Anemia is associated with increased morbidity and mortality in older adults. Diagnostic cutoff values for defining anemia vary with age, sex, and possibly race. Anemia is often asymptomatic and discovered incidentally on laboratory testing. Patients may present with symptoms related to associated conditions, such as blood loss, or related to decreased oxygen-carrying capacity, such as weakness, fatigue, and shortness of breath. Causes of anemia in older adults include nutritional deficiency, chronic kidney disease, chronic inflammation, and occult blood loss from gastrointestinal malignancy, although in many patients the etiology is unknown. The evaluation includes a detailed history and physical examination, assessment of risk factors for underlying conditions, and assessment of mean corpuscular volume. A serum ferritin level should be obtained for patients with normocytic or microcytic anemia. A low serum ferritin level in a patient with normocytic or microcytic anemia is associated with iron deficiency anemia. In older patients with suspected iron deficiency anemia, endoscopy is warranted to evaluate for gastrointestinal malignancy. Patients with an elevated serum ferritin level or macrocytic anemia should be evaluated for underlying conditions, including vitamin B12 or folate deficiency, myelodysplastic syndrome, and malignancy. Treatment is directed at the underlying cause. Symptomatic patients with serum hemoglobin levels of 8 g per dL or less may require blood transfusion. Patients with suspected iron deficiency anemia should be given a trial of oral iron replacement. Lower-dose formulations may be as effective and have a lower risk of adverse effects. Normalization of hemoglobin typically occurs by eight weeks after treatment in most patients. Parenteral iron infusion is reserved for patients who have not responded to or cannot tolerate oral iron therapy.
