Am Fam Physician. 2016;94(9):727
Author disclosure: No relevant financial affiliations.
Although rates of uninsured Americans are declining because of the Affordable Care Act (ACA), there is growing concern about out-of-pocket expenditures associated with private high-deductible insurance plans. Although lower premiums are attractive to many, the trade-offs are large deductibles (more than $1,200 per person or more than $2,400 per family) and increased risk of medical debt. Many patients with these plans delay or avoid necessary treatment, including ambulatory and preventive care.
Compared with traditional private health insurance, high-deductible plans have been associated with increased use of high-cost emergency department services, and reduced use of low-cost primary and preventive services and medications.1 In addition to deductibles, patients with high-deductible plans may face coinsurance or copayments. Many high-deductible plans provide narrow networks, increasing the chance of unanticipated billing for out-of-network services. Medical debt is of greatest concern for individuals with chronic conditions, who use more health services. The ACA health exchanges will increase the number of low-income Americans who have low-premium, high-deductible insurance, but who are more likely to be chronically ill and at risk of deferring services and accruing medical debt because of the high deductible.2,3
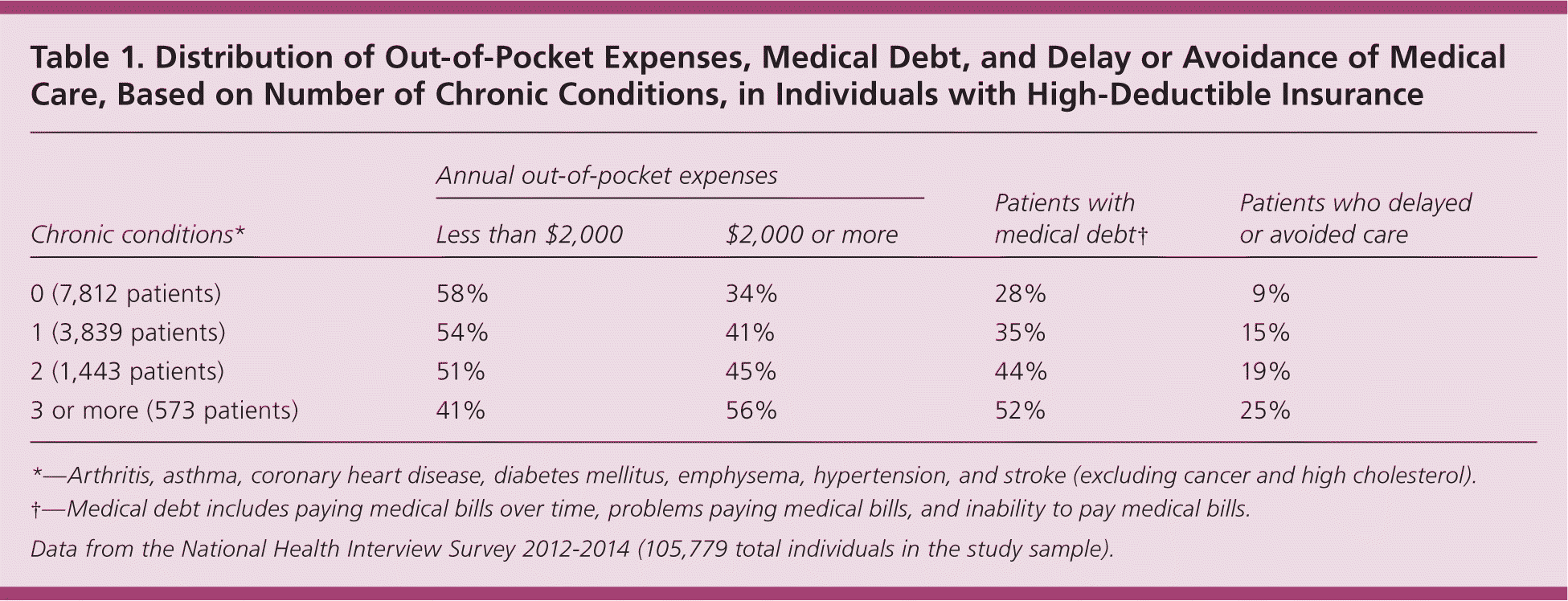
We used data from the National Health Interview Survey to measure out-of-pocket expenses, medical debt, and avoidance or delay of care, based on number of chronic conditions, among privately insured adults who have high deductibles (Table 1). Out-of-pocket expenses and medical debt increased with the number of chronic conditions. Those with three or more chronic conditions were nearly three times as likely to delay or avoid care as those without chronic conditions (25% vs. 9%). Delay or avoidance of necessary care risks earlier development of chronic disease complications or preventable disease.
Now that the ACA has reduced the uninsured, policy makers should focus on mitigating the health and economic consequences of financial barriers to ambulatory and preventive care associated with high-deductible plans.
This information does not necessarily reflect the views or the policy of the AAFP.