Summary of Recommendations and Evidence
The USPSTF recommends that clinicians screen for intimate partner violence (IPV) in women of reproductive age and provide or refer women who screen positive to ongoing support services (Table 1). B recommendation.
TABLE 1 Screening for Intimate Partner Violence, Elder Abuse, and Abuse of Vulnerable Adults: Clinical Summary of the USPSTF Recommendation
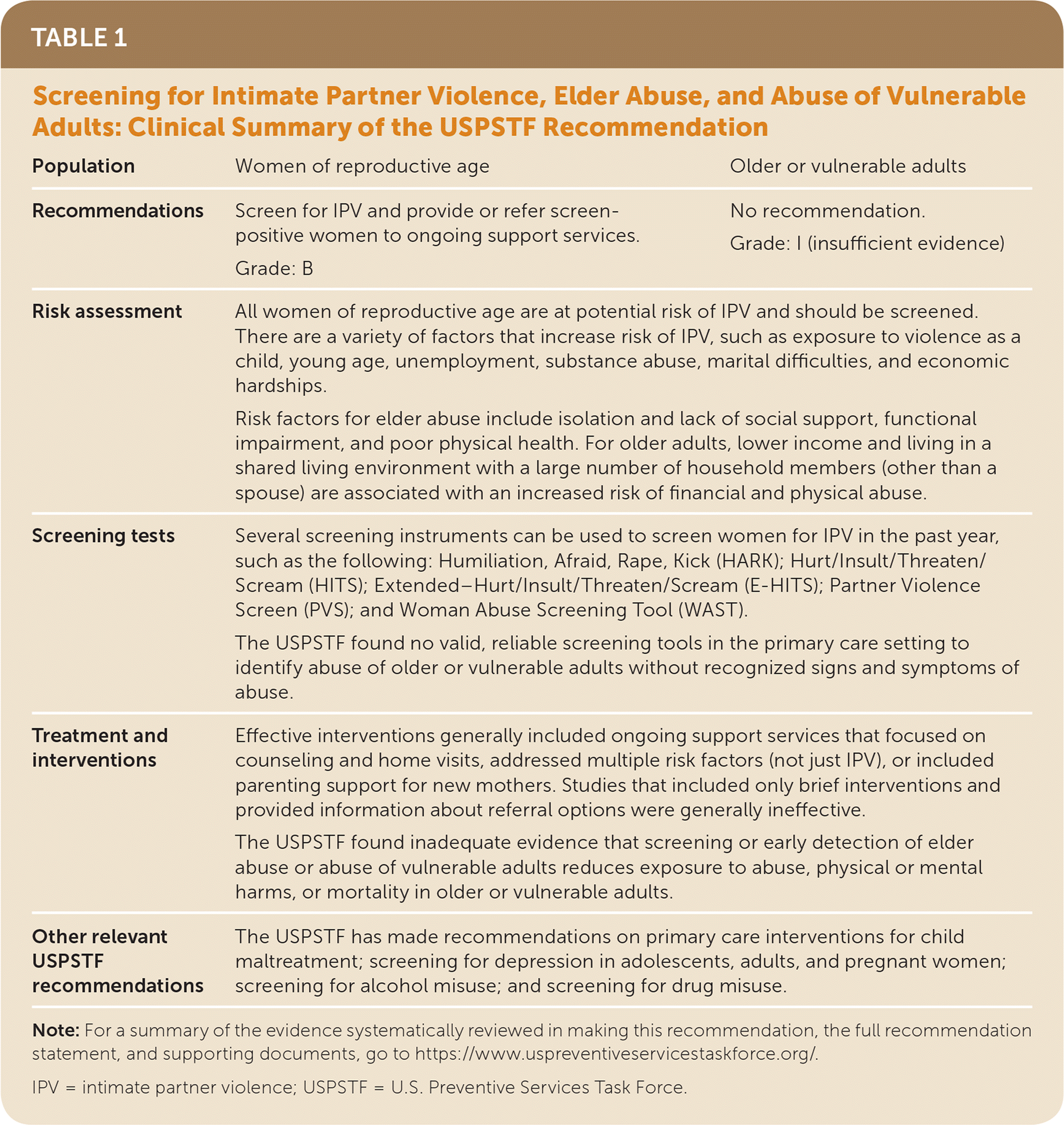
| Population | Women of reproductive age | Older or vulnerable adults |
| Recommendations | Screen for IPV and provide or refer screen-positive women to ongoing support services. Grade: B | No recommendation. Grade: I (insufficient evidence) |
| Risk assessment | All women of reproductive age are at potential risk of IPV and should be screened. There are a variety of factors that increase risk of IPV, such as exposure to violence as a child, young age, unemployment, substance abuse, marital difficulties, and economic hardships. Risk factors for elder abuse include isolation and lack of social support, functional impairment, and poor physical health. For older adults, lower income and living in a shared living environment with a large number of household members (other than a spouse) are associated with an increased risk of financial and physical abuse. | |
| Screening tests | Several screening instruments can be used to screen women for IPV in the past year, such as the following: Humiliation, Afraid, Rape, Kick (HARK); Hurt/Insult/Threaten/Scream (HITS); Extended–Hurt/Insult/Threaten/Scream (E-HITS); Partner Violence Screen (PVS); and Woman Abuse Screening Tool (WAST). The USPSTF found no valid, reliable screening tools in the primary care setting to identify abuse of older or vulnerable adults without recognized signs and symptoms of abuse. | |
| Treatment and interventions | Effective interventions generally included ongoing support services that focused on counseling and home visits, addressed multiple risk factors (not just IPV), or included parenting support for new mothers. Studies that included only brief interventions and provided information about referral options were generally ineffective. The USPSTF found inadequate evidence that screening or early detection of elder abuse or abuse of vulnerable adults reduces exposure to abuse, physical or mental harms, or mortality in older or vulnerable adults. | |
| Other relevant USPSTF recommendations | The USPSTF has made recommendations on primary care interventions for child maltreatment; screening for depression in adolescents, adults, and pregnant women; screening for alcohol misuse; and screening for drug misuse. | |
Note: For a summary of the evidence systematically reviewed in making this recommendation, the full recommendation statement, and supporting documents, go to https://www.uspreventiveservicestaskforce.org/.
IPV = intimate partner violence; USPSTF = U.S. Preventive Services Task Force.
See the Clinical Considerations section for more information on effective ongoing support services for IPV and for information on IPV in men.
