Osteoarthritis (OA) should be suspected in patients with pain in the fingers, shoulders, hips, knees, or ankles, especially if they are older than 40 years. Patients older than 50 years who have joint pain, minimal morning stiffness, and functional impairment likely have OA. Radiography can confirm the diagnosis and may be helpful before surgical referral, but findings generally do not correlate well with symptoms. Exercise, physical therapy, knee taping, and tai chi are beneficial for knee OA. Medical therapy provides modest benefits in pain reduction and functional improvement; however, nonsteroidal anti-inflammatory drugs, tramadol, and other opioids have significant potential harms. Joint replacement may be considered for patients with moderate to severe pain and radiographically confirmed OA. Corticosteroid injections may be helpful in the short term. Vitamin D supplements, shoes specifically designed for persons with OA, antioxidant supplements, physical therapy for hip OA, ionized wrist bracelets, lateral wedge insoles for medial knee OA, and hyaluronic acid injections are not effective.
Osteoarthritis (OA) is a condition commonly encountered in primary care. This article provides a brief summary and review of the best available patient-oriented evidence for OA.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
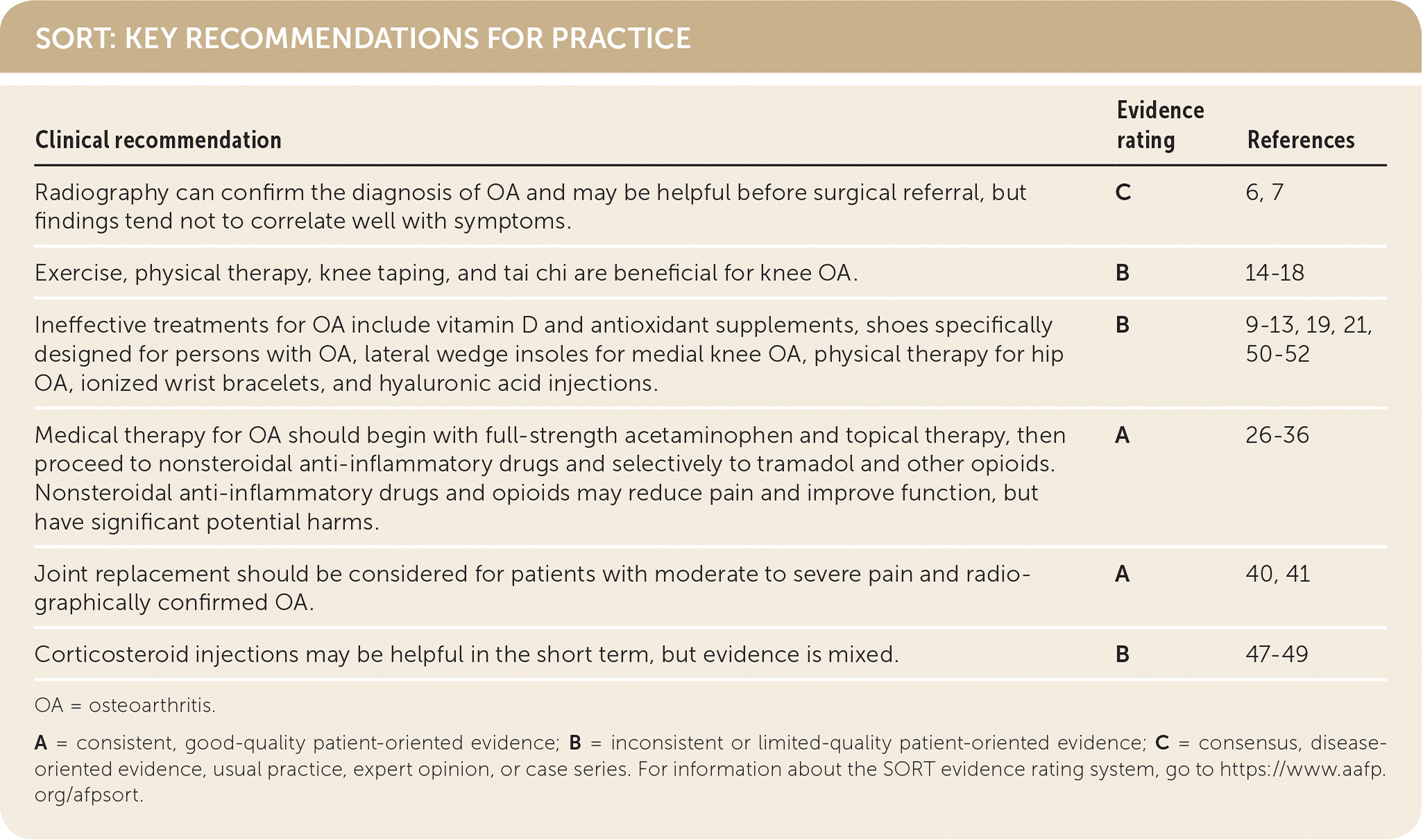
OA = osteoarthritis.
