
Am Fam Physician. 2018;98(6):377-378
Author disclosure: No relevant financial affiliations.
An 82-year-old man who worked in a hardware store presented for a routine health examination. He did not have fevers, chills, night sweats, or unintentional weight loss, and his vital signs were normal. His only concern was a nontender lesion on his thumbnail that he noticed about three months earlier. He had no recent trauma.
Physical examination revealed a longitudinal melanonychia on the radial edge of the left thumbnail. Brown-black pigmentation was noted over the proximal nail fold (Figure 1). The pigment tapered distally, and a V-shaped nick in the nail plate was present at the distal aspect of the streak.
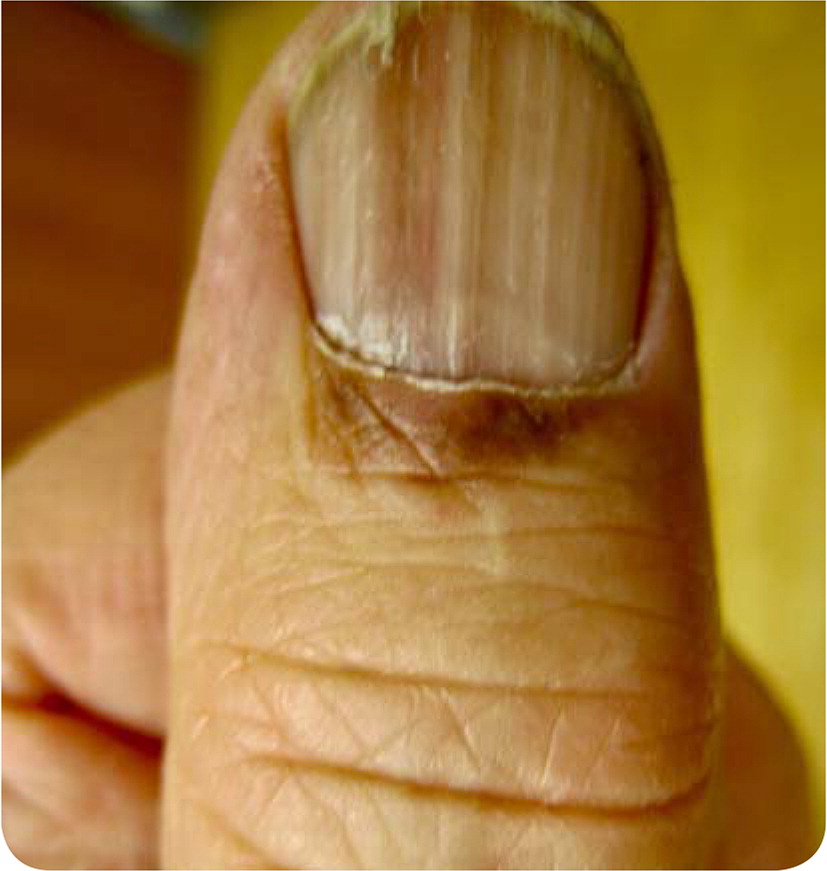
Question
Discussion
The answer is A: acral melanoma. Recognition of a subungual melanoma can be challenging, and prognosis is generally worse than for other cutaneous melanomas because of delayed diagnosis.1,2 Hutchinson nail sign (black or brown pigmentation extending from the nail bed to the proximal or lateral nail folds) is associated with acral lentiginous melanoma.3 More common benign causes of longitudinal melanonychia, such as matrix nevi, may look similar but typically occur concurrently in multiple nail beds.4 Biopsy of the lesion is warranted to rule out melanoma. In situ nail matrix melanomas may be treated with conservative excision of the entire nail apparatus (nail plate, bed, and matrix).5
Melanonychia striata is a band of black or brown pigmentation due to melanin beneath the nail plate and is common in patients with darker skin complexions. The band is of uniform width, whereas melanoma of the nail apparatus is generally wider at the base, tapering distally, and may cause knicking of the distal nail plate. Melanonychia striata may be caused by trauma; medication use (e.g., minocycline [Minocin], zidovudine [Retrovir], bleomycin, antimalarials); and bacterial, fungal, or human immunodeficiency virus infections.6
Nail matrix hematomas are caused by traumatic injury to the nail bed, leading to accumulation of blood beneath the fingernail. Increased pressure from hematoma expansion can cause tenderness. Pain usually resolves within days of the injury. The nail bed color will evolve from red to purple, and later to dark brown or black as the blood clots and is subsequently resorbed. Persistent pain from the hematoma may require pressure relief by trephination, or drainage of the hematoma with a sharp object performed by a health care professional.
Infection with Pseudomonas aeruginosa can cause green discoloration of the nail bed. It is often diagnosed based on clinical appearance but can be confirmed with fingernail cultures. It commonly occurs as a complication of chronic paronychia or onycholysis. It generally affects one or two nails, particularly after prolonged water exposure.
