Delivering serious, bad, or life-altering news to a patient is one of the most difficult tasks physicians encounter. Broadly defined as information that may alter a patient's view of his or her future, bad news may include information related to a chronic disease (e.g., diabetes mellitus), a life-altering illness (e.g., multiple sclerosis), or an injury leading to significant change (e.g., a season-ending knee injury). Patients prefer to receive such news in person, with the physician's full attention, and in clear, easy-to-understand language with adequate time for questions. Most patients prefer to know their diagnosis, but the amount of desired details varies among different cultures and by education level, age, and sex. The physician should respect the patient's unique preferences for receiving bad news. Physicians may experience stress related to providing bad news that extends beyond the actual conversation. For example, physicians are afraid of eliciting an emotional reaction, being blamed for the bad news, and expressing their emotions during the process. Physicians often withhold information or are overly optimistic regarding prognosis, but this can lead to confusion for patients regarding their condition. There are several algorithms available to help guide the physician in the delivery of bad news, including the SPIKES protocol (setting, perception, invitation, knowledge, emotion, and strategy and summary). Skillful delivery of bad news can provide comfort for the patient and family.
Family physicians, through building long-term, multigenerational relationships with patients and families, often find themselves the bearer of bad or serious news. Bad news is broadly defined as information that will alter a patient's view of his or her future and result in persistent cognitive, behavioral, and emotional responses.1 Some research suggests that alternative terms, including serious news or life-altering news, may be more appropriate.2 Ultimately, the determination of what is bad news lies not with the physician, but with the person receiving the news.3 Although classically related to cancer or a terminal diagnosis, bad or serious news may also include information related to diagnosis of a chronic disease (e.g., diabetes mellitus), a life-altering illness (e.g., multiple sclerosis), or an injury leading to a significant change (e.g., a season-ending knee injury). Most of the research into the delivery of bad news, however, has focused on patients with cancer and subsequently applied to the delivery of bad or serious news in nononcologic settings.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
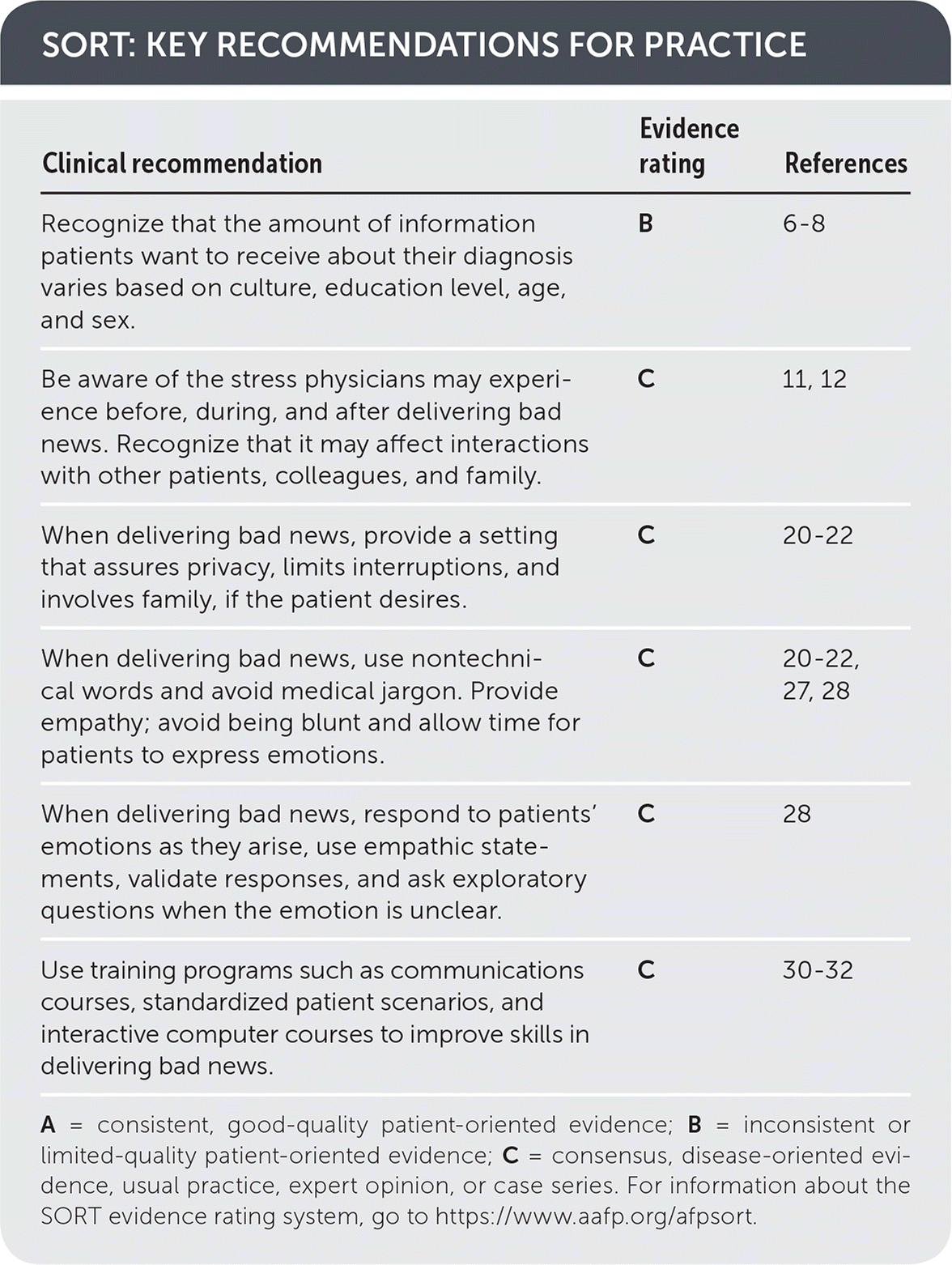
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Recognize that the amount of information patients want to receive about their diagnosis varies based on culture, education level, age, and sex. | B | 6–8 |
| Be aware of the stress physicians may experience before, during, and after delivering bad news. Recognize that it may affect interactions with other patients, colleagues, and family. | C | 11, 12 |
| When delivering bad news, provide a setting that assures privacy, limits interruptions, and involves family, if the patient desires. | C | 20–22 |
| When delivering bad news, use nontechnical words and avoid medical jargon. Provide empathy; avoid being blunt and allow time for patients to express emotions. | C | 20–22, 27, 28 |