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN ORTHOPEDICS

| Recommendation | Sponsoring organization |
|---|---|
| Do not use glucosamine and chondroitin to treat patients with symptomatic osteoarthritis of the knee. | American Academy of Orthopaedic Surgeons |
| Do not use lateral wedge insoles to treat patients with symptomatic medial compartment osteoarthritis of the knee. | American Academy of Orthopaedic Surgeons |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
Epidemiology
- Older age (especially older than 50 years)
- Female sex
- Overweight or obesity
- Previous joint injury
- Job that requires bending or squatting
- Family history
- Participation in sports associated with repetitive impact (e.g., soccer, American football).2
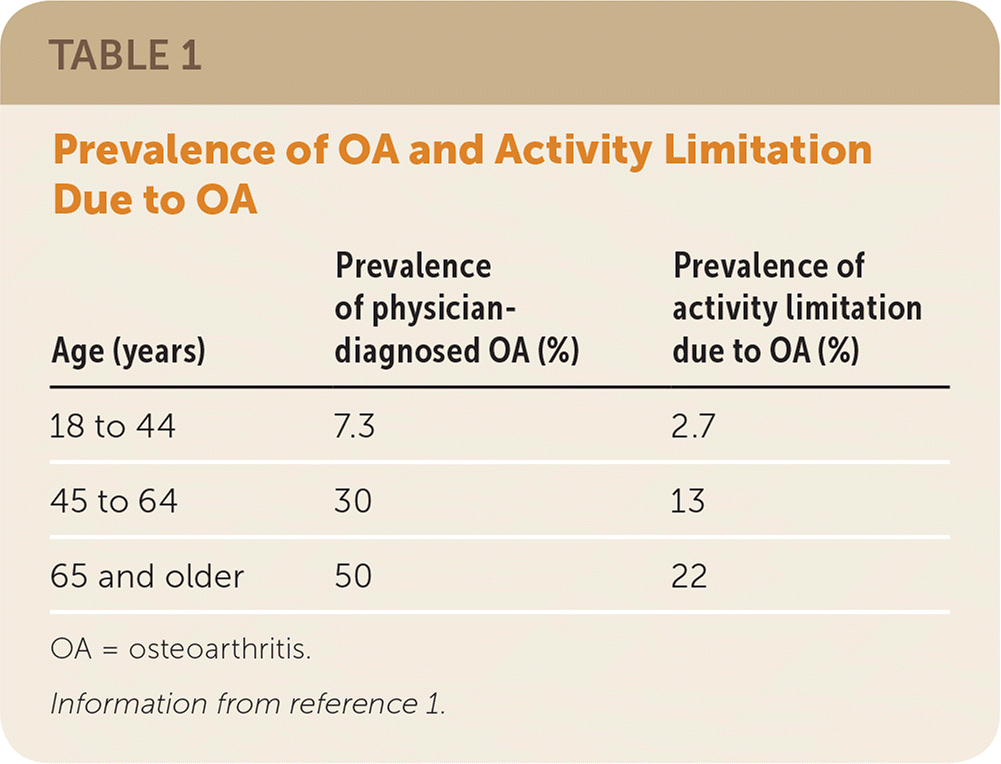
TABLE 1. Prevalence of OA and Activity Limitation Due to OA
| Age (years) | Prevalence of physician-diagnosed OA (%) | Prevalence of activity limitation due to OA (%) |
|---|---|---|
| 18 to 44 | 7.3 | 2.7 |
| 45 to 64 | 30 | 13 |
| 65 and older | 50 | 22 |
OA = osteoarthritis.
Information from reference 1.
Diagnosis
- OA should be suspected in patients with pain in the fingers, shoulders, hips, knees, or ankles, especially if they are older than 40 years.2,3
- Alternative diagnoses should be considered in patients with inflammation, erythema, or pain that increases or changes significantly.
- The differential diagnosis includes collagen vascular disease, gout and pseudogout, trauma, septic arthritis, ankylosing spondylitis, and psoriatic arthritis.
SIGNS AND SYMPTOMS
Signs and symptoms that are common in OA include:
- Pain that is typically worse later in the day and relieved by rest.
