Most foot disorders do not require podiatry referral or complex interventions. After the clinical diagnosis is made, these conditions can typically be managed with over-the-counter (OTC) and home remedies, with guidance from the primary care physician. Stretching and strengthening exercises, along with the use of heel cups, resolve most plantar fasciitis cases and are at least as effective as nonsteroidal anti-inflammatory drugs or steroid injections. Hallux rigidus is best managed with a hard-soled shoe or rigid insert that relieves pain by restricting motion across the metatarsophalangeal joint. Hallux valgus responds to use of wide toe box shoes, and surgery is not clearly beneficial beyond one year. Plantar warts can be treated effectively at home with OTC salicylic acid and cryotherapy topical agents, which have equal effectiveness to liquid nitrogen. In patients with corns and calluses, OTC topical salicylic acid has short-term benefits, and pads and inserts that more evenly redistribute contact forces have long-term benefits. Inserts are commonly recommended to redistribute forefoot pressure and relieve pain. Several OTC preparations are available for the treatment of tinea pedis, with topical allylamines being the most effective. Although OTC topical treatments have been widely used for onychomycosis, they have poor long-term cure rates compared with prescription oral medications.
Foot pain reportedly affects 30% of the general population.1 In addition to causing pain and inconvenience, some foot problems are associated with disability and fall-related morbidity.2 Many common foot ailments do not require podiatry referral or complex interventions and are best managed with appropriate over-the-counter (OTC) treatments and home care, with careful guidance from the family physician.
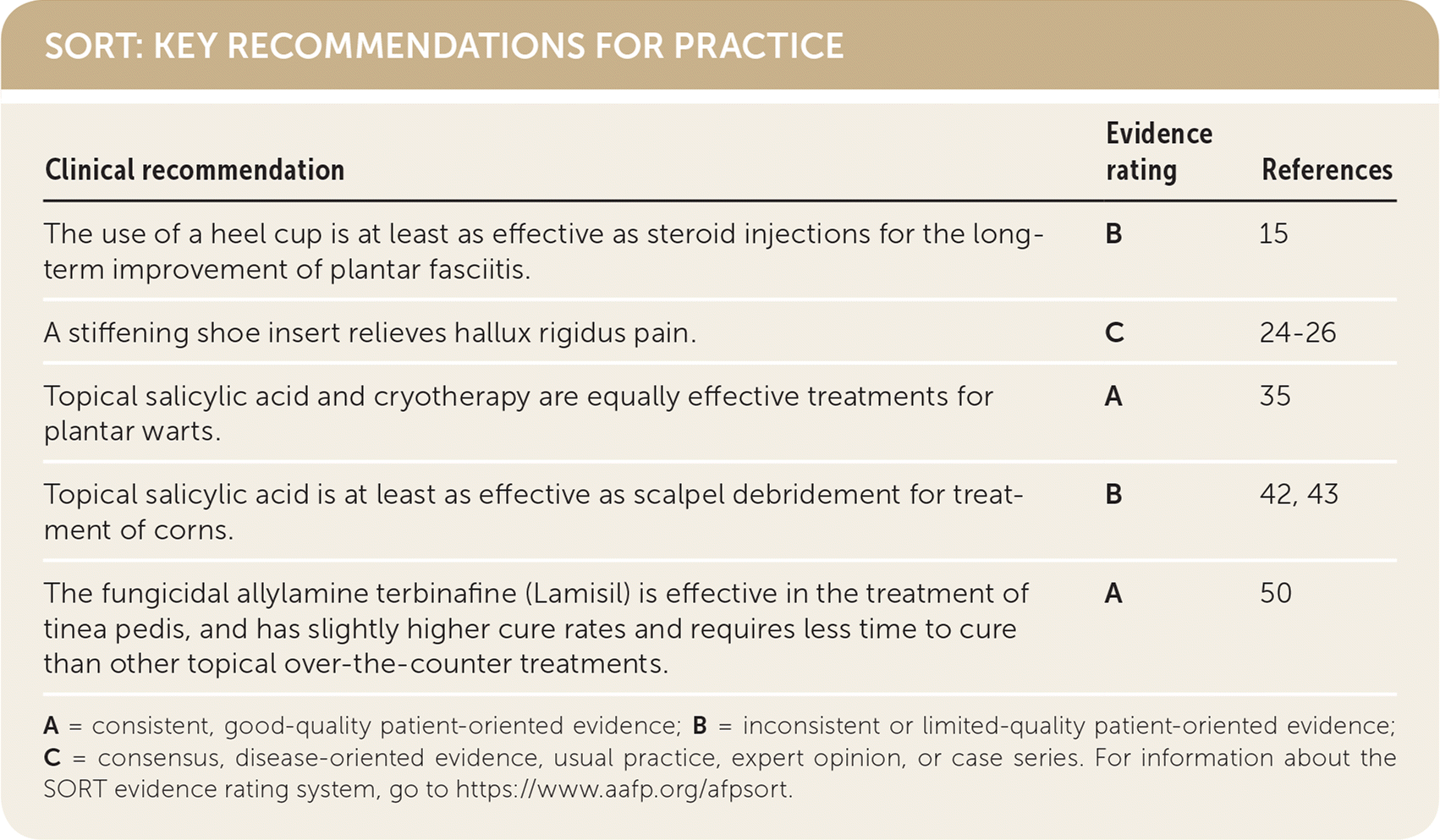
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| The use of a heel cup is at least as effective as steroid injections for the long-term improvement of plantar fasciitis. | B | 15 |
| A stiffening shoe insert relieves hallux rigidus pain. | C | 24–26 |
| Topical salicylic acid and cryotherapy are equally effective treatments for plantar warts. | A | 35 |
| Topical salicylic acid is at least as effective as scalpel debridement for treatment of corns. | B | 42, 43 |
| The fungicidal allylamine terbinafine (Lamisil) is effective in the treatment of tinea pedis, and has slightly higher cure rates and requires less time to cure than other topical over-the-counter treatments. | A | 50 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Plantar Fasciitis
Each year, more than 800,000 Americans younger than 65 years seek outpatient treatment of plantar fasciitis.3 In 80% of plantar fasciitis cases, symptoms resolve with OTC and home therapies alone, most often within six months of commencing treatment.4 Those who seek care within 12 months of onset are more likely to have resolution of symptoms.4 Many therapies address biomechanical and