Adhesive capsulitis, also known as “frozen shoulder,” is a common shoulder condition characterized by pain and decreased range of motion, especially in external rotation. Adhesive capsulitis is predominantly an idiopathic condition and has an increased prevalence in patients with diabetes mellitus and hypothyroidism. Although imaging is not necessary to make the diagnosis, a finding of coracohumeral ligament thickening on noncontrast magnetic resonance imaging yields high specificity for adhesive capsulitis. Traditionally, it was thought that adhesive capsulitis progressed through a painful phase to a recovery phase, lasting one to two years with full resolution of symptoms without treatment. Recent evidence of persistent functional limitations if left untreated has challenged this theory. The most effective treatment for adhesive capsulitis is uncertain. Nonsurgical treatments include nonsteroidal anti-inflammatory drugs, short-term oral corticosteroids, intra-articular corticosteroid injections, physiotherapy, acupuncture, and hydrodilatation. Physiotherapy and corticosteroid injections combined may provide greater improvement than physiotherapy alone. Surgical treatment options for patients who have minimal improvement after six to 12 weeks of nonsurgical treatment include manipulation under anesthesia and arthroscopic capsule release.
Adhesive capsulitis, also known as “frozen shoulder,” is a common condition of the shoulder defined as a pathologic process in which contracture of the glenohumeral capsule is a hallmark. Clinically, it presents as pain, stiffness, and dysfunction of the affected shoulder.1 Adhesive capsulitis is often self-limited; however, it can persist for years with some patients never regaining full function of their shoulder.
SORT: KEY RECOMMENDATIONS FOR PRACTICE

| Clinical recommendation | Evidence rating | References |
|---|---|---|
| Consider testing persons with adhesive capsulitis for diabetes mellitus or hypothyroidism. | C | 3, 4 |
| The combination of physiotherapy and corticosteroid injection may provide greater symptom improvement than physiotherapy alone. | B | 13 |
| The combination of hydrodilatation and corticosteroid injection may expedite recovery of pain free range of motion compared with corticosteroid injection alone. | B | 17 |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
Epidemiology and Natural History
The prevalence of adhesive capsulitis is estimated at 2% to 5% of the general population. Most patients diagnosed with adhesive capsulitis are women between 40 and 60 years of age.2
Evidence supports an association of adhesive capsulitis with diabetes mellitus and hypothyroidism. A 2016 meta-analysis found that patients with diabetes were five times more likely than the control group to have adhesive capsulitis. The same meta-analysis estimated the prevalence of diabetes in patients with adhesive capsulitis to be 30% (95% confidence interval [CI], 24% to 37%).3 A 2017 case-control study reported the prevalence of a hypothyroidism diagnosis to be significantly higher in the adhesive capsulitis group compared with the control group (27.2% vs. 10.7%; P = .001).4
