All major health organizations recommend breastfeeding as the optimal source of infant nutrition, with exclusive breastfeeding recommended for the first six months of life. After six months, complementary foods may be introduced. Most organizations recommend breastfeeding for at least one year, and the World Health Organization recommends a minimum of two years. Maternal benefits of breastfeeding include decreased risk of breast cancer, ovarian cancer, postpartum depression, hypertension, cardiovascular disease, and type 2 diabetes mellitus. Infants who are breastfed have a decreased risk of atopic dermatitis and gastroenteritis, and have a higher IQ later in life. Additional benefits in infants have been noted in observational studies. Clinicians can support postdischarge breastfeeding by assessing milk production and milk transfer; evaluating an infant's latch to the breast; identifying maternal and infant anatomic variations that can lead to pain and poor infant weight gain; knowing the indications for frenotomy; and treating common breastfeeding-related infections, dermatologic conditions, engorgement, and vasospasm. The best way to assess milk supply is by monitoring infant weight and stool output during wellness visits. Proper positioning improves latch and reduces nipple pain. Frenotomy is controversial but may reduce pain in the short term. The U.S. Preventive Services Task Force recommends primary care interventions to support breastfeeding and improve breastfeeding rates and duration.
Breastfeeding is beneficial for both the mother and infant. Although more than 80% of women in the United States initiate breastfeeding, many stop before the recommended 12 to 24 months.1 Any amount of breastfeeding is better than none, and greater benefits accrue with increased duration.2 Postdischarge primary care support for breastfeeding mothers and infants can increase breastfeeding rates and duration.
WHAT IS NEW ON THIS TOPIC: BREASTFEEDING
A 2015 systematic review and meta-analysis of 17 studies found that breastfed infants performed better on intelligence tests later in life than those who were not breastfed, even after controlling for maternal IQ.
The UK Infant Feeding Survey of 2010 found that concerns about insufficient milk supply (31%), inadequate latch (19%), and painful nipples or breasts (12%) were the top three reasons women stopped breastfeeding.
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
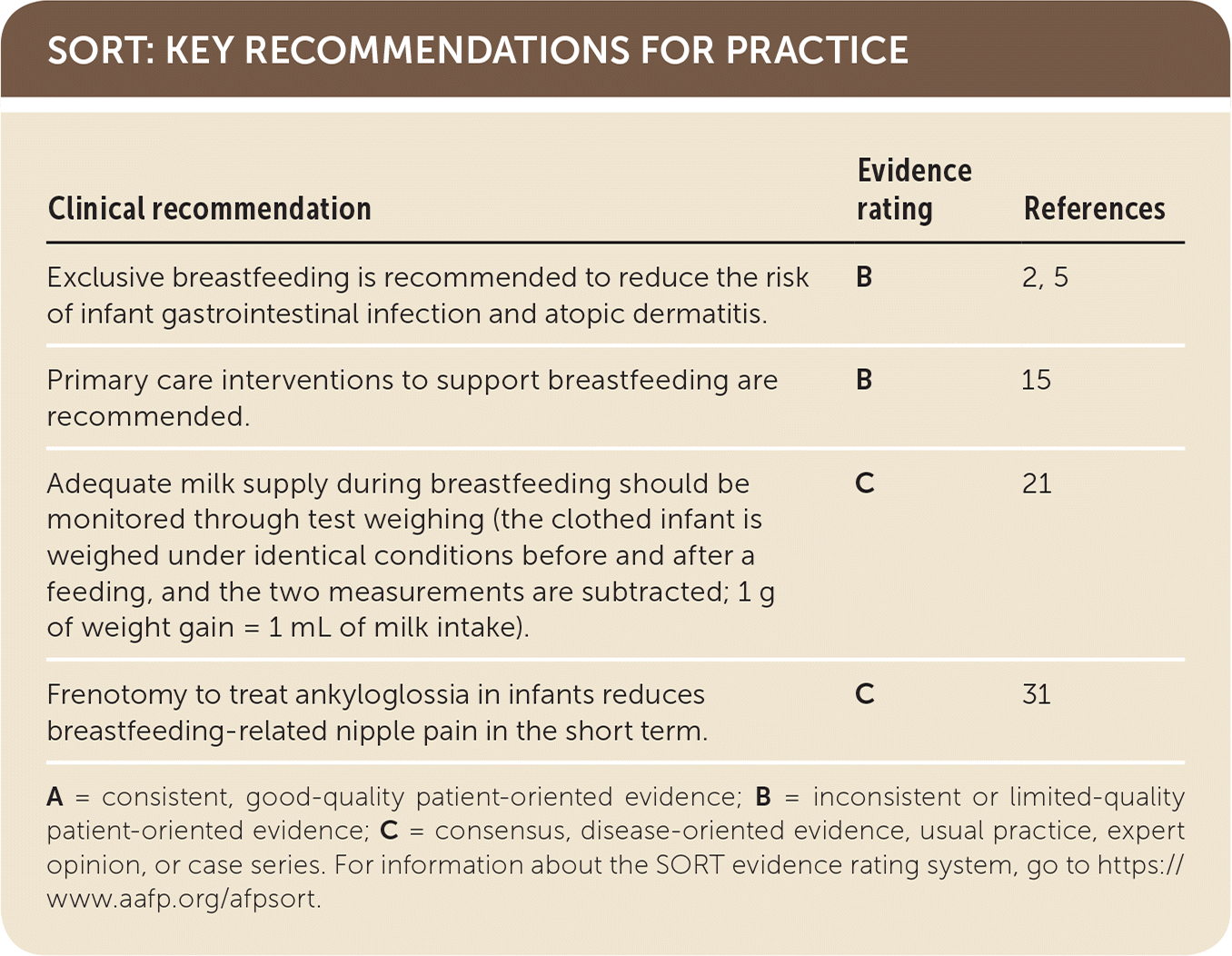
| Exclusive breastfeeding is recommended to reduce the risk of infant gastrointestinal infection and atopic dermatitis. | B | 2, 5 |
| Primary care interventions to support breastfeeding are recommended. | B | 15 |
| Adequate milk supply during breastfeeding should be monitored through test weighing (the clothed infant is weighed under identical conditions before and after a feeding, and the two measurements are subtracted; 1 g of weight gain = 1 mL of milk intake). | C | 21 |
| Frenotomy to treat ankyloglossia in infants reduces breastfeeding-related nipple pain in the short term. | C | 31 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
BEST PRACTICES IN NEONATOLOGY

| Recommendation | Sponsoring organization |
|---|---|