Anemia is a common condition in adults 60 years and older. Given the demographic growth of this population and the morbidity and mortality associated with anemia, primary care physicians should be familiar with the evaluation and management of anemia in older persons.
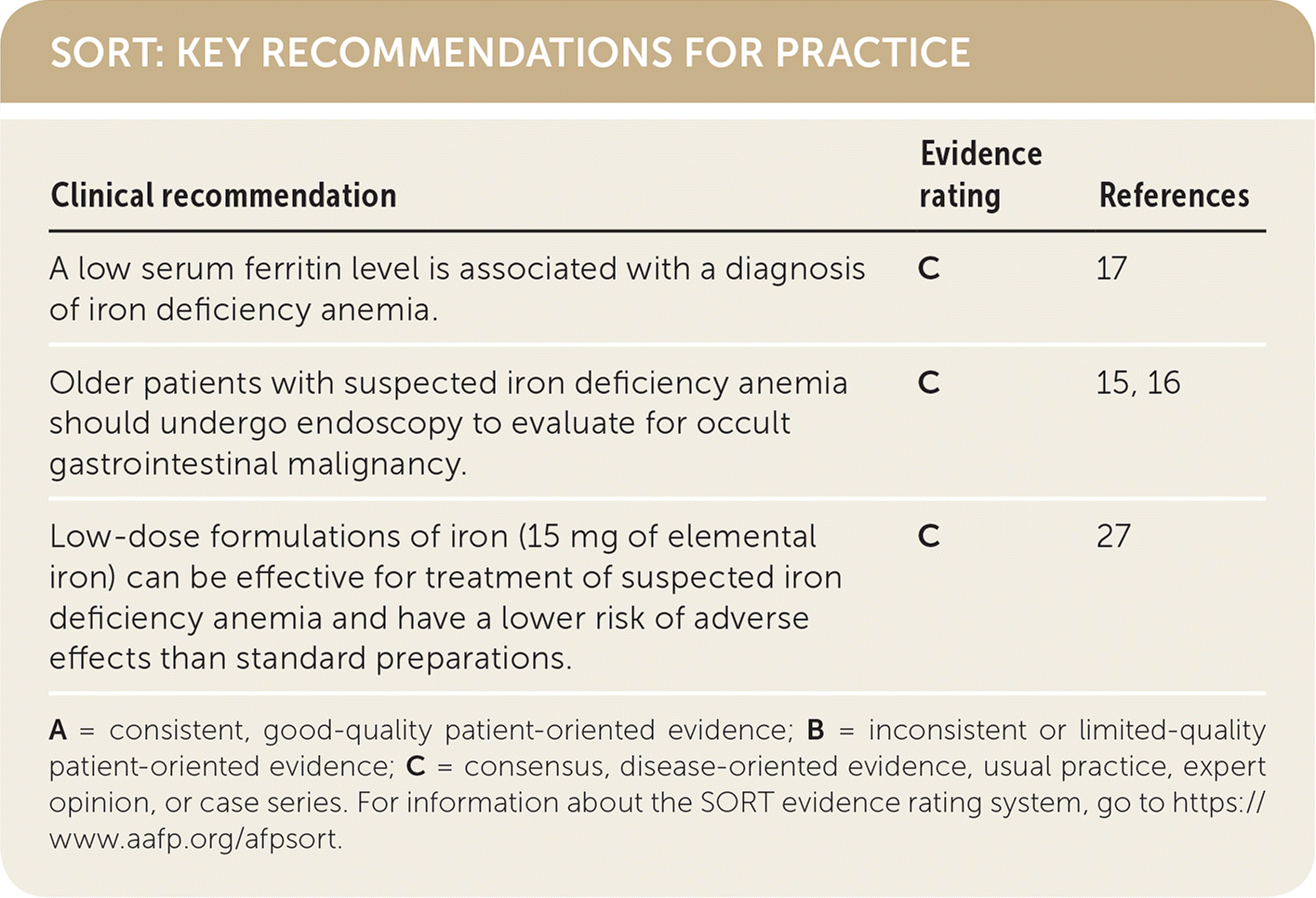
SORT: KEY RECOMMENDATIONS FOR PRACTICE
| Clinical recommendation | Evidence rating | References |
|---|---|---|
| A low serum ferritin level is associated with a diagnosis of iron deficiency anemia. | C | 17 |
| Older patients with suspected iron deficiency anemia should undergo endoscopy to evaluate for occult gastrointestinal malignancy. | C | 15, 16 |
| Low-dose formulations of iron (15 mg of elemental iron) can be effective for treatment of suspected iron deficiency anemia and have a lower risk of adverse effects than standard preparations. | C | 27 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
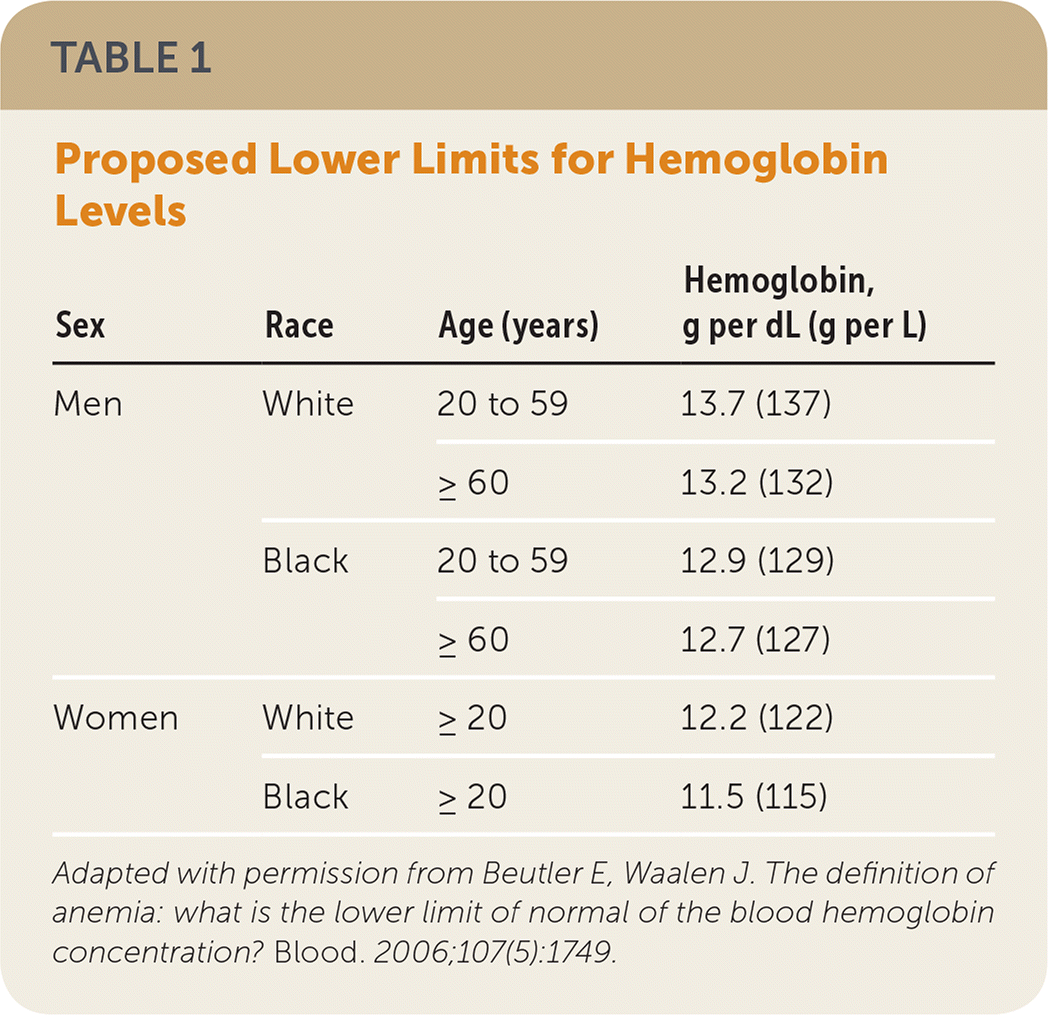
Anemia has historically been defined as a hemoglobin level of less than 12 g per dL (120 g per L) in women and less than 13 g per dL (130 g per L) in men.1 These values and reference ranges remained static until recently, when cohort studies such as the third National Health and Nutrition Examination Survey suggested that this definition needs to be adjusted because of the variability in normal hemoglobin levels with age, sex, and black race (values for different ethnicities are not available). A revised definition that may better reflect these differences has been proposed (Table 1).2
TABLE 1. Proposed Lower Limits for Hemoglobin Levels
| Sex | Race | Age (years) | Hemoglobin, g per dL (g per L) |
|---|---|---|---|
| Men | White | 20 to 59 | 13.7 (137) |
| ≥ 60 | 13.2 (132) | ||
| Black | 20 to 59 | 12.9 (129) | |
| ≥ 60 | 12.7 (127) | ||
| Women | White | ≥ 20 | 12.2 (122) |
| Black | ≥ 20 | 11.5 (115) |
Adapted with permission from Beutler E, Waalen J. The definition of anemia: what is the lower limit of normal of the blood hemoglobin concentration? Blood. 2006;107(5):1749.