Traditionally, the natural history of frozen shoulder has been described as a progression through three phases: painful, stiffness, and recovery. Full resolution of symptoms without treatment has been the expected outcome for most patients over one to two years. However, recent clinical evidence of persistent functional limitation, lasting for years, has challenged this theory. A 2017 systematic review of seven studies found low-quality evidence that no treatment yielded some, but not complete improvement in range of motion after one to four years of follow-up. Moderate-quality evidence from three randomized controlled trials with longitudinal data demonstrated that most improvement in pain and range of motion occurs early, not late.5
Clinical Presentation
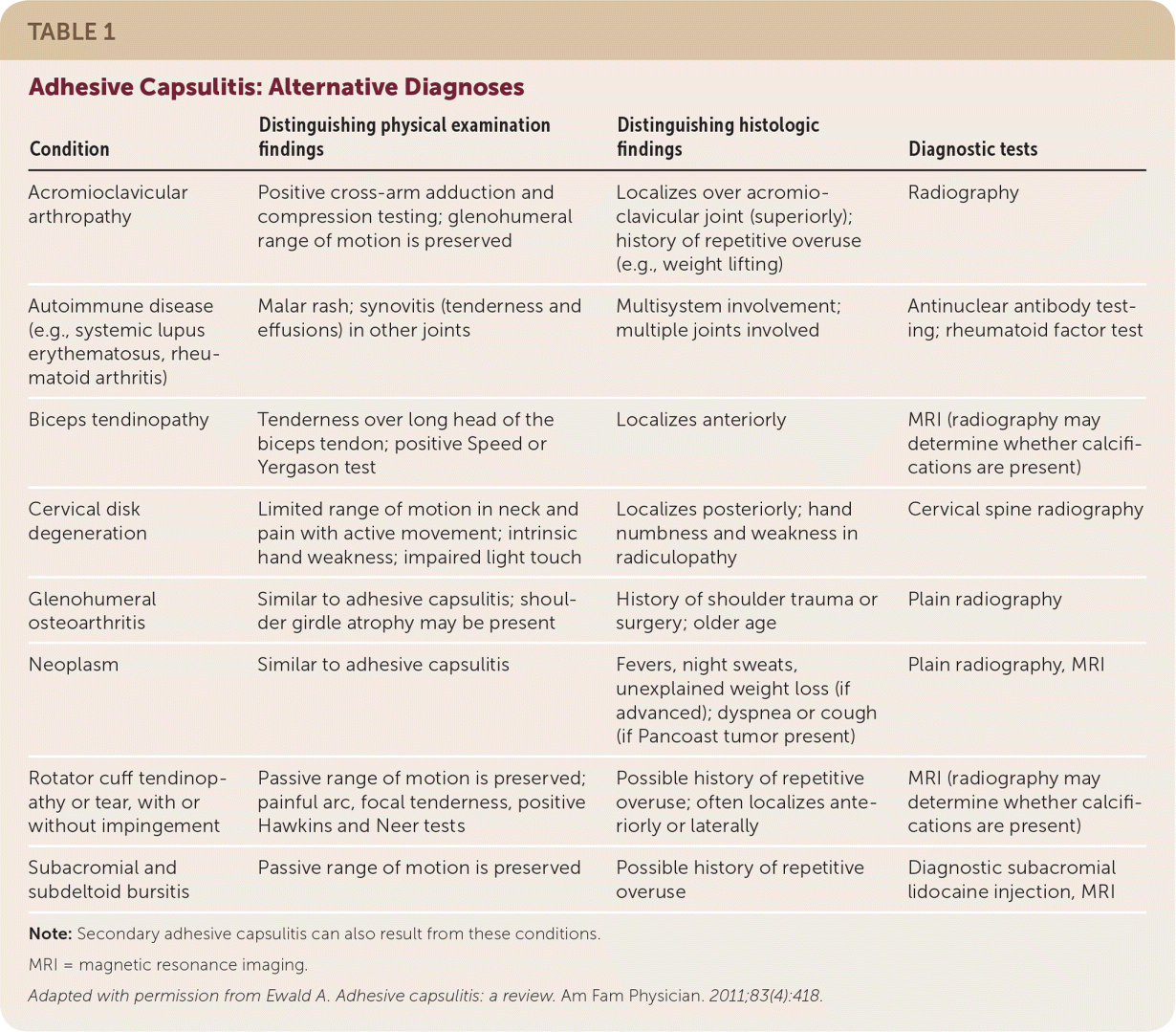
Shoulder pain accompanied by a marked decrease in range of motion is the chief characteristic of adhesive capsulitis. Pain is described as a poorly localized, dull ache, and may radiate into the biceps. Reaching overhead or behind the back may stimulate the sensation of pain and stiffness. Symptoms such as fever, night sweats, malaise, or unexplained weight loss should prompt the physician to consider an alternative diagnosis such as neoplasm or an autoimmune disease. The presence of neuropathic symptoms is suggestive of cervical radiculopathy.2 Table 1 lists alternative diagnoses for shoulder pain and their distinguishing findings.6
TABLE 1 Adhesive Capsulitis: Alternative Diagnoses
| Condition | Distinguishing physical examination findings | Distinguishing histologic findings | Diagnostic tests |
|---|---|---|---|
| Acromioclavicular arthropathy | Positive cross-arm adduction and compression testing; glenohumeral range of motion is preserved | Localizes over acromioclavicular joint (superiorly); history of repetitive overuse (e.g., weight lifting) | Radiography |
| Autoimmune disease (e.g., systemic lupus erythematosus, rheumatoid arthritis) | Malar rash; synovitis (tenderness and effusions) in other joints | Multisystem involvement; multiple joints involved | Antinuclear antibody testing; rheumatoid factor test |
| Biceps tendinopathy | Tenderness over long head of the biceps tendon; positive Speed or Yergason test | Localizes anteriorly | MRI (radiography may determine whether calcifications are present) |
| Cervical disk degeneration | Limited range of motion in neck and pain with active movement; intrinsic hand weakness; impaired light touch | Localizes posteriorly; hand numbness and weakness in radiculopathy | Cervical spine radiography |
| Glenohumeral osteoarthritis | Similar to adhesive capsulitis; shoulder girdle atrophy may be present | History of shoulder trauma or surgery; older age | Plain radiography |
