
Am Fam Physician. 2016;94(11):918-920
Author disclosure: No relevant financial affiliations.
Key Clinical Issue
What are the effectiveness and adverse consequences of strategies for reducing antibiotic use in adults and children with uncomplicated acute respiratory tract infections (RTIs)?
Evidence-Based Answer
Procalcitonin point-of-care testing reduces antibiotic prescribing in adults (Strength of recommendation [SOR]: A, based on consistent, good-quality patient-oriented evidence), but increases antibiotic prescribing and adverse consequences in children. (SOR: B, based on inconsistent or limited-quality patient-oriented evidence.) Rapid streptococcal antigen point-of-care testing, viral polymerase chain reaction testing (adults only), and C-reactive protein testing reduced antibiotic prescribing, but studies of adverse consequences were lacking. Delayed prescribing practices reduced antibiotic prescribing, but reduced patient satisfaction and increased symptom length. (SOR: A, based on consistent, good-quality patient-oriented evidence.) Electronic decision supports reduced antibiotic prescribing without affecting the risk of complications.
Practice Pointers
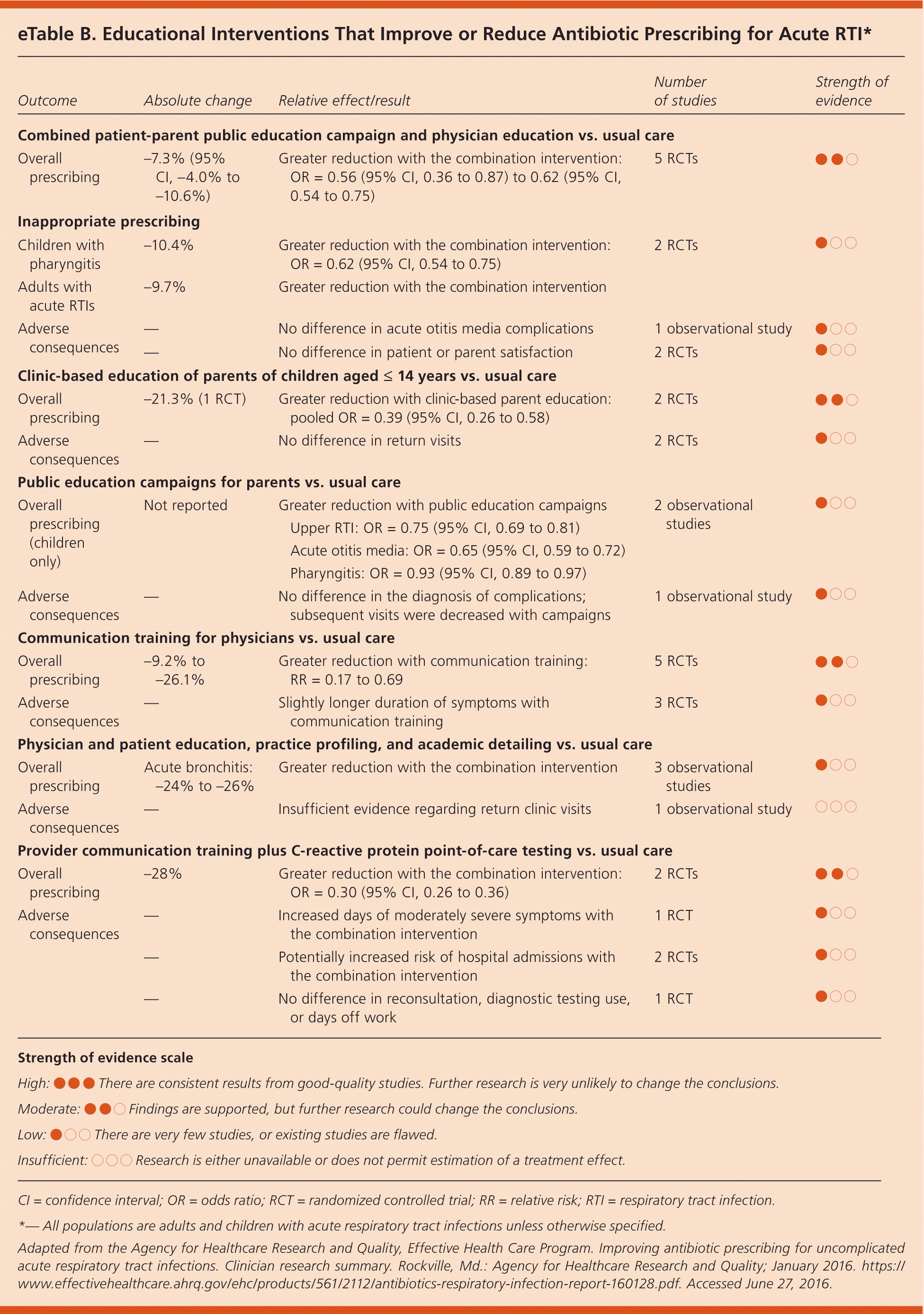
Antibiotic-resistant bacterial infections lead to approximately 23,000 deaths in the United States each year.1 Inappropriate antibiotic prescribing is the leading cause of resistance and accounts for one-third of all antibiotic prescriptions each year.2 Clinical, system-level, or educational interventions that reduce inappropriate prescribing (eTable A and eTable B) have the potential to dramatically decrease deaths and slow the progression of resistant organisms.

| Category | Explanations and examples |
|---|---|
| Clinical | Point-of-care tests to rapidly determine the likelihood that a patient has a specific infection (e.g., rapid streptococcal antigen test of a throat swab sample, multiviral polymerase chain reaction, or an influenza-specific test of throat or nasopharyngeal secretions) or has a bacterial infection instead of a viral one (e.g., blood procalcitonin, blood C-reactive protein); tympanometry to aid in diagnosing acute otitis media; delayed antibiotic prescribing (e.g., giving prescriptions to patients with instructions to delay filling, leaving prescriptions for patient collection, postdating prescriptions, requesting recontact with physician); clinical scoring tools based on combinations of signs and symptoms |
