Diet is the single most significant risk factor for disability and premature death. Patients and physicians often have difficulty staying abreast of diet trends, many of which focus primarily on weight loss rather than nutrition and health. Recommending an eating style can help patients make positive change. Dietary patterns that support health include the Mediterranean diet, the Dietary Approaches to Stop Hypertension diet, the 2015 Dietary Guidelines for Americans, and the Healthy Eating Plate. These approaches have benefits that include prevention of cardiovascular disease, cancer, type 2 diabetes mellitus, and obesity. These dietary patterns are supported by strong evidence that promotes a primary focus on unprocessed foods, fruits and vegetables, plant-based fats and proteins, legumes, whole grains, and nuts. Added sugars should be limited to less than 5% to 10% of daily caloric intake. Vegetables (not including potatoes) and fruits should make up one-half of each meal. Carbohydrate sources should primarily include beans/legumes, whole grains, fruits, and vegetables. An emphasis on monounsaturated fats, such as olive oil, avocados, and nuts, and omega-3 fatty acids, such as flax, cold-water fish, and nuts, helps prevent cardiovascular disease, type 2 diabetes, and cognitive decline. A focus on foods rather than macronutrients can assist patients in understanding a healthy diet. Addressing barriers to following a healthy diet and utilizing the entire health care team can assist patients in following these guidelines.
Although diet is the single most significant risk factor for disability and premature death,1 most Americans do not adhere to U.S. dietary recommendations,2 and nutrition is minimally addressed in health care.1 When nutrition is discussed with patients, much of what is presented is inconsistent with existing evidence.3 Patients and clinicians are often overwhelmed with information on diet and the nutritional value of foods. Although