Prevalence
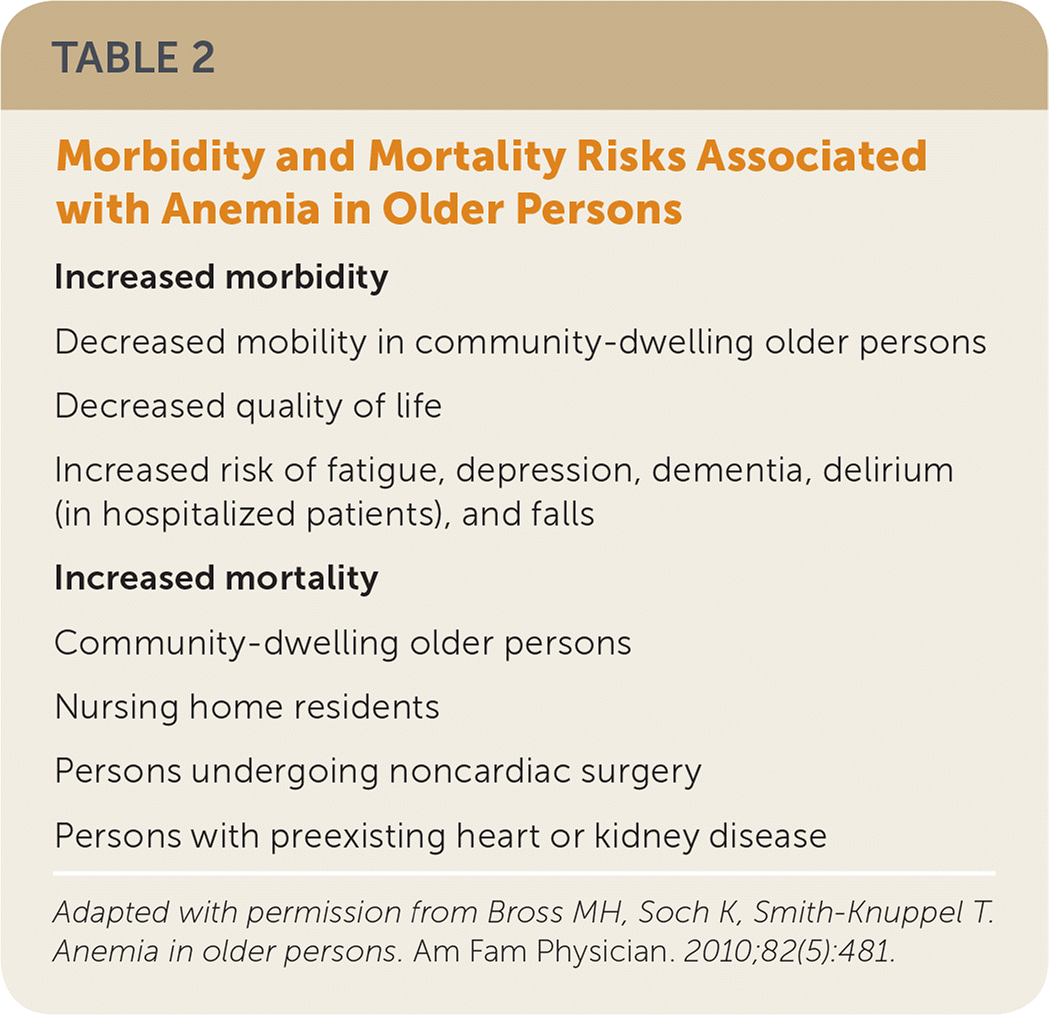
The overall prevalence of anemia is 17% in older adults (7% to 11% of community-dwelling older adults, 47% of those in nursing homes, and 40% in hospitalized patients).3,4 Most of these patients have mild anemia (hemoglobin level of 11 g per dL [110 g per L] or greater), but even mild anemia is independently associated with increased morbidity and mortality.5–9 A prospective cohort analysis of 3,758 patients 65 years and older found that new-onset anemia and decreased hemoglobin levels with or without anemia are associated with increased mortality (hazard ratios of 1.39 [95% confidence interval (CI), 1.15 to 1.69] and 1.11 [95% CI, 1.04 to 1.18], respectively, per 1 g per dL decrease in hemoglobin).5 Common causes of morbidity in these patients are listed in Table 2.5 A 2016 British prospective cohort study of 220 patients with a mean age of 83.6 years found that anemia is associated with increased all-cause mortality one year after hospitalization.10 After adjusting for comorbid conditions, anemia in community-dwelling older adults is associated with functional decline and decreased mobility, balance, and ability to rise from a chair.11,12 Overall, one-third of older patients with anemia have a nutritional deficiency, which includes iron deficiency due to subsidiary causes (e.g., bowel malignancy), one-third have chronic inflammation or chronic kidney disease (CKD), and one-third have an unknown cause.13
TABLE 2. Morbidity and Mortality Risks Associated with Anemia in Older Persons
Increased morbidity
|
Increased mortality
|
Adapted with permission from Bross MH, Soch K, Smith-Knuppel T. Anemia in older persons. Am Fam Physician. 2010;82(5):481.
