Recurrent strokes make up almost 25% of the nearly 800,000 strokes that occur annually in the United States. Risk factors for ischemic stroke include hypertension, diabetes mellitus, hyperlipidemia, sleep apnea, and obesity. Lifestyle modifications, including tobacco cessation, decreased alcohol use, and increased physical activity, are also important in the management of patients with a history of stroke or transient ischemic attack. Antiplatelet therapy is recommended to reduce the risk of recurrent ischemic stroke. The selection of antiplatelet therapy should be based on timing, safety, effectiveness, cost, patient characteristics, and patient preference. Aspirin is recommended as initial treatment to prevent recurrent ischemic stroke. Clopidogrel is recommended as an alternative monotherapy and in patients allergic to aspirin. The combination of clopidogrel and aspirin is not recommended for long-term use (more than two to three years) because of increased bleeding risk. Aspirin/dipyridamole is at least as effective as aspirin alone, but it is not as well tolerated. Warfarin should not be used for prevention of recurrent ischemic stroke.
Stroke is the fifth-leading cause of death in the United States.1 The total cost of direct stroke-related medical care is projected to rise from $71.6 billion in 2012 to $184.1 billion by 2030.1 Out of the 795,000 strokes each year in the United States, 691,000 are ischemic, and 185,000 are recurrent events.1 The American Heart Association (AHA) and the American Stroke Association (ASA) define a transient ischemic attack (TIA) as a transient episode of neurologic dysfunction caused by focal brain, spinal cord, or retinal ischemia without acute infarction.2 They define an ischemic stroke as brain, spinal cord, or retinal cell death due to ischemia based on neuropathology, neuroimaging, or clinical evidence of permanent injury.3
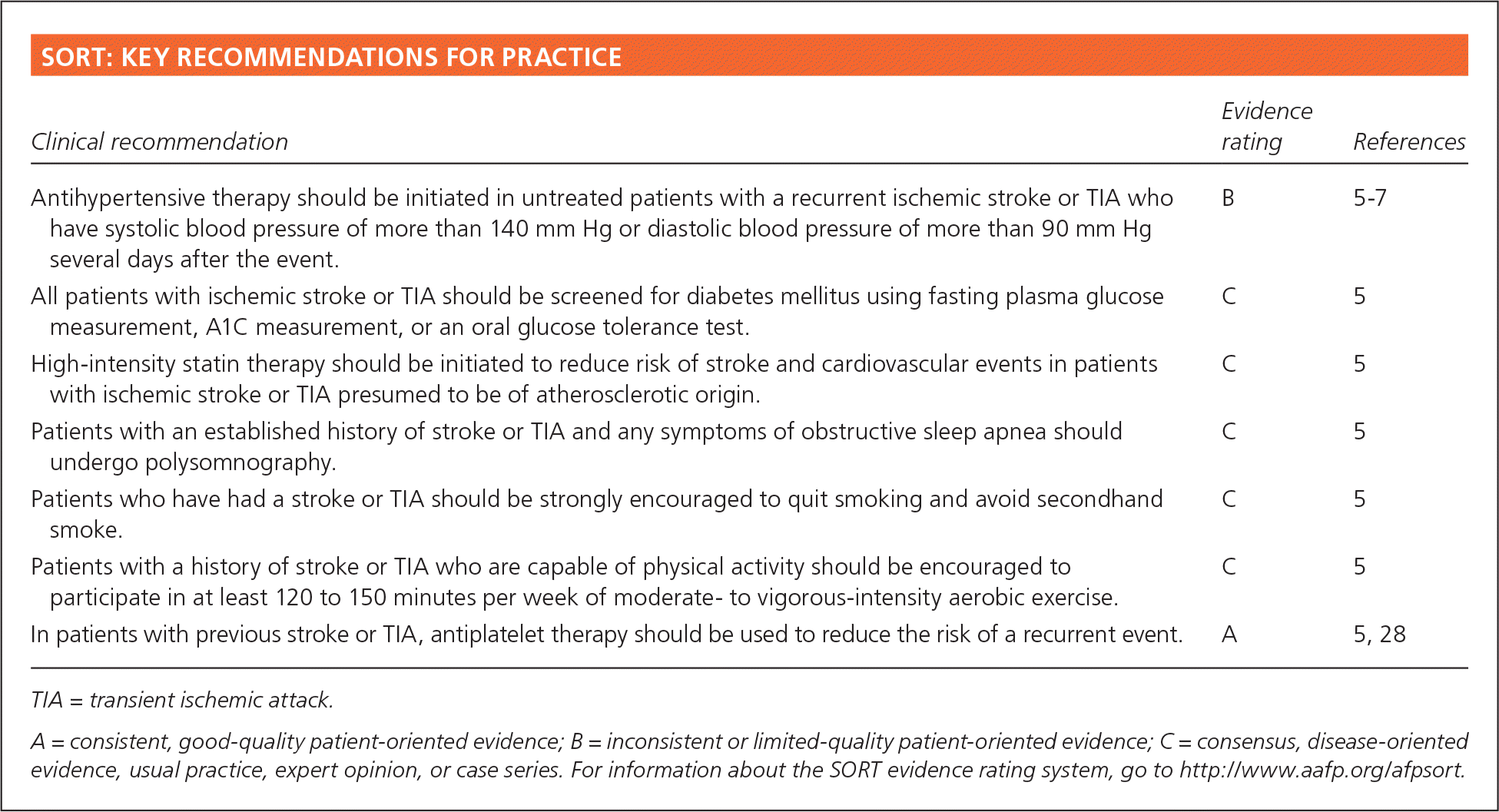
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Antihypertensive therapy should be initiated in untreated patients with a recurrent ischemic stroke or TIA who have systolic blood pressure of more than 140 mm Hg or diastolic blood pressure of more than 90 mm Hg several days after the event. | B | 5–7 |
| All patients with ischemic stroke or TIA should be screened for diabetes mellitus using fasting plasma glucose measurement, A1C measurement, or an oral glucose tolerance test. | C | 5 |
| High-intensity statin therapy should be initiated to reduce risk of stroke and cardiovascular events in patients with ischemic stroke or TIA presumed to be of atherosclerotic origin. | C | 5 |
| Patients with an established history of stroke or TIA and any symptoms of obstructive sleep apnea should undergo polysomnography. | C | 5 |
| Patients who have had a stroke or TIA should be strongly encouraged to quit smoking and avoid secondhand smoke. | C | 5 |
| Patients with a history of stroke or TIA who are capable of physical activity should be encouraged to participate in at least 120 to 150 minutes per week of moderate- to vigorous-intensity aerobic exercise. | C | 5 |
