An estimated 10% to 30% of the global population has an allergic disease. Clinical presentations of allergic diseases, respiratory infections, and autoimmune conditions have similar features. Allergy and immunologic testing can help clarify the diagnosis and guide treatment. Immediate immunoglobulin E (IgE) and delayed T cell–mediated reactions are the main types of allergic responses. The allergens suspected in an immediate IgE-mediated response are identified through serum IgE-specific antibody or skin testing. For patients with an inhalant allergy, skin or IgE-specific antibody testing is preferred. In patients with food allergies, eliminating the suspected allergenic food from the diet is the initial treatment. If this is ineffective, IgE-specific antibody or skin testing can exclude allergens. An oral food challenge should be performed to confirm the diagnosis. Patients with an anaphylactic reaction to an insect sting should undergo IgE-specific antibody or skin testing. Skin testing for penicillin has a high negative predictive value and can help when penicillin administration is indicated and there are limited alternatives. Testing for other drug allergies has less well-determined sensitivity and specificity, but can guide the diagnosis. Patch testing can help identify the allergen responsible for contact dermatitis.
An estimated 10% to 30% of the global population has an allergic disease.1 The most common reasons that family physicians request a consultation for allergy testing are recurrent or persistent respiratory symptoms, skin rashes, repeated infections, and adverse reactions to foods, medications, and insect stings.2 Family physicians should consider referring patients to an allergist when there is an inadequate response to treatment or when a more accurate diagnosis would help with management.
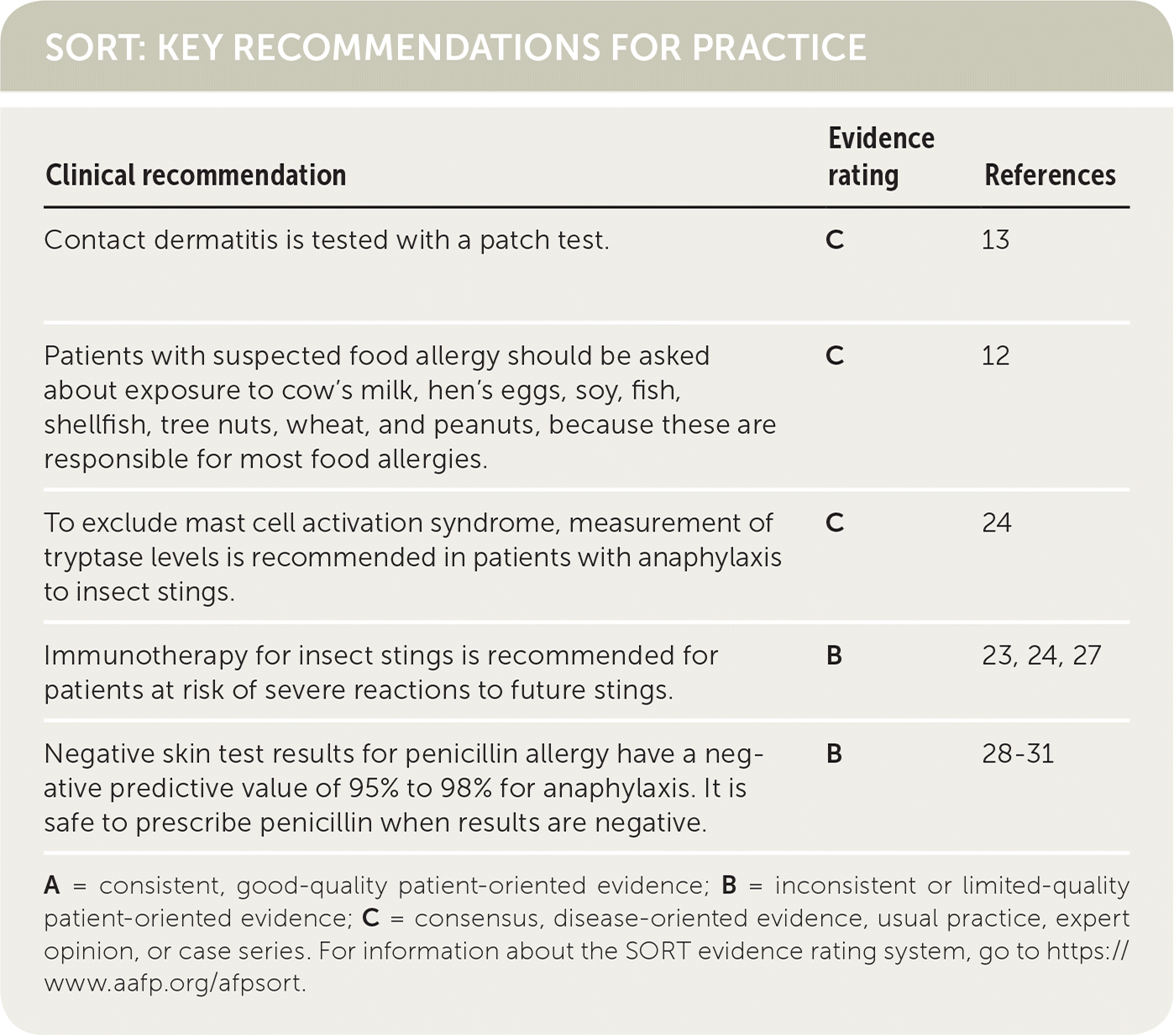
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Contact dermatitis is tested with a patch test. | C | 13 |