environmental factors, such as a reduced angle of ankle dorsiflexion, prolonged standing for work, and obesity.5 Stretching is likely effective because it counteracts shortening of the plantar fascia. The plantar fascia is contiguous with the Achilles tendon at its origin, where it then goes on to insert at the toes in individual bands.6,7 The plantar fascia is also vulnerable to compressive trauma at the base of the calcaneus, where it is protected only by a fat pad that thins with age.8
There may be benefit to adding plantar fascia stretches (Figure 1) to the commonly used Achilles stretching regimen.9 However, a systematic review found a lack of evidence to support any stretching over placebo.10 A randomized controlled trial found that plantar fascia strengthening exercises (Figure 2) are superior to other stretching exercises for pain and function in the short term, but there were no differences between the groups at six and 12 months.11 A 2017 systematic review found low-quality evidence to support strengthening exercises for plantar fasciitis, although it is unclear if all strengthening regimens have comparable benefits.12
FIGURE 1
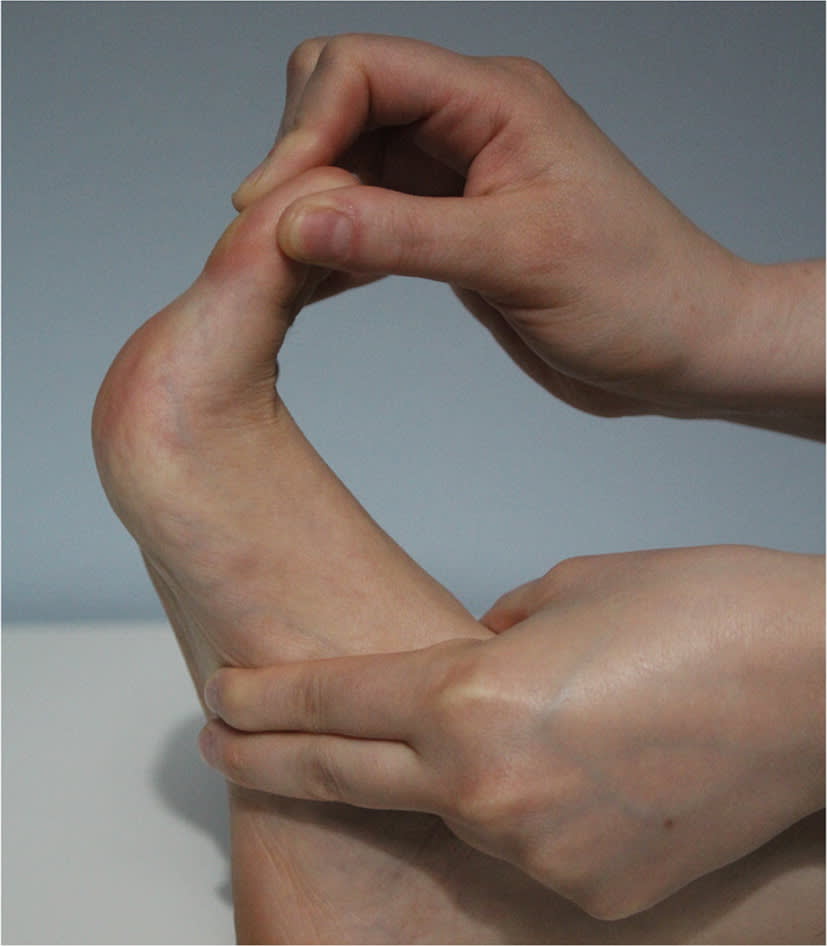
Plantar fascia stretch. The patient confirms effectiveness of the stretch by palpating a taut plantar fascia.
FIGURE 2
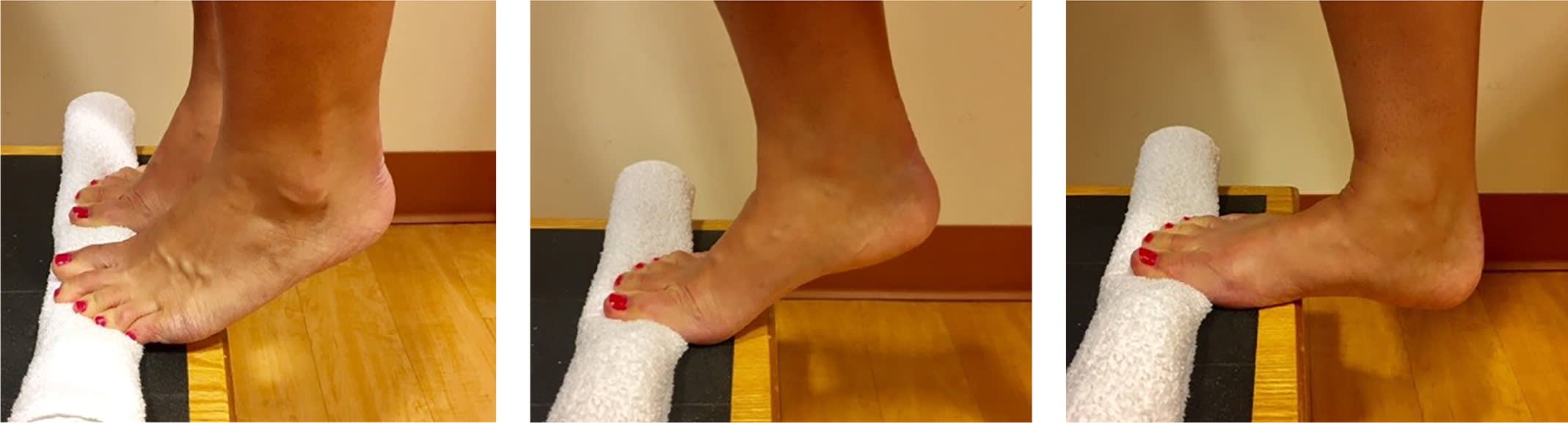
Heel drop exercises focus on eccentric strengthening for plantar fasciitis. Body weight is raised with both feet, then lowered slowly on the affected foot.