| In patients with previous stroke or TIA, antiplatelet therapy should be used to reduce the risk of a recurrent event. | A | 5, 28 |
TIA = transient ischemic attack.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
About one-half of patients who survive an ischemic stroke or TIA are at increased risk of recurrent stroke within a few days or weeks of the initial event, with the greatest risk during the first week.4 Patients who have a TIA have a 10-year stroke risk of 19% and a combined 10-year risk of stroke, myocardial infarction, and vascular death of 43%.1 Recurrent events lead to prolonged hospitalization, worsened functional outcome, and increased mortality.
This article discusses current recommendations for risk factor management and antithrombotic therapy for the prevention of recurrent ischemic stroke based on the AHA/ASA guidelines, with a focus on non-cardioembolic stroke management. Preventing a TIA and preventing an ischemic stroke are equally important, and the current AHA/ASA guidelines apply to both.5
Risk Factors for Recurrent Stroke
HYPERTENSION
Hypertension is a major risk factor for ischemic stroke, and its treatment can drastically reduce the risk of recurrent ischemic stroke.5 Two major trials—PATS (Post-stroke Antihypertensive Treatment Study), which studied a diuretic, and PROGRESS (Perindopril Protection Against Recurrent Stroke Study), which studied an angiotensin-converting enzyme inhibitor alone or in combination with a diuretic—demonstrated that lowering blood pressure was associated with marked reduction in recurrent stroke risk.6,7
The AHA/ASA guidelines recommend lifestyle interventions, such as weight loss, a Mediterranean-style diet, reduced sodium intake, regular aerobic physical activity, and limited alcohol consumption, to lower blood pressure.5,8 The guidelines also recommend initiating blood pressure therapy in untreated patients with a recurrent ischemic stroke or TIA who have systolic blood pressure of more than 140 mm Hg or diastolic blood pressure of more than 90 mm Hg several days after the event; the benefit of starting therapy in patients with lower blood pressure is unclear.5 Treatment should be individualized, with a recommended blood pressure goal of less than 140 mm Hg systolic or 90 mm Hg diastolic, and the mechanism of action and the patient's medical history (e.g., history of diabetes mellitus, renal disease, or cardiovascular disease) should be considered. For patients with previous lacunar stroke, the recommended goal is a systolic blood pressure of less than 130 mm Hg.5 Current evidence suggests using thiazide diuretics alone or in combination with an angiotensin-converting enzyme inhibitor.5–7
DIABETES
The AHA/ASA recommends screening all patients with a TIA or ischemic stroke for diabetes using a fasting plasma glucose measurement, A1C measurement, or oral glucose tolerance test and then following American Diabetes Association guidelines for glycemic control.5 There are no trials that look at specific therapies for the secondary prevention of stroke and TIA in patients with diabetes.
