A 29-year-old woman with a history of oral herpes simplex virus presented with sore throat, cough, headache, fatigue, and a reported fever of 102°F (38.9°C). She had experienced malaise over the previous three weeks. Mouth lesions and a burning sensation when she drank hot tea developed about two days before presentation.
On physical examination, the patient was not in acute distress, and she had normal vital signs. She had mildly tender anterior and posterior cervical lymphadenopathy. Vesicular lesions were visible on the bilateral labial commissures, and the dorsal tongue had well-demarcated bare patches with raised erythematous borders (Figure 1). The tongue lesions seemed to change and migrate daily. She had no genital lesions.
FIGURE 1
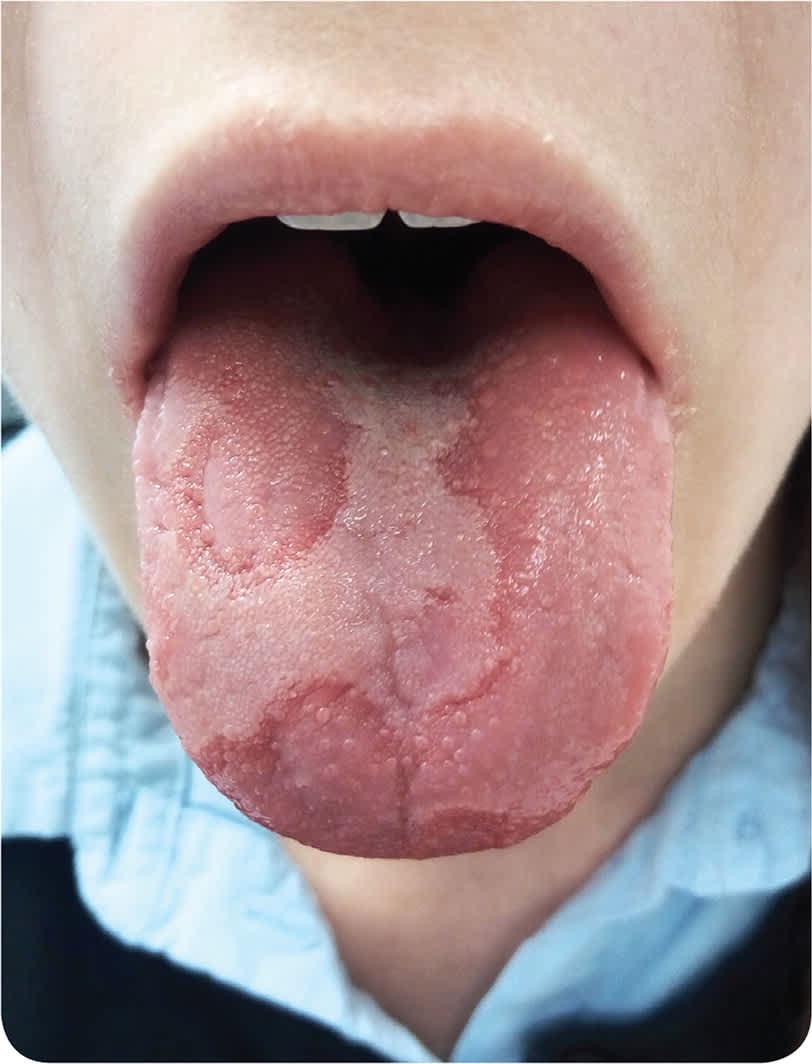
Laboratory findings included a negative rapid streptococcal test result and a nonreactive human immunodeficiency virus test, but a positive mononucleosis spot test result. A throat culture was positive for non–group A beta-hemolytic streptococcus.
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Atrophic glossitis.
B. Behçet syndrome.
C. Burning tongue.
D. Geographic tongue.
E. Oral hairy leukoplakia.
Discussion
The answer is D: geographic tongue, also known as benign migratory glossitis. The condition often resembles a map of the world, hence its name.1 It is thought to be an inflammatory disorder of unknown etiology.2 Focal regions of papillary atrophy on the dorsum of the tongue lead to ulcer-like patches surrounded by serpiginous, erythematous borders. The patches can rapidly resolve and migrate.3 Geographic tongue affects 1% to 14% of the U.S. population and has an inverse correlation with smoking, but there is no clearly established association with a disease process.3
Geographic tongue is usually self-limited and requires no treatment. Some patients with geographic tongue may report tongue sensitivities to hot or spicy foods.4 Topical steroid gels and antihistamine mouth rinses may reduce sensitivity.3
This patient tested positive for mononucleosis and non–group A beta-hemolytic streptococcus. However, these illnesses were not associated with the tongue findings.