| System-level | Electronic decision support (computer-aided, evidence-based prescribing recommendations); paper-based physician reminders about prescribing; physician audit plus feedback; financial or regulatory incentives for physicians or patients; antimicrobial stewardship programs |
| Educational | Clinic-based patient or parent education about when antibiotics may be appropriate (e.g., videos, pamphlets, verbal education, waiting room posters); public education campaigns (e.g., billboards, bus advertisements, radio and television advertisements); clinician education about current treatment guidelines; communication skills training programs for physicians |
| Multifaceted | Combination of interventions from one or more categories |
| Outcome | Absolute change | Relative effect/result | Number of studies | Strength of evidence | |
|---|---|---|---|---|---|
| Combined patient-parent public education campaign and physician education vs. usual care | |||||
| Overall prescribing | −7.3% (95% CI, −4.0% to −10.6%) | Greater reduction with the combination intervention: OR = 0.56 (95% CI, 0.36 to 0.87) to 0.62 (95% CI, 0.54 to 0.75) | 5 RCTs | ● ● ○ | |
| Inappropriate prescribing | |||||
| Children with pharyngitis | −10.4% | Greater reduction with the combination intervention: OR = 0.62 (95% CI, 0.54 to 0.75) | 2 RCTs | ● ○ ○ | |
| Adults with acute RTIs | −9.7% | Greater reduction with the combination intervention | |||
| Adverse consequences | — | No difference in acute otitis media complications | 1 observational study | ● ○ ○ | |
| — | No difference in patient or parent satisfaction | 2 RCTs | ● ○ ○ | ||
| Clinic-based education of parents of children aged ≤ 14 years vs. usual care | |||||
| Overall prescribing | −21.3% (1 RCT) | Greater reduction with clinic-based parent education: pooled OR = 0.39 (95% CI, 0.26 to 0.58) | 2 RCTs | ● ● ○ | |
| Adverse consequences | — | No difference in return visits | 2 RCTs | ● ○ ○ | |
| Public education campaigns for parents vs. usual care | |||||
| Overall prescribing (children only) | Not reported | Greater reduction with public education campaigns | 2 observational studies | ● ○ ○ | |
| Upper RTI: OR = 0.75 (95% CI, 0.69 to 0.81) | |||||
| Acute otitis media: OR = 0.65 (95% CI, 0.59 to 0.72) | |||||
| Pharyngitis: OR = 0.93 (95% CI, 0.89 to 0.97) | |||||
| Adverse consequences | — | No difference in the diagnosis of complications; subsequent visits were decreased with campaigns | 1 observational study | ● ○ ○ | |
| Communication training for physicians vs. usual care | |||||
