Clinical Question
What is the best way to assess bleeding risk in patients with atrial fibrillation who are taking anticoagulants?
Evidence Summary
Family physicians are often faced with the dilemma of balancing the benefit of stroke prevention with the risk of major bleeding when deciding on anticoagulation treatment in patients with atrial fibrillation. Over the past 10 years, several decision support tools have been developed and validated to assess the risk of major bleeding in patients taking anticoagulants. Major bleeding is typically defined as bleeding that requires hospitalization or transfusion, or a decrease in hemoglobin of at least 2 g per dL (20 g per L). Most tools share common risk factors, such as advanced age, previous bleeding, and renal/liver impairment.1,2
The ATRIA tool includes five risk factors and was developed in a study of 9,186 patients with nontransient, nonvalvular atrial fibrillation who were receiving warfarin (Coumadin), with five-year follow-up.3 The major limitation is the lack of information about aspirin use in the study patients. The HAS-BLED tool (https://www.mdcalc.com/has-bled-score-major-bleeding-risk) includes seven risk factors and was developed in a study of 3,978 patients with nontransient, nonvalvular atrial fibrillation who were receiving oral anticoagulant monotherapy, an oral anticoagulant combined with an antiplatelet drug, an antiplatelet drug alone, or no anti-thrombotic therapy.4 The overall mean age was 67 years, and 59% of study patients were men. Patients were followed for one year to assess for major bleeding events. The limitation of this tool is that 25% of the data regarding the occurrence of major bleeding