| Patients with suspected food allergy should be asked about exposure to cow's milk, hen's eggs, soy, fish, shellfish, tree nuts, wheat, and peanuts, because these are responsible for most food allergies. | C | 12 |
| To exclude mast cell activation syndrome, measurement of tryptase levels is recommended in patients with anaphylaxis to insect stings. | C | 24 |
| Immunotherapy for insect stings is recommended for patients at risk of severe reactions to future stings. | B | 23, 24, 27 |
| Negative skin test results for penicillin allergy have a negative predictive value of 95% to 98% for anaphylaxis. It is safe to prescribe penicillin when results are negative. | B | 28–31 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN ALLERGY/IMMUNOLOGY

| Recommendation | Sponsoring organization |
|---|---|
| Do not overuse non–beta-lactam antibiotics in patients with a history of penicillin allergy without an appropriate evaluation. | American Academy of Allergy, Asthma and Immunology |
| Do not perform food IgE testing without a history consistent with potential IgE-mediated food allergy. | American Academy of Allergy, Asthma and Immunology |
| Do not perform screening panels for food allergies without previous consideration of medical history. | American Academy of Pediatrics |
IgE = immunoglobulin E.
Source: For more information on the Choosing Wisely Campaign, see https://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
When Should Allergy Testing Be Considered?
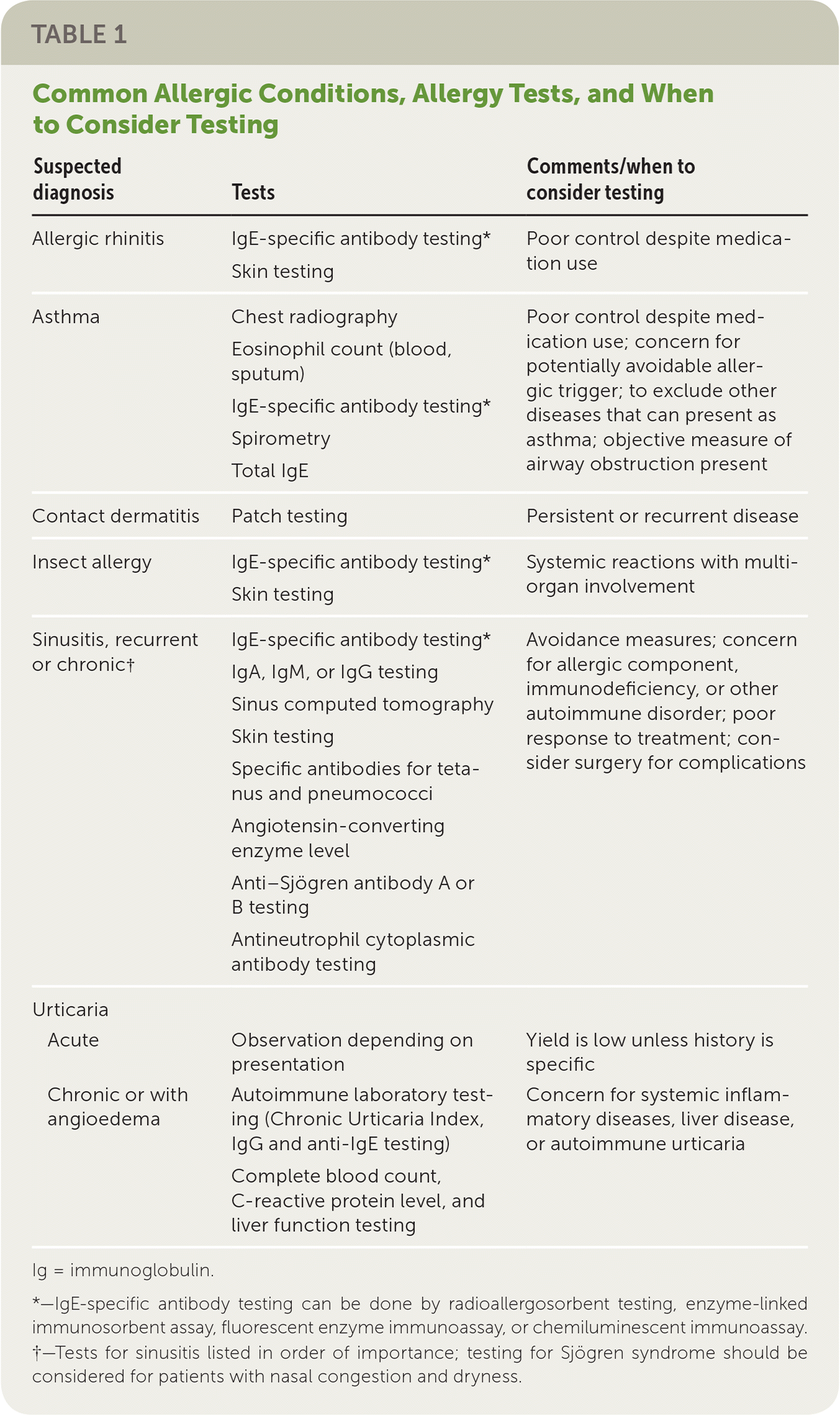
Clinical presentations of allergic diseases, respiratory infections, and autoimmune conditions have similar features. When the frequency, duration, and sequelae of upper respiratory infections exceed the norm or when rhinosinusitis or asthma symptoms persist despite treatment, further evaluation for allergic, anatomic, and immunologic causes should be considered.3 Allergy evaluation and testing should also be considered when it is important to determine the trigger for atopic dermatitis (eczema), contact dermatitis, urticaria, angioedema, and adverse reactions to foods2,4–6 (Table 1).
