Prostate cancer is the most common nonskin cancer and causes about 27,000 deaths in U.S. men each year.1 However, the only U.S. randomized trial of prostate-specific antigen (PSA) screening did not find a mortality benefit after 13 years of follow-up.2 Even after results from a European trial found slightly lower prostate cancer–specific (but not all-cause) mortality in screened participants, the U.S. Preventive Services Task Force (USPSTF) concluded in 2012 that the harms of screening outweigh potential benefits in most men and recommended against PSA-based screening for prostate cancer.3
Since the USPSTF made this recommendation, PSA screening rates have decreased substantially.4,5 Some observers think this practice is consistent with current evidence.6 Others note that metastatic prostate cancer rates have declined since PSA screening became widespread,7 and warn that discontinuing screening may result in more men dying from potentially curable prostate cancers. Although the debate continues, guidelines from the American Urological Association, American Cancer Society, and American College of Physicians concur that physicians should discuss the benefits and harms of screening with men 55 to 69 years of age, practice shared decision making, and order PSA screening only if the patient expresses a clear preference to be screened.8–10
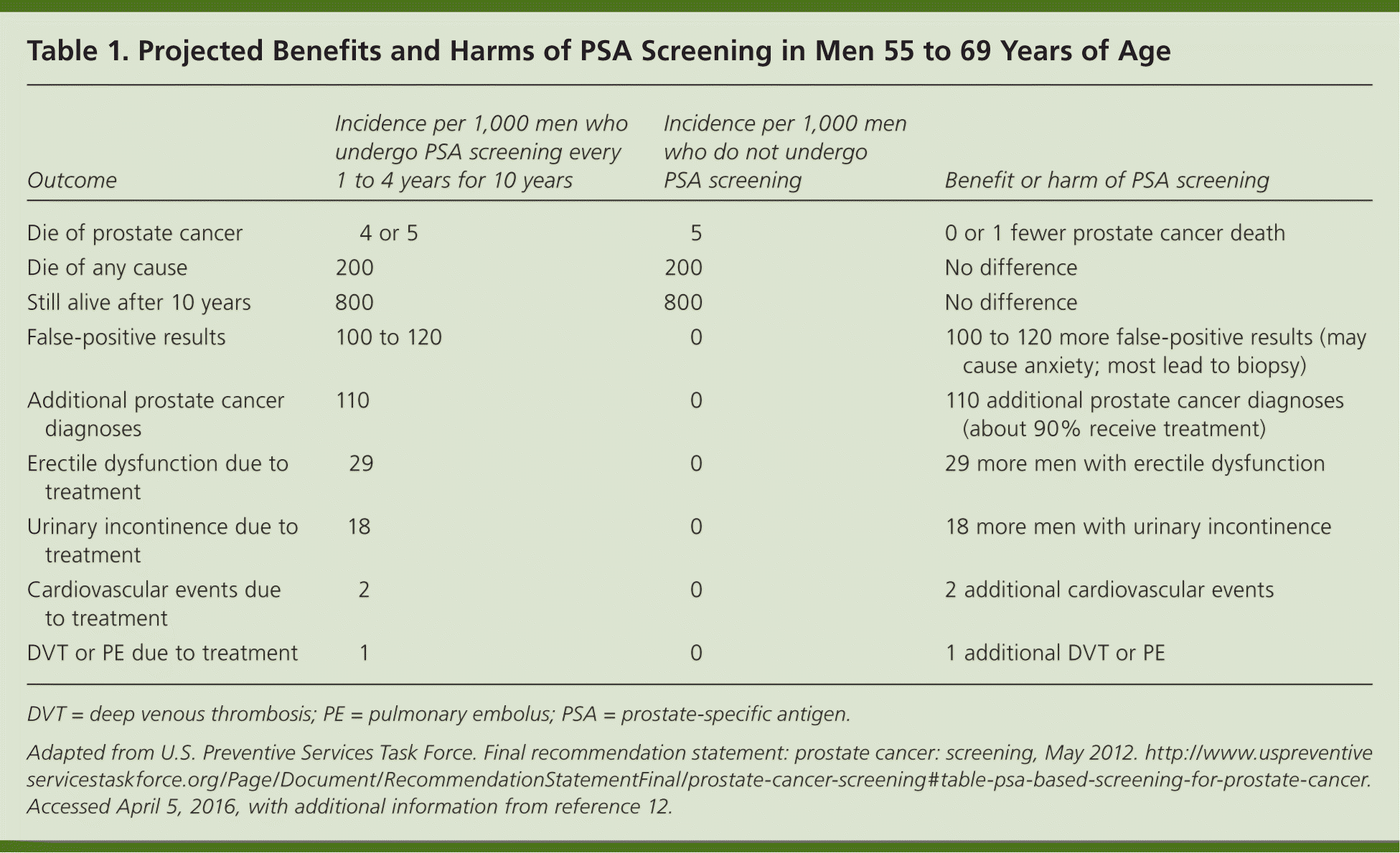
For family physicians to put this guidance into practice, they must elicit patients' preferences and provide accurate, understandable information about the benefits and harms of PSA screening. Web-based and print decision aids can help patients make informed choices and improve their satisfaction with PSA screening decisions.11 These tools range from straightforward infographics (http://www.cancer.gov/types/prostate/psa-infographic) to more time-consuming questionnaires (http://www.uofmhealth.org/health-library/aa38144). Regardless of the decision aid used, physicians should provide men with quantitative information on the benefits and harms of screening, represented as numbers needed to screen to benefit or harm,12 or a projected outcomes table (Table 13,12 ). Compared with no screening, for every 1,000 men who have PSA screening every one to four years for 10 years, one man avoids death from prostate cancer (while another man dies of something else), 100 to 120 have at least one false-positive test result, and treatment of 110 additional men diagnosed with prostate cancer leads to 29 developing cases of erectile dysfunction and 18 developing cases of urinary incontinence.