| When delivering bad news, respond to patients' emotions as they arise, use empathic statements, validate responses, and ask exploratory questions when the emotion is unclear. | C | 28 |
| Use training programs such as communications courses, standardized patient scenarios, and interactive computer courses to improve skills in delivering bad news. | C | 30–32 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Patient Preferences
In the paternalistic patient-care model, the physician acts as the patient's guardian, providing selected information to steer the patient to what the physician identifies as the best decision.4 The patient-centered decision-making model became prevalent in the late 20th century, prompting the publication of several expert consensus guidelines to aid physicians in delivering bad news.5 At the same time, there has been increased attention to end-of-life care and to teaching communication skills in medical school. There has also been increased study of patient preferences in an effort to move toward evidence-based guidelines.
Most patients prefer to know their diagnosis, but the amount of information they want varies among demographics. For example, younger patients, female patients, and patients with higher education levels tend to desire more detailed information.6,7 The amount of information is also dependent on cultural norms and ethnicity. For example, one study found that Korean Americans and Mexican Americans are more likely to favor a family-centered medical decision model; in contrast, African Americans and European Americans prefer a model with more individual patient autonomy.8 Given such nuances, it is essential that physicians recognize and determine patients' preferences before delivering bad or serious news.
Patients prefer to receive bad news in person with the physician's full attention, and they want to be confident in the physician's skill.9 Patients desire honesty, simple and clear language that they can understand, and adequate time for questions.7 Even among patients who desire details of the diagnosis and treatment options, many patients are not interested in a specific prognosis.6
Cultural Barriers
Compared with a century ago, when most deaths occurred in the home, most deaths now occur in a hospital or facility. Because many persons lack firsthand experience with death, discussing it may be more difficult. Patients have unrealistic expectations of health and life, perhaps secondary to overplayed media reports of medical advances or unrealistic television portrayals. For example, the fictional survival rate of cardiopulmonary resuscitation portrayed on television is twice that of real-life statistics.10 In addition, religious diversity makes it increasingly common that the physician and patient will have different views about an afterlife.
Physician Fears
Physicians experience stress related to providing bad news, and this stress often extends beyond the actual conversation.11 Evidence suggests that this stress does not lessen with a physician's years in practice or experience with delivering bad news.12 In general, physicians fear eliciting an emotional reaction, being blamed for the bad news, and expressing their emotions during the process.