weight loss is a common focus, no diet has been proven superior to others. However, when health is considered, specific dietary patterns—including particular macronutrients and foods—have good evidence for primary and secondary prevention of several chronic diseases. Patients are more likely to understand information about foods rather than nutrients, so focusing on food categories may be useful. Diets for the treatment of specific medical conditions are beyond the scope of this article.
WHAT IS NEW ON THIS TOPIC: DIETS FOR HEALTH
Large, prospective cohort studies show that vegetarian diets reduce the risk of coronary heart disease and type 2 diabetes mellitus, and that vegan diets offer additional benefits for obesity, hypertension, type 2 diabetes, and cardiovascular mortality.
Eating nuts, including peanuts, is associated with decreased cardiovascular disease and mortality, lower body weight, and lower diabetes risk.
In a prospective cohort study, consumption of artificially sweetened beverages increased the risk of type 2 diabetes about one-half as much as sugar-sweetened beverages.
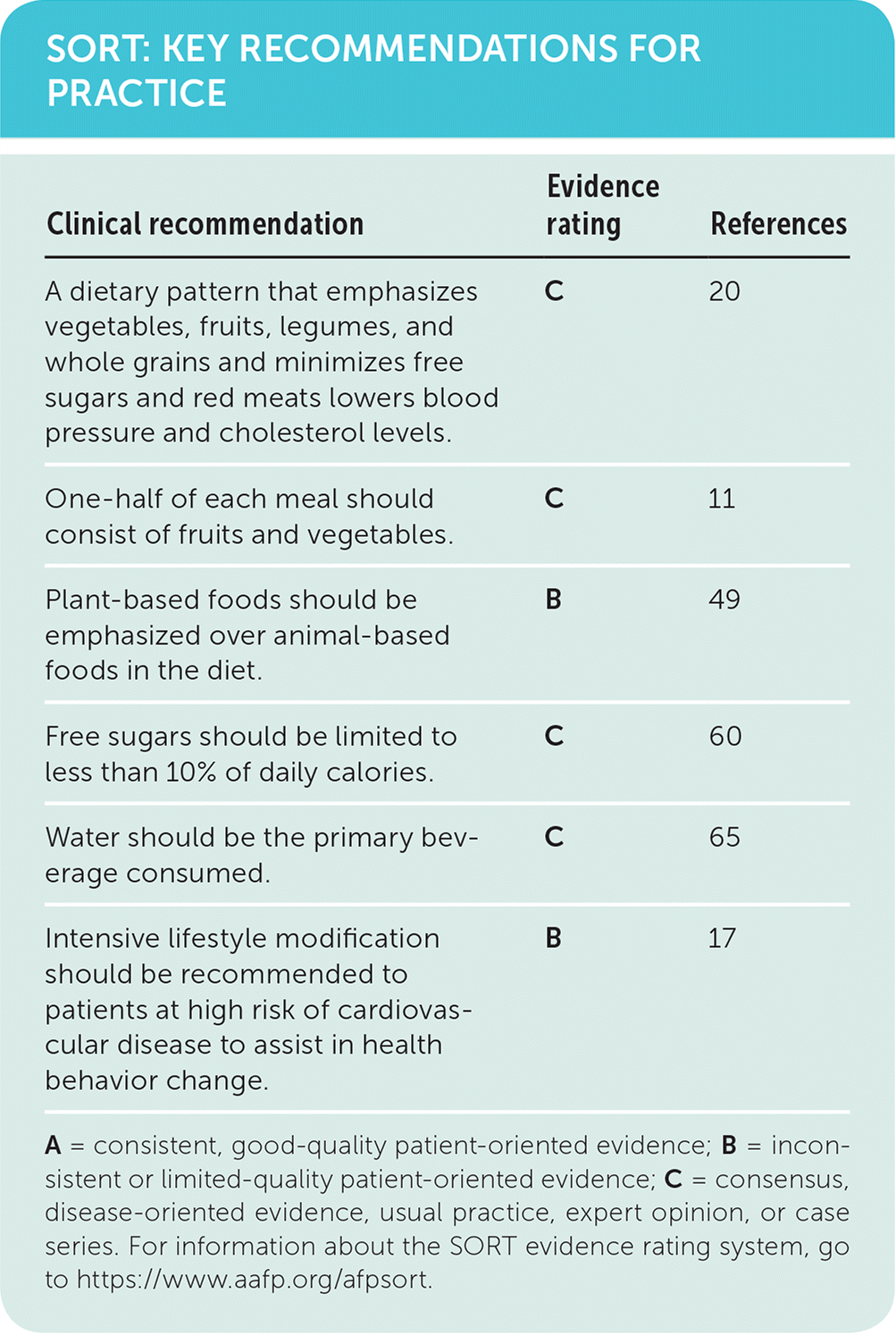
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| A dietary pattern that emphasizes vegetables, fruits, legumes, and whole grains and minimizes free sugars and red meats lowers blood pressure and cholesterol levels. | C | 20 |
| One-half of each meal should consist of fruits and vegetables. | C | 11 |
| Plant-based foods should be emphasized over animal-based foods in the diet. | B | 49 |
| Free sugars should be limited to less than 10% of daily calories. | C | 60 |
| Water should be the primary beverage consumed. | C | 65 |
| Intensive lifestyle modification should be recommended to patients at high risk of cardiovascular disease to assist in health behavior change. | B | 17 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Dietary Patterns
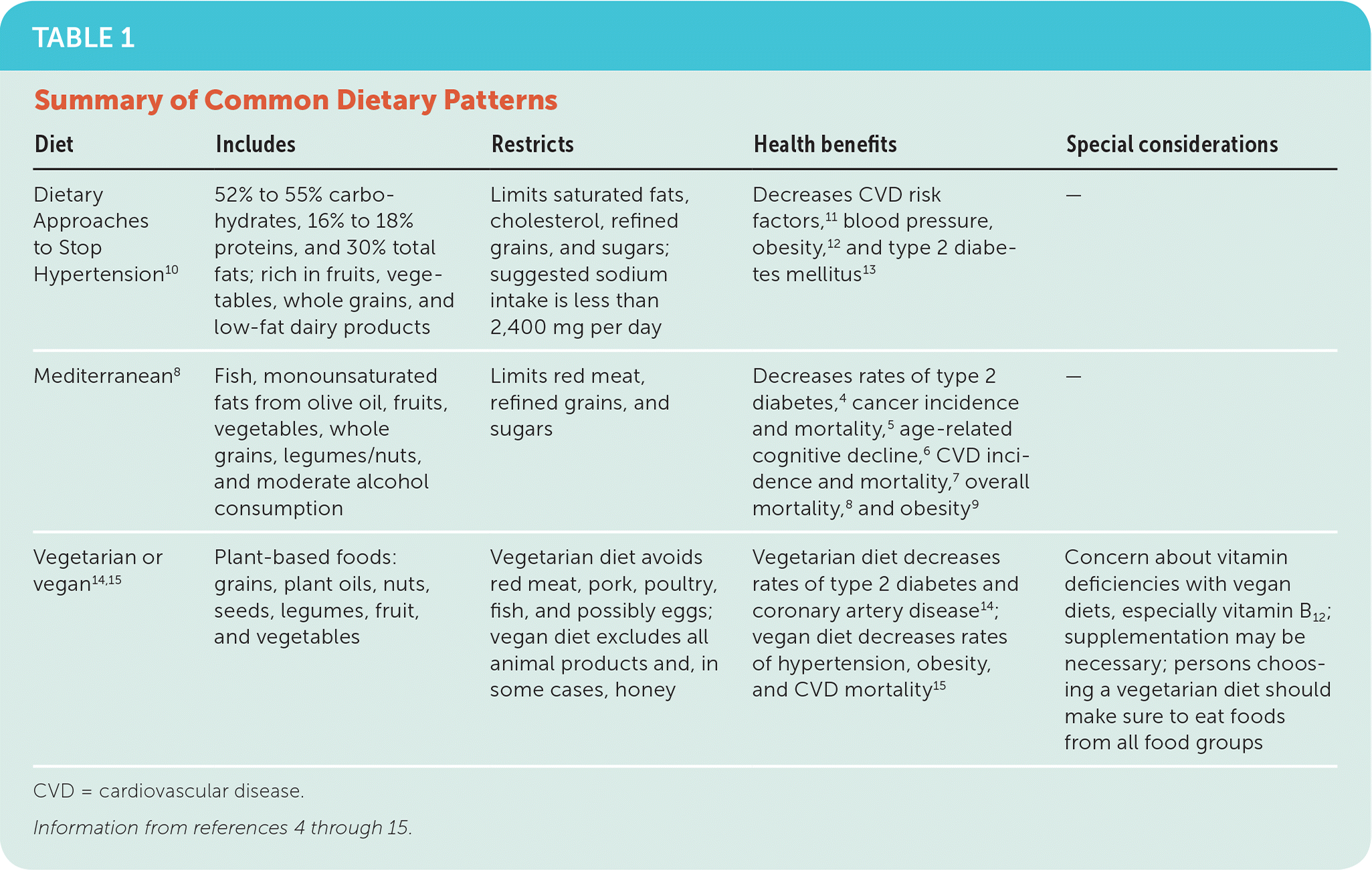
