The U.S. Department of Health and Human Services has identified opioid use disorder as a national crisis,1 and in August 2017 President Trump declared it a national emergency.2 Drug overdose is the leading cause of accidental injury among U.S. adults, and rates of opioid-related overdoses increased 200% between 2000 and 2014.3 Estimates suggest that drug overdose has emerged as the leading cause of death for Americans younger than 50 years.4
A previous editorial in American Family Physician outlined several important roles for family physicians in combatting the opioid epidemic, with a focus on responsible opioid prescribing and a call for physicians to consider training to prescribe buprenorphine, a medication that can be used in conjunction with behavior therapy to treat opioid use disorder in primary care settings.5 Compared with nonpharmacologic treatment of opioid use disorder, medication-assisted treatment (MAT) with buprenorphine is more effective in reducing opioid use, retaining patients in treatment, and reducing the risk of overdose death.6,7 However, access to buprenorphine-based MAT remains limited.8 Of the estimated 2.5 million adolescents and adults with opioid use disorder in 2012, only 1 million received medication.9 Many physicians who complete the required eight-hour training to prescribe buprenorphine do not go on to prescribe. Reported barriers include insufficient nursing/office support, lack of institutional support, inadequately trained staff, insufficient time, inadequate office space, cumbersome regulations, and lack of knowledge.10,11 Table 1 lists online resources for physicians who are interested in caring for patients with opioid use disorder.
TABLE 1. Resources for Physicians Caring for Patients with Opioid Use Disorder

| Agency for Healthcare Research and Quality (https://integrationacademy.ahrq.gov/implementing-medication-assisted-treatment-opioid-use-disorder-rural-primary-care-environmental-scan?utm_source=ahrqamp;&utm_medium=dpilsamp;&utm_term=amp;&utm_content=1amp;&utm_campaign=ahrq_opud_2017) Provides resources to help physicians overcome obstacles in treating opioid use disorder in rural primary care settings |
| American Society of Addiction Medicine (http://www.asam.org/quality-practice/definition-of-addiction and http://www.asam.org/quality-practice/practice-resources) Provides information on addiction, practice resources for buprenorphine prescribers, and online and live CME (some free) |
| Bup Practice (https://www.buppractice.com) Offers training for DATA waivers for physicians and nurse practitioners/physician assistants |
| California Society of Addiction Medicine (http://cme.csam-asam.org) Hosts live and recorded webinars that offer CME (some free) |
| Provider's Clinical Support System for Opioid Therapies (http://pcssmat.org/education-training) Offers free training for buprenorphine DATA waiver and hosts live (free) webinars that offer CME on addiction treatment and pain management |
CME = continuing medical education; DATA = Drug Abuse Treatment Act.
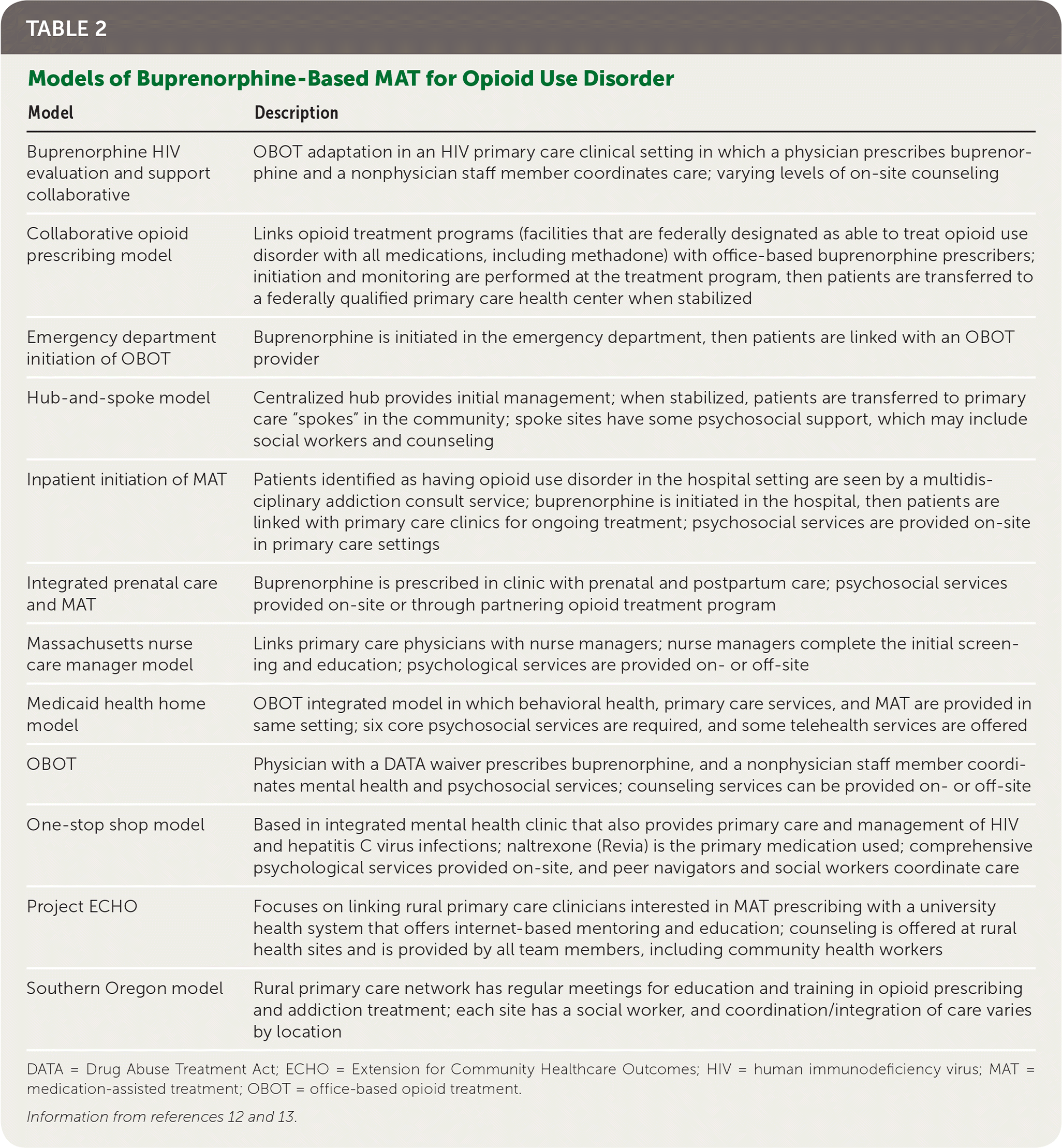
The Agency for Healthcare Research and Quality (AHRQ) recently reviewed 12 models of MAT delivery in primary care settings, ranging from office-based teams (e.g., a physician working closely with a “glue person” to help with coordination of services while psychosocial services are provided off-site) to much larger systems of care involving links between subspecialty centers and primary care offices (Table 2).12,13
TABLE 2. Models of Buprenorphine-Based MAT for Opioid Use Disorder
| Model | Description |
|---|---|
| Buprenorphine HIV evaluation and support collaborative | OBOT adaptation in an HIV primary care clinical setting in which a physician prescribes buprenorphine and a nonphysician staff member coordinates care; varying levels of on-site counseling |
| Collaborative opioid prescribing model | Links opioid treatment programs (facilities that are federally designated as able to treat opioid use disorder with all medications, including methadone) with office-based buprenorphine prescribers; initiation and monitoring are performed at the treatment program, then patients are transferred to a federally qualified primary care health center when stabilized |
| Emergency department initiation of OBOT | Buprenorphine is initiated in the emergency department, then patients are linked with an OBOT provider |
