pertussis.
Information from:
Banks SD, et al. Insecticide-treated clothes for the control of vector-borne diseases. Med Vet Entomol. 2014;28(suppl 1):14–25.
Bazemore AW, Huntington M. The pretravel consultation. Am Fam Physician. 2009;80(6):583–590.
Brunette GW, Kozarsky PE, Cohen NJ. CDC Health Information for International Travel 2016. New York, NY: Oxford University Press; 2016.
Institute for Clinical Systems Improvement. Health care guideline: immunizations update. May 2014. https://www.icsi.org/_asset/lzd430/Immun.pdf. Accessed September 20, 2015.
ROUTINE VACCINES
In general, the diseases on the routine domestic immunization schedule are more common in travelers than are the travel-specific illnesses; hence, travelers should be up to date on the routine vaccines recommended by the Advisory Committee on Immunization Practices. The most common vaccine-preventable illnesses in international travelers are influenza and hepatitis A. The influenza season is between April and September in the southern hemisphere, and it occurs year-round in locations near the equator. Immunization for influenza should be advised when available. Hepatitis A, transmitted by contaminated food and water, is ubiquitous in low-income nations, and the vaccine is appropriate for all travelers older than one year.15
TRAVEL-SPECIFIC VACCINES
Travel-specific immunizations include those for typhoid fever,16 yellow fever, Japanese encephalitis, rabies, and cholera. Travelers may be required to show proof of vaccination for yellow fever to enter or return from nations within endemic regions (tropical Africa and tropical South America). Physicians should document yellow fever vaccination on travelers' International Certificate of Vaccination or Prophylaxis (“yellow card,” as approved by the World Health Organization). An example of the vaccine certificate is available at http://www.who.int/ihr/IVC200_06_26.pdf?ua=1. If travelers have a contraindication to the yellow fever immunization, clinicians should write a letter of exemption or complete the waiver section of the vaccine certificate; these are generally accepted at international borders. Travelers to Saudi Arabia for the annual hajj and umrah (Muslim pilgrimage) are required to show proof of immunization for meningococcal meningitis.
Protection Against Insects and Other Arthropods
PERSONAL PROTECTION MEASURES
It is important to stress to travelers that taking antimalarials does not negate the need for personal protection measures (Table 417 ), which guard against malaria and numerous other arthropod-borne diseases (e.g., dengue fever, a common illness in most tropical countries).18,19
Table 4. Personal Protection Measures Against Arthropod-Borne Diseases

| Measure | Comments |
|---|---|
| Insect repellent applied to exposed skin | The most effective insect repellents contain 20% to 50% DEET or 20% picaridin. |
| DEET should be avoided in infants two months and younger. Picaridin does not have the petrochemical odor of DEET and may be better tolerated by children and travelers sensitive to the odor. | |
| Other effective options are oil of lemon eucalyptus (PMD) and IR3535 (available as Skin-So-Soft Bug Guard Plus IR3535 lotion). IR3535 does not provide adequate protection against Anopheles mosquitoes and should not be used in malaria-endemic areas. | |
| Insect repellent should not be applied onto or under clothing; regular reapplication is important. | |
| Permethrin applied to clothing | Travelers may apply permethrin to clothing or purchase clothing pretreated with permethrin. It should be applied to outer clothing only and not to underwear. |
| Bed nets | A bed net is most effective when impregnated with permethrin. The bed net should reach the floor or be tucked under the mattress to provide a seal. |
| Activity modification | Outdoor activities should be avoided during dusk, nighttime, and dawn hours when mosquitos are more active. |
| Checking for ticks | Travelers should inspect their bodies and clothing after outdoor activity and at the end of the day with the aid of a mirror or companion. |
| Climate modification | Air-conditioning reduces the risk of malaria; malaria transmission usually occurs between 77°F (25°C) and 86°F (30°C). |
| Long sleeves and pants | Wearing long sleeves, tucking the shirt into pants, tucking pants into socks, and wearing closed-toe shoes are beneficial but may be difficult in hot or humid climates. |
DEET = diethyltoluamide.
Information from reference 17.
Insect repellent should be applied to exposed skin. The most effective insect repellents contain 20% to 50% diethyltoluamide (DEET)20,21 or 20% picaridin. Other effective insect repellents are oil of lemon eucalyptus (PMD) and IR3535. Insect repellent should not be applied onto or under clothing. Regular reapplication is important.
