A 24-year-old woman (gravida 1 para 1) gave birth via spontaneous vaginal delivery. At birth, the newborn had a red lesion on the crown of her head. There was no family history of congenital skin abnormalities. Prenatal laboratory test results were normal.
The newborn examination revealed a 3.5- × 2-cm erythematous lesion on the scalp (Figures 1 and 2). The lesion was well-circumscribed and surrounded by a collar of hair. Ultrasonography revealed an anechoic subcutaneous mass that was 14 × 18 × 6 mm in size. The lesion was not connected to the brain.
Figure 1.
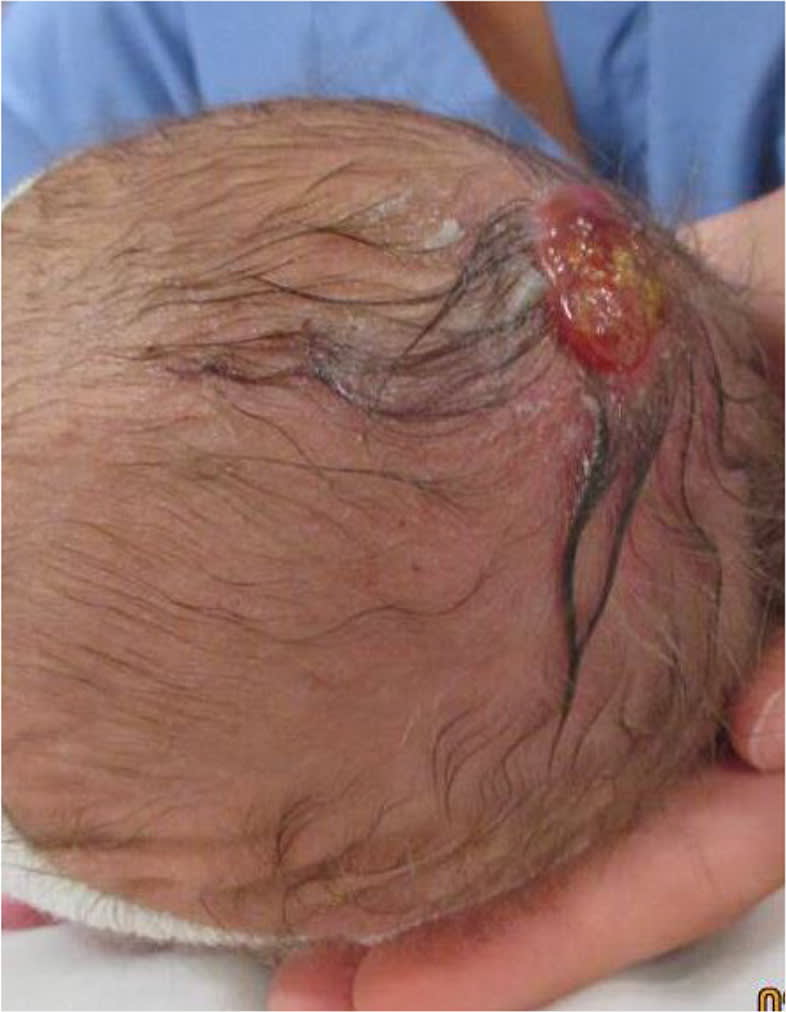
Figure 2.
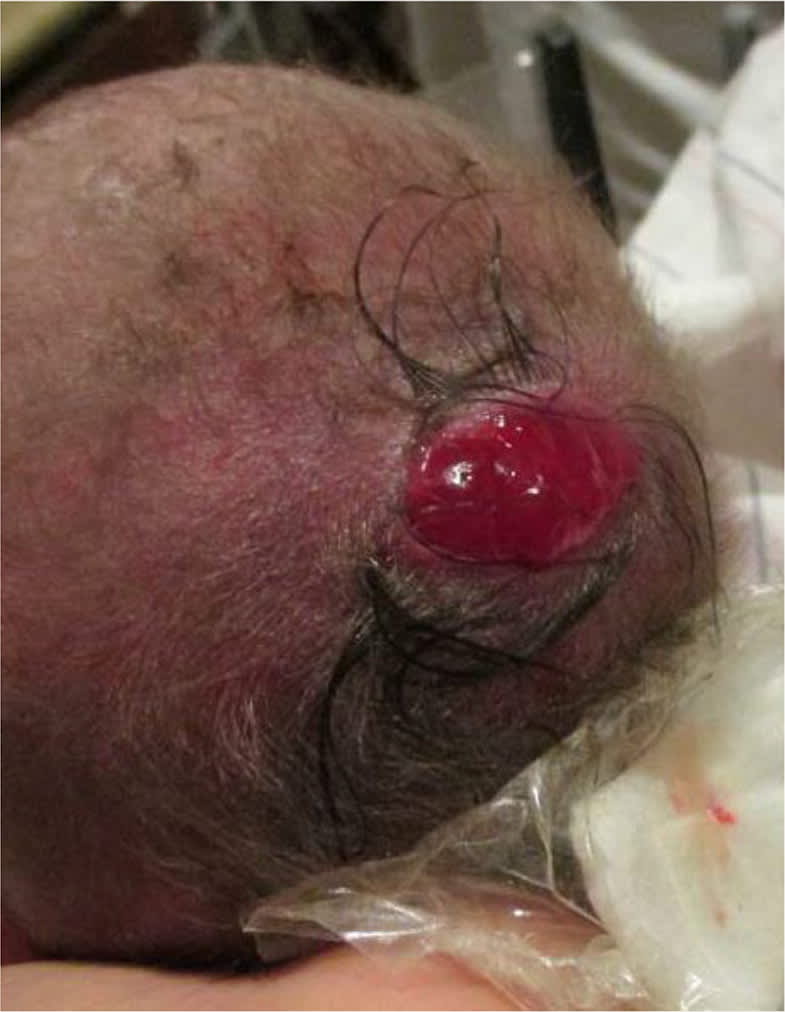
Question
Based on the patient's history, physical examination, and ultrasound findings, which one of the following is the most likely diagnosis?