HYPERLIPIDEMIA
The 2013 American College of Cardiology/AHA Guideline on the Treatment of Blood Cholesterol to Reduce Atherosclerotic Cardiovascular Risk in Adults focuses on patient risk instead of specific cholesterol targets.9 Patients with recurrent stroke or TIA presumed to be of atherosclerotic origin, regardless of low-density lipoprotein cholesterol level, should receive high-intensity statin therapy such as atorvastatin (Lipitor), 40 mg or more, or rosuvastatin (Crestor), 20 mg.5,10,11 This recommendation is based on a meta-analysis of statins vs. placebo that showed that statins reduced the risk of cerebrovascular disease in persons with or without cerebrovascular disease,12 and on the SPARCL (Stroke Prevention by Aggressive Reduction in Cholesterol Levels) trial, which demonstrated a lower risk of recurrent stroke after a recent stroke or TIA.13 Benefits in patients older than 75 years, including all-cause mortality and primary prevention, have not been established. Because of unclear benefits and possible adverse effects and drug-drug interactions, there is uncertainty regarding statin use after 75 years of age.14
Obesity has not been established as a risk factor for recurrent stroke, even though it is associated with vascular risk factors, such as diabetes, hypertension, and hyperlipidemia, and there is a 5% increased risk of first stroke for every 1 kg per m2 increase in body mass index over 20 kg per m2.10,15 Recent studies indicate that obese patients with stroke have a somewhat lower risk of having another major vascular event (i.e., stroke, myocardial infarction, or vascular death) than nonobese patients.16,17 Therefore, the role of weight loss recommendations in obese patients with stroke is uncertain based on the available data.18
OBSTRUCTIVE SLEEP APNEA
Polysomnography is recommended for patients with an established history of stroke or TIA and any symptoms of obstructive sleep apnea.5,19 Among patients with previous stroke or TIA, 50% to 75% have sleep apnea, which is often undiagnosed.5,20 Sleep apnea symptoms may include daytime sleepiness, loud snoring, witnessed breathing interruptions, or awakenings because of gasping or choking.19
TOBACCO USE
Cigarette smoking is an independent risk factor for first ischemic stroke5,21 and increases the risk of silent brain infarction.22 Exposure to environmental or passive secondhand smoke may also contribute to the risk of stroke.5 Although data are limited, one study showed an increased risk of recurrent stroke in older smokers.23 Patients who have had a stroke or TIA should be strongly encouraged to quit smoking and avoid secondhand smoke.5
ALCOHOL USE
Heavy alcohol use (more than two drinks per day) and binge drinking (more than four drinks in one sitting) may increase the risk of recurrent stroke.24 Heavy drinkers with a history of stroke or TIA should eliminate or reduce their alcohol consumption. One or two drinks per day for men and one drink per day for nonpregnant women may be reasonable for prevention of recurrent stroke.5 Non-drinkers who have had a stroke should not start drinking.
