A 62-year-old woman presented with an erythematous, pruritic, expanding rash on her back, chest, and left lower abdomen (Figures 1 and 2). It appeared two months earlier and did not improve with conservative home treatment, including application of skin lotion, petroleum jelly, and an over-the-counter topical steroid cream. There was no pain or drainage from the affected area. The patient was diagnosed with breast cancer three years earlier, for which she underwent right simple mastectomy and left modified radical mastectomy.
Figure 1
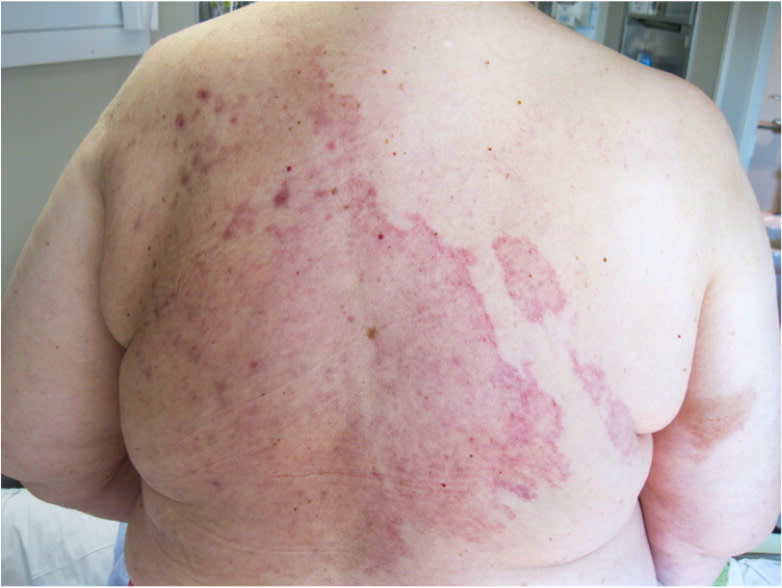
Figure 2
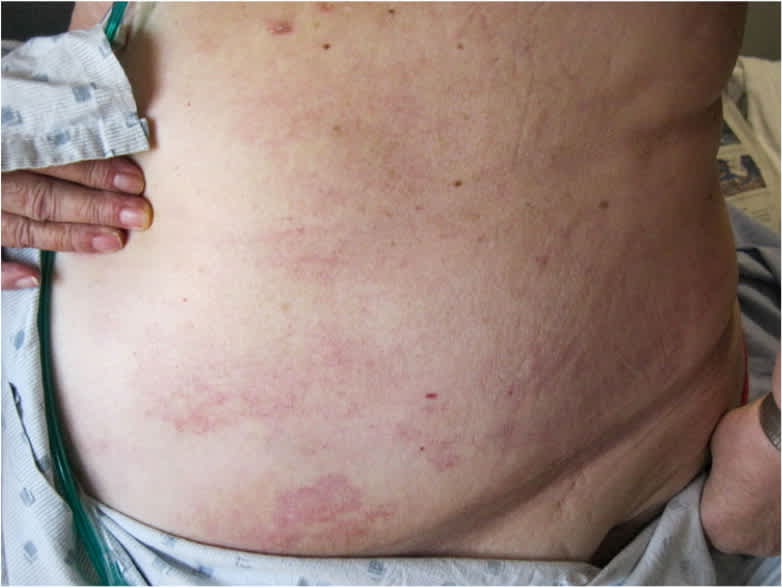
She was afebrile on physical examination. The rash was a large, erythematous plaque with discrete borders. There was some slight edema noted in the lower portion of the back. There was no tenderness or warmth. A punch biopsy was performed.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Inflammatory breast cancer.
B. Mycosis fungoides.
C. Radiation dermatitis.
D. Tinea corporis.
Discussion
The answer is A: inflammatory breast cancer. Inflammatory breast cancer is a rare subtype of locally advanced primary breast cancer, accounting for roughly 2.5% of breast cancers in the United States.1 It is characterized by the disruption of dermal lymphatics with tumor emboli, leading to diffuse skin erythema, ulceration, and edema.2 It is commonly high grade, estrogen receptor negative, and progesterone receptor negative, and it often affects younger patients.3 Onset of symptoms can be rapid over days to weeks. Erythema and edema can appear overnight, and the breast may swell to two to three times its normal size within weeks. Recurrent inflammatory breast cancer appears with the same skin and microscopic characteristics as the original primary breast cancer biopsies.
Inflammatory breast cancer is an aggressive carcinoma with a five-year survival rate of roughly 50% even with multimodal therapy.1 Poor prognostic factors include metastasis to lymph nodes, extensive erythema, estrogen receptor–negative disease, and the TP53 gene mutation.4 This highly malignant cancer is often misdiagnosed as a benign infectious or inflammatory process and can also mimic other tumors, such as sarcomas.5
Mycosis fungoides is the most common form of cutaneous T cell lymphoma. It has a variable presentation, including rash-like patches or lesions that may be pruritic. Diagnosis is based on clinical presentation and histopathology.