Recommending an eating style can be one way to support healthy dietary changes. The list of popular diets is lengthy, and most have not been carefully evaluated. The Mediterranean diet has moderate to strong evidence for preventing type 2 diabetes mellitus,4 decreasing cancer incidence and mortality,5 preventing age-related cognitive decline,6 preventing cardiovascular disease (CVD) incidence and mortality,7 decreasing overall mortality,8 and treating obesity9 (Table 14–15 ).
TABLE 1. Summary of Common Dietary Patterns
| Diet | Includes | Restricts | Health benefits | Special considerations |
|---|---|---|---|---|
| Dietary Approaches to Stop Hypertension10 | 52% to 55% carbohydrates, 16% to 18% proteins, and 30% total fats; rich in fruits, vegetables, whole grains, and low-fat dairy products | Limits saturated fats, cholesterol, refined grains, and sugars; suggested sodium intake is less than 2,400 mg per day | Decreases CVD risk factors,11 blood pressure, obesity,12 and type 2 diabetes mellitus13 | — |
| Mediterranean8 | Fish, monounsaturated fats from olive oil, fruits, vegetables, whole grains, legumes/nuts, and moderate alcohol consumption | Limits red meat, refined grains, and sugars | Decreases rates of type 2 diabetes,4 cancer incidence and mortality,5 age-related cognitive decline,6 CVD incidence and mortality,7 overall mortality,8 and obesity9 | — |
| Vegetarian or vegan14,15 | Plant-based foods: grains, plant oils, nuts, seeds, legumes, fruit, and vegetables | Vegetarian diet avoids red meat, pork, poultry, fish, and possibly eggs; vegan diet excludes all animal products and, in some cases, honey | Vegetarian diet decreases rates of type 2 diabetes and coronary artery disease14; vegan diet decreases rates of hypertension, obesity, and CVD mortality15 | Concern about vitamin deficiencies with vegan diets, especially vitamin B12; supplementation may be necessary; persons choosing a vegetarian diet should make sure to eat foods from all food groups |
CVD = cardiovascular disease.