PHYSICAL ACTIVITY
Regular physical activity improves stroke risk factors and may also reduce stroke risk itself.5 There are currently two ongoing trials to help clarify the role of physical activity in the prevention of recurrent stroke.25,26 Patients with a history of stroke or TIA should be encouraged to participate in at least 120 to 150 minutes of aerobic physical activity per week, involving moderate-intensity exercise (e.g., brisk walking) or vigorous-intensity exercise (e.g., jogging).5 Barriers to physical activity in patients with stroke may include motor weakness, altered proprioception and balance, and impaired cognition.22 Structured physical therapy or cardiac rehabilitation should be considered for those with exercise barriers.5
Antithrombotic Therapy
The AHA/ASA guidelines recommend the use of anti-platelet agents to reduce the risk of a recurrent event.5 Three options are approved by the U.S. Food and Drug Administration: aspirin, clopidogrel (Plavix), and aspirin/dipyridamole (Aggrenox).5 The relative risk reduction from antiplatelet therapy for recurrent ischemic stroke is approximately 22%, with a number needed to treat of 28 over 2.5 years.27 The selection of antiplatelet therapy should be based on timing, safety, effectiveness, cost, patient characteristics, and patient preference (Table 1).28
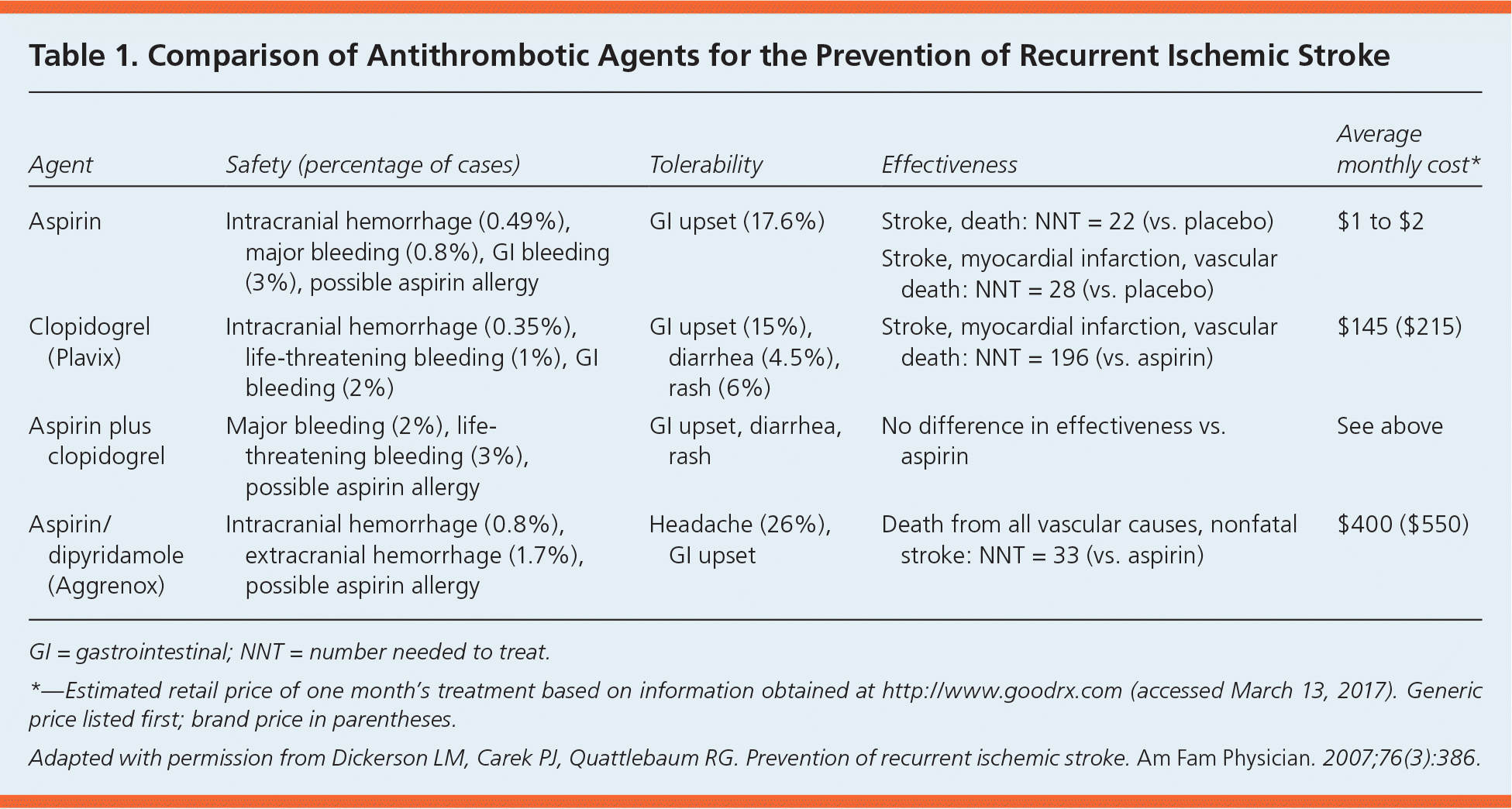
Table 1. Comparison of Antithrombotic Agents for the Prevention of Recurrent Ischemic Stroke
| Agent | Safety (percentage of cases) | Tolerability | Effectiveness | Average monthly cost* |
|---|---|---|---|---|
| Aspirin | Intracranial hemorrhage (0.49%), major bleeding (0.8%), GI bleeding (3%), possible aspirin allergy | GI upset (17.6%) | Stroke, death: NNT = 22 (vs. placebo) | $1 to $2 |
| Stroke, myocardial infarction, vascular death: NNT = 28 (vs. placebo) | ||||
| Clopidogrel (Plavix) | Intracranial hemorrhage (0.35%), life-threatening bleeding (1%), GI bleeding (2%) | GI upset (15%), diarrhea (4.5%), rash (6%) | Stroke, myocardial infarction, vascular death: NNT = 196 (vs. aspirin) | $145 ($215) |
| Aspirin plus clopidogrel | Major bleeding (2%), life-threatening bleeding (3%), possible aspirin allergy | GI upset, diarrhea, rash | No difference in effectiveness vs. aspirin | See above |
| Aspirin/dipyridamole (Aggrenox) | Intracranial hemorrhage (0.8%), extracranial hemorrhage (1.7%), possible aspirin allergy | Headache (26%), GI upset | Death from all vascular causes, nonfatal stroke: NNT = 33 (vs. aspirin) | $400 ($550) |
GI = gastrointestinal; NNT = number needed to treat.
