A 13-year-old boy presented with increased breast size and darkening of the areola, which began at 11 years of age. He had occasional soreness in the breast area but no nipple discharge. His medical history included asthma, allergic rhinitis, obesity, and dyslipidemia treated with pravastatin (Pravachol). He was not using any other medications or illicit drugs.
Physical examination revealed grade 3 gynecomastia with ptotic, or sagging, breasts (Figures 1 and 2). The nipples fell below the inframammary crease. The breasts appeared to consist of fat and glandular tissues with enlarged and darkened areolas. No palpable masses were noted.
Figure 1
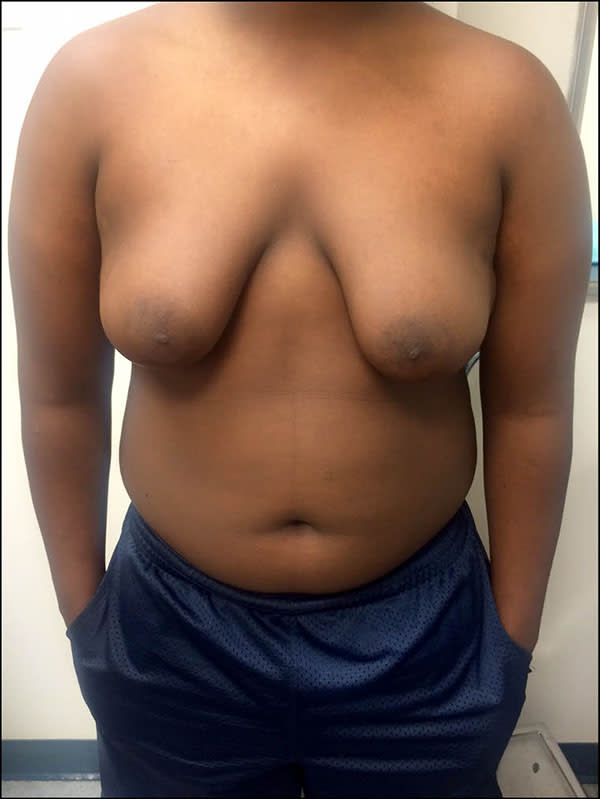
Figure 2
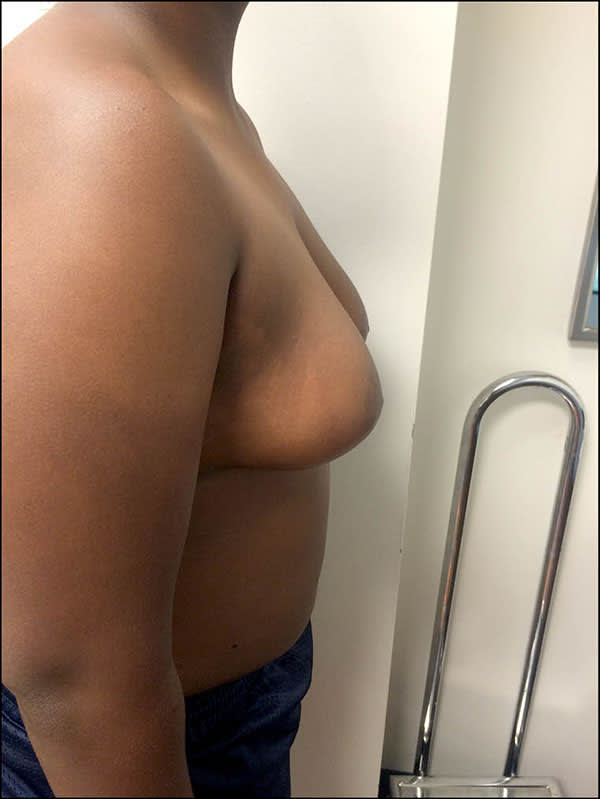
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Medication or illicit drug use.