Atrophic glossitis has a smooth, glossy appearance on a pink or red background.3 There is uniform atrophy of the papillae. The condition is often associated with a nutritional deficiency (e.g., iron, folic acid, vitamin B12, riboflavin, niacin) or an underlying systemic infection (e.g., syphilis). It may also be related to localized candidal infection, amyloidosis, celiac disease, protein-calorie malnutrition, or xerostomia.3
Behçet syndrome is a neutrophilic inflammatory disorder resulting in recurrent, nonchanging oral aphthae and often genital ulcers.5 Lesions have a white-yellow necrotic base with surrounding erythema and well-defined borders. The diagnosis requires recurrent oral ulcerations (more than twice in one year) in addition to two other clinical findings: genital ulcers, eye lesions, skin lesions, or a positive pathergy test result.5
Burning tongue is the sudden onset of a scalded tongue sensation that becomes more frequent throughout the day.3,6 The sensation can present as a primary syndrome or secondary to an underlying condition that leads to the degradation of the tongue surface, such as candidal infection or a vitamin deficiency.3 The tongue often appears normal.3,6
Oral hairy leukoplakia is characterized by white patches on the lateral borders and occasionally on the dorsum of the tongue.7 The patches do not scrape off. Oral hairy leukoplakia is caused by intense replication of Epstein-Barr virus and often occurs in patients with human immunodeficiency virus infection.3,7 Patients with this condition do not usually have a fever, and it is not considered premalignant.7
SUMMARY TABLE
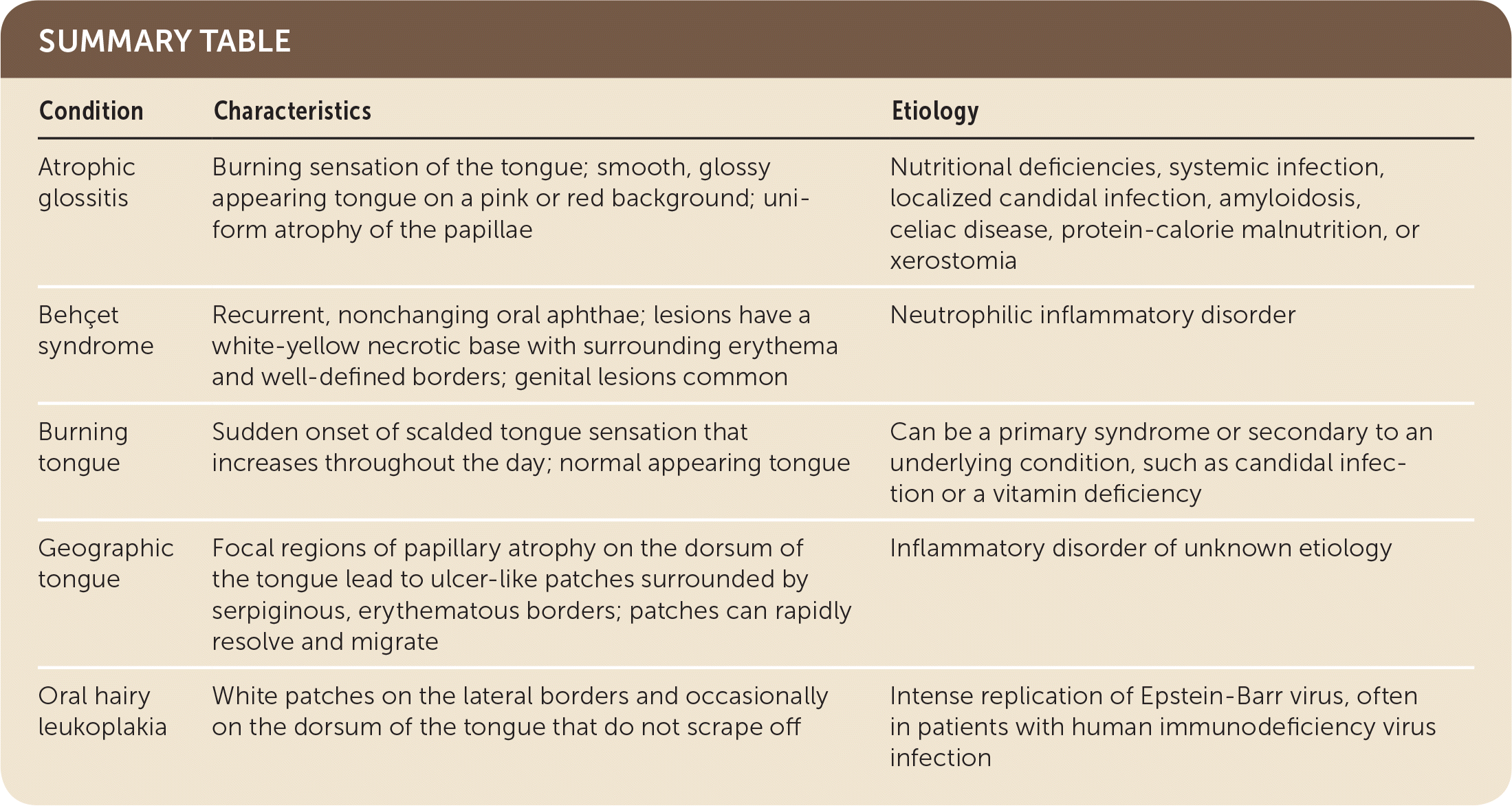
| Condition | Characteristics | Etiology |
|---|---|---|
| Atrophic glossitis | Burning sensation of the tongue; smooth, glossy appearing tongue on a pink or red background; uniform atrophy of the papillae | Nutritional deficiencies, systemic infection, localized candidal infection, amyloidosis, celiac disease, protein-calorie malnutrition, or xerostomia |
| Behçet syndrome | Recurrent, nonchanging oral aphthae; lesions have a white-yellow necrotic base with surrounding erythema and well-defined borders; genital lesions common | Neutrophilic inflammatory disorder |
| Burning tongue | Sudden onset of scalded tongue sensation that increases throughout the day; normal appearing tongue | Can be a primary syndrome or secondary to an underlying condition, such as candidal infection or a vitamin deficiency |
| Geographic tongue | Focal regions of papillary atrophy on the dorsum of the tongue lead to ulcer-like patches surrounded by serpiginous, erythematous borders; patches can rapidly resolve and migrate | Inflammatory disorder of unknown etiology |
| Oral hairy leukoplakia | White patches on the lateral borders and occasionally on the dorsum of the tongue that do not scrape off | Intense replication of Epstein-Barr virus, often in patients with human immunodeficiency virus infection |