Applying permethrin to clothing markedly increases protection against insect bites.22,23 Travelers to malaria-endemic regions should sleep under a bed net impregnated with permethrin unless there is air-conditioning. Wearing long sleeves and pants offers additional protection. The vector for malaria is the female Anopheles mosquito, which feeds at dusk, nighttime, and dawn; minimizing time outdoors during these times will reduce risk. IR3535 does not provide adequate protection against Anopheles mosquitoes and should not be used in malaria-endemic areas.
MALARIA PROPHYLAXIS
Travelers to endemic regions should receive malaria prophylaxis.24,25 The choice of prophylactic medication (Table 520,26 ) should be based on whether the patient is going to an area with chloroquine-sensitive or chloroquine-resistant malaria, whether there could be potential adverse effects or interactions with the patient's medical conditions or other medications, the convenience of dosing schedule, and the cost. A summary of countries where malaria is endemic and prophylaxis recommendations from the Centers for Disease Control and Prevention are available at http://www.cdc.gov/malaria/travelers/country_table/a.html. Recommendations from the World Health Organization are available at http://www.who.int/ith/2015-ith-chapter7.pdf?ua=1.
Table 5. Drugs for Malaria Prophylaxis

| Drug | Dosage | Comments | |
|---|---|---|---|
| Chloroquine-sensitive malaria | |||
|
|
| |
|
| ||
| Chloroquine-resistant malaria | |||
|
|
| |
|
|
| |
|
| Contraindications include epilepsy, psychiatric conditions (including anxiety and depression), and cardiac conduction disorders; may be used in all trimesters of pregnancy | |
| Short-term travel to areas with more than 90% | |||
|
|
| |
G6PD = glucose-6-phosphate dehydrogenase.
Adapted with permission from Bazemore AW, Huntington M. The pretravel consultation. Am Fam Physician. 2009;80(6):589, with additional information from reference 20.
Regions where chloroquine-sensitive malaria is endemic include Mexico and Central America (west of the Panama Canal), and the island of Hispaniola (Haiti and the Dominican Republic). Options for prophylaxis in these regions are chloroquine (Aralen) and hydroxychloroquine (Plaquenil). Potential adverse effects of these medications include blurred vision, headache, nausea, and vomiting. Hydroxychloroquine may be better tolerated than chloroquine. Primaquine may be used for prophylaxis in areas affected primarily by Plasmodium vivax malaria.
The options for travelers to chloroquine-resistant regions (including most of South America, Asia, and Africa) are doxycycline, atovaquone/proguanil (Malarone), and mefloquine; these agents are equally effective. Doxycycline, which is taken daily, is relatively inexpensive. Potential adverse effects include nausea, photosensitivity, vaginal yeast infections, and esophageal ulceration. Atovaquone/proguanil, also a daily medication, is the most expensive option but has the lowest incidence of adverse effects. Mefloquine, taken weekly, is well-tolerated by most patients, but has a U.S. Food and Drug Administration boxed warning because of its neurologic and psychiatric adverse effects. In some areas of Southeast Asia, malaria is resistant to mefloquine, and doxycycline or atovaquone/proguanil should be used. Antimalarials should not be purchased in low-income nations because there is a high risk of counterfeit, adulterated, or expired medications.
ZIKA VIRUS INFECTION
Zika virus infection is primarily transmitted by mosquitoes, but it can also be sexually transmitted. Since May of 2015, this disease has spread to Mexico and essentially every country in Central and South America and the Caribbean. Risk of microcephaly in the newborn if a woman is infected in the first trimester of pregnancy has been estimated at 1% to 13%. Pregnant women should avoid travel to areas with Zika transmission. Men who live in or visit a Zika-endemic area should use a condom or abstain from sex with a pregnant partner for the remainder of the pregnancy.27,28
Traveler's Diarrhea
Traveler's diarrhea (TD) is by far the most common infection in international travelers, with a rate of 30% to 70% depending on destination and season of travel. The risk is highest in the first two weeks of travel and slowly declines thereafter.29 Taking medications that reduce gastric acidity, including proton pump inhibitors and antacids, significantly increases the risk of TD.10 Other risk factors include younger age, diabetes, and immunosuppression.