- Joint swelling and tenderness, with or without crepitus.
- Bony enlargement in prolonged or severe OA.
- Joint pain, minimal morning stiffness, and functional impairment in patients older than 50 years.2,3 The presence of these findings is moderately helpful in ruling in OA, but their absence does not rule it out3 (Table 24 ).
- Older age, obesity, difficulty walking down stairs, and clinical findings of decreased range of motion, effusion, and crepitus in patients with knee pain.5
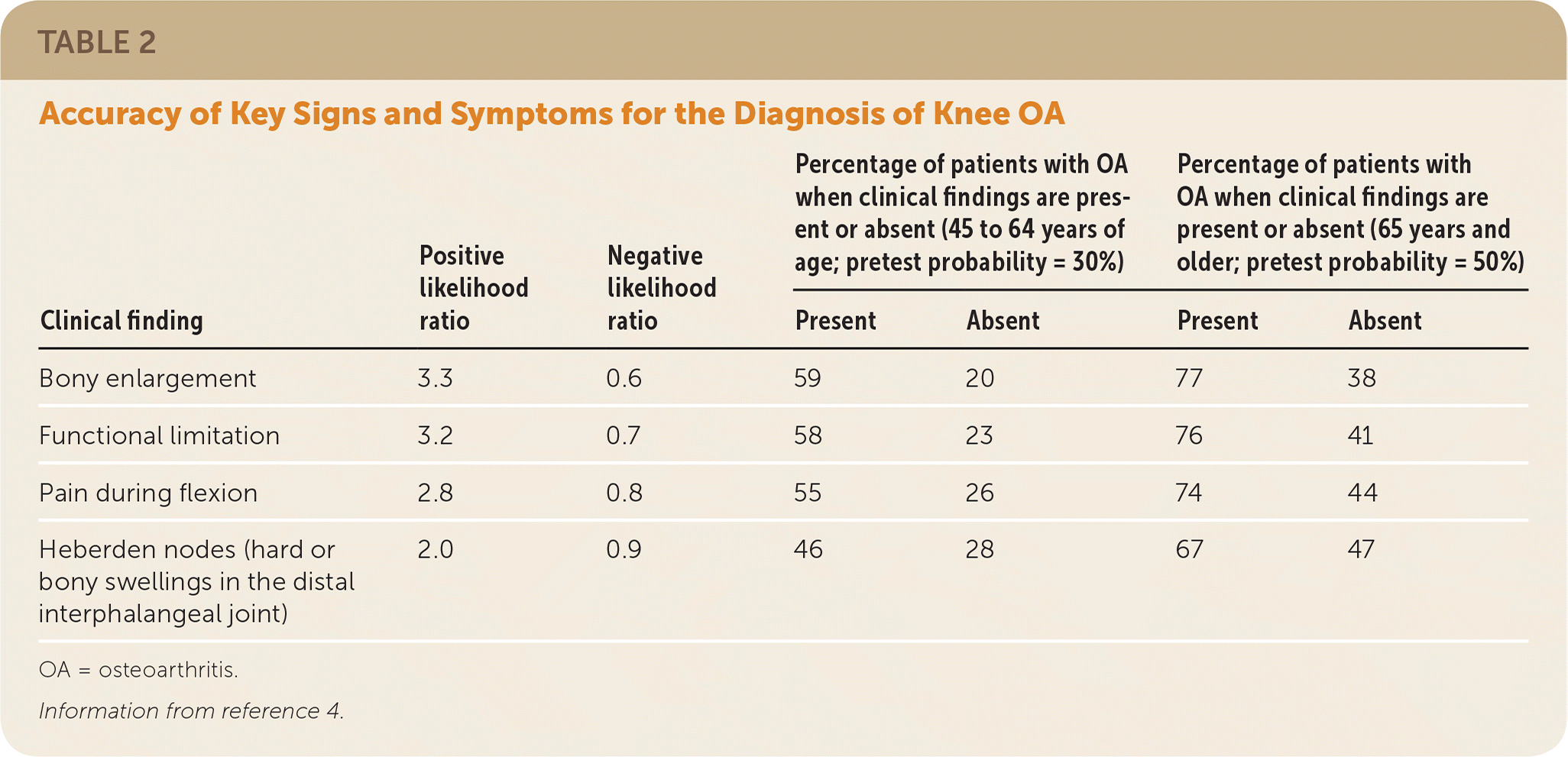
TABLE 2. Accuracy of Key Signs and Symptoms for the Diagnosis of Knee OA
| Clinical finding | Positive likelihood ratio | Negative likelihood ratio | Percentage of patients with OA when clinical findings are present or absent (45 to 64 years of age; pretest probability = 30%) | Percentage of patients with OA when clinical findings are present or absent (65 years and older; pretest probability = 50%) | ||
|---|---|---|---|---|---|---|
| Present | Absent | Present | Absent | |||
| Bony enlargement | 3.3 | 0.6 | 59 | 20 | 77 | 38 |
| Functional limitation | 3.2 | 0.7 | 58 | 23 | 76 | 41 |
| Pain during flexion | 2.8 | 0.8 | 55 | 26 | 74 | 44 |
| Heberden nodes (hard or bony swellings in the distal interphalangeal joint) | 2.0 | 0.9 | 46 | 28 | 67 | 47 |
OA = osteoarthritis.