| Do not separate mothers and newborns at birth unless medically necessary. Instead, help the mother to place her newborn in skin-to-skin contact immediately after birth and encourage her to keep her newborn in her room during hospitalization after the birth. | American Academy of Nursing |
Source: For more information on the Choosing Wisely Campaign, see http://www.choosingwisely.org. For supporting citations and to search Choosing Wisely recommendations relevant to primary care, see https://www.aafp.org/afp/recommendations/search.htm.
What Are the Infant and Maternal Benefits of Breastfeeding?
Infant benefits include decreased risk of atopic dermatitis and gastroenteritis, as well as higher IQ later in life. Maternal benefits include decreased risk of breast cancer, ovarian cancer, cardiometabolic disease (type 2 diabetes mellitus, hypertension, and cardiovascular disease), and postpartum depression. Table 1 lists the benefits of breastfeeding.2–5
TABLE 1. Maternal and Infant Health Benefits of Breastfeeding

| Maternal health benefits |
| Decreased risk of breast and ovarian cancers, cardiometabolic disease (type 2 diabetes mellitus, hypertension, cardiovascular disease), and postpartum depression |
| Infant health benefits |
| Decreased risk of atopic dermatitis and intestinal gastroenteritis |
| Higher IQ later in life |
| Potential infant health benefits based on cohort studies |
| Decreased risk of childhood leukemia, hypertension, necrotizing enterocolitis, obesity, otitis media, respiratory illnesses such as asthma, severe lower respiratory infections, sudden infant death syndrome, and types 1 and 2 diabetes |
EVIDENCE SUMMARY
The Promotion of Breastfeeding Intervention Trial (PROBIT), including more than 17,000 breastfeeding mothers randomized to increased breastfeeding support or standard care, showed significantly fewer episodes of gastrointestinal infections and atopic dermatitis in the increased support group.2,5 A follow-up study demonstrated that those who were breastfed had a 5.9-point higher IQ overall later in life than those who were not breastfed.3 A meta-analysis that included PROBIT also found higher IQs in children who were breastfed compared with those who were not.4 The PROBIT did not find that breastfeeding protects infants against respiratory tract infections, obesity, or hypertension. Cohort studies support other potential benefits of breastfeeding but are based on observational trials.5
A systematic review of prospective cohort and case-control studies suggests that breastfeeding decreases the risk of type 2 diabetes, breast cancer, and ovarian cancer in mothers. The study also showed an increased risk of postpartum depression in mothers who did not breastfeed or who breastfed for less than six months.5,6
How Long Should Mothers Breastfeed?
All major health organizations recommend exclusive breastfeeding for the first six months of life. After six months, complementary foods may be introduced with continued breastfeeding until at least 12 months of age; the World Health Organization recommends breastfeeding for at least 24 months.6–8 For those at high risk of peanut allergy, introduction of solid foods containing peanuts may be considered at four to six months. Breastfeeding beyond six months may provide additional benefits to the infant, such as decreased risk of respiratory illnesses, including asthma, and decreased risk of obesity, although the data are insufficient to support these benefits.
