A 69-year-old man and self-described hermit presented with erythema on his left leg. He was prescribed a seven-day course of trimethoprim/sulfamethoxazole for suspected cellulitis. A lower extremity venous duplex scan was negative for deep venous thrombosis. He presented to the emergency department one week later with spreading erythema and increased pain on weight bearing. He had new petechiae on his right lower extremity. He had a history of tobacco use, long-term daily alcohol use, and hypertension.
Physical examination revealed an open eschar over the left medial malleolus (Figure 1). There was no fluctuance, crepitus, or warmth. Posterior tibial pulses were weak but present on Doppler ultrasonography. Capillary refill was normal. Laboratory workup was notable for chronic iron deficiency anemia and an international normalized ratio of 1.4 without anticoagulation. An arterial duplex scan showed complete occlusion of the midanterior and distal anterior tibial artery. Magnetic resonance imaging showed intramuscular lesions consistent with chronic fibrosis from ischemia. Lower extremity punch biopsies were conducted to assist with diagnosis. Pathology showed perifollicular hemorrhage.
FIGURE 1
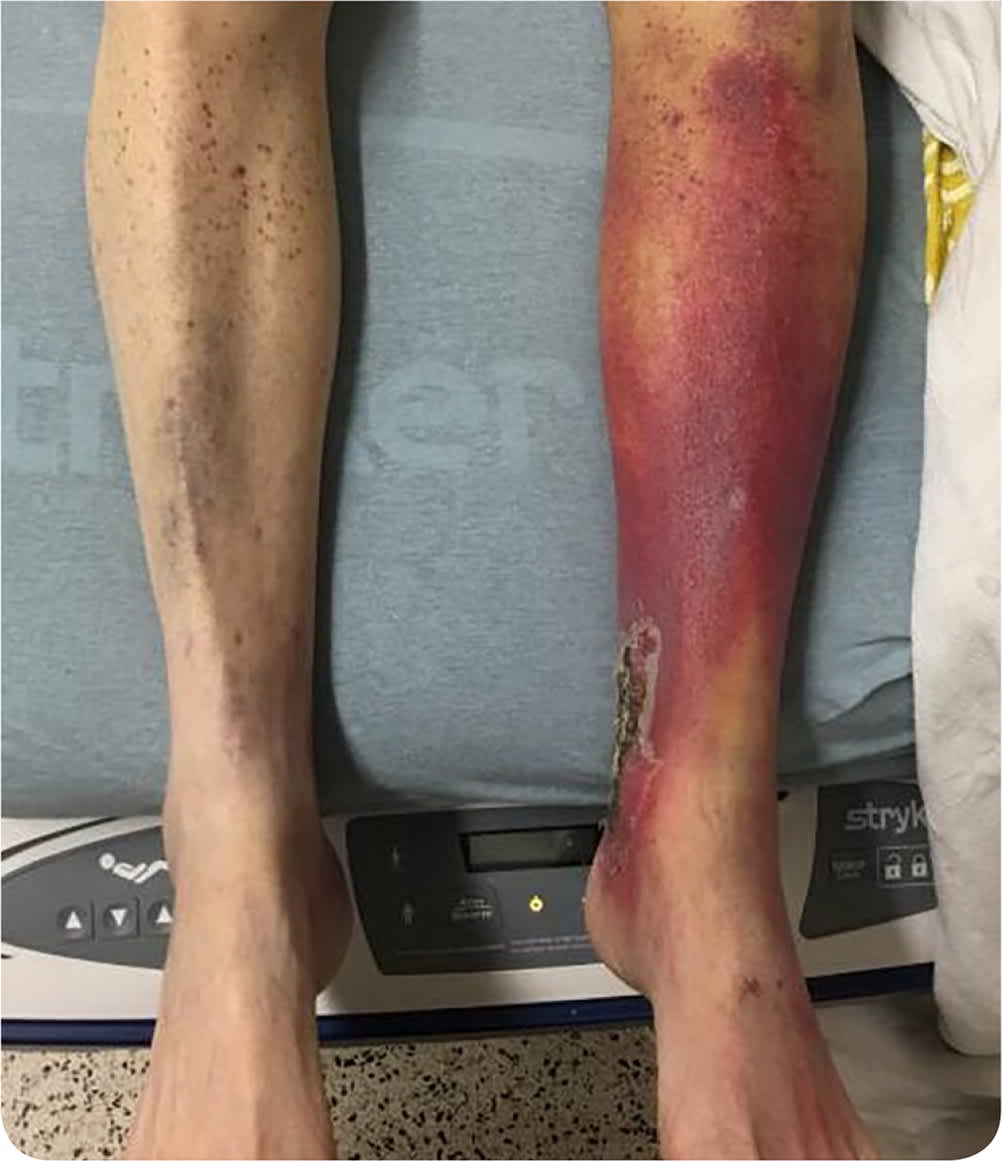
Question
Based on the patient's history, physical examination, and test results, which one of the following is the most likely diagnosis?