Diagnosis
Recognizing clinical signs and symptoms of anemia is an important first step. However, some patients will be asymptomatic, and diagnosis will occasionally be based on incidental laboratory findings. In acute presentations, patients will have symptoms secondary to volume loss, such as lightheadedness, syncope, and hypotension. Chronic anemia may be asymptomatic but in severe cases presents with symptoms related to decreased oxygen-carrying capacity, such as weakness, fatigue, shortness of breath, and worsening of comorbid conditions such as angina, heart failure, CKD, and chronic obstructive pulmonary disease. These conditions are more common in older patients and may cause many of the same clinical symptoms as anemia; thus, a high clinical suspicion must be maintained.
In addition to clinical manifestations, risk factors for anemia should guide the evaluation. Risk factors that are more common in older patients include chronic alcohol use, malnutrition, CKD, liver disease, myelodysplastic disorders, gastrointestinal bleeding, cancer, androgen deficiency, and age-related decline in stem cell proliferation. The clinical history should focus on identifying these risk factors, as well as symptoms that may suggest a specific condition. Melena, hematochezia, and unintentional weight loss may indicate gastrointestinal bleeding. Recurrent skin infections may be a sign of immunocompromise suggestive of myelodysplastic syndrome.14 The presence or absence of these risk factors should guide further evaluation and treatment.
Once anemia is suspected, a complete blood count with differential should be obtained. If the results indicate anemia, further studies are needed to evaluate the underlying cause and to guide treatment. The mean corpuscular volume is used to classify anemia as microcytic (less than 80 fL), normocytic (80 to 100 fL), or macrocytic (greater than 100 fL), and allows for a more specific and tailored evaluation.
Microcytic and Normocytic Anemia: Overlapping Clinical Manifestations
Microcytic and normocytic anemias are most common in older adults. Although microcytic anemia is classically associated with iron deficiency, and normocytic with chronic disease or unknown causes, there is significant overlap between the manifestations of these diseases. Iron deficiency anemia occurs in 11% to 57% of patients with colorectal cancer and may be the presenting symptom in 15%.15,16 Therefore, obtaining a serum ferritin level is the first step when evaluating these patients (Figure 1).15–19 A level less than 19 ng per mL (43 pmol per L) is highly suggestive of iron deficiency anemia (positive likelihood ratio [LR+] = 41), but this condition can be present in patients with higher levels (LR+ = 3.1 in patients with serum ferritin of 45 ng per mL [101 pmol per L] or less).17 Iron deficiency anemia is less likely in patients with serum ferritin levels of 46 to 100 ng per mL (103 to 225 pmol per L), although it cannot be ruled out. In these patients, the serum transferrin receptor–ferritin index can be used to distinguish between iron deficiency anemia and other types. (An online calculator is available for registered users.) An index of more than 1.5 supports the diagnosis of iron deficiency anemia. Fecal occult blood testing should be performed to assess for gastrointestinal blood loss, and endoscopic evaluation should be strongly considered for patients with iron deficiency anemia or in whom occult blood is identified, taking into consideration factors such as patient comorbidities and the risk of complications.18,19
FIGURE 1.