The Dietary Approaches to Stop Hypertension (DASH) diet is promoted by the National Institutes of Health to treat hypertension. It has strong evidence for improving risk factors for CVD and lowering blood pressure,11 and more limited evidence for weight loss12 and managing or preventing type 2 diabetes.13
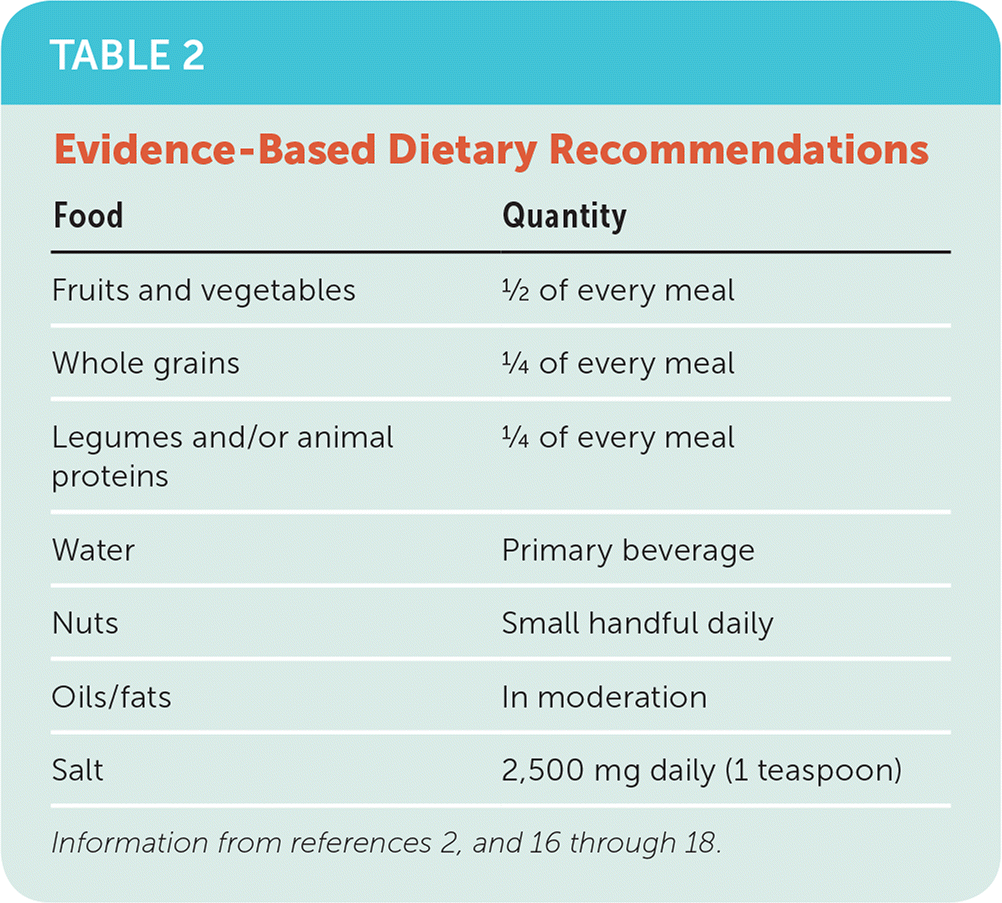
The 2015 Dietary Guidelines for Americans is another healthy eating pattern.16 Choose My Plate (U.S. Department of Agriculture [USDA]) and the Healthy Eating Plate (Harvard University) provide useful tools for achieving these dietary guidelines (Table 22,16–18 ). The Healthy Eating Plate is consistent with the Mediterranean diet and emphasizes covering one-half of the plate with fruits and vegetables, one-fourth with whole grains, and the remaining one-fourth with healthy protein; consuming water as the primary beverage; and engaging in regular physical activity. Plant oils and proteins are highlighted. The Healthy Eating Plate recommendations are closely aligned with the suggestions in this article and offer another tool to help patients achieve comprehensive changes to their diets. All of these diets limit added sugars, sweetened beverages, and highly refined grains.