A. Cellulitis refractory to treatment.
B. Ischemia due to peripheral artery disease.
C. Necrotizing fasciitis.
D. Small vessel vasculitis.
E. Vitamin C deficiency (scurvy).
Discussion
The answer is E: vitamin C deficiency (scurvy). A diagnostic punch biopsy demonstrated perifollicular hemorrhage consistent with scurvy. Low vitamin C levels predicate decreased synthesis of collagen, which allows for the breakdown of connective tissue, followed by the development of erythema, necrotic areas, and anemia. Many patients with scurvy have eschars.1,2 Because of his isolated lifestyle, the patient may have other nutrient deficiencies.
Cellulitis presents as skin breakdown followed by unilateral painful erythema that is warm to the touch. It is typically associated with induration, fluctuance, or drainage. Cellulitis often leads to systemic symptoms such as fevers, chills, or tachycardia, especially with failed outpatient therapy.3
The patient had pulses on Doppler ultrasonography and adequate capillary refill, which rules out acute ischemia. Despite the eschar, he did not have evidence of frank ischemia or gangrene. The tibial artery clot was thought to be chronic because of the atherosclerosis and collateralization seen on imaging. Unless there are signs of acute thrombus and ischemia, the management of peripheral vascular disease is optimization of medical therapy.4