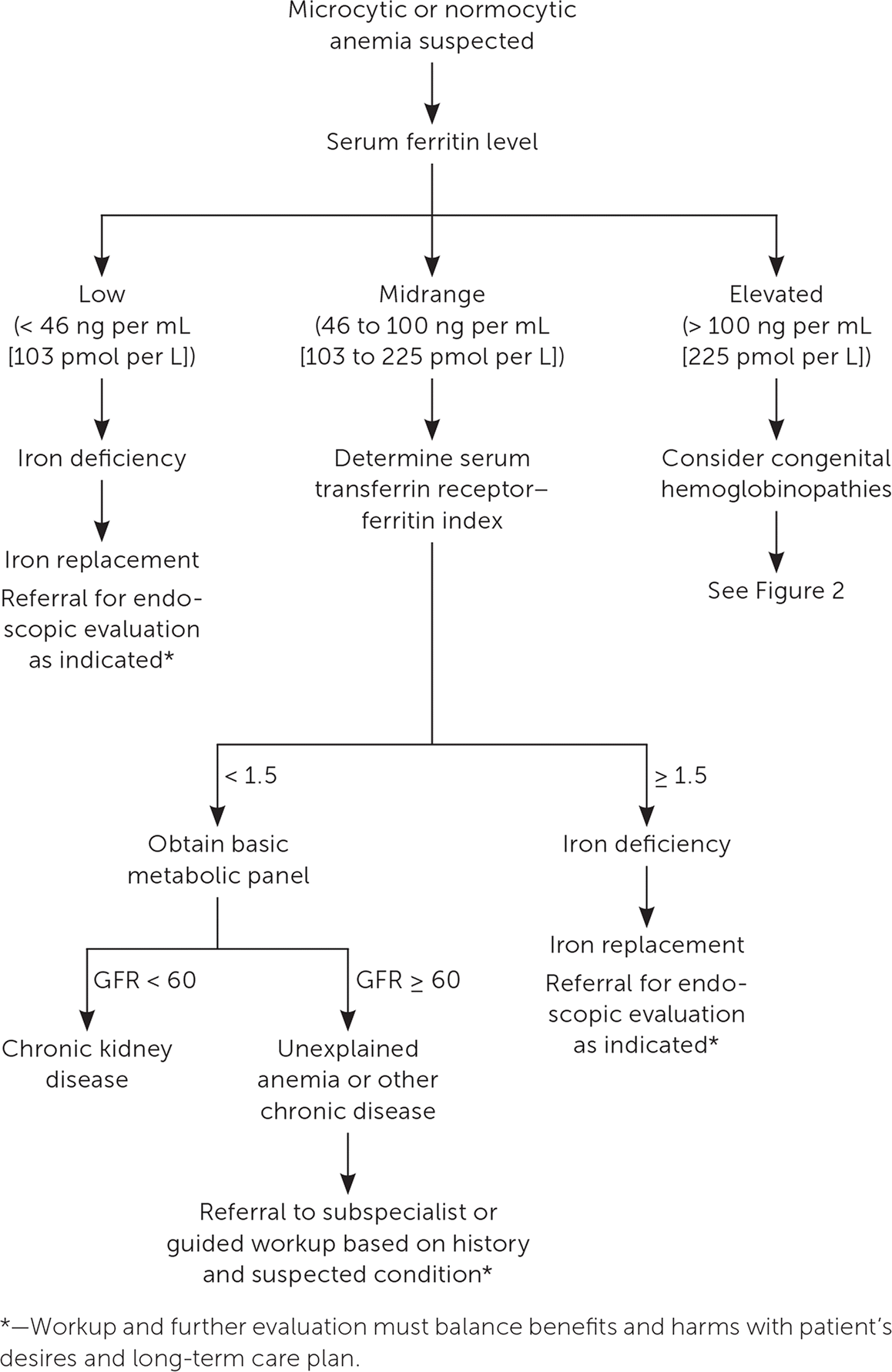
Diagnosis of microcytic and normocytic anemia. (GFR = glomerular filtration rate.)
Information from references 15 through 19.
If iron deficiency anemia is excluded, anemia of chronic disease is the most likely cause of microcytic or normocytic anemia. In older patients, anemia of chronic disease is most often caused by CKD, which can be assessed with serum creatinine and the glomerular filtration rate. Further evaluation based on clinical presentation is necessary for patients in whom iron deficiency anemia and CKD have been excluded. Evaluation should begin with a peripheral blood smear and reticulocyte count, with further evaluation based on results of these tests.
Macrocytic Anemia
If the serum ferritin level is greater than 100 ng per mL, or if macrocytic anemia is identified, the most likely cause shifts to other etiologies. A peripheral blood smear and reticulocyte count are the first steps in the evaluation of macrocytic anemia. Abnormalities in the peripheral blood smear should prompt consideration of a myelodysplastic syndrome or malignancy, and hematologic consultation is warranted. An elevated reticulocyte count (reticulocyte index greater than 2%) is associated with increased bone marrow production of red blood cells and is associated with hemolysis, hypersplenism, or recent blood loss (Figure 2).5 A low reticulocyte count can occur in patients with vitamin B12 or folate deficiency. These deficiencies can occur with chronic alcoholism, or they can be the result of malabsorption due to diet or surgery.20 Long-term use of proton pump inhibitors, histamine H2 receptor antagonists, or metformin can also cause vitamin B12 deficiency.21,22 Recognition and treatment are important because of the significant impact vitamin B12 deficiency can have on neurodegenerative disease and cognitive impairment.23 The diagnosis can be made when serum cobalamin levels are unequivocally low (less than 100 pg per mL [74 pmol per L]); elevated methylmalonic acid and homocysteine levels are more sensitive for the diagnosis of vitamin B12 deficiency in patients with higher serum cobalamin levels.24
FIGURE 2.