EVIDENCE SUMMARY
The World Health Organization's 2001 recommendation for six months of exclusive breastfeeding is based on a systematic review that included two Honduran randomized controlled trials showing an increase in lactational amenorrhea, increased postpartum weight loss, and decreased infant morbidity and mortality from gastrointestinal illnesses.8 A Cochrane review including two randomized controlled studies and 18 other nonrandomized studies demonstrated that exclusive breastfeeding for six months was more beneficial than just three to four months of exclusive breastfeeding or mixed breastfeeding (some breastfeeding and some formula) based on decreased risk of infant gastrointestinal illnesses, more rapid maternal weight loss, and longer lactational amenorrhea.9
Although most infants should be exclusively breastfed for six months,10 based on recent studies, infants with a high risk of peanut allergy may benefit from introduction of foods containing peanuts at four to six months of age.11
What Strategies Can Be Used to Assist Women in Initiating and Continuing Breastfeeding?
Skin-to-skin contact at birth, early initiation of breastfeeding, lactation support, the Baby-Friendly Hospital Initiative (BFHI), breastfeeding education, and following professional recommendations are important for the initiation and continuation of breastfeeding. Professional, face-to-face support is better than telephone or layperson support.12
EVIDENCE SUMMARY
Infants who have skin-to-skin contact at birth are more likely to breastfeed longer and more effectively.13 It is well documented that offering any breastfeeding support to mothers increases the duration and exclusivity of breastfeeding.14 In 2016, the U.S. Preventive Services Task Force concluded that primary care interventions can be more effective than usual care in increasing short- and long-term breastfeeding rates.15
Face-to-face support strategies are significantly more successful than telephone contacts in preventing breastfeeding cessation.12 The BFHI has been shown to increase initiation of breastfeeding in the hospital; however, these rates are not sustained after discharge.15,16 The BFHI combined with home-visit support increases breastfeeding duration compared with the BFHI alone.15,16 A systematic review showed that professional support, such as from physicians and nurses trained in lactation support, lactation counselors, and lactation consultants, is beneficial in prolonging breastfeeding.12 The U.S. Preventive Services Task Force found that layperson support significantly increases the rate of any breastfeeding and exclusive breastfeeding in the short term; however, a systematic review showed a nonsignificant reduction in breastfeeding cessation.12,15
What Are the Most Common Breastfeeding Problems?
The most common factors leading to cessation of breastfeeding are insufficient milk supply, inadequate latching, and painful nipples or breasts.17–19
EVIDENCE SUMMARY
According to a survey in the United Kingdom, up to 81% of mothers initiated breastfeeding at birth; however, the rate dropped to 42% by six months, and 71% of breastfeeding mothers reported a concern with breastfeeding.17 This is comparable to data in the United States showing 81.1% of capable women initiate breastfeeding, 51.8% continue for six months, and 30.7% continue for 12 months.1 In the UK survey, the top three reasons why women discontinued breastfeeding were concerns about insufficient milk supply (31%), inadequate latching (19%), and painful nipples or breasts (12%).20
What Is the Best Way to Assess for an Insufficient Milk Supply?
