A 60-year-old woman with a history of nonverbal autism, intellectual disability, and quadriplegia presented with a nonhealing erosion of the left distal index finger and skin changes involving both hands. The patient was unable to provide further history.
Physical examination revealed bilateral thick, adherent, white-gray scaling and crusting involving the hands, fingers, and web spaces with associated fissures. Diffuse xerosis and fine scale on the head, neck, trunk, and other extremities were also noted (Figure 1).
FIGURE 1
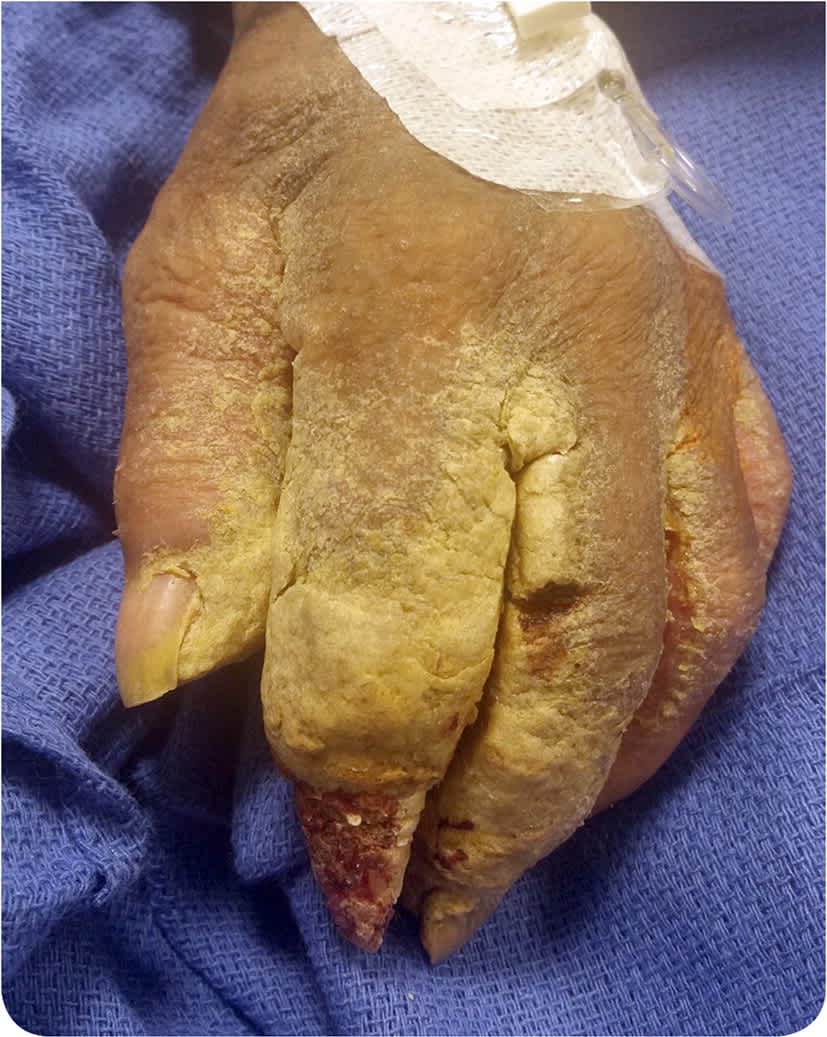
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Atopic dermatitis.
B. Crusted scabies.
C. Psoriasis.
D. Retention hyperkeratosis.
E. Tinea manuum.
Discussion
The answer is B: crusted scabies (also called hyperkeratotic scabies and Norwegian scabies). Crusted scabies presents as a severe and highly contagious form of scabies, characterized by skin hyperinfestation with up to millions of Sarcoptes scabiei mites.1 The heavy mite burden leads to the development of scaly, white-gray, hyperkeratotic plaques typically localized to the scalp, face, hands, feet, or buttocks. Plaques are often associated with deep fissures, making patients prone to secondary bacterial infections and increased risk of sepsis.2
Crusted scabies is most common in individuals with severe immunosuppression (e.g., from human immunodeficiency virus infection or use of immunosuppressant therapy). However, it also occurs in patients with cognitive impairment or physical disabilities who are unable to scratch to decrease the mite burden. Scabies is transmitted by direct skin-to-skin contact, although transmission from bed sheets or contaminated clothing can also occur.1 Because of the large number of mites, crusted scabies is far more contagious than typical scabies. If the infection is unrecognized, there is potential for scabies outbreaks in health care facilities and nursing homes.2
The diagnosis is confirmed with a mineral oil preparation demonstrating mites and/or mite feces. Patients must be isolated to prevent spread. Treatment consists of topical permethrin 5% cream applied every two days for up to 12 weeks, with a three-, five-, or seven-dose regimen of oral ivermectin (Stromectol) depending on severity.1,3 All clothing and bedding should be washed in hot water, then dried using high heat. Exposure to temperatures higher than 122°F (50°C) for 10 minutes will kill mites.4 Contacts should be treated prophylactically with a single application of permethrin 5% cream to the entire body.1