*—Estimated retail price of one month's treatment based on information obtained at http://www.goodrx.com (accessed March 13, 2017). Generic price listed first; brand price in parentheses.
Adapted with permission from Dickerson LM, Carek PJ, Quattlebaum RG. Prevention of recurrent ischemic stroke. Am Fam Physician. 2007;76(3):386.
ASPIRIN
Aspirin, 50 to 325 mg daily, is recommended for initial therapy to prevent recurrent ischemic stroke. The benefit is similar for any dose, but the adverse effect profiles vary greatly.27,29–33 The major adverse reaction is gastrointestinal bleeding, which increases with increased daily dosing.29,30 Patients taking 325 mg or less daily have a 0.4% annual risk of gastrointestinal bleeding.32–35 For patients who have a recurrent stroke during aspirin therapy, there is no clear evidence that increasing the dose of aspirin decreases the risk of another event.5 Aspirin is the most cost-effective therapy option.
CLOPIDOGREL
Clopidogrel monotherapy, 75 mg daily, is recommended for secondary prevention of stroke and can also be used in patients who are allergic to aspirin.5 Comparison studies show that patients taking clopidogrel monotherapy, aspirin monotherapy, or aspirin/dipyridamole have similar rates of recurrent stroke and TIA.5 Clopidogrel is considered to be as safe as aspirin with fewer bleeding episodes.36
The effectiveness of clopidogrel may be decreased when used with a proton pump inhibitor because of possible cytochrome P450 2C19 interactions. For patients with concomitant gastroesophageal reflux disease, a histamine H2 blocker or pantoprazole (Protonix) should be used instead of omeprazole (Prilosec) because of its decreased effects at CYP2C19.34,36,37
ASPIRIN PLUS CLOPIDOGREL
The CHANCE (Clopidogrel in High-Risk Patients with Acute Nondisabling Cerebrovascular Events) trial demonstrated that starting aspirin plus clopidogrel within 24 hours of a minor ischemic stroke or TIA and continuing it for up to 21 days may prevent recurrent stroke.38 The aspirin plus clopidogrel combination is not recommended for long-term use (more than two to three years) because bleeding risk increases.5 Two trials comparing aspirin plus clopidogrel with each therapy alone did not show an improvement in recurrent stroke or TIA rates, and the combination increased bleeding events.35,39
ASPIRIN/DIPYRIDAMOLE
Aspirin/dipyridamole, 25 mg/200 mg twice daily, is indicated for initial therapy after TIA or ischemic stroke for recurrent stroke prevention.5,40,41 In one trial, aspirin/dipyridamole demonstrated a 33% relative risk reduction vs. placebo for stroke or death, with a number needed to treat of 11.40 In a second trial, aspirin/dipyridamole demonstrated a 23% relative risk reduction vs. aspirin monotherapy for stroke.41 When the trials were compared, the combination was at least as effective as aspirin alone for secondary stroke prevention, but it was not as well tolerated as aspirin monotherapy.5
WARFARIN
Vitamin K antagonists such as warfarin (Coumadin) are no better than other antiplatelet therapies with increased bleeding risk, and they are not recommended for prevention of recurrent ischemic stroke.42–44
This article updates previous articles on this topic by Dickerson, et al.28; Ezekowitz, et al.45; Ryan, et al.46; and Hart and Benavente.47
Data Sources: We searched PubMed, Cochrane Database of Systematic Reviews, U.S. Preventive Services Task Force, and UpToDate. The search included meta-analyses, randomized controlled trials, clinical trials, guidelines, and reviews. The key terms strokes and recurrent were searched with the other key terms diet, salt reduction, DASH diet, exercise, weight loss, smoking, obstructive sleep apnea, meditation, alcohol use, and supplements. Search dates: September 1, 2016, to January 8, 2017.