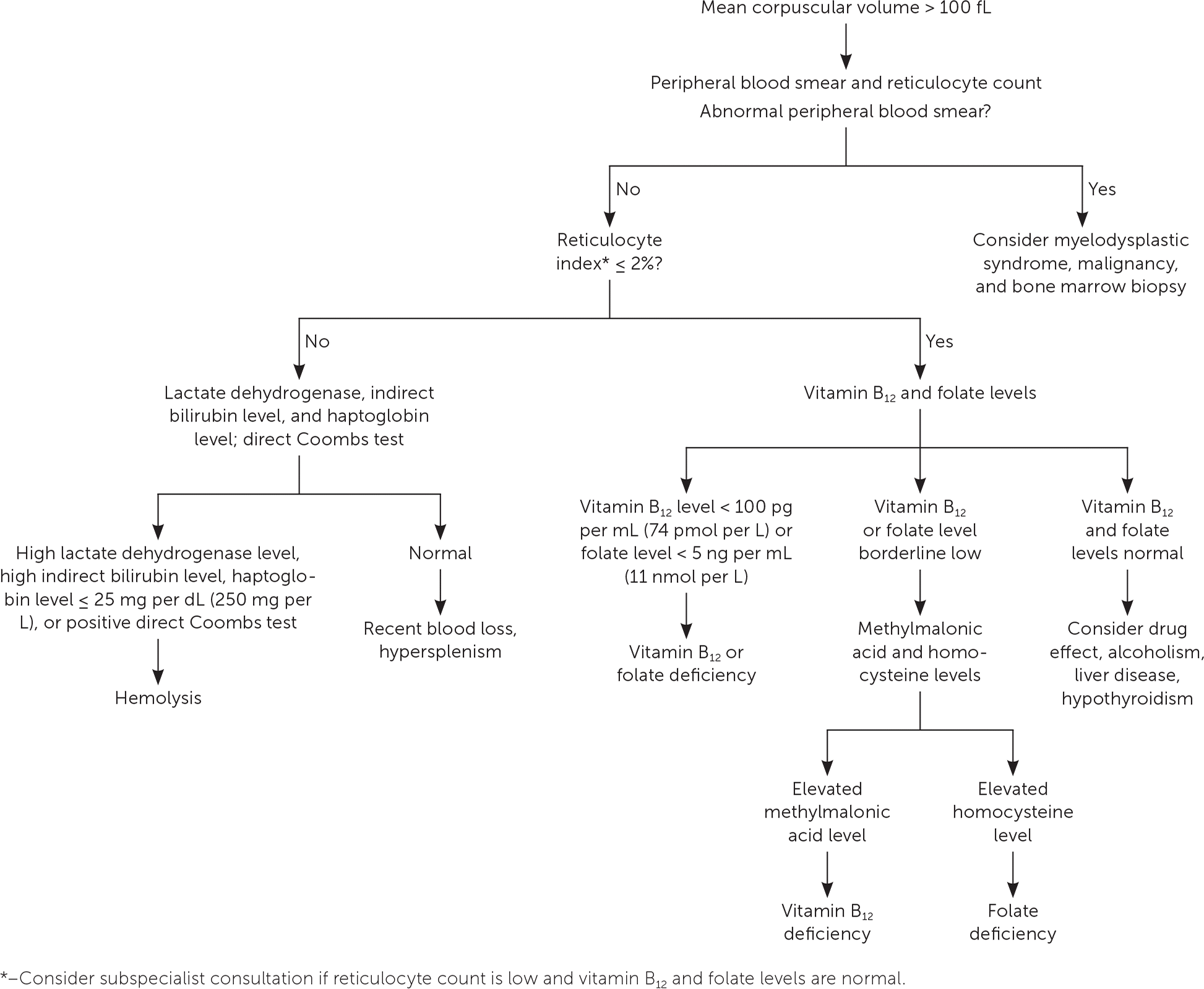
Diagnosis of macrocytic anemia.
Adapted with permission from Bross MH, Soch K, Smith-Knuppel T. Anemia in older persons. Am Fam Physician. 2010;82(5):484.
Treatment and Referral
Treatment of anemia is ultimately guided by the underlying diagnosis. This article focuses on treatment in the outpatient setting for the most common etiologies in older patients. Hospital admission and blood transfusion should be considered if there is concern for significant anemia (hemoglobin level less than 7 to 8 g per dL [70 to 80 g per L]) or if the patient is symptomatic.25,26 When developing a treatment plan, the underlying cause of anemia should be considered, as should any comorbidities. The primary care physician should discuss the potential benefits and harms of treatment with the patient and caregivers.