It is likely that plantar fasciitis does not result from inflammation, but instead from repetitive microtears in the contracted fascia.13 The lack of an inflammatory mechanism could explain why nonsteroidal anti-inflammatory drugs (NSAIDs) do not appear to be helpful and why OTC remedies such as heel cups are at least as effective as steroid injections.14,15 A recent Cochrane review found that steroid injections are marginally more effective than placebo in reducing pain, but only for one month.16 Steroid injections also carry risks such as fascial rupture, infection, and atrophy of the fat pad.
OTC shoe inserts are as effective as custom orthotics for improving plantar fasciitis pain.17,18 Night splints, another OTC remedy for plantar fasciitis, may be beneficial only if both the ankle and toes are dorsiflexed.19,20
Hallux Rigidus
Hallux rigidus (Figure 3) is common, affecting more than 40% of men and 50% of women by their early 70s. Significant hallux rigidus will develop in 20% of persons by their early 40s.21 Hallux rigidus presents as joint pain, swelling, and progressive limitation of motion in the great toe, often as a result of osteoarthritis in the metatarsophalangeal (MTP) joint. As the condition advances, acute flare-ups become more frequent and severe,22 and they are sometimes mistaken for gout.
FIGURE 3
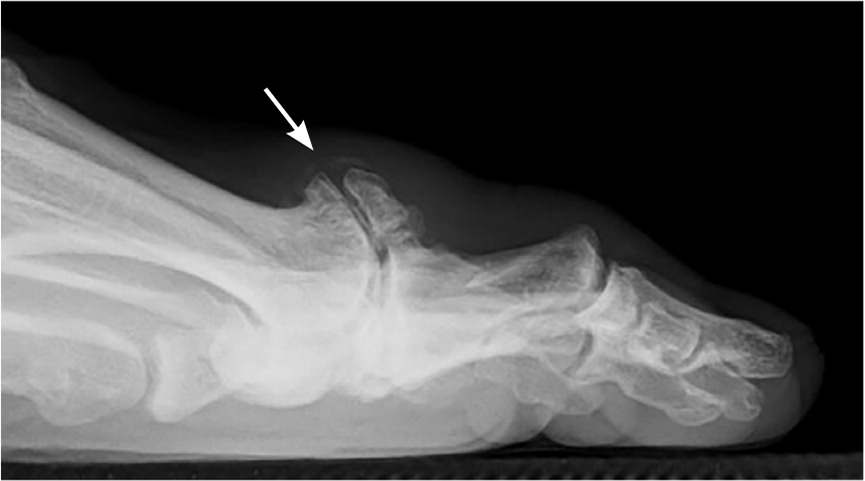
Lateral radiograph of the left foot showing osteoarthritic changes at the first metatarsophalangeal joint (arrow) that are common with hallux rigidus.
A large retrospective analysis suggests that hallux rigidus symptoms usually improve without surgery.23 Although few studies have compared OTC inserts with custom orthotics, rigid inserts and hard-soled shoes relieve pain by restricting motion across the MTP joint.24,25 Adding an OTC stiffening shoe insert may improve pain and function for three months or longer.26 The use of modified footwear is more effective than NSAIDs.27 Although some experts recommend using a curved sole, or rocker-bottom shoe, to reduce motion at the MTP joint, its effectiveness has not been studied.