| Overall prescribing | −9.2% to −26.1% | Greater reduction with communication training: RR = 0.17 to 0.69 | 5 RCTs | ● ● ○ | |
| Adverse consequences | — | Slightly longer duration of symptoms with communication training | 3 RCTs | ● ○ ○ | |
| Physician and patient education, practice profiling, and academic detailing vs. usual care | |||||
| Overall prescribing | Acute bronchitis: −24% to −26% | Greater reduction with the combination intervention | 3 observational studies | ● ○ ○ | |
| Adverse consequences | — | Insufficient evidence regarding return clinic visits | 1 observational study | ○ ○ ○ | |
| Provider communication training plus C-reactive protein point-of-care testing vs. usual care | |||||
| Overall prescribing | −28% | Greater reduction with the combination intervention: OR = 0.30 (95% CI, 0.26 to 0.36) | 2 RCTs | ● ● ○ | |
| Adverse consequences | — | Increased days of moderately severe symptoms with the combination intervention | 1 RCT | ● ○ ○ | |
| — | Potentially increased risk of hospital admissions with the combination intervention | 2 RCTs | ● ○ ○ | ||
| — | No difference in reconsultation, diagnostic testing use, or days off work | 1 RCT | ● ○ ○ | ||
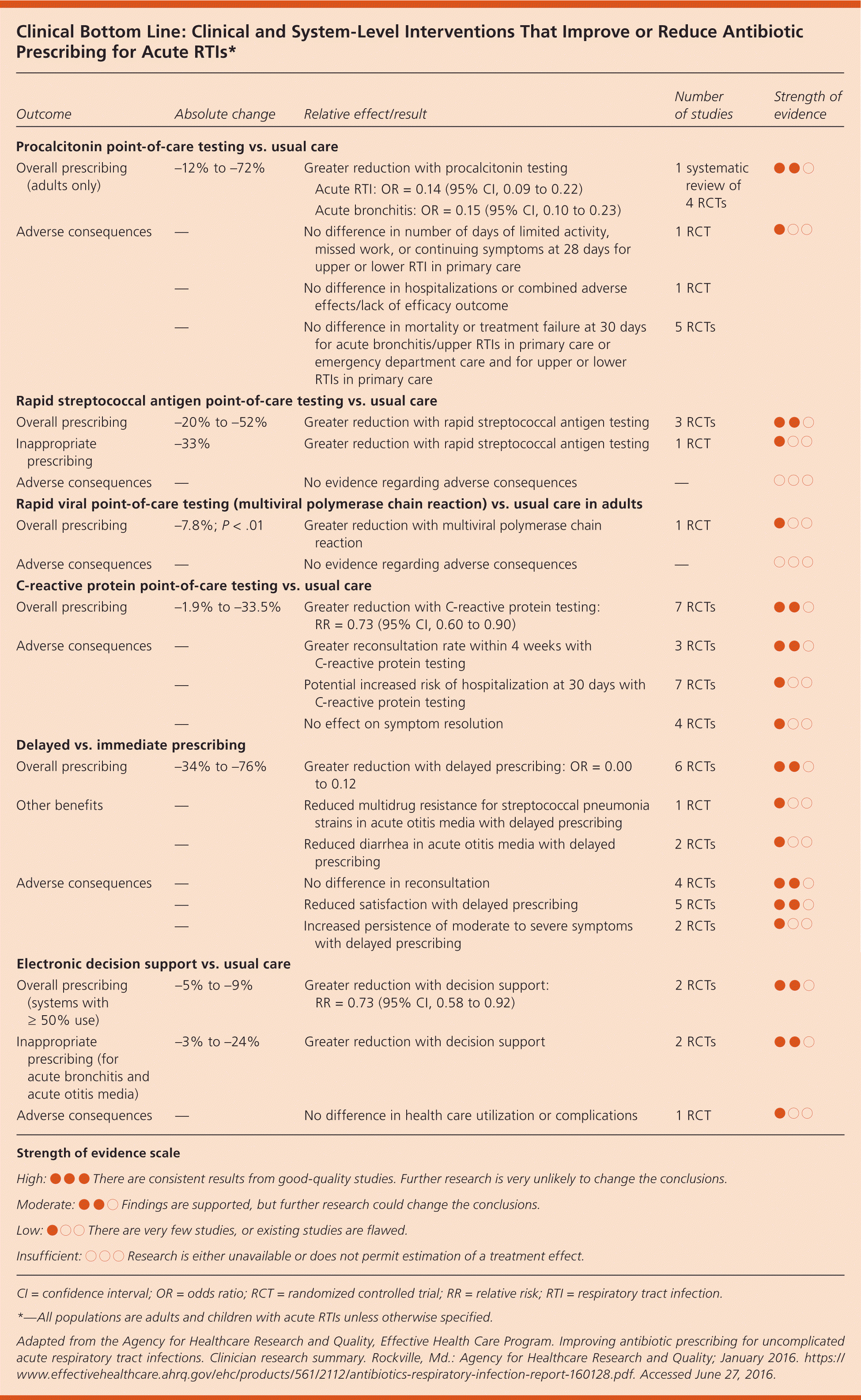
This Agency for Healthcare Research and Quality review considered multiple approaches to antibiotic overprescribing. Although individual studies varied with respect to practice setting, the combination of interventions, and the selection of RTIs for which effectiveness was shown, point-of-care testing generally reduced overprescribing. The addition of rapid streptococcal antigen testing decreased overall antibiotic prescribing by 20% to 52% and decreased inappropriate prescribing by 33% over usual care. Procalcitonin testing reduced antibiotic prescribing in adults by 12% to 72%, but led to a 22% increase in antibiotic prescriptions in children. C-reactive protein testing also reduced prescribing by 1.9% to 33.5%, but was associated with increased hospitalizations at one month (1.1% of those triaged with C-reactive protein testing were hospitalized as opposed to 0.2% of those who received usual care).1
Delayed prescribing (e.g., providing a prescription and instructing the patient to delay filling it) reduced antibiotic use by 34% to 76%, but was associated with reduced patient satisfaction and increased persistence of moderate to severe symptoms. Electronic decision support tools produced more modest reductions in overall prescribing (5% to 9%) with no difference in complications, whereas educational interventions targeting physicians, patients, or parents showed some promise (4% to 28% decline in overall prescriptions based on a mix of modalities used), without changing the rate of complications.1