Iron replacement therapy can be used as a treatment, as well as a diagnostic discriminator. Initiating therapy with oral agents is reasonable as long as there is no concern for malabsorption and the patient is informed about potential adverse effects. These medications should not be taken with food because of the potential for reduced absorption, but they can be taken after meals to minimize gastrointestinal adverse effects. Medications that reduce gastric acid secretion can also reduce absorption and should not be taken at the same time.
Classically, oral therapy with 325 mg of ferrous sulfate three times per day has been recommended to achieve 100 to 200 mg of elemental iron daily. However, this regimen is associated with high rates of adverse effects, including dark or black stools (up to 91%), abdominal discomfort (up to 70%), diarrhea (up to 70%), nausea and vomiting (up to 67%), and constipation (up to 23%).27 Although there are only limited studies in older adults, new evidence demonstrates that lower doses of iron and less-frequent dosing may be equally effective while reducing the risk of adverse effects.27–29 Liquid elemental iron in dosages as low as 15 mg per day, given with orange juice to enhance absorption, can be effective while minimizing adverse effects. Liquid formulations also allow for easy dose titration. There are no specific guidelines for length of therapy, but recommendations generally advise continuing for three to six months once hemoglobin and serum ferritin levels have normalized, which typically occurs after six to eight weeks of oral therapy.
If oral iron replacement therapy is ineffective, a trial of parenteral iron infusion should be attempted.30 This may be especially necessary in patients with a risk of malabsorption with oral dosing (e.g., patients who have undergone bariatric surgery, gastrectomy, gastrojejunostomy, or other small bowel surgeries). In these patients, parenteral therapy can be considered a first-line option because of its effectiveness and significant reduction in adverse effects. Parenteral iron may also be appropriate in patients who cannot tolerate oral iron because of gastrointestinal adverse effects, and in those with ongoing blood loss that exceeds the ability to replace iron via oral administration. Infusion strategies vary by product, but all are equally safe and effective.31,32 Adverse effects with parenteral iron are rare but include allergic reactions, hypotension, dyspnea, abdominal pain, chest pain, back pain, nausea, and vomiting. Life-threatening adverse effects from parenteral iron are uncommon.31 Generally, one to five infusions are given, then laboratory studies are repeated six to eight weeks after treatment.33 Availability and cost of intravenous infusions vary based on local resources and insurance coverage. eTable A summarizes parenteral iron preparations. Celiac disease should be considered in patients with an inadequate response to iron replacement therapy.34
eTABLE A Summary of Parenteral Preparations of Iron
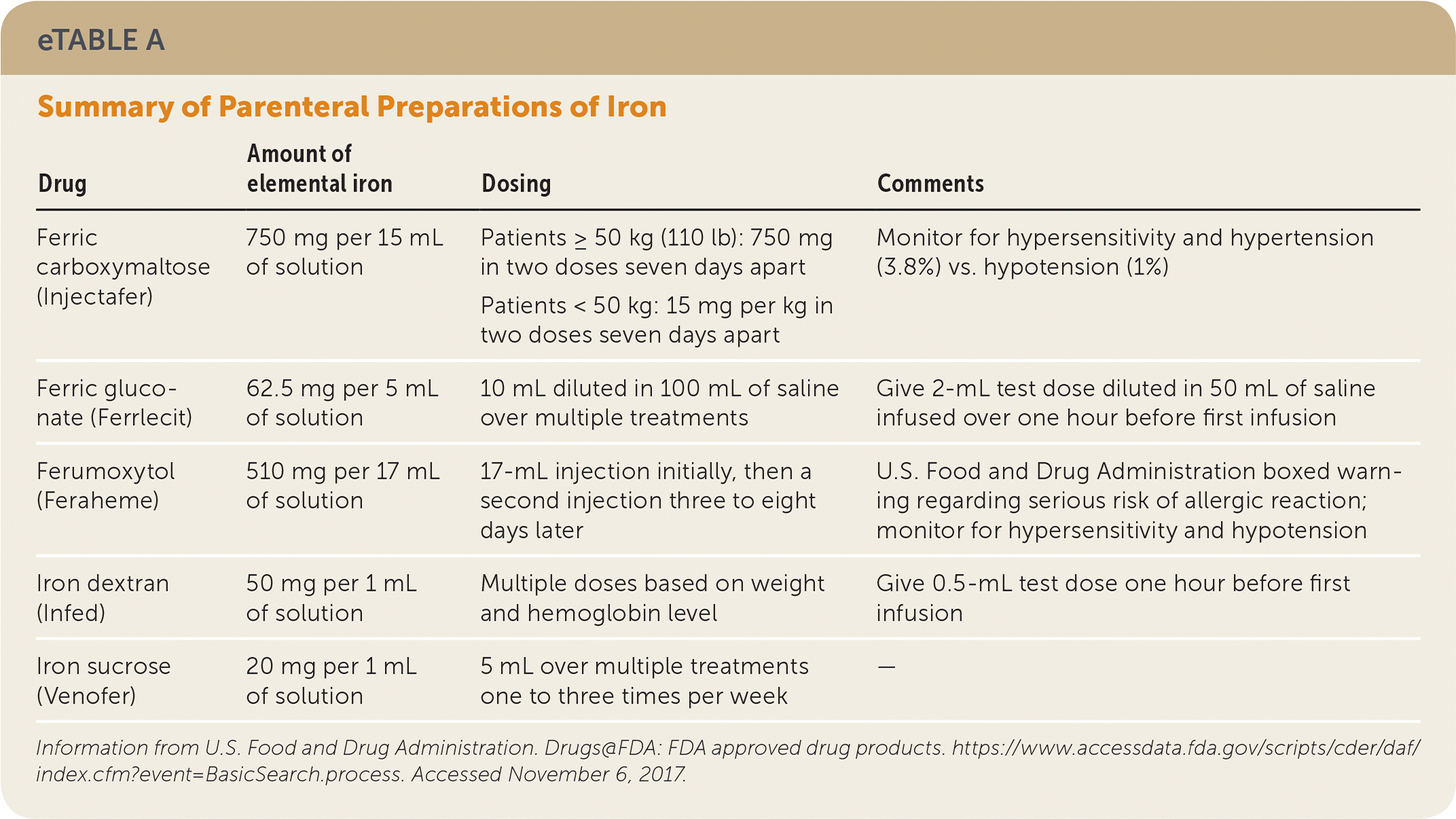
| Drug | Amount of elemental iron | Dosing | Comments |
|---|---|---|---|