The etiology of TD is bacterial in 80% to 90% of cases; the remainder are caused by viral or protozoan organisms. Bacterial and viral TD usually present as the sudden onset of loose stools, cramping, and nausea. Other manifestations may include abdominal pain, fever, vomiting, and bloody stools. TD caused by protozoan organisms, such as Giardia, tends to have a more insidious onset and a longer duration of symptoms.30
PREVENTION
Traditional advice (e.g., avoiding food from street stands, tap water, raw foods, and ice) has not been shown to reduce the incidence of TD.31 Hand washing reduces risk by 30%; alcohol-based hand sanitizer also significantly reduces risk.32
Prophylactic antibiotics are not routinely recommended. For patients at particularly high risk, taking bismuth subsalicylate (Pepto-Bismol; two tablets four times daily for the duration of the trip) reduces risk by 50% to 65%.20,33 Possible adverse effects of bismuth subsalicylate include a black tongue and dark stool, and contraindications include aspirin allergy, renal insufficiency, breastfeeding, and concurrent use of anticoagulants. There is insufficient evidence for the use of probiotics to prevent TD.
TREATMENT
The primary supportive treatment for TD is rehydration. However, in general, TD is not dehydrating, except for in persons who are very young or old or who have chronic illnesses. If dehydration occurs, travelers can rehydrate with most fluids, including water, juice, soda pop, or tea.
Loperamide (Imodium) is a safe and effective antimotility agent that can be used with or without antibiotics. It should be avoided in persons with warning signs, such as blood in the stool or fever, and in children younger than six years. Diphenoxylate is an alternative antimotility agent.
Without treatment, TD usually lasts three to seven days. A short course of antibiotics usually shortens symptom duration to six to 24 hours.34,35 Fluoroquinolones are effective for self-treatment of TD in Africa and Latin America. One regimen is ciprofloxacin taken as one 500-mg tablet followed by a second 500-mg tablet 12 hours later. However, a macrolide, such as azithromycin (Zithromax; 500 mg daily for one to three days or one 1,000-mg tablet [higher incidence of nausea]) is more effective in South and Southeast Asia because of the high prevalence of TD caused by fluoroquinolone-resistant Campylobacter. Given the recent warning by the U.S. Food and Drug Administration regarding adverse effects of fluoroquinolones,36 clinicians may consider prescribing a macrolide for self treatment of TD regardless of destination. Rifaximin (Xifaxan), an antibiotic with minimal systemic absorption, can be used as a preventive medication (200 mg once or twice daily) or as treatment (200 mg three times daily for three days). It is not approved by the U.S. Food and Drug Administration for TD prophylaxis.
Because TD is usually self-limited, and antibiotics have potential adverse effects, a course of carry-along antibiotics should be prescribed for the patient to use only if needed. To reduce the risk of creating drug-resistant bacteria, antibiotics should be taken only for severe diarrhea.37
Travelers with TD who develop syncope, dehydration, or symptoms lasting more than one week should seek medical care. Studies show that 3% to 17% of TD cases may result in chronic postinfectious irritable bowel syndrome; the risk increases with multiple bouts of TD.38,39
Emergency Medical Evacuation Insurance
Emergent medical evacuation from a low-income nation can cost $50,000 to $75,000 or more. Emergency medical evacuation insurance is particularly important for older travelers, for those with chronic medical conditions, and for those engaged in high-risk activities, such as high-altitude climbing. Travelers can visit https://www.squaremouth.com/ to compare travel insurance options, including medical and emergency evacuation insurance.
Travelers with Chronic Medical Conditions
Persons with most medical conditions can travel without restriction, but additional advance preparation may be necessary. Medical conditions should be stable before travel, and patients requiring frequent medical interventions should postpone travel to low-income nations.
Travelers who have chronic medical conditions should carry a list of their medications and physician contact information. Medications should be transported in carry-on, not checked, luggage and remain in the labeled containers in which they were dispensed from the pharmacy. Travelers who have diabetes should accept somewhat higher than usual glucose values during travel days to avoid hypoglycemia. Those requiring oxygen should contact the airline several weeks in advance to arrange for oxygen during flights. The Federal Aviation Administration does not allow passengers to carry their own oxygen tanks; battery-powered portable oxygen concentrators approved by the Department of Transportation may be used. Travelers who have a significant history of cardiac events should travel with a recent electrocardiogram.
Pregnant Women
Most airlines allow pregnant women to fly until 36 weeks of gestation. Pregnant women should not scuba dive because of the potential risk of decompression sickness in the fetus and fetal malformations.40
Data Sources: We searched PubMed, the Cochrane Database of Systematic Reviews, Essential Evidence Plus, AHRQ Evidence Reports, and BMJ Clinical Evidence. Key words: travel medicine, immunizations, malaria prophylaxis, traveler's diarrhea, motor vehicle injuries, pretravel consultation. Search dates: May and September 2015, and June 2016.
note: This review updates previous articles by Bazemore and Huntington,26 Lo Re and Guzman,41 and Dick.42