The best way to assess milk supply is by monitoring infant weight through test weighing and measuring stool output during wellness visits. This distinguishes between true and perceived milk insufficiency. Clinicians should accurately assess milk supply before recommending supplementation, and age-appropriate volumes should be used for supplementation if implemented.21,22 Supplementation can decrease breast milk production if the mother is not educated on the indications for supplementation, age-appropriate volumes, and how to maintain her milk supply. Perceived insufficiency can be managed with patient education, support, and reassurance.
EVIDENCE SUMMARY
Milk supply is dependent on adequate breast stimulation and sufficient removal of milk from the breast. A fussy infant and smaller, less full breasts are not necessarily associated with low supply. Perceived insufficiency often leads to unnecessar y supplementation with formula. Test weighing is recommended to determine the amount of milk transferred to the infant during a feeding.21 It is performed by weighing the clothed infant under identical conditions before and after a feeding, then subtracting the prefeeding weight from the postfeeding weight. It is estimated that 1 g of weight gain is equivalent to 1 mL of milk intake.21 Table 2 includes normal milk intake and stooling patterns for breastfed infants.23,24
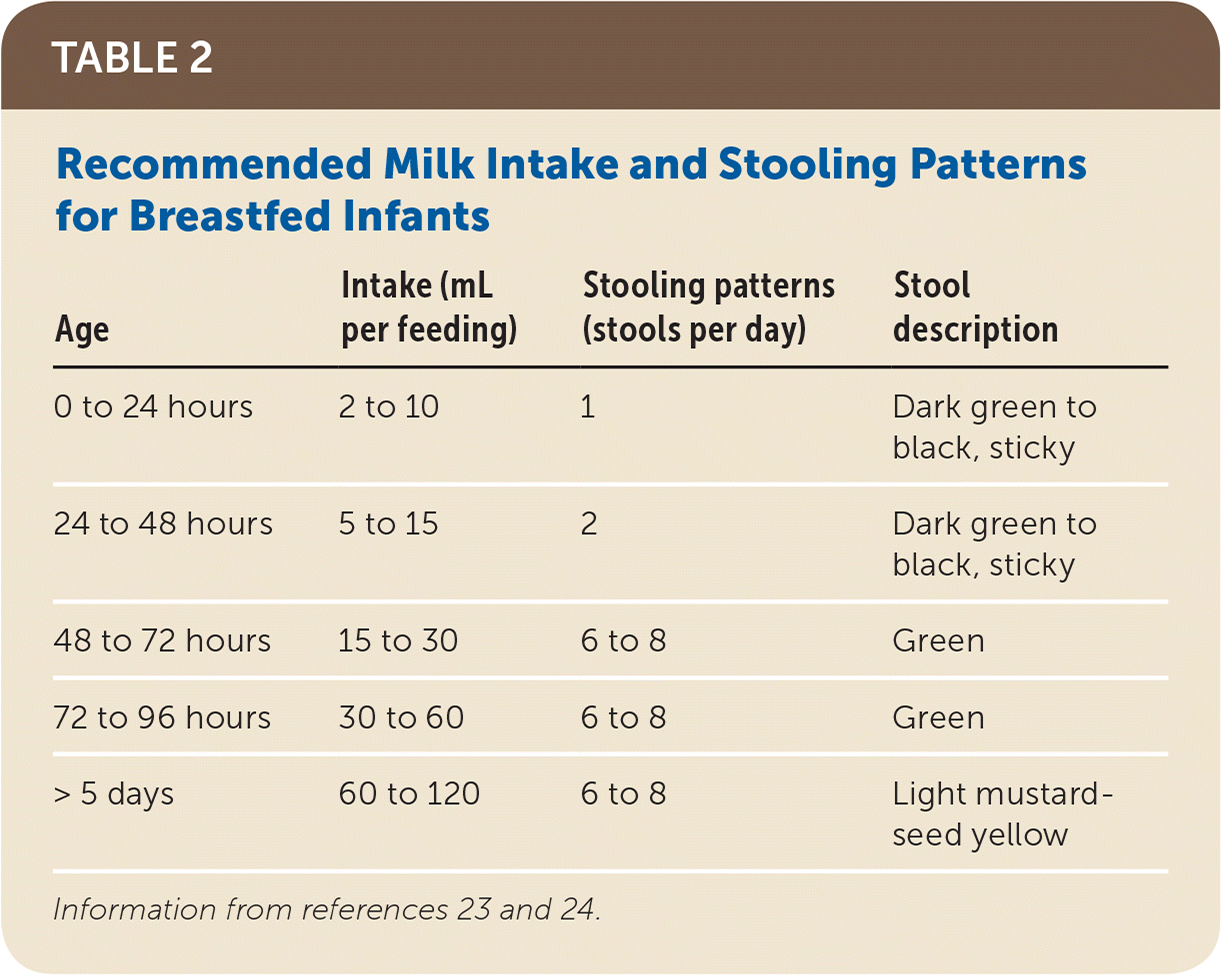
TABLE 2. Recommended Milk Intake and Stooling Patterns for Breastfed Infants
| Age | Intake (mL per feeding) | Stooling patterns (stools per day) | Stool description |
|---|---|---|---|
| 0 to 24 hours | 2 to 10 | 1 | Dark green to black, sticky |
| 24 to 48 hours | 5 to 15 | 2 | Dark green to black, sticky |
| 48 to 72 hours | 15 to 30 | 6 to 8 | Green |
| 72 to 96 hours | 30 to 60 | 6 to 8 | Green |
| > 5 days | 60 to 120 | 6 to 8 | Light mustard-seed yellow |
Another method for evaluating adequate milk supply is assessing feedings, pumping, and infant stooling and voiding patterns. Newborns normally feed 10 to 12 times per day. Stools are initially dark green to black and sticky. Newborns should have at least one stool in the first 24 hours and two stools within the first 48 hours, and then increase to the typical six to eight stools per day by day 3 when the stools change to a green color. Stools become characteristically light mustard-seed yellow around day 5 to 7.
During the first 24 hours, healthy full-term newborns require about 6 mL of breast milk per feeding. They need about 30 mL per feeding by day 3 and about 60 mL per feeding by day 5.23,24 Newborns should gain about 105 to 210 g per week (15 to 30 g per day).23,24 If these milestones are not met, clinicians should recognize signs of ineffective breastfeeding. These signs include the following21:
- Infant weight loss of more than 7%
- Continued infant weight loss after three days of life
- No audible swallowing while feeding
- Fewer than six wet diapers per day after four days of life
- Fewer than three stools per day after four days of life
- Minimal maternal breast changes (absence of heaviness, leaking of milk) by the fifth day postpartum
- Maternal nipple pain that persists past the initial 30 seconds to one minute after latching
If the milk supply is low, delayed lactogenesis or, rarely, failed lactogenesis II should be considered. Lactogenesis is a stage between 32 and 96 hours postpartum marked by an increase in lactose secretion in the milk, increase in milk volume, and change in viscosity to a thinner, more watery consistency. Delayed or failed lactogenesis may require additional evaluation and treatment.21 For medically necessary formula supplementation, the Academy of Breast-feeding Medicine protocol for supplementation should be used.