TABLE 2. Evidence-Based Dietary Recommendations
Large, prospective cohort studies show that primarily vegetarian diets reduce the risk of coronary artery disease (CAD) and type 2 diabetes, and that vegan diets benefit patients with obesity, hypertension, type 2 diabetes, or other CVD risk factors.14,15 Each of the dietary patterns discussed in this article is consistent with dietary advice recommended by the American Academy of Family Physicians.19,20
FRUITS AND VEGETABLES
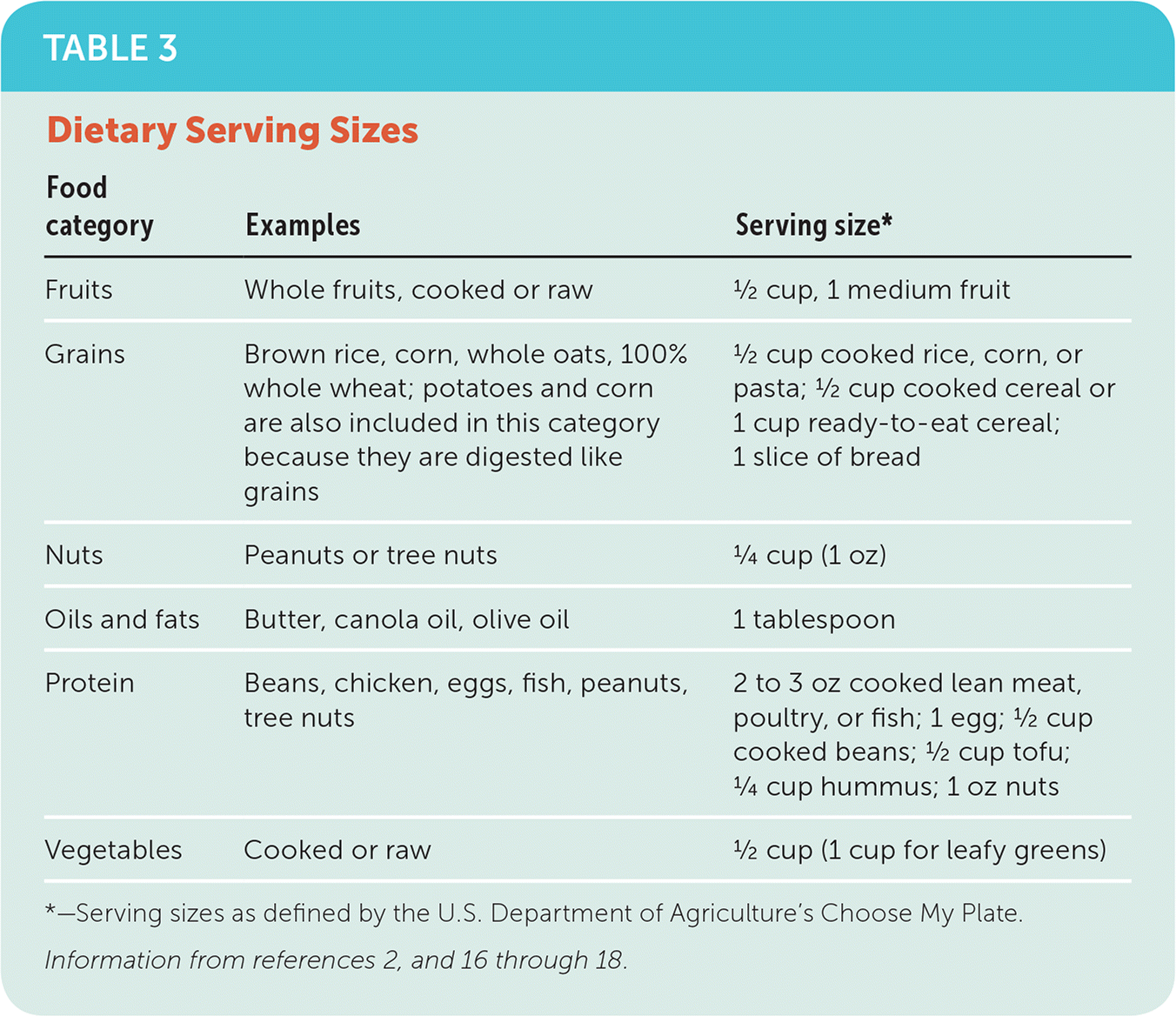
Most dietary guidelines recommend that one-half of each meal consist of vegetables and fruits.11,16 Whole fruits and vegetables are preferred over juices because of their higher fiber content and lower glycemic index (a measure of how quickly a food is digested). Potatoes are not included in this recommendation because they are more nutritionally similar to grains. Observational studies have examined the relationship between disease and intake of fruits and vegetables. Higher intake has been associated with reductions in CAD,21 cerebrovascular disease,22 cancer,23 and gastrointestinal conditions.24 Participants in the Nurses' Health Study and the Health Professionals Follow-Up Study who had the highest intake of fruits and vegetables (more than five servings per day) had a 30% decrease in the risk of CVD compared with those who ate 1.5 servings or less per day.25 Green leafy vegetables seem to have the most benefits. Nine daily servings of vegetables and fruits—in a variety of colors to maximize intake of various phytochemicals, antioxidants, and vitamins—are recommended (Table 3).2,16–18
TABLE 3. Dietary Serving Sizes
| Food category | Examples | Serving size* |
|---|---|---|
| Fruits | Whole fruits, cooked or raw | ½ cup, 1 medium fruit |
| Grains | Brown rice, corn, whole oats, 100% whole wheat; potatoes and corn are also included in this category because they are digested like grains | ½ cup cooked rice, corn, or pasta; ½ cup cooked cereal or 1 cup ready-to-eat cereal; 1 slice of bread |
| Nuts | Peanuts or tree nuts | ¼ cup (1 oz) |
| Oils and fats | Butter, canola oil, olive oil | 1 tablespoon |
| Protein | Beans, chicken, eggs, fish, peanuts, tree nuts | 2 to 3 oz cooked lean meat, poultry, or fish; 1 egg; ½ cup cooked beans; ½ cup tofu; ¼ cup hummus; 1 oz nuts |
| Vegetables | Cooked or raw | ½ cup (1 cup for leafy greens) |
*—Serving sizes as defined by the U.S. Department of Agriculture's Choose My Plate.
LEGUMES
Legumes include a variety of beans, which are high in soluble fiber, protein, iron, B vitamins, and minerals,26 and have a low glycemic index. Because of their unique nutrients, legumes are considered both a protein and a vegetable, and are important components of healthy eating patterns. Eating legumes four times per week compared with less than once per week is associated with reduced CAD and CVD risk,27 decreased recurrence of colorectal polyps, increased longevity, improved blood glucose control, and better weight management.26,28 USDA dietary guidelines recommend eating 1.5 to 3 cups of beans per week.2
GRAINS