during follow-up were missing, contributing to a very low major bleeding rate of 1.5%.4 This may introduce the possibility of selection bias. The HAS-BLED tool is currently recommended by the European Society of Cardiology 5 and the Canadian Cardiovascular Society 6 for bleeding risk assessment in patients with atrial fibrillation. Both tools are summarized in Table 1.3,4
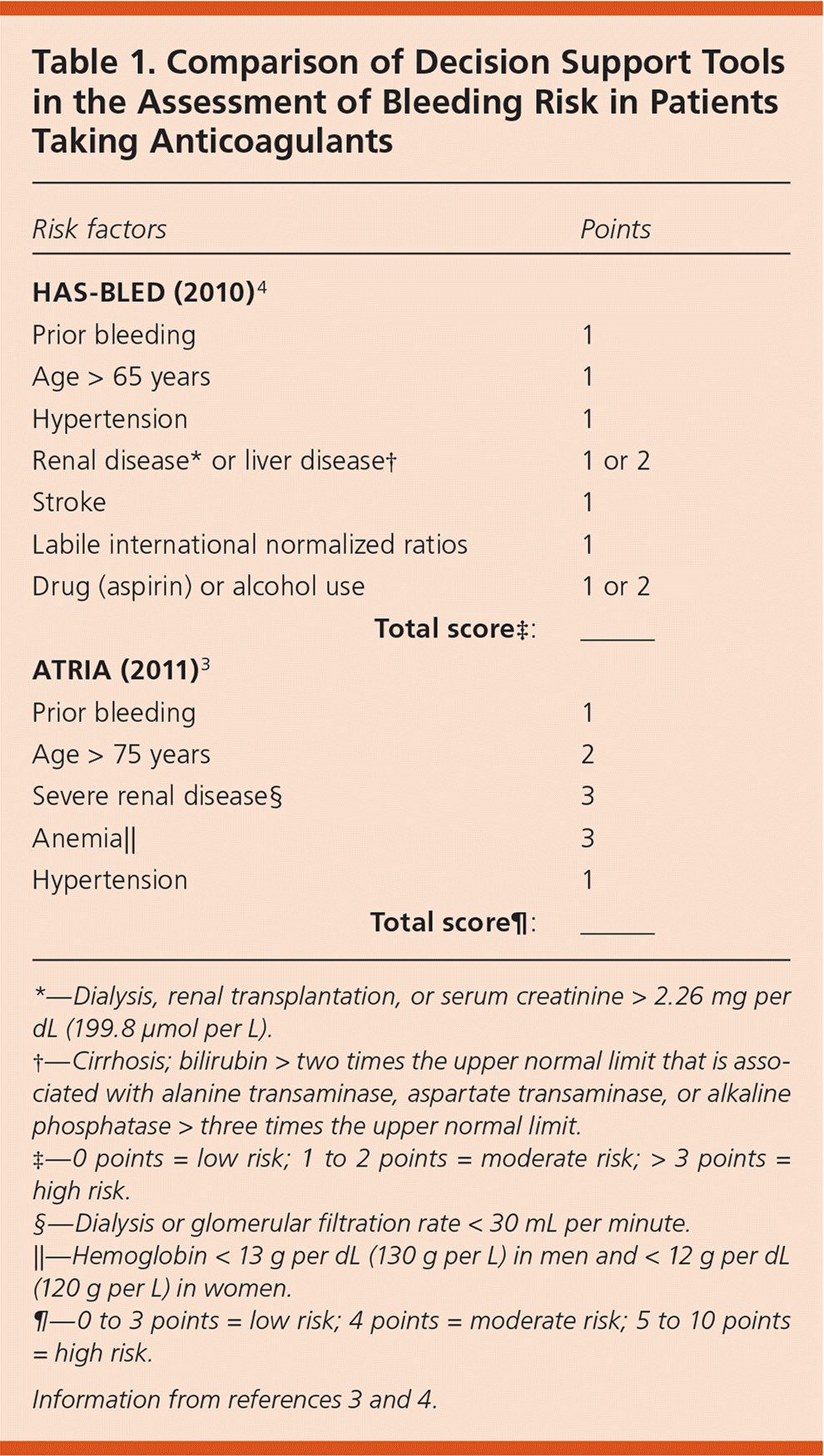
Table 1. Comparison of Decision Support Tools in the Assessment of Bleeding Risk in Patients Taking Anticoagulants
| Risk factors | Points |
|---|---|
| HAS-BLED (2010)4 | |
| Prior bleeding | 1 |
| Age > 65 years | 1 |
| Hypertension | 1 |
| Renal disease* or liver disease† | 1 or 2 |
| Stroke | 1 |
| Labile international normalized ratios | 1 |
| Drug (aspirin) or alcohol use | 1 or 2 |
| Total score‡: | — |
| ATRIA (2011)3 | |
| Prior bleeding | 1 |
| Age > 75 years | 2 |
| Severe renal disease§ | 3 |
| Anemia‖ | 3 |
| Hypertension | 1 |
| Total score¶: | — |
*—Dialysis, renal transplantation, or serum creatinine > 2.26 mg per dL (199.8 μmol per L).
†—Cirrhosis; bilirubin > two times the upper normal limit that is associated with alanine transaminase, aspartate transaminase, or alkaline phosphatase > three times the upper normal limit.
‡—0 points = low risk; 1 to 2 points = moderate risk; ≥ 3 points = high risk.
§—Dialysis or glomerular filtration rate < 30 mL per minute.
‖—Hemoglobin < 13 g per dL (130 g per L) in men and < 12 g per dL (120 g per L) in women.
¶—0 to 3 points = low risk; 4 points = moderate risk; 5 to 10 points = high risk.
See https://www.mdcalc.com/has-bled-score-major-bleeding-risk for an online calculator based on the HAS-BLED scoring system.
