A 57-year-old man presented with an ulcer on his upper lip that had been present for approximately two weeks. It was mildly painful and initially oozed honey-colored fluid. He did not recall any blisters or vesicles, and there was no trauma to the area. His history was significant for chlamydia, genital herpes, and well-controlled human immunodeficiency virus (HIV) infection, with a recent CD4 cell count of 426 mm3 (0.43 × 109 per L) and an HIV-RNA level of less than 20 copies per mL. Five years earlier, he was treated with three weekly injections of intramuscular penicillin G benzathine for late latent syphilis. He reported having one regular male sex partner.
He had no recent fevers, oral pain, rhinorrhea, rashes, genital sores, or swollen glands. Physical examination revealed a crusted ulcer (Figure 1) without surrounding induration or tenderness on palpation. He was afebrile and well appearing. He did not have intraoral ulcers or cervical lymphadenopathy.
FIGURE 1
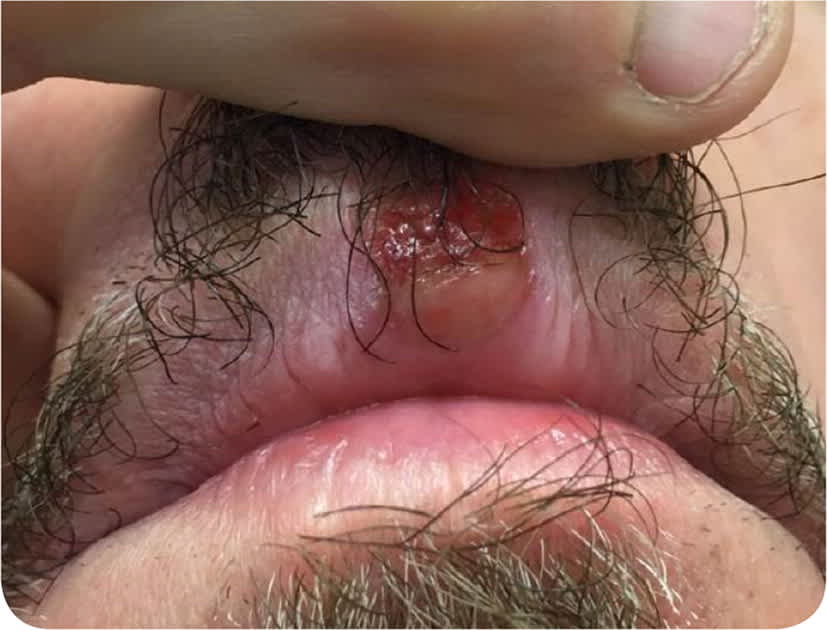
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Aphthous ulcer.
B. Chancroid.
C. Herpes labialis.
D. Pemphigus vulgaris.
E. Primary syphilis.
Discussion
The answer is E: primary syphilis. The primary syphilis ulcer (chancre) is caused by the spirochete Treponema pallidum. The chancre is found on the genitals in 77% of primary syphilis cases and is sometimes associated with painless regional lymphadenopathy.1 An atypical presentation with multiple ulcers is more common in those with HIV infection.2,3 Syphilis can be transmitted via oral, genital, or anal sex.1–3 Primary syphilis can be diagnosed with dark-field microscopy, but this is not available at most clinical sites.
A definitive diagnosis requires a nontreponemal test (e.g., a titer from rapid plasma reagin test, the Venereal Disease Research Laboratory test) and a treponemal test (fluorescent treponemal antibody absorption or the T. pallidum passive particle agglutination test). The nontreponemal test helps guide treatment, and the treponemal test confirms the diagnosis and avoids a false-positive result.4
In this patient, the treponemal test result would have been positive because of the prior infection and was thus not repeated. A rapid plasma reagin test performed six months earlier was nonreactive, indicating that the patient's antibody titers were below the level of detection. On presentation, his rapid plasma reagin test was reactive, with a titer of 1:32.
Aphthous ulcers, or canker sores, are common oral mucosal lesions. Their etiology is unknown, but they cause significant morbidity, especially in immunocompromised patients. One or several discrete, painful, shallow, circular ulcers are visible on the oral mucosa but not on the lips at the vermilion border.5
Chancroid is a sexually transmitted infection caused by the gram-negative bacterium Haemophilus ducreyi. It is characterized by necrotizing genital ulcerations accompanied by inguinal lymphadenitis. The tender lymph nodes typically progress to abscesses. The ulcers are painful and have an erythematous base and ragged edges. Although lesions can occur orally at the site of inoculation, they most commonly occur on the penis in men and on the labia or the introitus or perianal area in women.6
Herpes labialis is caused by herpes simplex virus 1 or 2 and presents as vesicular lesions at the vermilion border of the lips. The lesions are typically painful and rarely coalesce to form a significant single ulceration.7
Pemphigus vulgaris often presents as multiple irregularly shaped, painful ulcers on the oral mucosa.8 Rapid progression to ulceration is common.
