Clinical Question
What is the best way to identify patients with acute pulmonary embolism (PE) who are at low risk of complications or death and may be candidates for early discharge?
Evidence Summary
Standard management of acute PE includes five days of inpatient treatment with parenteral anticoagulation, followed by long-term oral anticoagulation as an outpatient. However, guidelines from the American College of Chest Physicians state that early discharge before five days can be considered in some low-risk patients who have adequate home circumstances.1 These patients should meet four criteria: (1) clinically stable with good cardiopulmonary reserve; (2) no contraindications to anticoagulation, including recent bleeding; (3) no severe renal disease, liver disease, or thrombocytopenia; and (4) likely to adhere to therapy and feel well enough to be treated at home. Adequate home circumstances include well-maintained living conditions, a good support network, and the ability to be rehospitalized promptly if necessary.2
A recent meta-analysis identified 11 clinical decision rules that predict mortality in patients with newly diagnosed acute PE.2 The three rules with the highest sensitivity and the strongest evidence are the Pulmonary Embolism Severity Index (PESI), the simplified PESI (sPESI), and the European Society of Cardiology guidelines for the management of PE.
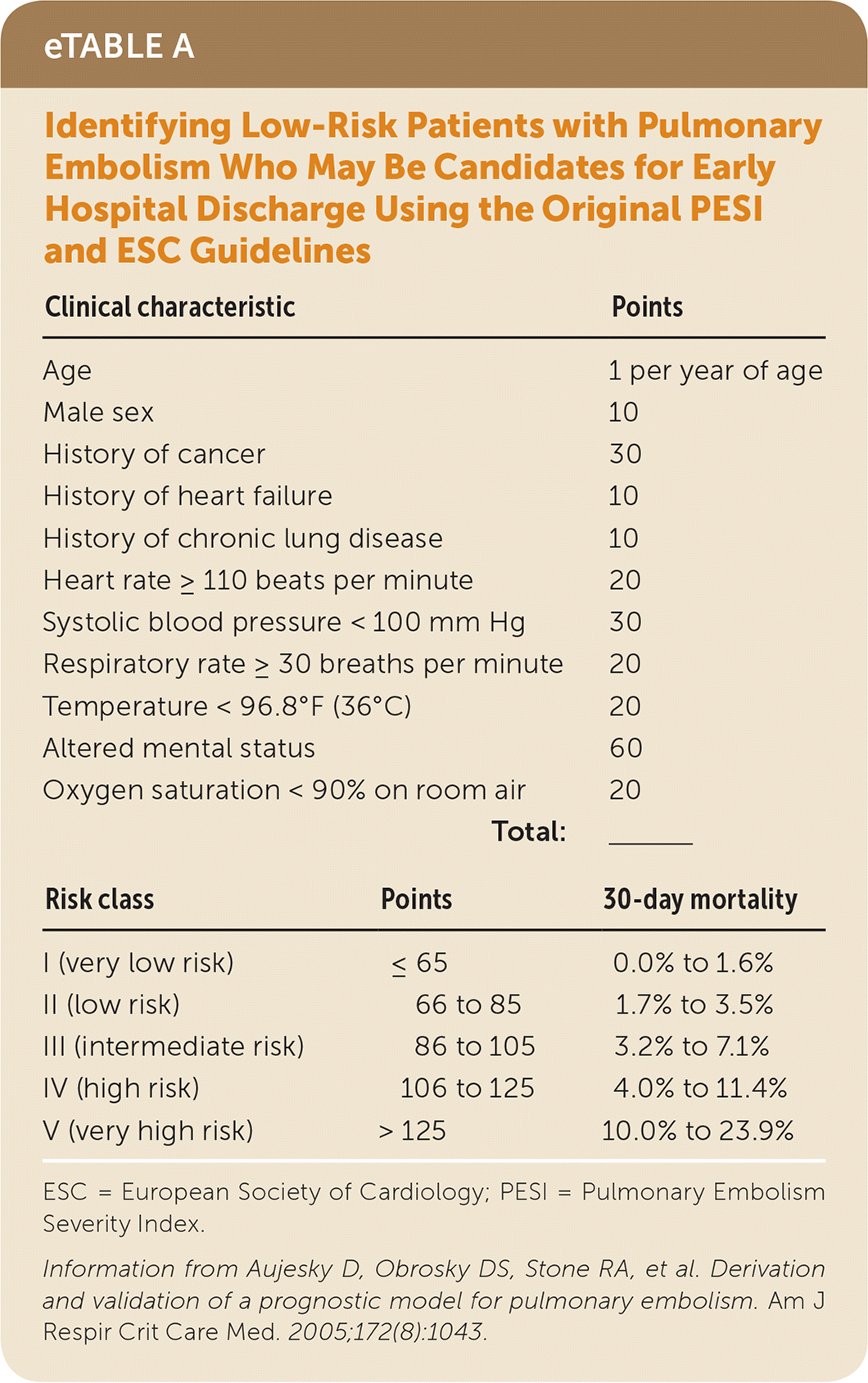
The PESI predicts 30-day outcomes in patients with PE and was created using 15,531 inpatients from 168 hospitals in the Pennsylvania Health Care Cost Containment Council database.3 It includes 11 clinical characteristics that are assigned different point values; the cumulative score puts patients in one of five risk categories (eTable A). It uses only objective information from the history and physical examination and does not require laboratory or radiographic testing.