Physicians also fear that delivering truthful news about a terminal illness will leave a patient depressed, without hope, and with a shortened life span if hospice is involved.13 In reality, end-of-life discussions are associated with less aggressive medical care, earlier hospice referral, and improved quality of life.14 Research demonstrates increased survival time for hospice patients overall, with the greatest increase observed in patients with congestive heart failure, lung cancer, or pancreatic cancer.15
Physicians, for a variety of reasons (e.g., sensitivity to cultural norms, a patient's emotional state, respect for patient and family wishes, fear of destroying hope), often withhold information or overestimate survival.16,17 The inability to effectively and truthfully deliver bad news can lead to patient confusion. For example, one study of patients with incurable lung cancer receiving palliative radiation found that more than 60% believed their treatment may lead to a cure.18 Although bad news may initially increase psychological stress, full and accurate disclosure may help the patient and family emotionally and practically, making the time the patient has left as meaningful as possible.19
Models
There are several protocols and mnemonics to guide the delivery of bad or serious news, including ABCDE (Table 120 ), BREAKS (Table 221 ), and SPIKES (Table 322 ). The SPIKES protocol, initially developed to guide oncologists in delivering bad news to patients with cancer, may also be used with children.2 Common themes of the protocols include establishing rapport in an appropriate setting, determining the patient's previous knowledge and desire for details, avoiding medical jargon and euphemisms, supporting patient emotions, allowing for questions, summarizing, and determining next steps.
TABLE 1. ABCDE Protocol for Delivering Bad News

| Advanced preparation Review the patient's history, mentally rehearse, and emotionally prepare. Arrange for a support person if the patient desires. Determine what the patient knows about his or her illness. |
| Build a therapeutic environment/relationship Ensure adequate time and privacy. Provide seating for everyone. Maintain eye contact and sit close enough to touch the patient, if appropriate. |
| Communicate well Avoid medical jargon, and use plain language. Allow for silence, and move at the patient's pace. |
| Deal with patient and family reactions Address emotions as they arise. Actively listen, explore feelings, and express empathy. |
| Encourage and validate emotions Correct misinformation. Explore what the bad news means to the patient. Be cognizant of your emotions and those of your staff. |
Adapted with permission from Rabow MW, McPhee SJ. Beyond breaking bad news: how to help patients who suffer. West J Med. 1999;171(4):261.
TABLE 2. BREAKS Protocol for Delivering Bad News

| Background Know the patient's background, clinical history, and family or support person. |
| Rapport Build rapport, and allow time and space to understand the patient's concerns. |
| Explore Determine the patient's understanding, and start from what the patient knows about the illness. |
| Announce Preface the bad news with a warning; use nonmedical language. Avoid long explanations or stories of other patients. Give no more than three pieces of information at a time. |
| Kindle Address emotions as they arise. Ask the patient to recount what you said. Be aware of denial. |
| Summarize Summarize the bad news and the patient's concerns. Provide a written summary for the patient. Ensure patient safety (e.g., suicidality, ability to safely drive home) and provide follow-up options (e.g., on-call physician, help line, office appointment). |
Information from reference 21.