Subungual verruca vulgaris is an atypical presentation of the wart caused by human papillomavirus arising from beneath the nail plate. The verrucae cause nail plate deformation, often evolving into hyperkeratotic, rough papules with an irregular surface. Reddish or brown discoloration may form because of capillary loop thrombosis.
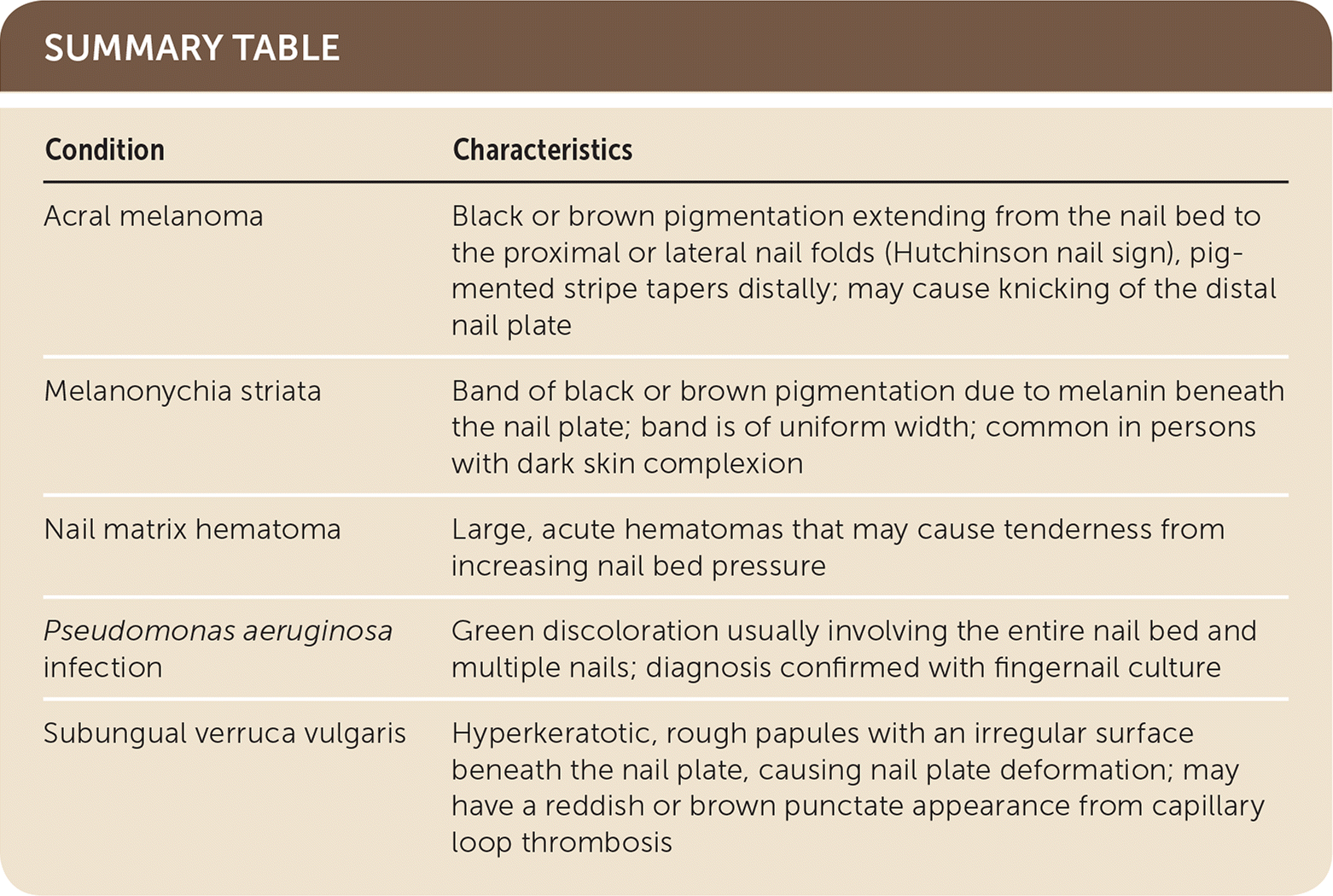
| Condition | Characteristics |
|---|---|
| Acral melanoma | Black or brown pigmentation extending from the nail bed to the proximal or lateral nail folds (Hutchinson nail sign), pigmented stripe tapers distally; may cause knicking of the distal nail plate |
| Melanonychia striata | Band of black or brown pigmentation due to melanin beneath the nail plate; band is of uniform width; common in persons with dark skin complexion |
| Nail matrix hematoma | Large, acute hematomas that may cause tenderness from increasing nail bed pressure |
| Pseudomonas aeruginosa infection | Green discoloration usually involving the entire nail bed and multiple nails; diagnosis confirmed with fingernail culture |
| Subungual verruca vulgaris | Hyperkeratotic, rough papules with an irregular surface beneath the nail plate, causing nail plate deformation; may have a reddish or brown punctate appearance from capillary loop thrombosis |