What Are Ways to Ensure an Adequate Latch?
Making sure that mothers are comfortable and can properly position their infants is essential to achieving a comfortable latch that adequately transfers milk. Mothers may need to try a variety of positions to achieve an effective latch. If the mother and infant are positioned properly with a good latch, pain from breastfeeding should improve. If pain does not improve, evaluation for ankyloglossia may be considered. Ankyloglossia is characterized by a short, thickened, or abnormally tight lingual frenulum that limits the infant's range of tongue movement. Treatment with frenotomy has been shown to decrease pain in the short term.
EVIDENCE SUMMARY
Positioning of the infant and a good latch during breastfeeding are important to promote oxytocin and prolactin release, facilitating milk production. 25 The infant's head and body should be facing the body of the mother, and the infant's neck should not be hyperextended or flexed to reach the nipple. The nipple should be guided toward the roof of the infant's mouth, filling the mouth with as much of the areola as possible. There should be 3 to 4 cm of breast tissue in the infant's mouth.26 Videos on achieving a good latch are available at https://www.youtube.com/watch?v=W5X1Dyzmf0Y and https://www.youtube.com/watch?v=kojUf0f4qGg. Table 3 lists signs of good positioning and latch.26,27
TABLE 3. Signs of Good Positioning and Latch for Successful Breastfeeding

| The infant's nose is free from the breast |
| The infant's chin is pressed against the breast |
| The infant's cheeks are rounded, not sunken in or dimpled |
| The infant's mouth is open wide like a yawn |
| If any areola is visible, more is seen above the infant's top lip, with little to none showing near the chin |
| The infant's lower lip is flanged outward |
| The infant's body is in line with the head and facing toward the mother (“tummy to tummy”) |
| Feeding is not painful to the mother after the initial 30 seconds to one minute after latching |
| The infant has a rhythmic suck and swallow pattern |
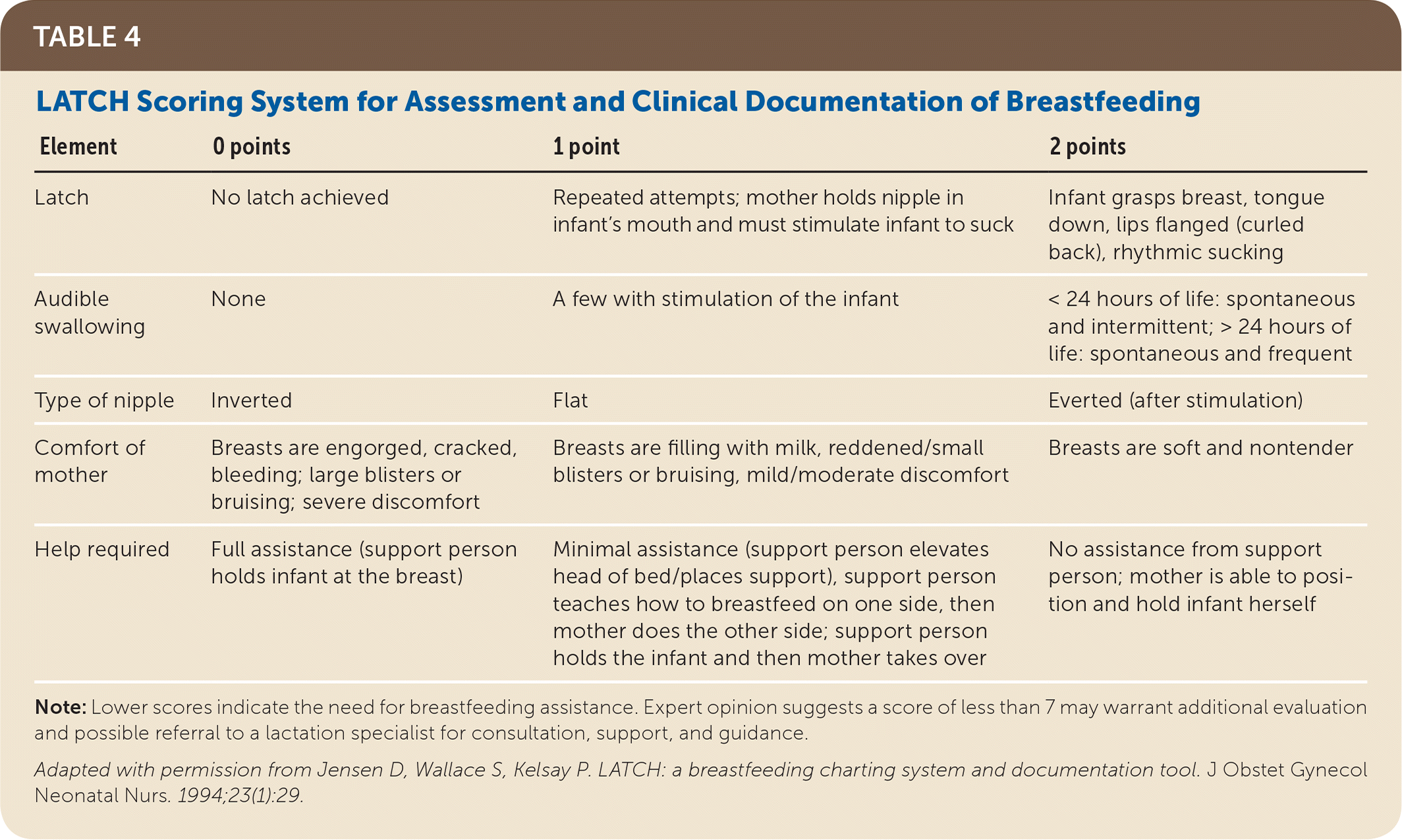
The LATCH (latch, audible swallowing, type of nipple, comfort of mother, help required) score is one of three valid and reliable scoring systems to assess an adequate latch.28–30 The LATCH score uses maternal and infant variables and defines areas needing intervention (Table 4).29
TABLE 4. LATCH Scoring System for Assessment and Clinical Documentation of Breastfeeding
| Element | 0 points | 1 point | 2 points |
|---|---|---|---|
| Latch | No latch achieved | Repeated attempts; mother holds nipple in infant's mouth and must stimulate infant to suck | Infant grasps breast, tongue down, lips flanged (curled back), rhythmic sucking |
| Audible swallowing | None | A few with stimulation of the infant | < 24 hours of life: spontaneous and intermittent; > 24 hours of life: spontaneous and frequent |
| Type of nipple | Inverted | Flat | Everted (after stimulation) |