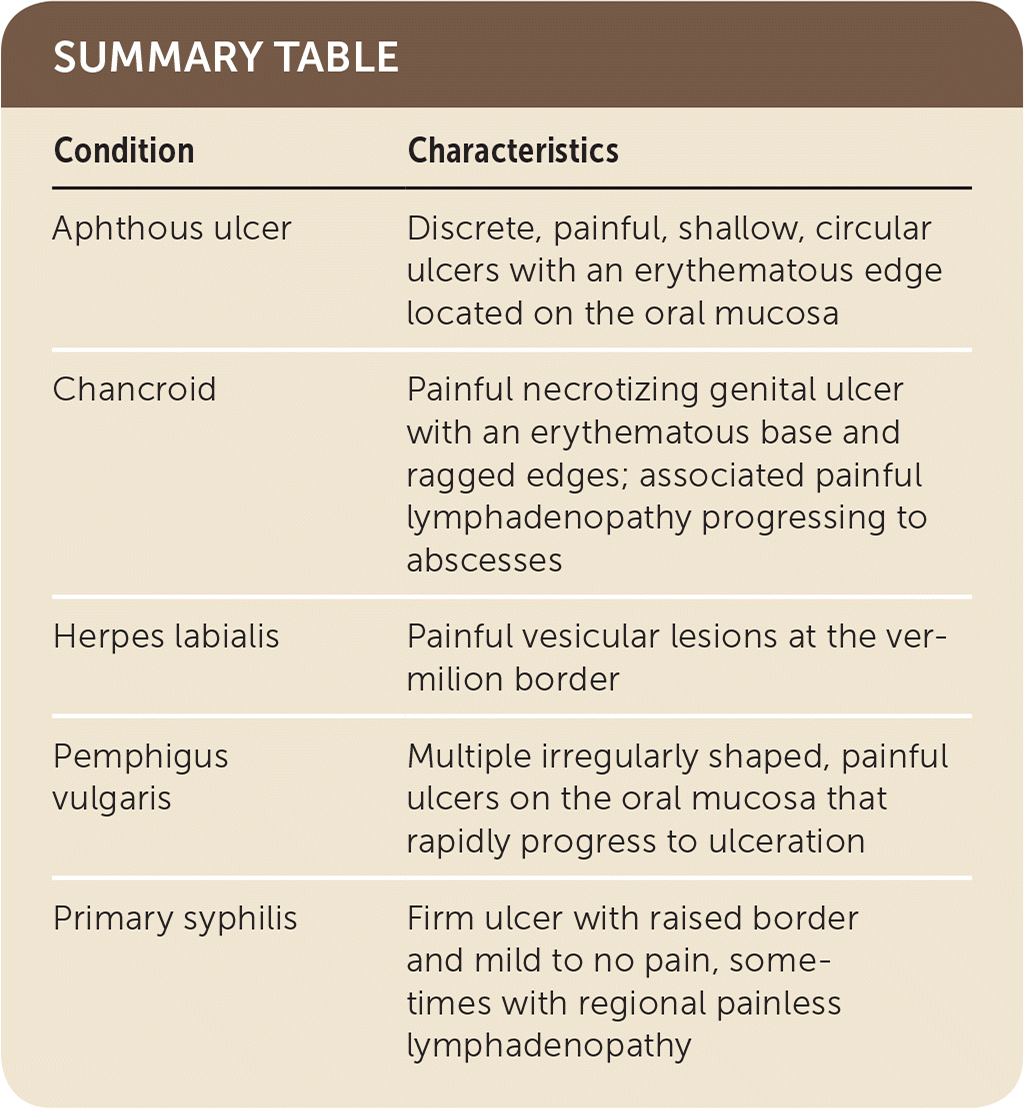
SUMMARY TABLE
| Condition | Characteristics |
|---|---|
| Aphthous ulcer | Discrete, painful, shallow, circular ulcers with an erythematous edge located on the oral mucosa |
| Chancroid | Painful necrotizing genital ulcer with an erythematous base and ragged edges; associated painful lymphadenopathy progressing to abscesses |
| Herpes labialis | Painful vesicular lesions at the vermilion border |
| Pemphigus vulgaris | Multiple irregularly shaped, painful ulcers on the oral mucosa that rapidly progress to ulceration |
| Primary syphilis | Firm ulcer with raised border and mild to no pain, sometimes with regional painless lymphadenopathy |