Multiple effective interventions exist to help physicians be good stewards of antibiotics. The Institute for Clinical Systems Improvement does not recommend antibiotics for RTIs that are suspected to be viral, and recommends reserving antibiotics for acute sinusitis when decongestants are ineffective or patients have complications.3 The American Academy of Pediatrics suggests observation, rather than immediate antibiotic prescription, as an option in children 24 months or older with nonsevere acute otitis media (mild otalgia for less than 48 hours and a temperature less than 102.2°F [39°C]).4 Despite this, the longer physicians are in practice, the less likely they are to follow the guidelines.5 Many physicians feel that patient expectations and time constraints make it difficult to explain to a patient why they do not need an antibiotic.6,7 Of the point-of-care modalities tested, rapid streptococcal antigen testing seems the most helpful in guiding antibiotic prescribing and is recommended by the Infectious Diseases Society of America.8 There may be a role for procalcitonin and C-reactive protein testing, but major clinical practice guidelines do not endorse their routine use.9–11
| Outcome | Absolute change | Relative effect/result | Number of studies | Strength of evidence | |
|---|---|---|---|---|---|
| Procalcitonin point-of-care testing vs. usual care | |||||
| Overall prescribing (adults only) | −12% to −72% | Greater reduction with procalcitonin testing | 1 systematic review of 4 RCTs | ● ● ○ | |
| Acute RTI: OR = 0.14 (95% CI, 0.09 to 0.22) | |||||
| Acute bronchitis: OR = 0.15 (95% CI, 0.10 to 0.23) | |||||
| Adverse consequences | — | No difference in number of days of limited activity, missed work, or continuing symptoms at 28 days for upper or lower RTI in primary care | 1 RCT | ● ○ ○ | |
| — | No difference in hospitalizations or combined adverse effects/lack of efficacy outcome | 1 RCT | |||
| — | No difference in mortality or treatment failure at 30 days for acute bronchitis/upper RTIs in primary care or emergency department care and for upper or lower RTIs in primary care | 5 RCTs | |||
| Rapid streptococcal antigen point-of-care testing vs. usual care | |||||
| Overall prescribing | −20% to −52% | Greater reduction with rapid streptococcal antigen testing | 3 RCTs | ● ● ○ | |