TABLE 1. Common Allergic Conditions, Allergy Tests, and When to Consider Testing
| Suspected diagnosis | Tests | Comments/when to consider testing | |
|---|---|---|---|
| Allergic rhinitis | IgE-specific antibody testing* | Poor control despite medication use | |
| Skin testing | |||
| Asthma | Chest radiography | Poor control despite medication use; concern for potentially avoidable allergic trigger; to exclude other diseases that can present as asthma; objective measure of airway obstruction present | |
| Eosinophil count (blood, sputum) | |||
| IgE-specific antibody testing* | |||
| Spirometry | |||
| Total IgE | |||
| Contact dermatitis | Patch testing | Persistent or recurrent disease | |
| Insect allergy | IgE-specific antibody testing* | Systemic reactions with multiorgan involvement | |
| Skin testing | |||
| Sinusitis, recurrent or chronic† | IgE-specific antibody testing* | Avoidance measures; concern for allergic component, immunodeficiency, or other autoimmune disorder; poor response to treatment; consider surgery for complications | |
| IgA, IgM, or IgG testing | |||
| Sinus computed tomography | |||
| Skin testing | |||
| Specific antibodies for tetanus and pneumococci | |||
| Angiotensin-converting enzyme level | |||
| Anti–Sjögren antibody A or B testing | |||
| Antineutrophil cytoplasmic antibody testing | |||
| Urticaria | |||
| Acute | Observation depending on presentation | Yield is low unless history is specific | |
| Chronic or with angioedema | Autoimmune laboratory testing (Chronic Urticaria Index, IgG and anti-IgE testing) | Concern for systemic inflammatory diseases, liver disease, or autoimmune urticaria | |
| Complete blood count, C-reactive protein level, and liver function testing | |||
Ig = immunoglobulin.
*—IgE-specific antibody testing can be done by radioallergosorbent testing, enzyme-linked immunosorbent assay, fluorescent enzyme immunoassay, or chemiluminescent immunoassay.
†—Tests for sinusitis listed in order of importance; testing for Sjögren syndrome should be considered for patients with nasal congestion and dryness.
