Charlie is a 79-year-old former teacher. He has advanced heart and lung disease and chronic kidney disease. He has been getting weaker and weaker. As his family physician, Dr. Fields, was finishing charts after a busy clinic day, she noticed that Charlie was in the intensive care unit (ICU) after being discharged the week before. Noting his full code status, she rushed to the hospital. When Charlie's wife died last year in the ICU, he told Dr. Fields he did not want that for himself as he got sicker. After she and Charlie talked, they met with the ICU team and decided that only comfort measures would be performed. Charlie died peacefully in the hospital.
This is a familiar scenario. Dr. Fields and Charlie developed trust over the years, which helped them have a hard conversation in a moment of crisis. As a result, at the very end, Charlie got the care he wanted. But what if Dr. Fields had not opened the electronic health record (EHR)? How can we ensure that our seriously ill patients routinely get the right care without relying on individual sacrifice and luck?
Create a Process for Asking Adults 65 Years and Older to Complete a Health Care Proxy and Advance Directive as Part of Health Maintenance
When patients get very sick, their loved ones often make difficult medical decisions on their behalf.1 All adults, healthy or seriously ill, would benefit from identifying a health care proxy, completing an advance directive, and starting a conversation at home.2 Charlie's completion of an advance directive with his preferences regarding life-prolonging treatments would have been a great start, yet it is difficult to anticipate every medical situation that may occur. An even better approach is for patients and families to start a dialogue about values and priorities using a guide such as the Conversation Project Starter Kit or Prepare for Your Care.3–5 In the event of worsening illness, these conversations can serve as a guide for medical decisions and allow surrogate decision makers to speak for, rather than decide for, their loved ones.
Use Tools Such as the Serious Illness Conversation Guide
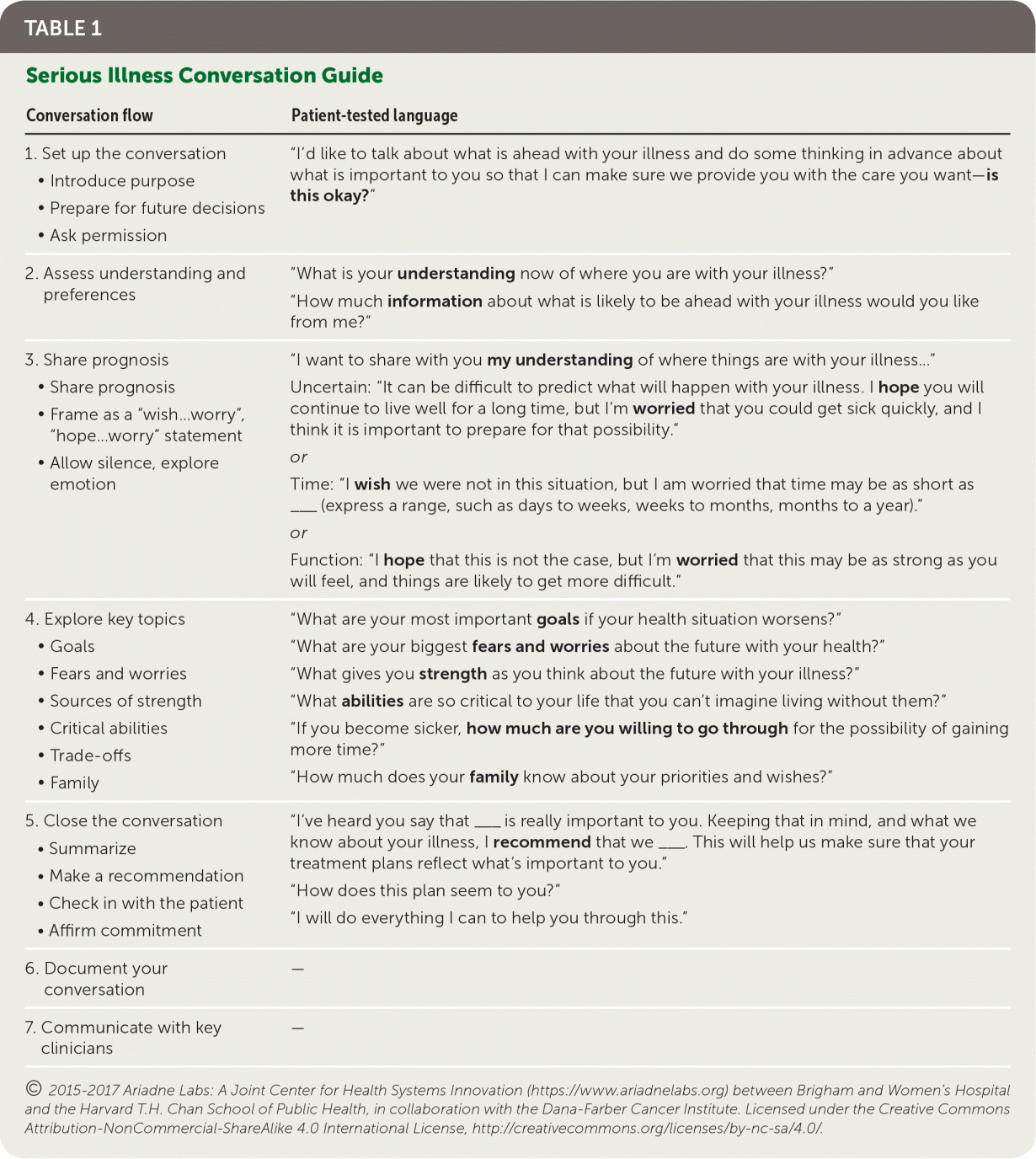
When faced with serious illness, patients make medical decisions based on their goals and worries for the future, trade-offs they are willing or not willing to make, and their understanding of their illness and the risks and benefits of treatments.6–9 Clinicians play a critical role in this process by sharing the prognosis, asking patients about what is most important, and making a recommendation grounded in each patient's values and priorities.10,11 One such approach is the Serious Illness Conversation Guide10,12 (Table 113 ). Derived from patient-tested language and best practices in palliative care, the guide suggests open-ended questions that can be adapted for any patient: What are your most important goals if your health situation worsens? What abilities are so critical to your life that you can't imagine living without them? These types of questions expand the dialogue beyond end-of-life procedures.