| Comfort of mother | Breasts are engorged, cracked, bleeding; large blisters or bruising; severe discomfort | Breasts are filling with milk, reddened/small blisters or bruising, mild/moderate discomfort | Breasts are soft and nontender |
| Help required | Full assistance (support person holds infant at the breast) | Minimal assistance (support person elevates head of bed/places support), support person teaches how to breastfeed on one side, then mother does the other side; support person holds the infant and then mother takes over | No assistance from support person; mother is able to position and hold infant herself |
Note: Lower scores indicate the need for breastfeeding assistance. Expert opinion suggests a score of less than 7 may warrant additional evaluation and possible referral to a lactation specialist for consultation, support, and guidance.
Adapted with permission from Jensen D, Wallace S, Kelsay P. LATCH: a breastfeeding charting system and documentation tool. J Obstet Gynecol Neonatal Nurs. 1994;23(1):29.
The infant should also be examined for palatal anomalies that may affect latch, such as ankyloglossia. Ankyloglossia occurs in 4% to 11% of infants.31 There is evidence for and against frenotomy for treatment of ankyloglossia. One case series of 24 mother-infant pairs with breastfeeding difficulties used ultrasound scans of the oral cavity before and after frenotomy and assessed milk transfer using test weighing, nipple pain, and LATCH scores. Infants had less compression of the nipple on ultrasonography and a significant improvement in LATCH score after frenotomy.32 A 2017 Cochrane review concluded that frenotomy reduced maternal nipple pain in the short term and, according to expert opinion, this may support continued breastfeeding.31
What Are the Most Common Causes of Nipple Pain, and How Should They Be Treated?
Nipple pain is a common breastfeeding complication. Improper latch and infant positioning are contributors in 89% of cases.33 After ruling out cellulitis, mastitis, and breast abscess, latch and positioning should be assessed. Blocked milk ducts, oversupply, candidiasis, dermatologic conditions, and vasospasm should also be considered.
EVIDENCE SUMMARY
In an Australian study of breastfeeding mothers, 36% of women had nipple pain.33 Common causes of nipple pain were inadequate positioning, flat or inverted nipples, ankyloglossia and palatal anomaly, infections, and vasospasm. There were no cases of nipple pain due to strong infant suck, milk blisters, or dermatologic conditions. In mothers who had difficulty with latch and positioning, 58% had resolution of pain after correcting the problem. Given the significant number of women who did not have resolution of pain, the cause of nipple pain may be multifactorial. Most recommendations for management and treatment of blocked milked ducts, oversupply, candidiasis, dermatologic conditions, and vasospasm are based on small randomized controlled trials and expert opinion. The Academy of Breastfeeding Medicine has clinical protocols for addressing mastitis and persistent pain. eTable A includes recommendations for managing common conditions that can affect breastfeeding.