B. Physiologic gynecomastia.
C. Primary hypogonadism.
D. Pseudogynecomastia.
E. Testicular cancer.
Discussion
The correct answer is B: physiologic gynecomastia. Physiologic gynecomastia is the most common form of gynecomastia1 and occurs in three distinct age groups: newborns, adolescents, and men older than 50 years. Neonatal physiologic gynecomastia is due to maternal transplacental estrogen.2 Approximately 60% to 90% of male newborns exhibit some degree of gynecomastia.2 Adolescent physiologic gynecomastia is due to increased circulating estradiol concentration or increased breast sensitivity to normal male levels of estrogens during puberty (typically 13 or 14 years of age).2 About 50% to 60% of adolescent males experience gynecomastia. Physiologic gynecomastia occurs in 35% to 65% of older men as a result of decreasing testosterone levels.2
Physiologic gynecomastia is characterized by the proliferation of glandular breast tissue. On physical examination, firm or rubbery breast tissue that is concentric to the nipple or areola is palpable. Physiologic gynecomastia is typically bilateral but may be unilateral. Further evaluation is warranted if gynecomastia occurs outside of the typical age groups for physiologic gynecomastia. Workup for gynecomastia may include liver and renal function tests, and measurements of thyroid-stimulating hormone, serum human chorionic gonadotropin, luteinizing hormone, follicle-stimulating hormone, estradiol, testosterone, and prolactin.1 Breast or testicular imaging may also be warranted if there are signs of a possible mass on physical examination. Physiologic gynecomastia commonly resolves spontaneously; however, further intervention, including treatment with a selective estrogen receptor modulator or breast reduction surgery, may be considered for aesthetic reasons.1
Medication or drug use is a well-known cause of gynecomastia (about 10% to 25% of cases).1 A detailed medication history is imperative in the evaluation of male breast enlargement. Findings include a discrete, round, mobile mass under the areola. It is usually bilateral. Common agents that can cause gynecomastia include spironolactone; anabolic steroids; antipsychotics, such as haloperidol; and illicit drugs, including marijuana, heroin, and amphetamines.1,3