EVIDENCE SUMMARY
Recurrent or Persistent Upper Respiratory Symptoms. Allergic diseases and rhinosinusitis are common in the general population. A national health survey in 2008 noted that 13.4% of adults had rhinosinusitis in the previous year.7 Adults have an average of two or three viral upper respiratory tract infections per year, and children have an average of six.8,9 These infections usually last seven to 10 days and tend to resolve within two weeks.3 When symptoms persist longer than these averages, family physicians should consider evaluating the patient for allergies. In patients with recurrent or persistent infections, immunodeficiency may need to be excluded. Primary immunodeficiencies occur in one out of 1,200 persons,10 and the incidence of acquired immunodeficiencies is higher.10,11
Dermatologic Conditions. Skin manifestations of allergic disorders include atopic dermatitis, contact dermatitis, urticaria, and angioedema. The clinical appearance of lesions and their duration and relationship with potential triggers assist with diagnosis. Allergy testing can help identify triggers. Food allergies cause up to 30% to 40% of eczema in young patients.12 In contact dermatitis, the lesions coincide with recent exposure to an allergen.13 Acute urticaria can be caused by an allergen exposure, infection (most commonly viral), autoimmune disease, or physical cause, or it can be idiopathic.14 Chronic urticaria is most likely due to autoimmune or physical causes, or is idiopathic.4,5 Potential causes of angioedema without urticaria include angiotensin-converting enzyme inhibitor use and hereditary or acquired C1 inhibitor deficiency. Angioedema is idiopathic in an estimated 10% of cases.15
What Are the Different Types of Allergy Testing?
Patch testing is preferred for delayed T cell–mediated response. Specific serum immunoglobulin E (IgE) antibody or allergy skin testing is preferred for patients with suspected IgE-mediated response.
EVIDENCE SUMMARY
Contact dermatitis is a classic example of a delayed T cell–mediated response, also known as type 4 delayed hypersensitivity. Common allergens that cause contact dermatitis include poison ivy, nickel, cosmetics, and rubber products. Patch testing is the preferred method and is usually performed in specialized dermatology clinics.13 The North American Contact Dermatitis Group patch tested 4,454 patients with contact dermatitis in 2005 and 2006.13 Approximately 19% were allergic to nickel, balsam of Peru, fragrances, quaternium-15, neomycin, bacitracin, and formaldehyde. Patch testing is performed by applying small metallic discs coated with the suspected allergens to the patient's back for 48 hours, after which the degree of erythema and dermatitis are documented. The sensitivity and specificity of the test vary depending on the substance and the severity of the reaction. For example, a mild or 1+ reaction to metal is 20% accurate, whereas a 3+ reaction is 90% accurate.6