eTABLE A Identifying Low-Risk Patients with Pulmonary Embolism Who May Be Candidates for Early Hospital Discharge Using the Original PESI and ESC Guidelines
| Clinical characteristic | Points | |
| Age | 1 per year of age | |
| Male sex | 10 | |
| History of cancer | 30 | |
| History of heart failure | 10 | |
| History of chronic lung disease | 10 | |
| Heart rate ≥ 110 beats per minute | 20 | |
| Systolic blood pressure < 100 mm Hg | 30 | |
| Respiratory rate ≥ 30 breaths per minute | 20 | |
| Temperature < 96.8°F (36°C) | 20 | |
| Altered mental status | 60 | |
| Oxygen saturation < 90% on room air | 20 | |
| Total: | ______ | |
| Risk class | Points | 30-day mortality |
| I (very low risk) | ≤ 65 | 0.0% to 1.6% |
| II (low risk) | 66 to 85 | 1.7% to 3.5% |
| III (intermediate risk) | 86 to 105 | 3.2% to 7.1% |
| IV (high risk) | 106 to 125 | 4.0% to 11.4% |
| V (very high risk) | > 125 | 10.0% to 23.9% |
ESC = European Society of Cardiology; PESI = Pulmonary Embolism Severity Index.
Information from Aujesky D, Obrosky DS, Stone RA, et al. Derivation and validation of a prognostic model for pulmonary embolism. Am J Respir Crit Care Med. 2005;172(8):1043.
The sPESI reduces the number of clinical characteristics to six and assigns one point for each. It was validated in 3,982 patients from an emergency department in Madrid, Spain.4 Overall, the sensitivity improved from 88.5% with the original PESI to 96% with the sPESI. The sPESI had the same positive predictive value of 11% and a higher negative predictive value (99% vs. 97.5%). Risk stratification was also simplified to two risk categories—low and high risk. Low-risk patients with an sPESI score of 0 had a 30-day mortality rate of 1% (95% confidence interval, 0.7% to 1.5%), whereas high-risk patients had a 30-day mortality rate of 9% (95% confidence interval, 8.1% to 9.8%).
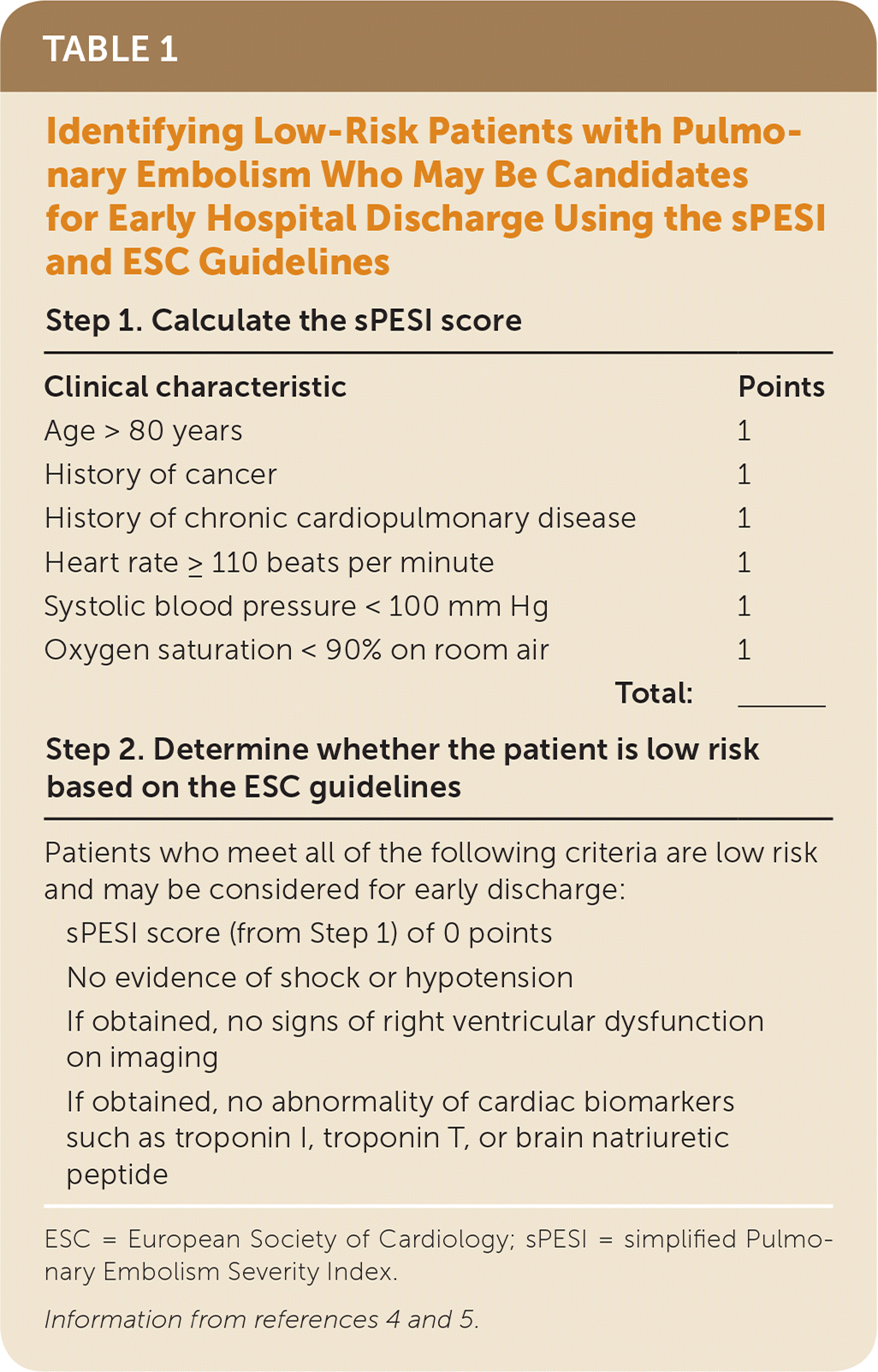
The European Society of Cardiology guidelines classify low-risk patients as those with a low-risk PESI score (risk class I or II using the original PESI and a score of 0 using the sPESI), as well as no shock or hypotension, no signs of right ventricular dysfunction on imaging, and no abnormality of cardiac biomarkers.5 Importantly, the European Society of Cardiology guidelines do not necessarily recommend obtaining cardiac biomarkers or cardiac imaging in every patient, but this additional information may be helpful when distinguishing low-risk patients from patients who may benefit from the standard five-day inpatient management. Table 1 summarizes risk prediction in patients with PE using the sPESI and European Society of Cardiology guidelines.4,5