eTABLE A Management of Common Conditions That Can Affect Breastfeeding
| Condition | Presentation | Treatment |
|---|---|---|
| Dermatoses | ||
| Bacterial infection | Erythema, purulent discharge | Most cultures are positive for Staphylococcus |
| Topical mupirocin (Bactroban) applied three times per day | ||
| Candidiasis | Salmon-colored nipples, flaky or shiny skin with associated itching or burning within the duct during feeding | Topical or oral antifungals |
| Oral fluconazole (Diflucan; two 150-mg doses given 48 hours apart or 100 mg per day for 10 days) is more effective than oral nystatin | ||
| Topical mupirocin applied three times per day for five to seven days can be considered because it may have antifungal properties and help prevent secondary bacterial infections | ||
| Gentian violet can be used with caution because of the risk of infant mucosal ulcerations: gentian violet 1% is applied to the nipple with a cotton swab (this is messy and will stain clothing and skin) followed by a feeding at the treated breast, then this is repeated on the other side; this process is continued daily for three or four days, and up to seven days if there is improvement | ||
| Dermatitis/eczema | Pruritic, erythematous, scaly rash | Remove offending agent |
| Rinse older infant's mouth between eating solids and breastfeeding | ||
| Class IV medium-potency topical corticosteroid, such as hydrocortisone valerate 0.2%, triamcinolone 0.1%, or fluocinolone 0.025% (Synalar) applied twice per day for seven days | ||
| Nipple damage | Erythema, broken skin, ulcerations, bruising | Adjustment of latch and infant position or pump flange size to stop trauma to the nipple |
| Expressed breast milk applied to the nipple after feedings and as needed between feedings | ||
| Lanolin, all-purpose nipple ointment, breast shells, or glycerin pads can be used but are no more effective than expressed breast milk; hydrogel dressings have been shown to manage pain more effectively than lanolin | ||
| Milk flow issues | ||
| Blocked milk ducts | Tender nodule confined to one or more ducts | Check breast pump flange sizes (during expression phase of pumping, the nipple and a small amount of areola should be pulled into the tunnel; the nipple should be centered and move freely in the tunnel) |
| Check the latch of the infant | ||
| Massage area or apply vibration (e.g., with an electric toothbrush or massager) | ||
| Improve/increase drainage of the breast by removing constricting clothing (e.g., underwire bras, tight sports bras), increasing the frequency of feedings, or pumping more often or between feedings; hand express to focus on one area for complete emptying | ||
| Dangle feeding: the breast is dangled over the infant, often with the infant lying flat or inclined and the mother leaning over the infant so that milk flows forward by gravity | ||
| Heat therapy: apply warm compresses or a heating pad to the breast for 20 minutes | ||
| Feed with the chin toward the blockage to increase suction on that area and improve drainage (this may require assistance from a support person to hold the infant in position or can be done with dangle feeding) | ||
| Reduce pain and inflammation with nonsteroidal anti-inflammatory drugs such as ibuprofen, 600 to 800 mg three times per day | ||
| The herbal remedy lecithin, 1,200 mg three or four times per day, can be considered for recurrence | ||
| Evaluate for milk blebs | ||
| Rest and hydration | ||
| Engorgement | Full, tender breasts; breasts are edematous and shiny, and nipples and areolae may appear similar to inverted nipple; difficulty with latching | Hot or cold packs, acupuncture, application of cabbage leaves, and massage therapy may be helpful to reduce discomfort |
| Reverse pressure softening (positive pressure applied around the nipple and areola temporarily moving interstitial fluid deeper into the breast away from the areola, making the areola softer and more pliable) decreases edema around the nipple and areola to help the infant latch more easily; a video of this method is available at https://m.youtube.com/watch?t=15s&v=2_RD9HNrOJ8 | ||
| Feed infant in a reclined position to reduce flow to infant | ||
| Hand express or pump just enough to soften the breast and provide relief but not completely drain the breast | ||
| Milk blebs | Milk-filled blisters on the nipple | Soak the breast in warm salt water for five to 10 minutes, and then gently rub the nipple with a washcloth to abrade it and unroof the blister; if this is ineffective, a sterile 18-gauge needle can be used to unroof the blister |
| Oversupply | Forceful let down; infant may pull away from or clamp down on the breast while feeding; infant may have loose, green stools with some mucus | Follow recommendations for engorgement |
| Reduce feedings or pumping sessions slowly to reduce milk production | ||
| Block feeding: allow infant to feed off same breast for all feedings until supply regulates; this should be done with supervision of a physician and lactation consultant to ensure weight gain of infant and to prevent mastitis | ||
| Serious infections | ||
| Breast abscess | Tender, fluctuant nodule; erythema; induration; warmth | Ultrasonography for diagnosis |
| Incision and drainage plus appropriate antibiotic therapy based on culture results | ||
| Usually associated with the systemic symptoms of mastitis | Because of the risk of sinus tract formation, referral to a breast surgeon or interventional radiologist for incision and drainage should be considered | |
| Mastitis without systemic symptoms | Tender nodule within a duct plus erythema and warmth | Treat for blocked ducts, including massage, warm compresses, rest, hydration, and nonsteroidal anti-inflammatory drugs, for 24 hours |
| If there is no improvement after 24 hours, start dicloxacillin, 500 mg four times per day for five days; add an additional five days if inflammation is still present | ||
| Mastitis with systemic symptoms | Symptoms of mastitis plus malaise, fatigue, and fever greater than 101°F (38.3°C) | Follow recommendations for mastitis without systemic symptoms |
| If symptoms do not resolve in 48 hours, a milk sample should be cultured; most cultures are positive for Staphylococcus | ||
| If there is a concern for methicillin-resistant Staphylococcus aureus, the patient should be treated accordingly | ||
| If symptoms are unresolved or there is an area of fluctuance, breast ultrasonography should be performed to evaluate for abscess | ||
| Vascular issues | ||
| Vasospasm | Breast pain after feeding | Prevent or reduce cold exposure; warm the nipples |
| Raynaud phenomenon: nipple blanches white after feeding, and then may flush purple-blue to red a few minutes later; similarsymptoms in hands or feet | Treat causes of nipple trauma | |
| Avoidance of vasoconstrictive products, including caffeine | ||
| Nifedipine, 30 mg per day for two weeks, can minimize pain and is safe in breastfeeding women | ||
Information from:
Amir LH. ABM clinical protocol #4: mastitis, revised March 2014. Breastfeed Med. 2014;9(5):239–243.