TABLE 3. SPIKES Protocol for Delivering Bad News
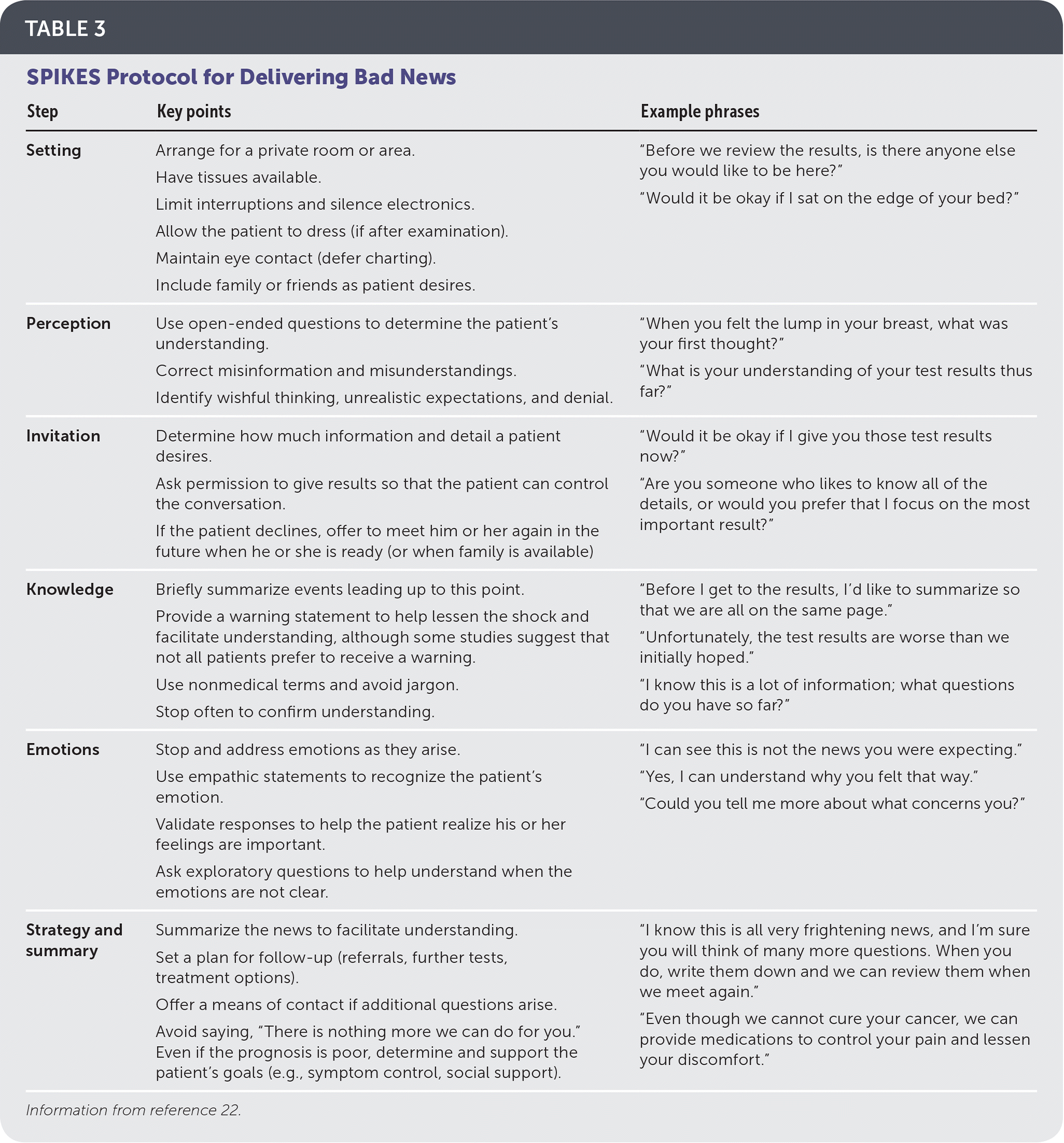
| Step | Key points | Example phrases |
|---|---|---|
| Setting | Arrange for a private room or area. Have tissues available. Limit interruptions and silence electronics. Allow the patient to dress (if after examination). Maintain eye contact (defer charting). Include family or friends as patient desires. | “Before we review the results, is there anyone else you would like to be here?” “Would it be okay if I sat on the edge of your bed?” |
| Perception | Use open-ended questions to determine the patient's understanding. Correct misinformation and misunderstandings. Identify wishful thinking, unrealistic expectations, and denial. | “When you felt the lump in your breast, what was your first thought?” “What is your understanding of your test results thus far?” |
| Invitation | Determine how much information and detail a patient desires. Ask permission to give results so that the patient can control the conversation. If the patient declines, offer to meet him or her again in the future when he or she is ready (or when family is available) | “Would it be okay if I give you those test results now?” “Are you someone who likes to know all of the details, or would you prefer that I focus on the most important result?” |
| Knowledge | Briefly summarize events leading up to this point. Provide a warning statement to help lessen the shock and facilitate understanding, although some studies suggest that not all patients prefer to receive a warning. Use nonmedical terms and avoid jargon. Stop often to confirm understanding. | “Before I get to the results, I'd like to summarize so that we are all on the same page.” “Unfortunately, the test results are worse than we initially hoped.” “I know this is a lot of information; what questions do you have so far?” |
| Emotions | Stop and address emotions as they arise. Use empathic statements to recognize the patient's emotion. Validate responses to help the patient realize his or her feelings are important. Ask exploratory questions to help understand when the emotions are not clear. | “I can see this is not the news you were expecting.” “Yes, I can understand why you felt that way.” “Could you tell me more about what concerns you?” |
| Strategy and summary | Summarize the news to facilitate understanding. Set a plan for follow-up (referrals, further tests, treatment options). Offer a means of contact if additional questions arise. Avoid saying, “There is nothing more we can do for you.” Even if the prognosis is poor, determine and support the patient's goals (e.g., symptom control, social support). | “I know this is all very frightening news, and I'm sure you will think of many more questions. When you do, write them down and we can review them when we meet again.” “Even though we cannot cure your cancer, we can provide medications to control your pain and lessen your discomfort.” |
Information from reference 22.