A. Aplasia cutis congenita.
B. Epidermolysis bullosa.
C. Erosion from herpes simplex virus.
D. Nevus sebaceus.
Discussion
The answer is A: aplasia cutis congenita. Aplasia cutis congenita is the absence of skin in a localized area of the scalp or trunk. It may be associated with other rare congenital syndromes such as epidermolysis bullosa, trisomy 13 syndrome, and limb defects.1,2 The condition is underreported, and some estimate that it occurs in one out of 3,000 births.3 It may be inherited in an autosomal dominant or recessive pattern.3 There are several types of aplasia cutis congenita. This newborn had the membranous form, which is most common.
Membranous aplasia cutis congenita is characterized by oval or round, well-circumscribed lesions with a punched-out appearance. They are usually less than 1 cm in size.1 The surface is atrophic, thin, glistening, and membrane-like.1 Bullous lesions that are drained may reform to the more typical flat appearance. The most common location is on the vertex of the scalp, but it may also occur on the parietal scalp off the midline. Lesions associated with underlying bone defects are typically larger (more than 3 cm) and have an irregular or stellate appearance. A collar of coarse hair surrounds the lesion (hair collar sign).
Midline lesions are thought to be caused by incomplete closure of the neural tube. Lateral lesions may occur because of incomplete closure of embryonic fusion lines. Histologic findings of aplasia cutis congenita are characteristic and include an atrophic and flattened epidermis with a normal superficial dermis replaced by loose connective tissue.1
Management of aplasia cutis congenita depends on the size, location, and presence of ulceration. Larger lesions may require surgical excision because of significant visible deformity. Large, stellate lesions require magnetic resonance imaging before excision because they are associated with rare but major complications.2
Epidermolysis bullosa is a genetic disease in which minor skin trauma causes noninflammatory blistering.4 It is not associated with underlying bony deformities. It occurs on the hands and feet but may be generalized. Depending on the layers of the skin involved, scarring is possible.
Herpes simplex virus lesions can present on the vertex of the scalp. However, there are usually several scattered vesicles that may have eroded and crusted. The lesions may follow a dermatome.
Nevus sebaceus is also found on the scalp and is oval to linear in shape. In infants and children, it presents as a smooth, waxy, hairless plaque. It presents as epidermal hyperplasia during puberty and secondary neoplasia in adults.4 Nevus sebaceus of Jadassohn is a rare subtype that includes a linear nevus sebaceus, convulsions, and intellectual disability.4
Summary Table

| Condition | Characteristics |
|---|---|
| Aplasia cutis congenita | Primarily occurs along vertex of scalp; small (< 1 cm), oval or round, well-circumscribed lesions with a punched-out appearance; atrophic surface with thin, glistening membrane; collar of coarse hair surrounds the lesion (hair collar sign) |
| Epidermolysis bullosa | Minor skin trauma causing noninflammatory blistering with or without scarring (depending on location); simplex form: blisters and erosions on the hands and feet; junctional form: persistent erosions on the central face and buttocks; dystrophic form: blisters that heal with scarring |
| Erosion from herpes simplex virus | Scattered vesicles that may have eroded and crusted; may follow a dermatome |
| Nevus sebaceus | Oval to linear; infants and children: smooth, waxy, hairless, thickenings of the skin; during puberty: epidermal hyperplasia; adults: secondary neoplasia |