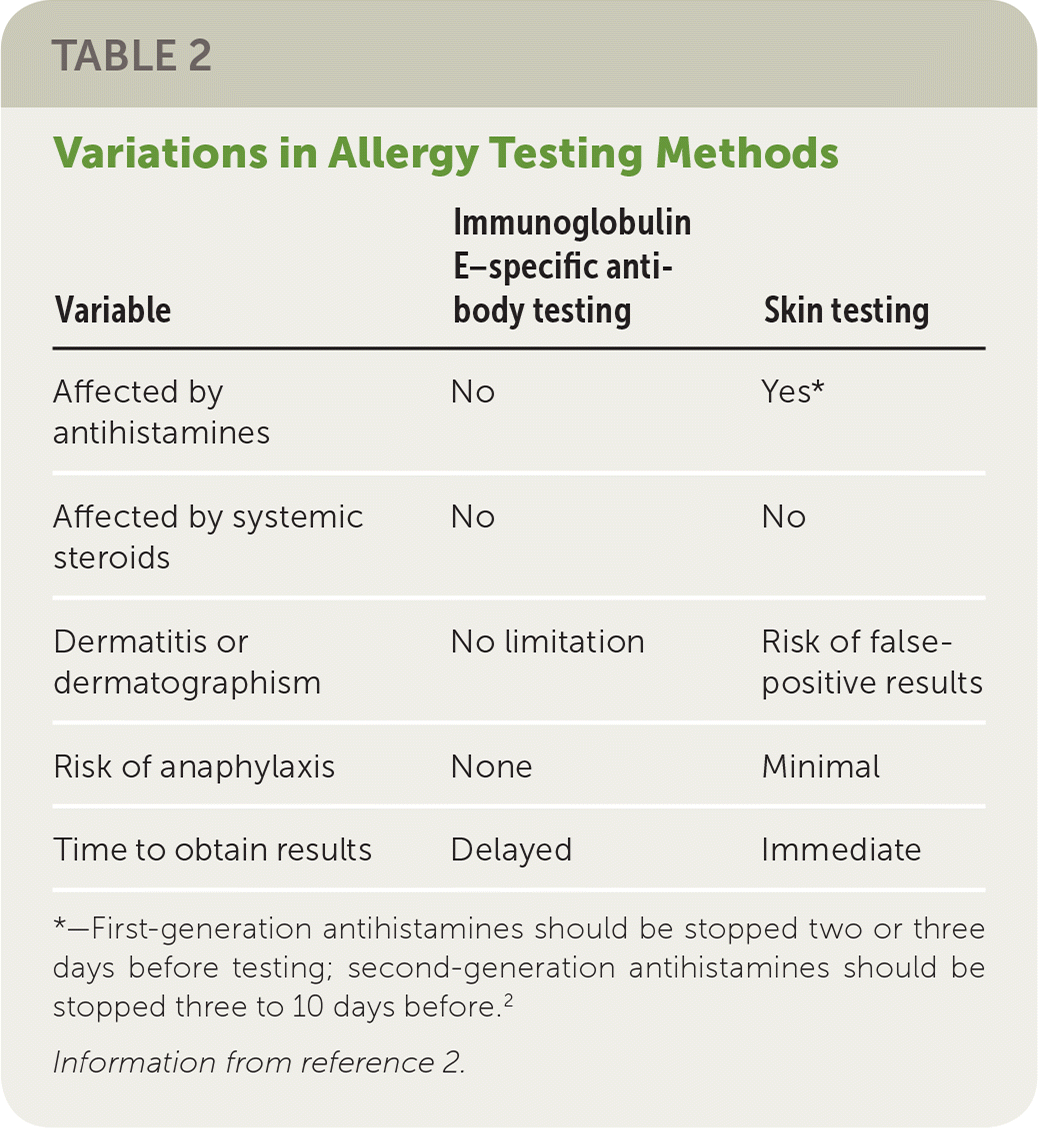
Allergic responses to inhalants, food, insect bites, or medications can precipitate an IgE response, which is characteristically rapid and, thus, called immediate-type hypersensitivity.16,17 The IgE response to an allergen can be assessed using skin or serum testing. Table 2 lists the advantages and disadvantages of allergy testing by IgE-specific antibody or skin testing.2
TABLE 2. Variations in Allergy Testing Methods
| Variable | Immunoglobulin E–specific antibody testing | Skin testing |
|---|---|---|
| Affected by antihistamines | No | Yes* |
| Affected by systemic steroids | No | No |
| Dermatitis or dermatographism | No limitation | Risk of false-positive results |
| Risk of anaphylaxis | None | Minimal |
| Time to obtain results | Delayed | Immediate |
*—First-generation antihistamines should be stopped two or three days before testing; second-generation antihistamines should be stopped three to 10 days before.2
Information from reference 2.
Skin testing using the prick method is typically performed by allergists. Skin testing can be percutaneous, in which a diluted allergen is pricked or scratched into the skin surface, or intradermal, in which the allergen is injected. Patients who require more sensitive testing for insect stings or a penicillin allergy should have an intradermal test. Knowing the causal allergen helps provide clinically relevant information for avoidance and treatment.
Serum IgE-specific antibody testing has no limitations in patients with dermographism or dermatitis, and it is not blocked by antihistamines. It is preferred in patients at risk of severe anaphylaxis. It is performed through radioallergosorbent testing, enzyme-linked immunosorbent assay (most common), fluorescent enzyme immunoassay, or chemiluminescent immunoassay. To determine the correct test to order, the clinician can search under IgE on the websites of many laboratories for a specific allergen.3 There has been a significant effort to standardize and evaluate the consistency of testing for more accurate results. The training and experience of the physician supervising the test improves performance and interpretation of results.16
Which Tests Are Available for Inhalant Allergens?
Both skin prick and IgE-specific antibody testing can be used to test for inhalant allergies. Skin testing is preferable because it is more cost-effective than laboratory testing, which allows for testing for more allergens.