| Neoplasm | Similar to adhesive capsulitis | Fevers, night sweats, unexplained weight loss (if advanced); dyspnea or cough (if Pancoast tumor present) | Plain radiography, MRI |
| Rotator cuff tendinopathy or tear, with or without impingement | Passive range of motion is preserved; painful arc, focal tenderness, positive Hawkins and Neer tests | Possible history of repetitive overuse; often localizes anteriorly or laterally | MRI (radiography may determine whether calcifications are present) |
| Subacromial and subdeltoid bursitis | Passive range of motion is preserved | Possible history of repetitive overuse | Diagnostic subacromial lidocaine injection, MRI |
Note: Secondary adhesive capsulitis can also result from these conditions.
MRI = magnetic resonance imaging.
Adapted with permission from Ewald A. Adhesive capsulitis: a review. Am Fam Physician. 2011;83(4):418.
Impaired range of motion with forward flexion, abduction, and external and internal rotation is the cardinal clinical finding for adhesive capsulitis. In advanced disease, observation of a patient's gait may reveal a loss in the natural arm swing that occurs with walking. Further examination of the affected shoulder may reveal muscular atrophy. Palpation may produce vague tenderness over the anterior and posterior shoulder; however, focal tenderness is uncommon and suggests an alternative diagnosis or concomitant pathology in the shoulder.
Diagnostic Testing
A fasting glucose or A1C level, or a thyroid-stimulating hormone measurement may be considered for patients at risk of or with signs and symptoms of diabetes and thyroid disease, respectively.4,6 Additional blood tests are not indicated to support a diagnosis of adhesive capsulitis.
Radiography may be useful in ruling out other pathologies of the shoulder joint such as advanced glenohumeral arthritis, pathologic fracture, avascular necrosis, and calcific rotator cuff tendinopathy, if suggested by clinical history and examination. Radiography is less helpful in detecting glenohumeral joint capsule pathology because it comprises soft tissue and is therefore not visible.
A 2017 study concluded that adhesive capsulitis can be accurately and consistently diagnosed with noncontrast magnetic resonance imaging (MRI) of the shoulder in conjunction with appropriate clinical criteria.7 MRI findings of coracohumeral ligament thickening, rotator interval infiltration of the subcoracoid fat, and axillary recess thickening yield high specificity for adhesive capsulitis. However, the diagnosis of adhesive capsulitis is a clinical diagnosis and the use of MRI should be reserved for the evaluation of other sources of shoulder pathology, not to confirm a diagnosis of adhesive capsulitis.
Treatment
The most effective treatment for adhesive capsulitis is still uncertain. Nonsurgical treatments include physiotherapy, oral or intra-articular corticosteroids, acupuncture, and hydrodilatation. Arthroscopic capsular release and manipulation under anesthesia are options in patients who do not improve with nonsurgical treatments.