Grains are available as highly refined food products that contribute to poor health (e.g., white bread) or as minimally processed whole grains that contribute to a healthy diet (e.g., brown rice). Patients may have difficulty understanding which grains and grain products are healthy. The glycemic index and glycemic load, which take into account the amount of carbohydrate in a food, can help with this understanding. The way a whole grain is processed determines the glycemic index: finely ground grains will be digested more quickly than less processed grains. Diets high in processed grains are associated with increased inflammation, higher rates of CVD, poorly controlled type 2 diabetes, and difficulty losing weight.29–33 Whole grains have a higher nutritional value with more vitamins, protein, and fiber than processed grains, and are associated with decreased rates of CVD.34 USDA dietary guidelines recommend eating 1.5 to 3 cups of grains per day, with at least 50% of this amount as whole grains.2
FIBER
Dietary fiber is divided into soluble and insoluble fiber; each type has different effects on health (Table 4).35–37 Good sources of fiber include whole grains, fruits, vegetables, and legumes. Patients may rely on grains, nuts, legumes, fruits, and vegetables to increase their intake of soluble and insoluble fiber. Fiber intake is associated with reduced rates of CVD and premature death; lower blood pressure, low-density lipoprotein (LDL) cholesterol levels, and breast cancer risk; and improved insulin sensitivity.35–38 USDA dietary guidelines recommend consuming a minimum of 14 g of fiber per 1,000 calories per day.2
TABLE 4. Health Benefits of Insoluble vs. Soluble Fiber

| Fiber type | Foods | Health benefits |
|---|---|---|
| Insoluble (does not dissolve in water) | Carrots, cucumbers, seeds, tomatoes, whole grains, and zucchini | Improved insulin sensitivity,35 prevention of cardiovascular disease,36 and reduced cancer incidence37 |
| Soluble (dissolves in water) | Apples, beans, blueberries, lentils, and oatmeal | Improvement in symptoms of irritable bowel syndrome, improved insulin sensitivity,35 prevention of cardiovascular disease,36 and reduced cancer incidence37 |
OILS, FATS, AND NUTS
Dietary fat is divided into three categories: saturated, polyunsaturated, and monounsaturated. All are essential nutrients, and every fat-containing food has a combination of each type. Trans fats are dangerous and have been banned. Efforts to reduce fat consumption over the past 40 years led to increased intake of refined carbohydrates in place of fat and overall increased caloric intake, which increased triglyceride levels and the risk of type 2 diabetes and contributed to weight gain, increased LDL cholesterol levels, and decreased high-density lipoprotein cholesterol levels, but did not affect rates of CAD.39,40
Dietary fats affect serum cholesterol levels and CAD risk differently. Compared with saturated fats, increasing mono- or polyunsaturated fats decreases the risk of CAD,39 although saturated fats found in plants may have a more beneficial effect on lipid levels.41,42
Omega-3 and -6 fatty acids are polyunsaturated fats. An unbalanced ratio of these fatty acids favoring omega-6 can lead to increased activation of the arachidonic acid pathway, with resulting increases in rates of thrombosis, vasospasm, cancer, obesity, and allergic and inflammatory disorders.43 Increasing consumption of foods high in omega-3 fatty acids (e.g., fish, nuts, canola oil, green vegetables) while limiting the use of corn and vegetable oils can increase the ratio of omega-3 to omega-6 fatty acids, leading to decreased inflammation and other health benefits.
Monounsaturated fats in olive oil, nuts, and avocados seem to be beneficial for preventing CVD.44 In general, a focus on omega-3 and monounsaturated fats from fish and plants is likely to be most beneficial. Eating nuts, including peanuts, has been associated with health benefits such as decreased risk of diabetes, CVD, and mortality,45 and lower body weight.46 When nuts are eaten as part of a Mediterranean diet, good-quality evidence shows decreased age-related cognitive decline.6