Information from reference 4.
DIAGNOSTIC TESTING
- Radiography is not required to diagnose OA in patients with risk factors and typical symptoms.3
- Radiographic findings in patients with OA do not always correlate well with symptoms. Two studies found that only 16% of patients with frequent hip pain had radiographic evidence of OA; conversely, only 21% of patients who met the radiographic criteria for hip OA had frequent pain.6
- Typical radiographic findings in patients with OA include joint space narrowing, osteophytes, and subchondral sclerosis.
- Radiography can be helpful before referral for joint replacement, as radiographic severity is an important factor in determining whether surgery is appropriate.
- Magnetic resonance imaging detects joint abnormalities in about 90% of both obese and nonobese adults older than 50 years who do not have joint pain.7
Treatment
Figure 1 presents a suggested approach to the treatment of OA. Several therapies are supported by good-quality evidence. However, some widely used treatments (e.g., hyaluronic acid injections, arthroscopic surgery) are not effective and should be abandoned.
FIGURE 1.
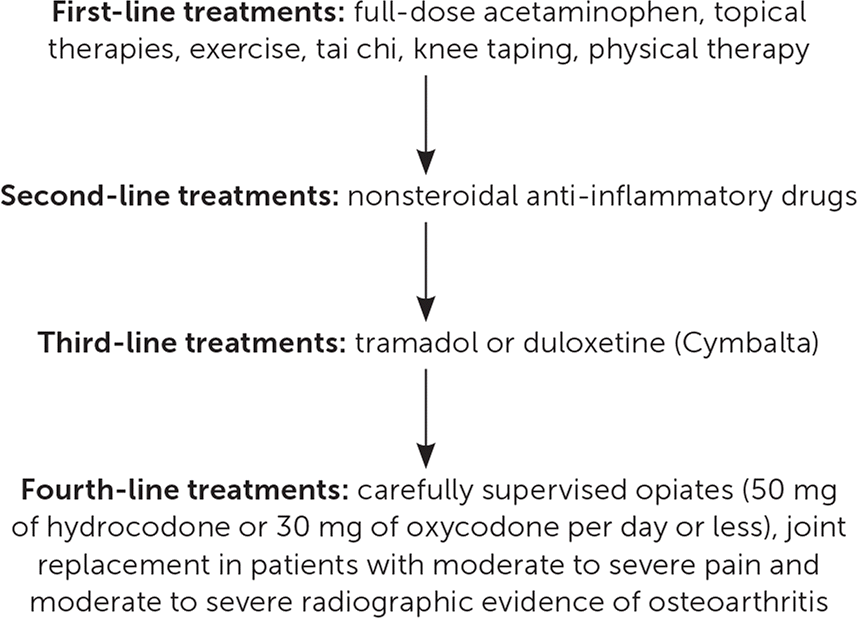
Suggested treatment approach to the patient with osteoarthritis.