Necrotizing fasciitis is an uncommon severe infection, typically of the extremities. The condition rapidly progresses over a few days. The skin changes begin as painful erythema, but patches of blue-gray skin and bullae often develop.5 The patient lacked signs of systemic toxicity.
Small vessel vasculitis usually affects multiple systems, whereas this patient's symptoms were localized to the lower extremities. A biopsy that is inconclusive or suggests vasculitis would warrant further workup with antinuclear antibody or antineutrophil cytoplasmic antibody testing.4,6
SUMMARY TABLE
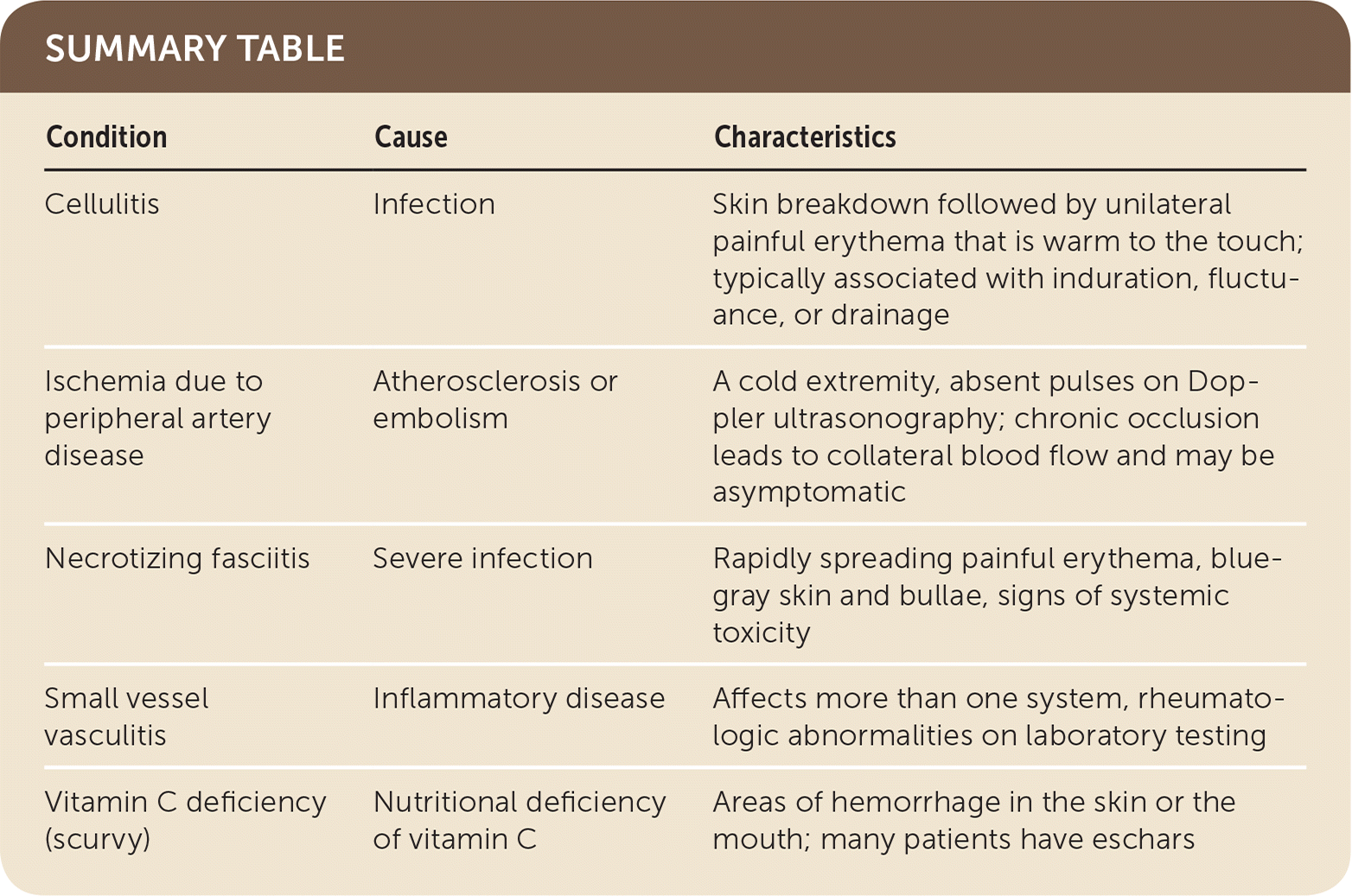
| Condition | Cause | Characteristics |
|---|---|---|
| Cellulitis | Infection | Skin breakdown followed by unilateral painful erythema that is warm to the touch; typically associated with induration, fluctuance, or drainage |
| Ischemia due to peripheral artery disease | Atherosclerosis or embolism | A cold extremity, absent pulses on Doppler ultrasonography; chronic occlusion leads to collateral blood flow and may be asymptomatic |
| Necrotizing fasciitis | Severe infection | Rapidly spreading painful erythema, blue-gray skin and bullae, signs of systemic toxicity |
| Small vessel vasculitis | Inflammatory disease | Affects more than one system, rheumatologic abnormalities on laboratory testing |
| Vitamin C deficiency (scurvy) | Nutritional deficiency of vitamin C | Areas of hemorrhage in the skin or the mouth; many patients have eschars |