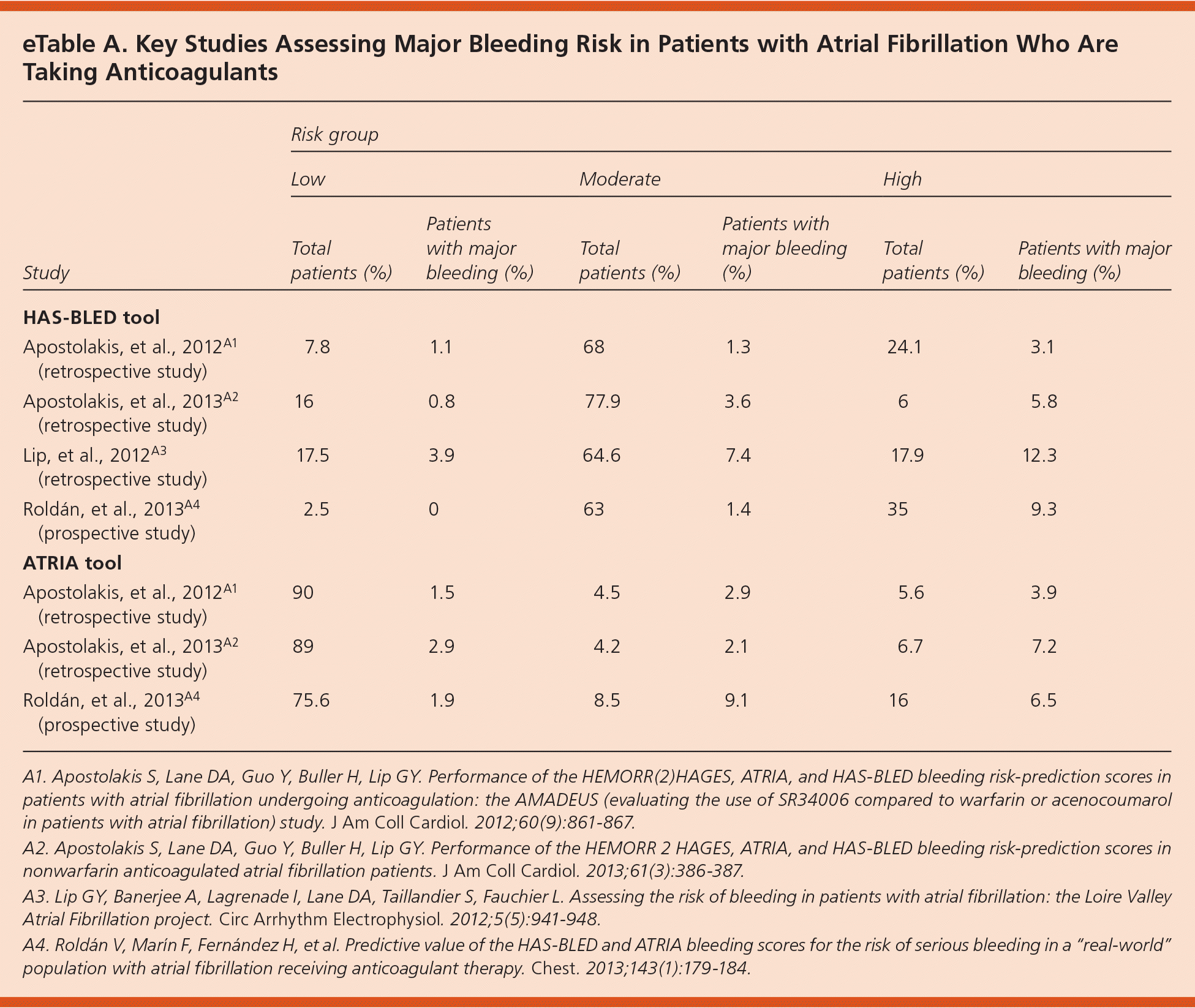
In several retrospective studies, the HAS-BLED tool showed better or equivalent predictive accuracy when compared with the ATRIA tool7–10 (eTable A). Higher-quality evidence from a prospective cohort study showed better predictive value with the HAS-BLED tool (bleeding risk of 0%, 1.4%, and 9.3% in low-, moderate-, and high-risk groups, respectively) compared with the ATRIA tool (1.9%, 9.1%, and 6.5%).11 However, in the same study, the ATRIA tool identified a larger number of patients as low risk than the HAS-BLED tool (75.6% vs. 2.5%).