TABLE 1 Serious Illness Conversation Guide
| Conversation flow | Patient-tested language |
|---|---|
1. Set up the conversation
| “I'd like to talk about what is ahead with your illness and do some thinking in advance about what is important to you so that I can make sure we provide you with the care you want—is this okay?” |
| 2. Assess understanding and preferences | “What is your understanding now of where you are with your illness?” “How much information about what is likely to be ahead with your illness would you like from me?” |
3. Share prognosis
| “I want to share with you my understanding of where things are with your illness…” Uncertain: “It can be difficult to predict what will happen with your illness. I hope you will continue to live well for a long time, but I'm worried that you could get sick quickly, and I think it is important to prepare for that possibility.” or Time: “I wish we were not in this situation, but I am worried that time may be as short as ___ (express a range, such as days to weeks, weeks to months, months to a year).” or Function: “I hope that this is not the case, but I'm worried that this may be as strong as you will feel, and things are likely to get more difficult.” |
4. Explore key topics
| “What are your most important goals if your health situation worsens?” “What are your biggest fears and worries about the future with your health?” “What gives you strength as you think about the future with your illness?” “What abilities are so critical to your life that you can't imagine living without them?” “If you become sicker, how much are you willing to go through for the possibility of gaining more time?” “How much does your family know about your priorities and wishes?” |
5. Close the conversation
| “I've heard you say that ___ is really important to you. Keeping that in mind, and what we know about your illness, I recommend that we ___. This will help us make sure that your treatment plans reflect what's important to you.” “How does this plan seem to you?” “I will do everything I can to help you through this.” |
| 6. Document your conversation | — |
| 7. Communicate with key clinicians | — |
© 2015–2017 Ariadne Labs: A Joint Center for Health Systems Innovation (https://www.ariadnelabs.org) between Brigham and Women's Hospital and the Harvard T.H. Chan School of Public Health, in collaboration with the Dana-Farber Cancer Institute. Licensed under the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License, http://creativecommons.org/licenses/by-nc-sa/4.0/.
Make Conversations About Serious Illness a Team Effort Involving All Clinicians and Staff in Your Clinic
Health care professionals need efficient ways of talking with patients and families in advance of crises and building conversations into the workflow. Supportive processes include identifying patients with serious illness, preparing them for the conversation, and scheduling an office visit for the discussion. This takes a team effort involving physicians, advanced practice clinicians, nurses, social workers, and staff.
One approach to identify patients is posing the “surprise” question to the team: Would you be surprised if this patient died in the next year?14,15 A serious illness conversation would likely benefit patients for whom the response is “No, I would not be surprised.”
Although billing codes for advance care planning now provide payment for these discussions,16 other barriers exist, especially time constraints.17,18 Health systems could facilitate these efforts by providing time and support for primary clinicians to have conversations about serious illness with patients.19
Our health care system is unprepared for patients such as Charlie, who have unpredictable illnesses and increasing frailty. Any clinician who sees Charlie during or after a significant change in his health needs should be willing to start or continue the conversation and coordinate with other clinicians involved in his care, including subspecialists. For this to happen, documentation of patients' wishes should be easily accessible in the EHR, which would require significant EHR changes.20 In addition, as Charlie got sicker and his goals became clear, recommending that he complete a Physician Orders for Life-Sustaining Treatment or an out-of-hospital do-not-resuscitate form may have prevented the ICU admission, which aligned with Charlie's goals. In considering these recommendations, clinicians cannot improve the care of people with serious illness alone—to be successful, they need health system changes that support better conversations over the continuum of care.