SPIKES Protocol
SETTING
Reviewing the patient's history and situation are critical components of the first step. Mental rehearsal may increase physician confidence. A proper setting also assures privacy, limits interruptions, and involves family if the patient desires. Tissues should be available. Sitting at the bedside increases the perceived time spent in discussion,23 and although one study found that women with cancer consider a seated physician more compassionate,24 sitting does not necessarily influence patient perception of the physician's bedside manner.25 For this reason, to enhance communication, the physician should ask the patient's preference.26
PERCEPTION
The second step is to determine the patient's understanding of his or her condition. The physician should use broad, open-ended questions, such as, “What is your understanding of what has occurred so far?” The physician may also identify misunderstanding, denial, and unrealistic expectations.
INVITATION
There is variability among patients' desire for detailed information. It is important to obtain the patient's permission before delivering the bad news. A phrase such as, “Would it be okay to give you the results of the tests right now?” engages the patient in shared decision making. If the patient declines the invitation, it is important to determine the reason (e.g., waiting for a spouse, partner, or other family member to provide support).
KNOWLEDGE
Physicians should use simple, nontechnical words and avoid medical jargon when delivering bad news. They should provide empathy by avoiding being blunt and by allowing time for patients to express emotions. Information should be provided in small amounts, followed by a confirmation of understanding. The SPIKES method advocates delivering a warning statement before the bad news (e.g., “I'm afraid the test results were worse than we initially hoped.”), but some research indicates that this is not a universal preference.27
EMOTIONS
Before providing additional information or even immediate reassurance, the physician should acknowledge and accept the patient's response. Empathic statements (e.g., “It seems like you are feeling…”) are useful during expressions of sadness and anger. Validating responses (e.g., “This has been a difficult time for you.”) helps patients realize their feelings are important. Supportive statements (e.g., “I am here to help you.”) guard against the feeling of abandonment, and exploratory questions (e.g., “You said you were worried about your children. Can you tell me more about that?”) are helpful when the emotion is not clear. NURSE (naming, understanding, respecting, supporting, exploring) is a useful acronym of the key steps in expressing empathy (Table 4).28 A physician can accept a patient's response (e.g., the desire to be cured of cancer), without agreeing with it (e.g., cure is not likely).