| Inappropriate prescribing | −33% | Greater reduction with rapid streptococcal antigen testing | 1 RCT | ● ○ ○ | |
| Adverse consequences | — | No evidence regarding adverse consequences | — | ○ ○ ○ | |
| Rapid viral point-of-care testing (multiviral polymerase chain reaction) vs. usual care in adults | |||||
| Overall prescribing | −7.8%; P < .01 | Greater reduction with multiviral polymerase chain reaction | 1 RCT | ● ○ ○ | |
| Adverse consequences | — | No evidence regarding adverse consequences | — | ○ ○ ○ | |
| C-reactive protein point-of-care testing vs. usual care | |||||
| Overall prescribing | −1.9% to −33.5% | Greater reduction with C-reactive protein testing: RR = 0.73 (95% CI, 0.60 to 0.90) | 7 RCTs | ● ● ○ | |
| Adverse consequences | — | Greater reconsultation rate within 4 weeks with C-reactive protein testing | 3 RCTs | ● ● ○ | |
| — | Potential increased risk of hospitalization at 30 days with C-reactive protein testing | 7 RCTs | ● ○ ○ | ||
| — | No effect on symptom resolution | 4 RCTs | ● ○ ○ | ||
| Delayed vs. immediate prescribing | |||||
| Overall prescribing | −34% to −76% | Greater reduction with delayed prescribing: OR = 0.00 to 0.12 | 6 RCTs | ● ● ○ | |
| Other benefits | — | Reduced multidrug resistance for streptococcal pneumonia strains in acute otitis media with delayed prescribing | 1 RCT | ● ○ ○ | |
| — | Reduced diarrhea in acute otitis media with delayed prescribing | 2 RCTs | ● ○ ○ | ||
| Adverse consequences | — | No difference in reconsultation | 4 RCTs | ● ● ○ | |
| — | Reduced satisfaction with delayed prescribing | 5 RCTs | ● ● ○ | ||
| — | Increased persistence of moderate to severe symptoms with delayed prescribing | 2 RCTs | ● ○ ○ | ||
| Electronic decision support vs. usual care | |||||
| Overall prescribing (systems with ≥ 50% use) | −5% to −9% | Greater reduction with decision support: RR = 0.73 (95% CI, 0.58 to 0.92) | 2 RCTs | ● ● ○ | |
| Inappropriate prescribing (for acute bronchitis and acute otitis media) | −3% to −24% | Greater reduction with decision support | 2 RCTs | ● ● ○ | |
| Adverse consequences | — | No difference in health care utilization or complications | 1 RCT | ● ○ ○ | |
editor's note: American Family Physician SOR ratings are different from the AHRQ Strength of Evidence (SOE) ratings.
The opinions and assertions contained herein are the private views of the author and are not to be construed as official or as reflecting the views of the U.S. Army Medical Department or the U.S. Army Service at large.