Hallux Valgus
Hallux valgus is known for the characteristic bunion deformity at the first MTP joint (Figure 4), which can lead to osteoarthritis of the joint. It is more prevalent in women, occurring in 26% of women 18 to 65 years of age and in 36% of those older than 65 years.28 Wearing restrictive shoes is the main risk factor for hallux valgus,29 and thus wearing shoes with a wide toe box is a common treatment to relieve compressive forces at the valgus deformity. Many shoemakers will stretch shoes for a fee to accommodate larger bunions. Although low-quality evidence suggests that surgery is beneficial for pain and function at 12 months, it is no better than orthoses or placebo after two years.30 There is no evidence that OTC night splints and interdigital pads correct bunion deformities or affect pain or function.31
FIGURE 4
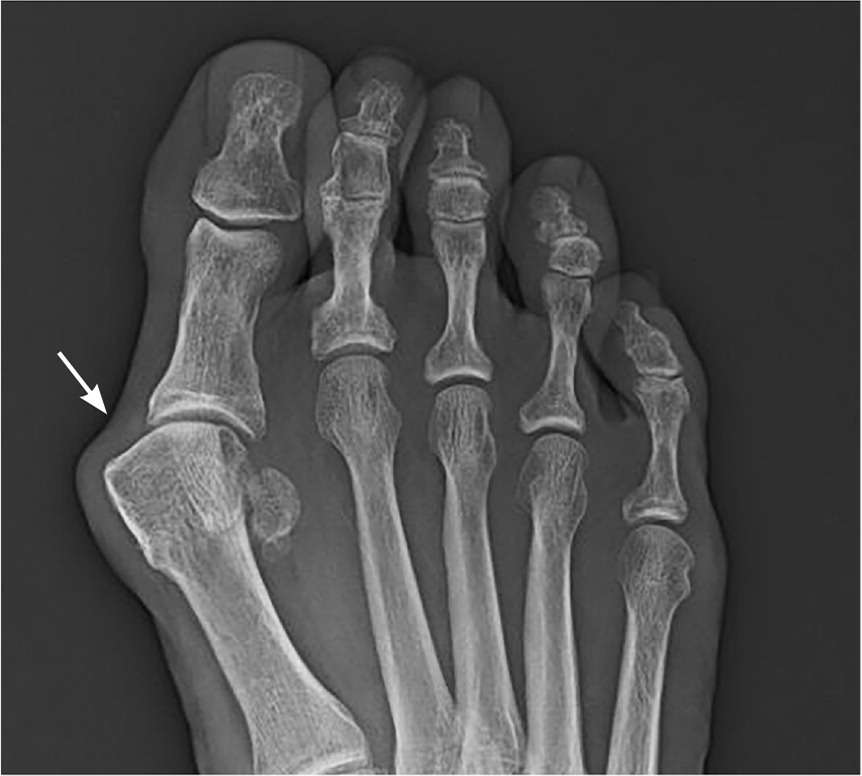
Anteroposterior radiograph of the right foot showing a hallux valgus deformity (arrow).
Plantar Warts
Viral plantar warts are most common in childhood, affecting 20% of children four to 12 years of age.32 Two-thirds of these lesions will resolve spontaneously within two years.33 Treatments aim to mobilize an immune response by irritating wart cells affected by the human papillomavirus. The rate of resolution and response to therapy may be affected by which human papillomavirus strain is involved.34
A Cochrane review found good evidence that salicylic acid is effective for the treatment of plantar warts. Although there was no clear benefit of cryotherapy over placebo, cryotherapy and salicylic acid were equally effective when compared with one another. Long-term outcomes of cryotherapy did not change if patients had repeat cryotherapy at two-, three-, or four-week intervals. Two randomized controlled trials evaluating application of duct tape showed it to be no better than placebo for wart treatment.35
There are numerous inexpensive OTC salicylic acid agents on the market. A small randomized controlled trial showed that zinc oxide had similar effectiveness to salicylic acid.36 Although studies testing cryotherapy typically use liquid nitrogen, cryotherapy agents such as dimethyl ether and propane are now available OTC. A randomized controlled trial showed that liquid nitrogen and dimethyl ether and propane have equal effectiveness, with more than 90% of patients achieving cure regardless of which treatment they received.37
Corns and Calluses
Corns and calluses are hyperkeratotic conditions that result from stimulation of the epidermis through increased pressure or friction. These changes can be caused by external factors such as shoes and repetitive movements, or internal factors such as hallux valgus or hammer toe deformities.38 Treatment of these sometimes painful lesions focuses on the redistribution of forces to allow the skin to heal.39 Remedies range from simple solutions such as modified footwear to more specific remedies such as pads, sleeves, and splints.40
Although there is little evidence regarding these treatments, there are general rules that can be helpful in guiding OTC treatments and home care. Assessment for ill-fitting shoes or wear patterns can allow for appropriate changes in shoes or insoles. This is more likely to aid against recurrence, whereas short-term measures can produce quicker relief of symptoms. Donut pads and metatarsal bars are commonly used to redistribute contact forces away from a lesion. Inserts and customized shoes and orthotics vary widely, precluding universal recommendations.41 Salicylic acid solutions to soften hyperkeratotic lesions are available OTC. Studies have compared fitted salicylic acid plasters to more aggressive treatments such as scalpel debridement. Specific outcomes vary, but all patients typically have notable improvement, suggesting that self-care with OTC solutions is beneficial.42,43