Amir LH. Managing common breastfeeding problems in the community. BMJ. 2014;348:g2954.
Anderson JE, Held N, Wright K. Raynaud's phenomenon of the nipple: a treatable cause of painful breastfeeding. Pediatrics. 2004;113(4):e360–e364.
Berens P, Brodribb W. ABM clinical protocol #20: engorgement, revised 2016. Breastfeed Med. 2016;11:159–163.
Berens P, Eglash A, Malloy M, Steube AM. ABM clinical protocol #26: persistent pain with breastfeeding. Breastfeed Med. 2016;11(2):46–53.
Boi B, Koh S, Gail D. The effectiveness of cabbage leaf application (treatment) on pain and hardness in breast engorgement and its effect on the duration of breastfeeding. JBI Libr Syst Rev. 2012;10(20):1185–1213.
Cotterman KJ. Reverse pressure softening: a simple tool to prepare areola for easier latching during engorgement. J Hum Lact. 2004;20(2):227–237.
Dennis CL, Jackson K, Watson J. Interventions for treating painful nipples among breastfeeding women. Cochrane Database Syst Rev. 2014;(12):CD007366.
de Wet PM, Rode H, van Dyk A, Millar AJ. Perianal candidosis—a comparative study with mupirocin and nystatin. Int J Dermatol. 1999;38(8):618–622.
Dodd V, Chalmers C. Comparing the use of hydrogel dressings to lanolin ointment with lactating mothers. J Obstet Gynecol Neonatal Nurs. 2003; 32(4):486–494.
Francis-Morrill J, Heinig MJ, Pappagianis D, Dewey KG. Diagnostic value of signs and symptoms of mammary candidosis among lactating women. J Hum Lact. 2004;20(3):288–295.
Goins RA, Ascher D, Waecker N, Arnold J, Moorefield E. Comparison of fluconazole and nystatin oral suspensions for treatment of oral candidiasis in infants. Pediatr Infect Dis J. 2002;21(12):1165–1167.
Kent JC, Ashton E, Hardwick CM, et al. Nipple pain in breastfeeding mothers: incidence, causes and treatments. Int J Environ Res Public Health. 2015;12(10):12247–12263.
Mangesi L, Zakarija-Grkovic I. Treatments for breast engorgement during lactation. Cochrane Database Syst Rev. 2016;(6):CD006946.
Newman J, Pitman T. Dr. Jack Newman's Guide to Breastfeeding. London, United Kingdom: Pinter & Martin; 2014.
Nicholas RO, Berry V, Hunter PA, Kelly JA. The antifungal activity of mupirocin. J Antimicrob Chemother. 1999;43(4):579–582.
Su CW, Gaskie S, Jamieson B, Triezenberg D. Clinical inquiries. What is the best treatment for oral thrush in healthy infants? J Fam Pract. 2008; 57(7):484–485.
van Veldhuizen-Staas CG. Overabundant milk supply: an alternative way to intervene by full drainage and block feeding. Int Breastfeed J. 2007;2:11.
Witt AM, Bolman M, Kredit S, Vanic A. Therapeutic breast massage in lactation for the management of engorgement, plugged ducts, and mastitis. J Hum Lact. 2016;32(1):123–131.
This article updates previous articles on this topic by Sinusas and Gagliardi,34 Biagioli,35 and Keister, et al.36
Data Sources: A PubMed search was completed in Clinical Queries using the key terms breastfeeding, pain, strategies, frenotomy, LATCH scores, latch, interventions, exclusivity, and duration. The search included meta-analyses, randomized controlled trials, and reviews. Also searched were the Cochrane Database of Systematic Reviews, Clinical Evidence, National Guideline Clearinghouse, U.S. Preventive Services Task Force, Essential Evidence Plus, EBM Online, and UpToDate. Search dates: May 12, 2017, and April 20, 2018.
The opinions and assertions contained herein are the private views of the authors and are not to be construed as official or as reflecting the views of the U.S. Army Medical Department or the U.S. Army Service at large.