TABLE 1. Identifying Low-Risk Patients with Pulmonary Embolism Who May Be Candidates for Early Hospital Discharge Using the sPESI and ESC Guidelines
| Step 1. Calculate the sPESI score | |
| Clinical characteristic | Points |
| Age > 80 years | 1 |
| History of cancer | 1 |
| History of chronic cardiopulmonary disease | 1 |
| Heart rate ≥ 110 beats per minute | 1 |
| Systolic blood pressure < 100 mm Hg | 1 |
| Oxygen saturation < 90% on room air | 1 |
| Total: | ______ |
| Step 2. Determine whether the patient is low risk based on the ESC guidelines | |
Patients who meet all of the following criteria are low risk and may be considered for early discharge:
| |
ESC = European Society of Cardiology; sPESI = simplified Pulmonary Embolism Severity Index.
Applying the Evidence
A 53-year-old woman presents to your primary care clinic with lower extremity deep venous thrombosis (DVT). She originally presented to an urgent care center earlier that day with two days of acute dyspnea and unilateral right leg swelling. The urgent care center ordered lower extremity Doppler ultrasonography and told the patient to follow up at her primary care office with the results. It was positive for an acute proximal DVT in the right leg.
The patient has no history of cancer, heart failure, or lung disease. She is an administrative assistant who lives at home with her husband and two children. On examination, she is afebrile with a body temperature of 98.3°F (36.8°C). Her heart rate is 96 beats per minute, blood pressure is 126/82 mm Hg, and respiratory rate is 14 breaths per minute. She is alert and oriented. She has an oxygen saturation of 95% on room air.
With her new-onset dyspnea and DVT, the patient's presentation is consistent with acute PE, prompting inpatient admission. On admission, the initial troponin T level is less than 0.01 ng per mL (0.01 mcg per L) and the initial brain natriuretic peptide level is 73 pg per mL (73 ng per L), suggesting no cardiac dysfunction. Using the sPESI and European Society of Cardiology guidelines, she is considered low risk. Because her home situation appears adequate with a good social support network and she is likely to adhere to treatment, it would be reasonable to consider early discharge rather than the standard five-day inpatient management.