| Ferric carboxymaltose (Injectafer) | 750 mg per 15 mL of solution | Patients ≥ 50 kg (110 lb):750 mg in two doses seven days apart | Monitor for hypersensitivity and hypertension (3.8%) vs. hypotension (1%) |
| Patients < 50 kg: 15 mg per kg in two doses seven days apart | |||
| Ferric gluconate (Ferrlecit) | 62.5 mg per 5 mL of solution | 10 mL diluted in 100 mL of saline over multiple treatments | Give 2-mL test dose diluted in 50 mL of saline infused over one hour before first infusion |
| Ferumoxytol (Feraheme) | 510 mg per 17 mL of solution | 17-mL injection initially, then a second injection three to eight days later | U.S. Food and Drug Administration boxed warning regarding serious risk of allergic reaction; monitor for hypersensitivity and hypotension |
| Iron dextran (Infed) | 50 mg per 1 mL of solution | Multiple doses based on weight and hemoglobin level | Give 0.5-mL test dose one hour before first infusion |
| Iron sucrose (Venofer) | 20 mg per 1 mL of solution | 5 mL over multiple treatments one to three times per week | — |
Information from U.S. Food and Drug Administration. Drugs@FDA: FDA approved drug products. https://www.accessdata.fda.gov/scripts/cder/daf/index.cfm?event=BasicSearch.process. Accessed November 6, 2017.
Vitamin B12 and folate can be replaced with oral therapy of 1 mg per day. The use of parenteral formulations is also effective,35 and patients who have had gastric bypass surgery should receive parenteral vitamin B12. Parenteral formulations can also be considered in patients who do not wish to take daily supplements. Patients with folate deficiency should have concomitant vitamin B12 deficiency corrected first, because repletion of folate can mask concurrent vitamin B12 deficiency.36 It may be beneficial to consult a nutritionist to assist with dietary recommendations and vitamin supplementation. The possibility of abuse or neglect should always be considered in older patients with malnutrition.
Subspecialty referral for treatment of underlying CKD, other inflammatory conditions, gastrointestinal disorders, or malignancies may be considered. Erythropoiesis-stimulating agents are associated with a reduced need for blood transfusions but have significant adverse effects, including an increased risk of thromboembolic events and mortality. These agents should be used with caution and only to treat to a target hemoglobin level of 11 g per dL.37,38
This article updates a previous article on this topic by Bross, et al.5
Data Sources: We searched PubMed for cohort studies, randomized controlled trials, meta-analyses, and systematic reviews from January 1990 to November 2016 in English only. Search terms included anemia, anemia in elderly, anemia prevalence, anemia cognitive impairment, anemia falls, anemia grip strength, anemia and renal or kidney disease, iron deficiency anemia, iron deficiency anemia elderly, and soluble transferrin receptor. We also performed bibliographic searches from practice recommendations and UpToDate to identify additional primary sources. Search dates: November 2016, January 2017, and June 2018.
The opinions and assertions in this article are those of the authors and do not represent official policy of the Army Medical Department, Department of the Army, or the Department of the Defense.