EVIDENCE SUMMARY
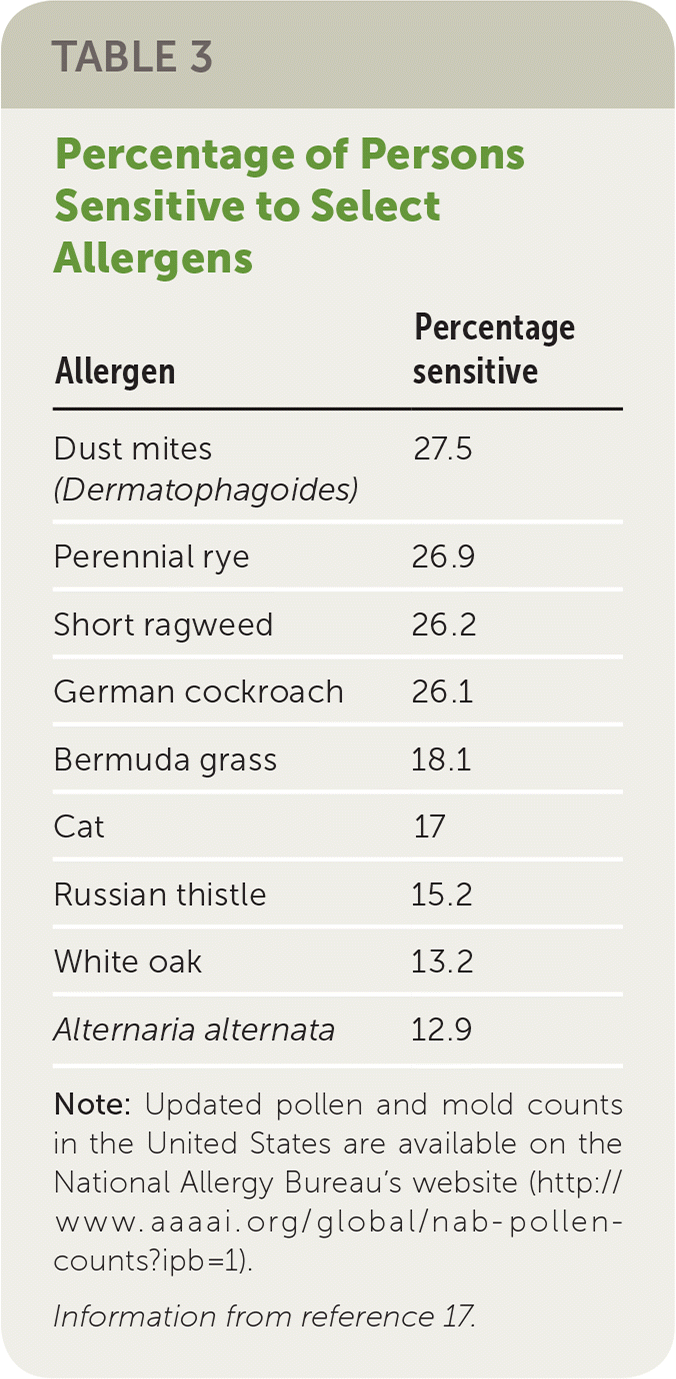
When testing for inhalant allergens, it is crucial to determine which allergens the patient is most commonly exposed to. Pollens are common inhalant allergens and vary by geographic region; Table 3 lists the most common ones in the United States.17 The results of IgE-specific antibody testing are reported as concentrations of specific IgE antibody in classes ranging from 0 to 6. The interpretation of results depends on the patient's clinical history.18
TABLE 3. Percentage of Persons Sensitive to Select Allergens
| Allergen | Percentage sensitive |
|---|---|
| Dust mites (Dermatophagoides) | 27.5 |
| Perennial rye | 26.9 |
| Short ragweed | 26.2 |
| German cockroach | 26.1 |
| Bermuda grass | 18.1 |
| Cat | 17 |
| Russian thistle | 15.2 |
| White oak | 13.2 |
| Alternaria alternata | 12.9 |
Note: Updated pollen and mold counts in the United States are available on the National Allergy Bureau's website (http://www.aaaai.org/global/nab-pollen-counts?ipb=1).
Information from reference 17.
Which Tests Are Available for Food Allergies?
Tests for food allergies include avoidance of the food, skin testing, laboratory testing, and an oral food challenge. In patients with suspected food allergy, the first step should be elimination of the suspected food to see if symptoms resolve. IgE-specific antibody and skin testing are helpful to confirm or exclude allergens. An oral food challenge is used to confirm a negative or questionable test result.