Atopic dermatitis is a chronic, relapsing inflammatory condition with areas of skin that are pruritic, erythematous, xerotic, or hyperkeratotic. It is often associated with asthma and allergic rhinitis. Atopic dermatitis can present on any part of the body, but it is most common in flexural areas. It is a chronic and relapsing disorder with onset usually during childhood.5
Psoriasis is a chronic inflammatory condition causing well-demarcated, pink plaques with adherent, silvery scale. It most commonly affects extensor surfaces (knees and elbows), the scalp, and the trunk. Nail involvement is characterized by pitting, subungual hyperkeratosis (“oil spots”), or separation of the nail plate from the nail bed (onycholysis). The lesions may be pruritic, especially during exacerbations.6
Retention hyperkeratosis, a benign dermatologic condition, is often related to poor hygiene. It is the result of an alteration in the normal desquamation of keratinocytes, resulting in a thickened stratum corneum with a yellow-brown appearance.7
Tinea manuum is a dermatophyte infection of the hands. It is transmitted by direct contact with infected persons or fomites. It presents as mild scaling and erythema on the dorsum of the hands or as chronic dry, scaly hyperkeratosis of the palms. Diagnosis is made by identifying hyphae on a potassium hydroxide preparation of lesion scrapings.8
SUMMARY TABLE
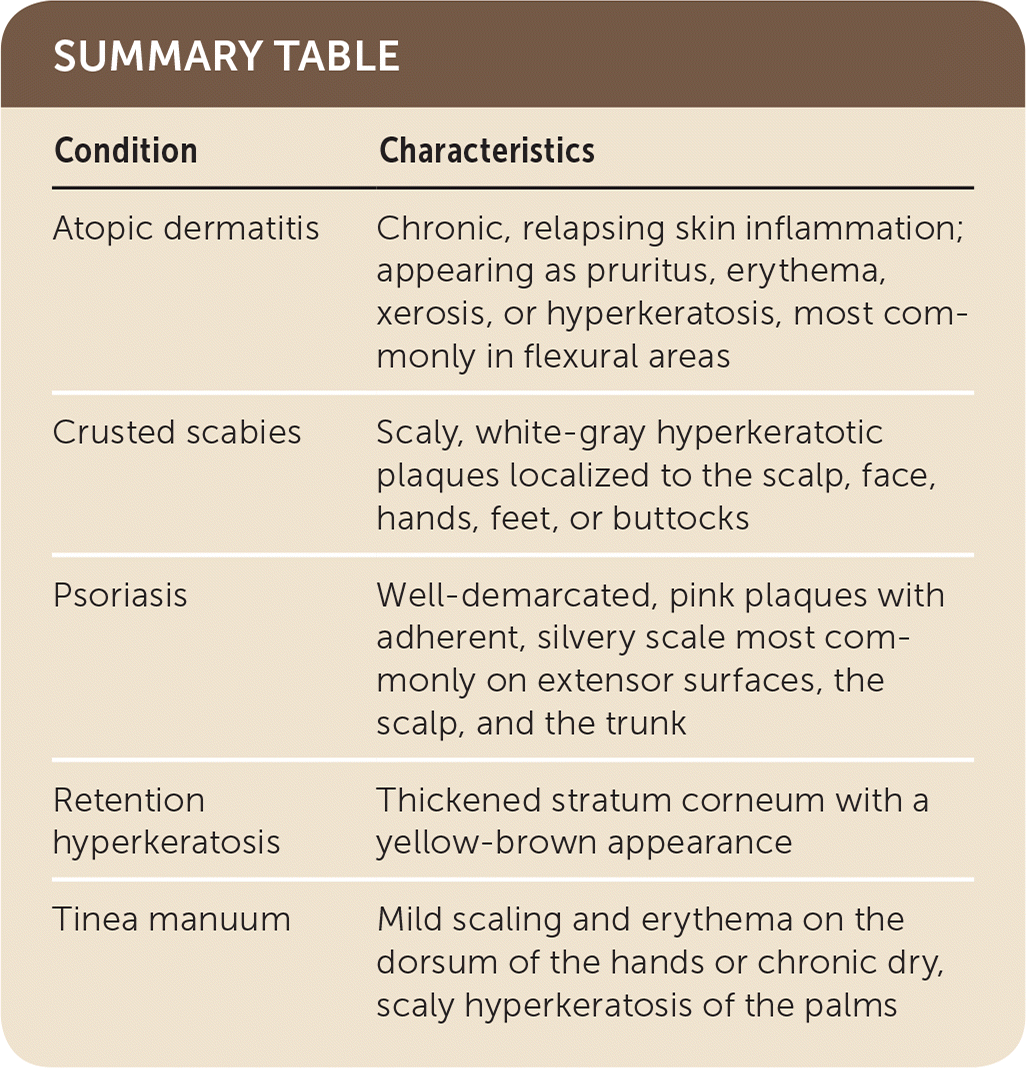
| Condition | Characteristics |
|---|---|
| Atopic dermatitis | Chronic, relapsing skin inflammation; appearing as pruritus, erythema, xerosis, or hyperkeratosis, most commonly in flexural areas |
| Crusted scabies | Scaly, white-gray hyperkeratotic plaques localized to the scalp, face, hands, feet, or buttocks |
| Psoriasis | Well-demarcated, pink plaques with adherent, silvery scale most commonly on extensor surfaces, the scalp, and the trunk |
| Retention hyperkeratosis | Thickened stratum corneum with a yellow-brown appearance |
| Tinea manuum | Mild scaling and erythema on the dorsum of the hands or chronic dry, scaly hyperkeratosis of the palms |