| Hub-and-spoke model | Centralized hub provides initial management; when stabilized, patients are transferred to primary care “spokes” in the community; spoke sites have some psychosocial support, which may include social workers and counseling |
| Inpatient initiation of MAT | Patients identified as having opioid use disorder in the hospital setting are seen by a multidisciplinary addiction consult service; buprenorphine is initiated in the hospital, then patients are linked with primary care clinics for ongoing treatment; psychosocial services are provided on-site in primary care settings |
| Integrated prenatal care and MAT | Buprenorphine is prescribed in clinic with prenatal and postpartum care; psychosocial services provided on-site or through partnering opioid treatment program |
| Massachusetts nurse care manager model | Links primary care physicians with nurse managers; nurse managers complete the initial screening and education; psychological services are provided on- or off-site |
| Medicaid health home model | OBOT integrated model in which behavioral health, primary care services, and MAT are provided in same setting; six core psychosocial services are required, and some telehealth services are offered |
| OBOT | Physician with a DATA waiver prescribes buprenorphine, and a nonphysician staff member coordinates mental health and psychosocial services; counseling services can be provided on- or off-site |
| One-stop shop model | Based in integrated mental health clinic that also provides primary care and management of HIV and hepatitis C virus infections; naltrexone (Revia) is the primary medication used; comprehensive psychological services provided on-site, and peer navigators and social workers coordinate care |
| Project ECHO | Focuses on linking rural primary care clinicians interested in MAT prescribing with a university health system that offers internet-based mentoring and education; counseling is offered at rural health sites and is provided by all team members, including community health workers |
| Southern Oregon model | Rural primary care network has regular meetings for education and training in opioid prescribing and addiction treatment; each site has a social worker, and coordination/integration of care varies by location |
DATA = Drug Abuse Treatment Act; ECHO = Extension for Community Healthcare Outcomes; HIV = human immunodeficiency virus; MAT = medication-assisted treatment; OBOT = office-based opioid treatment.
Most communities are not currently able to meet the demand for treatment of opioid use disorder,8 and family physicians can help fill this gap. The AHRQ review showed that there are different ways in which buprenorphine-based MAT can be safely and effectively delivered in primary care settings. Physicians who do not have on-site behavioral health support often report that they cannot prescribe buprenorphine, but the AHRQ review showed that there are several ways in which psychosocial support and counseling can be provided in office-based settings. For example, one study described a model in which primary care nurses were trained to offer a brief 20-minute weekly counseling session or a more extensive 45-minute weekly drug counseling session.14 Both models had significant reductions in opioid use with no difference in opioid abstinence or retention rates, highlighting the fact that nurses can provide effective counseling in a relatively short session.
Family physicians work in a variety of settings with different levels of staffing, and in communities with varying levels of potential external partners. This review shows that there are models that can fit almost any practice environment, and that there are many potential opportunities for collaboration with external partners.
Editor's Note: The AAFP's position paper, “Chronic Pain Management and Opioid Misuse: A Public Health Concern” (https://www.aafp.org/about/policies/all/pain-management-opioid.html), serves as a call to action for family physicians, with recommendations and resources for treating pain and managing medication misuse/abuse, including medication-assisted treatment. The AAFP also has a Chronic Pain Management Tooklit (https://www.aafp.org/patient-care/public-health/pain-opioids/cpm-toolkit.html).