Radiation dermatitis can be acute or chronic but is always associated with recent radiation therapy. Blisters and erythema are typically observed in the acute phase. Chronic radiation dermatitis presents as atrophic indurated plaques that are typically white or yellow.
Tinea corporis is a fungal infection that causes red, scaly, pruritic rings that are raised and dry. It can appear anywhere on the body but is more common in warm, moist areas, such as under the breasts or in the groin.
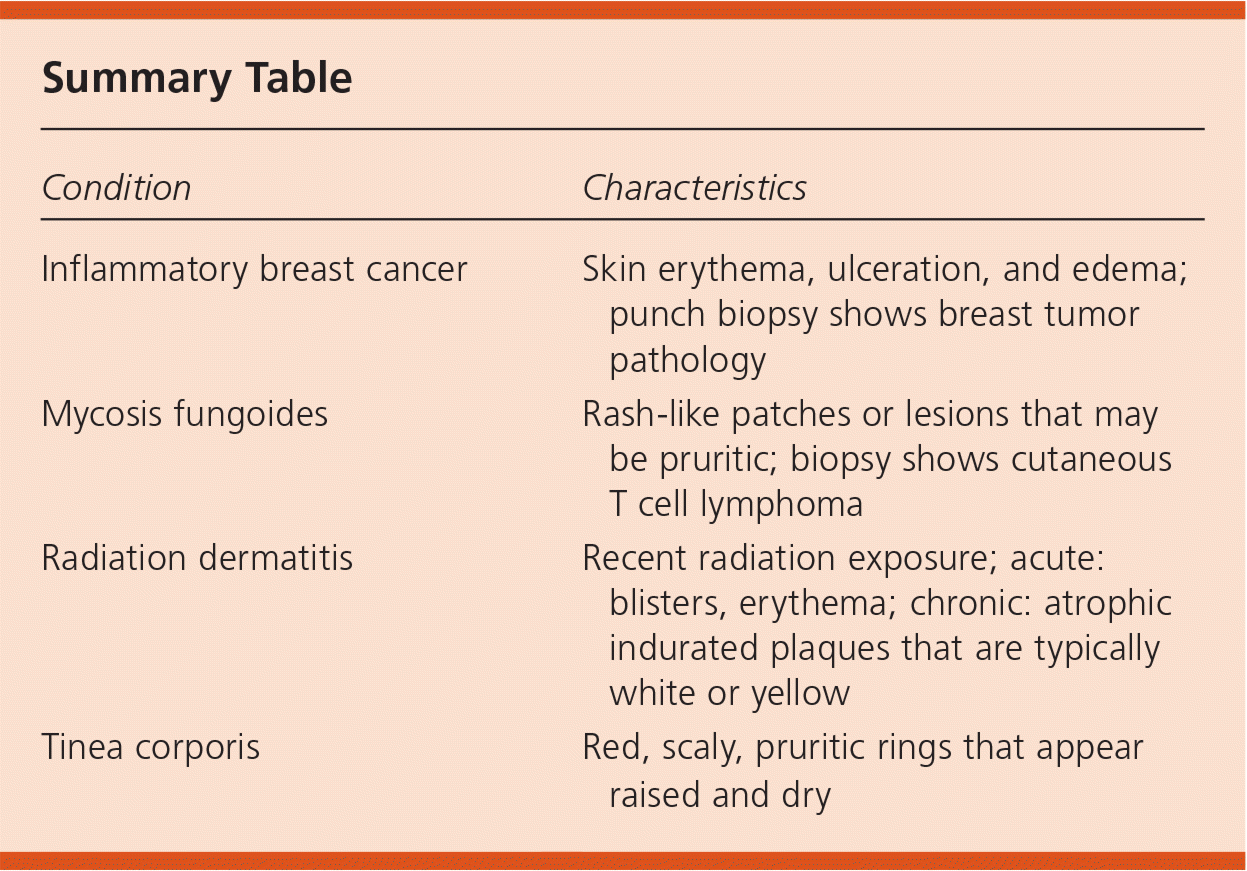
Summary Table
| Condition | Characteristics |
|---|---|
| Inflammatory breast cancer | Skin erythema, ulceration, and edema; punch biopsy shows breast tumor pathology |
| Mycosis fungoides | Rash-like patches or lesions that may be pruritic; biopsy shows cutaneous T cell lymphoma |
| Radiation dermatitis | Recent radiation exposure; acute: blisters, erythema; chronic: atrophic indurated plaques that are typically white or yellow |
| Tinea corporis | Red, scaly, pruritic rings that appear raised and dry |