ANIMAL PRODUCTS
There are conflicting health benefits for animal products, with red and processed meats having the most significant negative effects. For instance, there is a dose-response relationship between red meat intake and risk of all-cause mortality.47 Although higher protein and fat content relative to carbohydrate generally decreases CVD risk and improves lipid levels,48 data suggest that this is not the case when the protein comes from animal sources.49 Plant-based proteins are generally preferred as a primary source.49 When animal products are consumed, an emphasis on fish, dairy, eggs, and fowl is recommended.
Eggs are high in cholesterol but do not contain high amounts of saturated fats. Observational data suggest that consumption of up to one egg per day does not contribute to CVD; however, persons with type 2 diabetes may have a slightly increased risk.50 Eggs are also high in vitamins and protein.
Up to 70% of the world's population does not have the gene to produce lactase into adulthood, and therefore cannot fully digest dairy products.51 Dairy products are a significant source of added sugar and saturated fats. Although dairy products supply calcium, fat, protein, and carbohydrate, adequate amounts of each of these components can be obtained from other foods. Neither dairy consumption nor dietary calcium intake is associated with a reduction in hip fracture; in fact, they have been associated with increases in fracture and all-cause mortality.52 Nondairy sources of calcium include greens, nuts, and legumes. For those who can tolerate dairy, it is associated with a decreased risk of type 2 diabetes and metabolic syndrome,53 and compared with nondairy milk consumption, it may be associated with a slight increase in childhood height.54 Consumption of dairy products is not independently associated with weight gain.55
BEVERAGES
Beverages can have a significant impact on dietary quality. Persons who consume the most sugar-sweetened beverages have the highest caloric intake and the poorest quality nutrition. However, those who drink coffee and diet beverages eat more high-calorie, low-nutrient-density foods.56 Free sugars include added sugar and other caloric sweeteners such as honey, fruit juice concentrates, and maple syrup. Sweetened beverages such as soda and energy drinks are being increasingly linked to the development of multiple chronic diseases, and the risks of hypertension, type 2 diabetes, and obesity-related cancers increase with each additional serving.57–59 Fruit juice, which is high in free sugars, is associated with diabetes and should be discouraged.58 The World Health Organization recommends limiting free sugars to less than 5% to 10% of daily caloric intake60; the Dietary Guidelines for Americans recommends less than 10%.16
Artificially sweetened beverages may increase the risk of type 2 diabetes at about one-half the rate of sugar-sweetened beverages.61 However, evidence is emerging that compared with unsweetened beverages, early exposure to artificial sweeteners in utero or during early childhood may increase the risk of obesity in adulthood.62 Replacing sweetened beverages (sugar and artificially sweetened) with unsweetened beverages may reduce the risk of type 2 diabetes, obesity, and high blood pressure.