EVIDENCE SUMMARY
Patients with suspected food allergy should be asked about exposure to the foods that most commonly cause IgE-mediated reactions12,19 (Table 411,19 ). More than 170 foods have been reported as allergens, although any food can produce an allergy.19 Many patients mistakenly think they have a food allergy based on a positive allergy test, which is not clinically relevant; these patients most often can eat the tested food with no problem.12,19–22 IgE-specific antibody and skin testing have limited positive predictive value. In contrast, their negative predictive value is high and can help exclude allergies.20 For patients with a serum-specific IgE antibody level of less than 0.35 kUA per L and a negative skin prick test, the probability of a positive response to an oral food challenge is low.20 A negative food allergy result and negative oral food challenge can help reassure the patient and family that no allergy is present,20 and no further testing is necessary.
TABLE 4. Common Foods that Produce Allergic Reactions
IgE-specific antibody or skin testing can be helpful in the evaluation of patients who have an immediate reaction to a food. In patients with a history suggestive of anaphylaxis to a particular food, the response to specific IgE antibody levels and a skin test can confirm and predict the results of an oral food challenge.12,20 Oral food challenges are typically performed in an allergist's office where the proper equipment and expertise are available in the event of anaphylaxis. To avoid this possibility, the test is reserved for patients with a low risk of severe reaction, and the tested food is administered using progressive dosing until a customary meal dose is met.
When and How Should Testing for Insect Allergy Be Performed?
Skin prick, intradermal, or IgE-specific antibody testing is indicated for patients with anaphylaxis and those older than 17 years who have had systemic diffuse cutaneous reactions from insect stings. Allergy immunotherapy is indicated for patients with positive results; it has a high degree of protection against future reactions. Current guidelines recommend measuring tryptase levels in patients with anaphylaxis to exclude mast cell activation syndrome.23–27
EVIDENCE SUMMARY
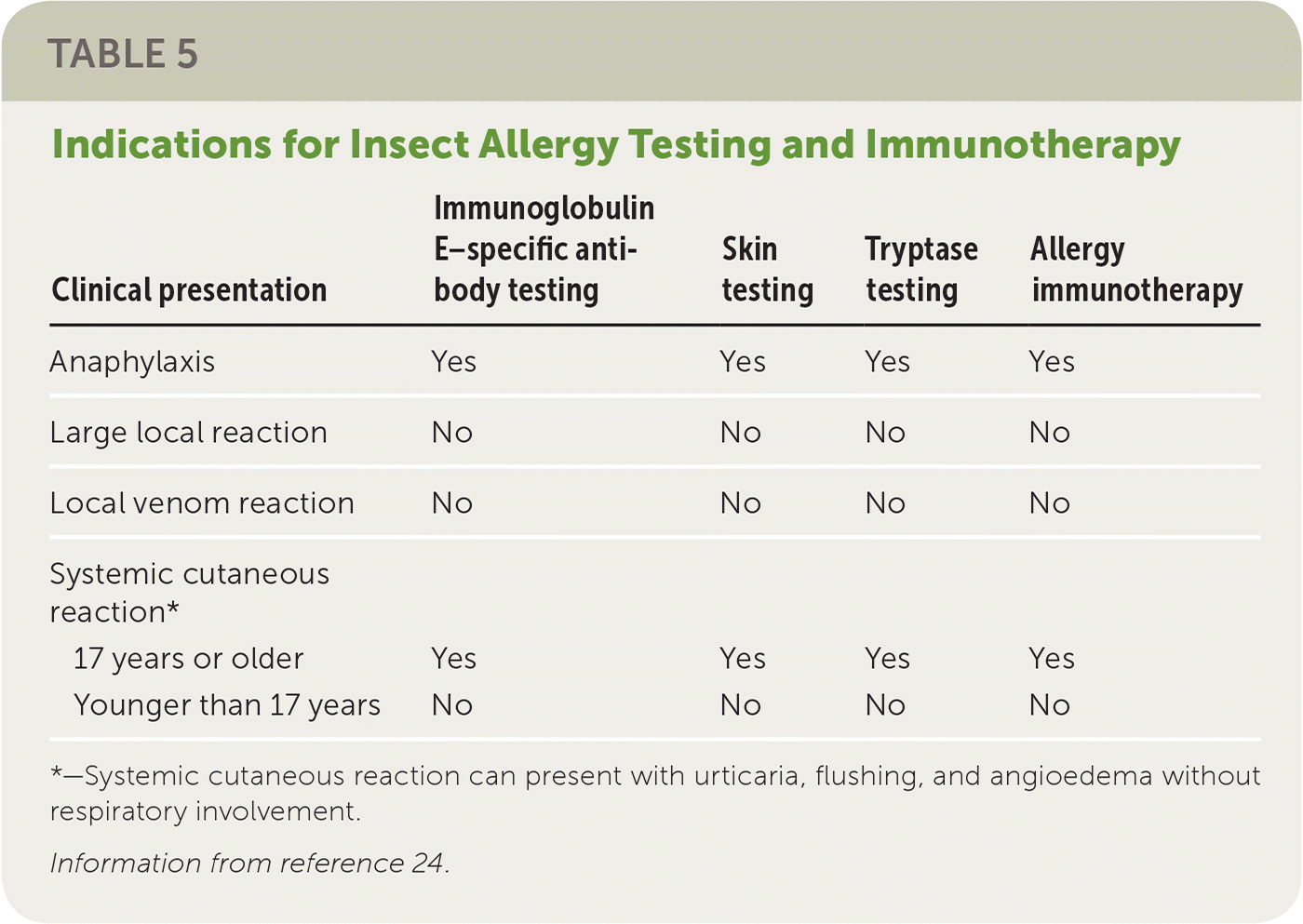
Stinging insects are responsible for approximately 10% of anaphylaxis cases.24 At least 40 deaths per year in the United States are attributed to insect sting–induced anaphylaxis.24 Reactions to insect stings are secondary to the venom itself (pain, burning, or a pustule) or are immunologically mediated. Immunologic reactions can present as large local reactions that manifest several hours after the sting and can persist for several days, but do not increase the risk of systemic reactions. They can also occur immediately, distant to the area of the sting, or have multiorgan involvement. Such reactions are considered systemic or anaphylactic and confer an increased risk of future anaphylaxis. Table 5 provides a summary of insect allergy testing and treatment approaches.24 It is often difficult to identify the stinging insect, and it is typical to test for the most common ones (fire ants, honey bees, yellow hornets, yellow jackets, wasps, and white-faced hornets).