NONSURGICAL TREATMENTS
Nonsteroidal anti-inflammatory drugs (NSAIDs) are often prescribed for pain relief; however, there is little evidence for their effectiveness in treating adhesive capsulitis specifically. A systematic review showed clinically significant improvement of pain in patients with various etiologies of shoulder pain treated with NSAIDs compared with placebo; however, the studies reviewed were generally small and of poor or moderate quality.4 A 2006 Cochrane review concluded that oral corticosteroids may produce a small short-term benefit (less than six weeks) in pain relief and improved range of motion, but it was not maintained in the long-term.8 Given the risks associated with extended oral corticosteroid usage, and the lack of long-term benefit, oral corticosteroids should not be used routinely to treat adhesive capsulitis.
Evidence suggests that intra-articular corticosteroid injections are more effective than placebo for pain relief in the short-term, but results vary in the long-term.6,9 A 2015 systematic review and meta-analysis of eight randomized controlled trials compared NSAIDs with corticosteroid injection in patients with shoulder pain of various etiologies that were not limited to adhesive capsulitis. The review concluded that compared with placebo, corticosteroid injection provided slightly more improvement in shoulder function (standardized mean deviation = 0.61; 95% CI, 0.08 to 1.14) but a similar degree of pain relief at four to six weeks.10
Physiotherapy has traditionally been used to treat adhesive capsulitis despite a lack of high-level studies demonstrating benefit over observation or medical therapy alone.9 A 2015 systematic review found fair evidence that manual mobilization techniques with exercise provided an increased range of motion and function in persons with adhesive capsulitis.11 Outcomes of intra-articular corticosteroid injections have been compared with physiotherapy, with varying results. A 2010 systematic review found that both interventions were effective compared with placebo; corticosteroid injection was superior to physiotherapy in improving shoulder function from six to seven weeks to 26 weeks following intervention, and was as effective as physiotherapy in pain relief at six to seven weeks and lasted up to 26 weeks.12 A 2015 systematic review of nine randomized controlled trials totaling 453 patients found no difference in functional improvement or pain relief between corticosteroid injection or physiotherapy.10 When combined, physiotherapy and corticosteroid injections may provide greater improvement than physiotherapy alone.13
There is limited evidence that shows that acupuncture can improve pain and function for two to four weeks in patients with shoulder pain.14 A 2017 randomized controlled trial demonstrated an immediate improvement in pain scores in patients with adhesive capsulitis who received acupuncture with physiotherapy. These results suggest that integrating acupuncture with conservative therapy may reduce time to pain relief compared with physiotherapy alone.15
Hydrodilatation (arthroscopic distension) is a nonoperative treatment that involves an injection of local anesthetic into the shoulder capsule at high pressure to distend and stretch the joint capsule. A randomized controlled study of 46 patients compared hydrodilatation with placebo and demonstrated statistically and clinically significant improvement in functional outcome scores at six weeks following intervention.16 A more recent systematic review concluded the combination of hydrodilatation and corticosteroid injection may potentially expedite recovery of pain free range of motion compared with corticosteroid injection alone, with the greatest benefit experienced within the first three months of intervention.17
SURGICAL TREATMENT
Surgical options for adhesive capsulitis include manipulation under anesthesia and arthroscopic capsule release. Manipulation is a technique performed under general anesthesia where the humerus is manipulated in an attempt to disrupt adhesions. Moderate evidence suggests that manipulation alleviates pain and can improve range of motion when followed by early physiotherapy.18
For patients with adhesive capsulitis who have minimal improvement in pain and who cannot tolerate their symptoms after six to 12 weeks of nonsurgical treatment, referral to an orthopedic surgeon may be considered.
This article updates previous articles on this topic by Ewald,6 and by Siegel, et al.19
Data Sources: A PubMed search was completed in Clinical Queries using the terms adhesive capsulitis, frozen shoulder, corticosteroid injection, and physiotherapy. The search included meta-analyses, randomized controlled trials, and reviews. Search dates: October 2017 and January 2019.