TABLE 4. NURSE Mnemonic for Expressing Empathy
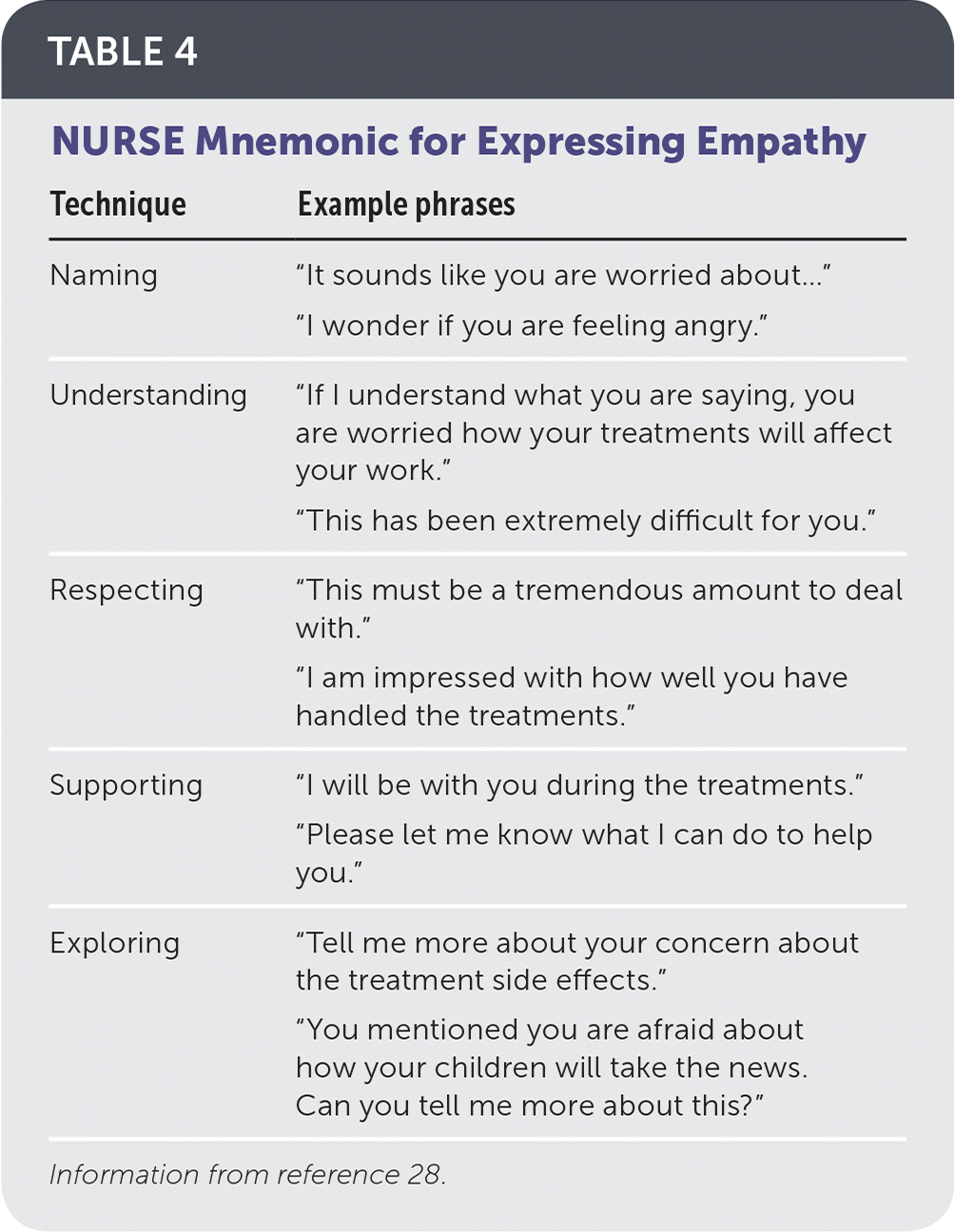
| Technique | Example phrases |
|---|---|
| Naming | “It sounds like you are worried about…” “I wonder if you are feeling angry.” |
| Understanding | “If I understand what you are saying, you are worried how your treatments will affect your work.” “This has been extremely difficult for you.” |
| Respecting | “This must be a tremendous amount to deal with.” “I am impressed with how well you have handled the treatments.” |
| Supporting | “I will be with you during the treatments.” “Please let me know what I can do to help you.” |
| Exploring | “Tell me more about your concern about the treatment side effects.” “You mentioned you are afraid about how your children will take the news. Can you tell me more about this?” |
Information from reference 28.
STRATEGY AND SUMMARY
Physicians should provide a summary, explore options, and determine patient-specific goals. Even with the worst prognosis, most patients prefer to know what is coming next.29 Follow-up should include the patient's next appointment and a way for the patient or family to contact the physician with questions. A second appointment in the next few days may be useful to review the bad news and to answer questions. A discussion of treatment options may be appropriate at that time, or it may be delayed, depending on patient preference. Physicians should avoid the phrase “I'm afraid there is nothing more we can do for you.” This leaves the patient feeling helpless and abandoned. Instead, in the absence of cure, the focus should be on defining and supporting the patient's redefined hopes (e.g., less pain, more time with family). Patients should be assured that the physician will be with them and support them.
Future Education
Despite marked advancements in medicine, not all patients can be cured. Skillful delivery of bad news can provide comfort for the patient and family. Communications courses,30 standardized patient scenarios,31 and interactive computer courses32 have all demonstrated improvement in physician communication skills. Education can improve a physician's skill in delivering bad news, but research has yet to document improved patient outcomes. Current algorithms and guidelines are not considered evidence-based,33 but increased research in the field continues to improve physician guidance with this difficult task.
This article updates a previous article on this topic by VandeKieft.29
Data Sources: A PubMed search was completed in Clinical Queries using the key terms bad news and communicating bad news. The search included meta-analyses, randomized controlled trials, clinical trials, and reviews. We also searched Essential Evidence Plus. Search date: March 22, 2017.