TABLE 5. Indications for Insect Allergy Testing and Immunotherapy
| Clinical presentation | Immunoglobulin E–specific antibody testing | Skin testing | Tryptase testing | Allergy immunotherapy | |
|---|---|---|---|---|---|
| Anaphylaxis | Yes | Yes | Yes | Yes | |
| Large local reaction | No | No | No | No | |
| Local venom reaction | No | No | No | No | |
| Systemic cutaneous reaction* | |||||
| 17 years or older | Yes | Yes | Yes | Yes | |
| Younger than 17 years | No | No | No | No | |
*—Systemic cutaneous reaction can present with urticaria, flushing, and angioedema without respiratory involvement.
Information from reference 24.
A study of the natural history of systemic cutaneous reactions in children younger than 17 years showed that subsequent reactions were milder, even in patients who did not undergo immunotherapy.26,27 Current guidelines recommend immunotherapy primarily for patients who are at risk of severe reactions from future stings.23–26 Tryptase levels should be measured in patients with systemic reactions from insect stings; if they are higher than 11.5 ng per mL, further evaluation is needed to exclude mast cell activation syndrome.24
When Should Allergy Testing for Antibiotics Be Considered?
Testing can be helpful in patients with a history of allergy to antibiotics when there are limited alternative treatments.28
EVIDENCE SUMMARY
Penicillin allergy is the most commonly reported drug allergy in the United States. However, only a small number of patients have IgE antibodies to penicillin, and most who claim to have a penicillin allergy will likely tolerate the drug.28 Skin testing shows that only 1% to 10% of patients with self-reported penicillin allergy have an actual allergy.29,30 Several reagents are required for penicillin allergy testing, which is best performed in an allergist's office. Negative skin test results have a negative predictive value of 95% to 98% for anaphylaxis.28–31 A negative result is often followed by an oral challenge, with monitoring for confirmation. It is safe to prescribe penicillin after a negative skin test result.30,31 Testing for allergy to other medications has less well-determined sensitivity and specificity, but can be used as a guide for a challenge or desensitization.32
Data Sources: We conducted searches in PubMed Clinical Queries, Essential Evidence Plus, and Google Scholar using the key terms allergy testing, allergic rhinitis, food allergy, insect allergy, asthma, urticaria, angioedema, and IgE. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. We also searched the American Academy of Allergy, Asthma and Immunology practice parameters, POEMs critical appraisals, Cochrane reviews, and decision tools. Search dates: May 31, 2017, to January 11, 2018.
The authors thank Sherri Mason Swilley, CPC, CPCO, and Kiarash P. Rahmanian, MPH, for assistance with the manuscript.