EXERCISE, DIET, AND PHYSICAL THERAPY
- Aquatic exercise has small short-term benefits for OA.8
- Vitamin D supplements, antioxidant supplements, shoes specifically designed for persons with OA, and ionized wrist bracelets are ineffective for OA.9–13
- Exercise, tai chi, knee taping, and physical therapy are beneficial for knee OA and can be recommended based on patient preference and acceptability.14–18
- Lateral wedge insoles are ineffective for medial knee OA.19
- Knee bracing has insufficient evidence to draw conclusions about its effectiveness.20
- Physical therapy was not beneficial for hip OA in a well-designed trial.21
- Weight loss has been recommended for patients with knee and hip OA22; however, a systematic review found only low-quality evidence that bariatric surgery reduces pain and improves function in morbidly obese persons with knee pain.23
- Ginger consumption significantly reduced pain and disability in five studies (N = 593) included in a systematic review.24 However, patients were more likely to stop taking it, and the overall quality of studies was moderate. Similarly, avocado unsaponifiables may be effective at dosages of 300 to 600 mg per day. Both of these interventions, although likely safe, are limited by the small number and methodologic flaws of studies.25
MEDICAL THERAPY
- Acetaminophen is less effective than nonsteroidal anti-inflammatory drugs (NSAIDs) for OA, but given its safety, a trial at an adequate dosage is appropriate.26,27
- Of the NSAIDs currently available in the United States, diclofenac, 150 mg per day, is most likely to be effective for OA, followed by naproxen, according to a systematic review.26 A Cochrane review concluded that topical diclofenac and ketoprofen are moderately effective.28
- Topical capsaicin appeared to be somewhat effective in several small trials, although it is associated with a transient burning sensation.29–32
- Tramadol is moderately effective for OA, according to a systematic review of 11 randomized trials (N = 1,019), and has a number needed to treat (NNT) of 6 for one person to report at least moderate improvement.33 Conversely, the number needed to harm (NNH) for one person to stop taking tramadol because of adverse effects is 8.
- Duloxetine (Cymbalta) is a serotonin–norepinephrine reuptake inhibitor approved for treatment of painful conditions. Its NNT is 7 for clinically significant pain reduction in OA.34,35 The most common adverse effect is mild to moderate nausea (23% vs. 7% for placebo; NNH = 6).36
- Because tramadol and duloxetine have harms and adverse effects similar in magnitude to their potential benefits, they should be used only in select patients.
- Propoxyphene (not available in the United States) plus acetaminophen is no better than acetaminophen alone, has more adverse effects, and should be avoided.37
- Oral and transdermal opioids (not including tramadol) have only modest benefits that are of questionable clinical significance, according to a Cochrane review.38 These medications also have significant adverse effects, and long-term use is discouraged. Patients taking opioids should be closely monitored, and the dose should be kept as low as possible. Daily dosages of more than 50 mg of hydrocodone or 30 mg of oxycodone are discouraged.39
- In general, it is reasonable to begin treatment with full-dose acetaminophen and/or topical therapy and progress to an NSAID such as naproxen or diclofenac, then, if necessary, to tramadol or duloxetine.
SURGICAL THERAPY
- Joint replacement is an option for patients with moderate to severe pain and radiographically confirmed OA.40 A randomized trial found that patients with moderate radiographically confirmed knee OA had significantly improved pain and function after joint replacement compared with those receiving usual care, although serious adverse effects can occur, including deep venous thrombosis, infection, and the need for further surgery or mobilization under anesthesia.41 Obese and nonobese patients have similar outcomes after knee replacement.42–44
- Arthroscopic meniscectomy with or without debridement is no more effective than sham procedures or exercise for knee OA, according to a systematic review of nine studies (N = 1,279).45 It is also ineffective for patients with degenerative meniscal tears.46
- Corticosteroid injections improve function and provide short-term pain relief, but do not improve overall quality of life, according to systematic reviews.47,48 A recent large randomized trial found no benefit and greater cartilage loss in patients receiving corticosteroid injections.49
- Hyaluronic acid injections are not effective for OA, according to a review of the highest-quality studies and unpublished research.50–52
- Dextrose prolotherapy injections showed a modest benefit for knee OA in two small randomized trials, but the evidence base is limited, and the technique may be operator-dependent and not easily reproduced.53,54
- Platelet-rich plasma or bone marrow aspirate concentrate injections are not effective for OA.55,56
COMPLEMENTARY THERAPY
The following complementary therapies have been studied for the treatment of OA:
- Acupuncture is at best minimally effective for OA of the knee or hip.57–59
- Oral glucosamine with or without chondroitin does not appear to be effective in well-designed trials.60–62
- S-adenylmethionine and methylsulfonylmethane have uncertain effectiveness based on systematic reviews.63,64 Observed benefits were small in magnitude and probably not clinically significant.
Prognosis
Symptoms of OA tend to progress over time, although they may temporarily improve in the short term.
Editor's Note: Rapid Evidence Review is a new article format that was created with the goal of providing key clinical information that can be read quickly and that answers questions at the point of care. These articles are unique in that the references are only available online and the SORT table recommendations are linked to the corresponding areas of the text in the online version of the article. Please let us know what you think of the new format by commenting online or e-mailing us at afpedit@aafp.org.
Data Sources: This article was based on literature cited in Essential Evidence Plus, the Cochrane database, recently published InfoPOEMs, and a PubMed search using the Clinical Queries database for the term osteoarthritis. Search date: July 2017.