Metatarsal Pain
Forefoot pain can be associated with numerous diagnoses, such as metatarsalgia and Morton neuroma. OTC shoe inserts are commonly recommended to redistribute forefoot pressure and relieve pain. Evidence supporting the effectiveness of orthotics or inserts for foot pain is generally lacking, with the exception of persons with pes cavus, juvenile idiopathic arthritis, and rheumatoid arthritis.44 Metatarsal pads were shown to relieve pain in a recent small cohort study, with roughly one-half of patients continuing to use them after one year.45 Among runners, the addition of an insert may be less effective in achieving comfort than simple cushioning of the forefoot.46 No further benefit has been shown with the addition of magnetic material to insoles or orthotics.47
Despite the large market for OTC inserts and custom orthotics, estimated to reach sales of $3.6 billion by 2021,48 there is little outcome-based evidence to support specific recommendations for these products. General recommendations for improving shoe fit and comfort (Table 149 ) may be the most helpful in preventing and managing forefoot conditions.
TABLE 1 Guidelines for Proper Shoe Fit to Avoid Foot Problems

| Properly fitted shoes do not need to be broken in, and instead should be comfortable to wear right out of the box. |
| Shoes should be fitted on both feet during weight bearing, preferably at the end of the day when the feet are most swollen. |
| Allow a space of 1/2 inch between the end of the shoe and the longest toe. For athletic shoes, allow up to 1 inch. |
| Check the width. Adequate room should be allowed across the ball of the foot. The first metatarsophalangeal joint should be in the widest part of the shoe. |
| The heel should fit snugly. |
| Check the fit over the instep. A shoe that laces allows for adjustment of this area. |
| Orthotics and inserts will change the fit of shoes. Shoes should be fitted while wearing the orthotic. |
Adapted with permission from Bedinghaus JM, Niedfeldt MW. Over-the-counter foot remedies. Am Fam Physician. 2001;64(5):791.
Tinea Pedis
The prevalence of tinea pedis, or athlete's foot, may be as high as 50% to 80% in some populations.50 OTC treatments include fungistatic treatments (e.g., miconazole, clotrimazole, tolnaftate [Tinactin]) and the fungicidal allylamine terbinafine (Lamisil). Older treatments such as undecylenic acid, although still available, are less effective. A Cochrane review found that allylamines have slightly higher cure rates and require less time to cure than other topical OTC treatments.50
Onychomycosis
Onychomycosis has an estimated prevalence of 6% to 14% in the general population and is more common in persons with tinea pedis.51,52 Prescription and OTC topical treatments have been widely used but have poor long-term cure rates compared with prescription oral medications.53 There is no clinical support for treating nail infections with the OTC antifungal creams used for tinea pedis. Tea tree oil, topically applied cough suppressants, coniferous resin, and sunflower oil have all been purported to treat onychomycosis. Case series have suggested that these methods are safe,54 but their ultimate effectiveness is uncertain.
This article updates a previous article on this topic by Bedinghaus and Niedfeldt.49
Data Sources: The terms plantar fasciitis, hallux rigidus, hallux valgus, plantar warts, orthotics, metatarsalgia, corns, callosities, tinea pedis, and onychomycosis were searched via PubMed, the Cochrane database, Essential Evidence Plus, and the Agency for Healthcare Research and Quality National Guideline Clearinghouse. Search date: March 28, 2017.