eTable A. Key Studies Assessing Major Bleeding Risk in Patients with Atrial Fibrillation Who Are Taking Anticoagulants
| Risk group | ||||||
|---|---|---|---|---|---|---|
| Low | Moderate | High | ||||
| Study | Total patients (%) | Patients with major bleeding (%) | Total patients (%) | Patients with major bleeding (%) | Total patients (%) | Patients with major bleeding (%) |
| HAS-BLED tool | ||||||
| Apostolakis, et al., 2012A1 (retrospective study) | 7.8 | 1.1 | 68 | 1.3 | 24.1 | 3.1 |
| Apostolakis, et al., 2013A2 (retrospective study) | 16 | 0.8 | 77.9 | 3.6 | 6 | 5.8 |
| Lip, et al., 2012A3 (retrospective study) | 17.5 | 3.9 | 64.6 | 7.4 | 17.9 | 12.3 |
| Roldán, et al., 2013A4 (prospective study) | 2.5 | 0 | 63 | 1.4 | 35 | 9.3 |
| ATRIA tool | ||||||
| Apostolakis, et al., 2012A1 (retrospective study) | 90 | 1.5 | 4.5 | 2.9 | 5.6 | 3.9 |
| Apostolakis, et al., 2013A2 (retrospective study) | 89 | 2.9 | 4.2 | 2.1 | 6.7 | 7.2 |
| Roldán, et al., 2013A4 (prospective study) | 75.6 | 1.9 | 8.5 | 9.1 | 16 | 6.5 |
A1. Apostolakis S, Lane DA, Guo Y, Buller H, Lip GY. Performance of the HEMORR(2)HAGES, ATRIA, and HAS-BLED bleeding risk-prediction scores in patients with atrial fibrillation undergoing anticoagulation: the AMADEUS (evaluating the use of SR34006 compared to warfarin or acenocoumarol in patients with atrial fibrillation) study. J Am Coll Cardiol . 2012;60(9):861–867.
A2. Apostolakis S, Lane DA, Guo Y, Buller H, Lip GY. Performance of the HEMORR 2 HAGES, ATRIA, and HAS-BLED bleeding risk-prediction scores in nonwarfarin anticoagulated atrial fibrillation patients. J Am Coll Cardiol. 2013;61(3):386–387.
A3. Lip GY, Banerjee A, Lagrenade I, Lane DA, Taillandier S, Fauchier L. Assessing the risk of bleeding in patients with atrial fibrillation: the Loire Valley Atrial Fibrillation project. Circ Arrhythm Electrophysiol. 2012;5(5):941–948.
A4. Roldán V, Marín F, Fernández H, et al. Predictive value of the HAS-BLED and ATRIA bleeding scores for the risk of serious bleeding in a “real-world” population with atrial fibrillation receiving anticoagulant therapy. Chest. 2013;143(1):179–184.
A recent systematic review and meta-analysis compared the two scores in the high-bleeding-risk category. The pooled sensitivity and specificity of HAS-BLED for predicting high bleeding risk were 41% and 78%, respectively, compared with 23% and 91% for ATRIA.12 The study was limited because it included heterogeneous studies, not all patients were anticoagulated, and different anticoagulants were used. Overall, the HAS-BLED tool appears to be more sensitive and easy-to-use, and thus is recommended for assessment of major bleeding risk.
Risk stratification using the tools can guide physicians in informed decision making and providing adequate follow-up and monitoring. However, it is important to keep in mind that all the tools share some limitations. All were derived from patients already taking anticoagulants, so patients who were considered too high risk for anticoagulation were not included. Therefore, these tools may underestimate the true risk of major bleeding, especially in older patients with multiple comorbidities. Regardless of which tool is used, physicians should use their best clinical judgment and focus on identifying and minimizing modifiable risk factors such as hypertension, alcohol use, unnecessary concomitant antiplatelet agents, and fall risk.
Applying the Evidence
A 78-year-old woman with a history of hypertension, stroke, and moderate dementia presented at a routine office visit with atrial fibrillation and a normal ventricular rate. She was not in discomfort. It was not clear how long she had been in atrial fibrillation. She used a walker for ambulation. She did not drink alcohol but took aspirin (81 mg) in addition to other medications. She had no history of major bleeding, renal disease, or liver disease.
Her HAS-BLED score was 4, putting her at high risk of major bleeding. Therefore, the physician decided against anticoagulation.