Primary hypogonadism occurs in approximately 8% of gynecomastia cases.1 Laboratory results consistent with primary hypogonadism include an elevated luteinizing hormone level and diminished testosterone level. There are several causes of primary hypogonadism, including Klinefelter syndrome, 5α-reductase deficiency, and testicular trauma.1
Pseudogynecomastia is increased adipose tissue in the breasts and should be considered in obese male patients. It can be distinguished from gynecomastia by physical examination findings of soft adipose tissue rather than glandular breast tissue.4
Testicular cancers, including Leydig cell and Sertoli cell tumors, can produce estrogen, which may result in gynecomastia (about 3% of cases).1 A testicular mass may be palpable on physical examination, and human chorionic gonadotropin levels may be elevated.5
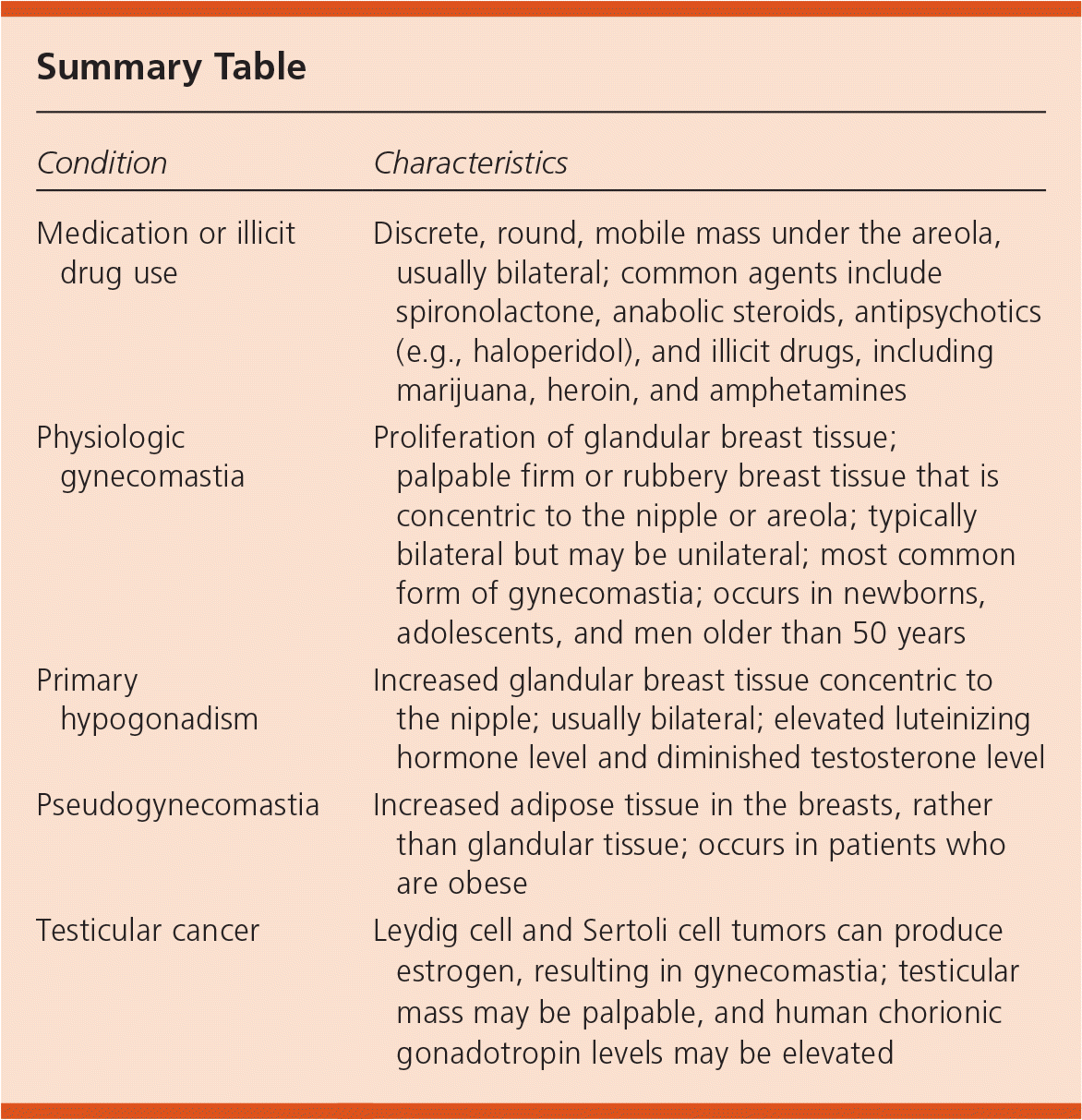
Summary Table
| Condition | Characteristics |
|---|---|
| Medication or illicit drug use | Discrete, round, mobile mass under the areola, usually bilateral; common agents include spironolactone, anabolic steroids, antipsychotics (e.g., haloperidol), and illicit drugs, including marijuana, heroin, and amphetamines |
| Physiologic gynecomastia | Proliferation of glandular breast tissue; palpable firm or rubbery breast tissue that is concentric to the nipple or areola; typically bilateral but may be unilateral; most common form of gynecomastia; occurs in newborns, adolescents, and men older than 50 years |
| Primary hypogonadism | Increased glandular breast tissue concentric to the nipple; usually bilateral; elevated luteinizing hormone level and diminished testosterone level |
| Pseudogynecomastia | Increased adipose tissue in the breasts, rather than glandular tissue; occurs in patients who are obese |
| Testicular cancer | Leydig cell and Sertoli cell tumors can produce estrogen, resulting in gynecomastia; testicular mass may be palpable, and human chorionic gonadotropin levels may be elevated |