Unsweetened black and green teas have some evidence of positive effects on LDL cholesterol and blood pressure,63 and coffee and tea have been proven to protect against depression.64
Water may be the most important and beneficial beverage. An analysis of data from the National Health and Nutrition Examination Survey showed that as plain water intake increased, total caloric intake decreased, especially from sugar-sweetened beverages.65 Inadequate hydration (as determined by elevated urine osmolality) is associated with higher body mass index.66
Moderate alcohol consumption (one drink per day for women, two per day for men) has been shown to decrease the risk of CAD.67 However, these results have been questioned by findings indicating that these studies did not carefully parse the amount and duration of alcohol consumption.68 Potential benefits seem to be independent of the type of alcohol. Because of risks associated with heavy use, clinicians should not recommend that patients start drinking alcoholic beverages.
SPICES
In addition to increasing the flavor complexity of foods, many spices are being studied for their potential health benefits. Salt is a common flavoring and has long been associated with an increased risk of CVD via its effect on elevating blood pressure. Approximately 90% of Americans consume more sodium than the 2,500 mg per day recommended by the USDA, the National Academy of Medicine, and the American Heart Association.69 According to a Cochrane review, decreasing salt intake from the current average of 9 to 12 g per day to a more modest 5 to 6 g per day would decrease systolic blood pressure by 5.8 mm Hg, thereby significantly reducing the overall population burden of CVD.70
Addressing Barriers to Behavior Change
There are many barriers to behavior change that can contribute to poor nutrition (Table 5). Addressing these barriers with patients is as essential as providing information about the health benefits of foods (Table 6). Helping patients with behavior change can be enhanced by techniques such as motivational interviewing or positive inquiry, utilizing others on the health care team, and making use of community resources. The U.S. Preventive Services Task Force recommends referral to intensive lifestyle programs to assist with nutrition and physical activity for patients with CVD risk factors17 and considering selective referral for those without risk factors.18
TABLE 5. Barriers to a Healthy Diet
| Barrier | Intervention | Resources |
|---|---|---|
| Cultural barriers | Education | Community resources Information about the U.S. food system (http://www.jhsph.edu/research/centers-and-institutes/johns-hopkins-center-for-a-livable-future/education/opencourseware) |
| Emotional eating | Counseling, education | Referral to psychologist or social services |
| Financial barriers | Education, food assistance | Education on cost of fresh vs. processed foods USDA Food Environment Atlas (https://www.ers.usda.gov/data-products/food-environment-atlas) |
| Lack of knowledge about healthy diets | Education (online, handouts), nutrition counseling | Harvard University Nutrition Source (https://www.hsph.harvard.edu/nutritionsource) USDA Choose My Plate (https://www.choosemyplate.gov) |
| Lack of satiety cues | Counseling, education on intuitive eating | Referral to psychologist or dietitian |
| Limited cooking skills | Education | Cooking classes through community centers, restaurants, or grocery stores |
USDA = U.S. Department of Agriculture.
TABLE 6. Dietary Resources for Patients
| American Academy of Family Physicians Patient Information Resource |
| Americans in Motion – Healthy Interventions |
| Centers for Disease Control and Prevention, Division of Nutrition, Physical Activity, and Obesity |
| Harvard University Nutrition Source |
| U.S. Department of Agriculture, Choose My Plate |
Data Sources: We searched PubMed, the Cochrane database, and Essential Evidence Plus using the key words diet, vegetable, fruit, legume, cardiovascular disease, diabetes, meat, dairy, nuts, carbohydrate, fats, and protein. We also reviewed http://www.nutrition.gov and http://www.nutritionsource.org. Search dates: January 2017 through March 2018.