Table 1. Projected Benefits and Harms of PSA Screening in Men 55 to 69 Years of Age
| Outcome | Incidence per 1,000 men who undergo PSA screening every 1 to 4 years for 10 years | Incidence per 1,000 men who do not undergo PSA screening | Benefit or harm of PSA screening |
|---|---|---|---|
| Die of prostate cancer | 4 or 5 | 5 | 0 or 1 fewer prostate cancer death |
| Die of any cause | 200 | 200 | No difference |
| Still alive after 10 years | 800 | 800 | No difference |
| False-positive results | 100 to 120 | 0 | 100 to 120 more false-positive results (may cause anxiety; most lead to biopsy) |
| Additional prostate cancer diagnoses | 110 | 0 | 110 additional prostate cancer diagnoses (about 90% receive treatment) |
| Erectile dysfunction due to treatment | 29 | 0 | 29 more men with erectile dysfunction |
| Urinary incontinence due to treatment | 18 | 0 | 18 more men with urinary incontinence |
| Cardiovascular events due to treatment | 2 | 0 | 2 additional cardiovascular events |
| DVT or PE due to treatment | 1 | 0 | 1 additional DVT or PE |
DVT = deep venous thrombosis; PE = pulmonary embolus; PSA = prostate-specific antigen.
Adapted from U.S. Preventive Services Task Force. Final recommendation statement: prostate cancer: screening, May 2012. http://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/prostate-cancer-screening#table-psa-based-screening-for-prostate-cancer. Accessed April 5, 2016, with additional information from reference12.
Many older men, especially those who have received PSA tests in the past, may be surprised to learn that screening is no longer routine. Primary care physicians should anticipate this possibility and be prepared to explain that more is now known about the outcomes of testing. Phrases that may be helpful to communicate changes in our understanding of the evidence include “the PSA test is now optional,” “this test has limitations and may not be for everyone,” and “there are some important downsides to being tested.” These strategies, combined with decision aids, should help our patients make informed choices that are consistent with their personal preferences on PSA screening.
editor's note: Dr. Lin is Associate Deputy Editor of AFP Online. Dr. Ebell is AFP's Deputy Editor of Evidence-Based Medicine and was a member of the USPSTF from 2012 to 2015. He is currently a consultant to the USPSTF.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Preventive Services Task Force or the Agency for Healthcare Research and Quality.