The USPSTF concludes that the current evidence is insufficient to assess the balance of benefits and harms of screening for abuse and neglect in all older or vulnerable adults. I statement.
See the Clinical Considerations section for suggestions for practice regarding the I statement.
Rationale
IMPORTANCE
IPV and abuse of older or vulnerable adults are common in the United States but often remain undetected. Although estimates vary, IPV (including sexual violence, physical violence, and stalking) is experienced by approximately 36% of U.S. women and 33% of U.S. men during their lifetime. Severe physical violence is experienced by 21% of U.S. women and 15% of U.S. men during their lifetime.1 Prevalence rates vary by age, race/ethnicity, and income. Estimates also vary for prevalence of elder abuse and abuse of vulnerable adults. A 2008 nationwide survey of U.S. adults 60 years or older found that the prevalence of any abuse or neglect in the past year was 10%.2 A 2004 survey of Adult Protective Services (APS) agencies found 40,848 substantiated reports of vulnerable adult abuse (in those aged 18 to 59 years) in 19 states.3
In addition to the immediate effects of IPV, such as injury and death, there are other health consequences, many with long-term effects, including development of mental health conditions such as depression, posttraumatic stress disorder, anxiety disorders, substance abuse, and suicidal behavior; sexually transmitted infections; unintended pregnancy; and chronic pain and other disabilities.4,5 Violence during pregnancy is associated with preterm birth and low birth weight 6 and adverse effects on maternal and infant health, including postpartum mental health problems7 and hospitalization during infancy.8
Long-term negative health effects from elder abuse include death,9 higher risk of nursing home placement10 among those referred to APS, and adverse psychological consequences (distress, anxiety, and depression).11
DETECTION
The USPSTF found adequate evidence that available screening instruments can identify IPV in women. The USPSTF found limited evidence about the performance of IPV screening instruments in men.
The USPSTF found inadequate evidence to assess the accuracy of screening instruments designed to detect elder abuse or abuse of vulnerable adults when there are no recognized signs and symptoms of abuse.
BENEFITS OF DETECTION AND EARLY INTERVENTION
The USPSTF found adequate evidence that effective interventions that provide or refer women to ongoing support services can reduce violence, abuse, and physical or mental harms in women of reproductive age. However, the USPSTF found inadequate direct evidence that screening for IPV can reduce violence, abuse, and physical or mental harms.
The recommendation on screening for IPV applies to women of reproductive age because the evidence demonstrating benefit of ongoing support services is predominantly found in studies of pregnant or postpartum women. The USPSTF extrapolated the evidence pertaining to interventions with ongoing support services from pregnant and postpartum women to all women of reproductive age.
The USPSTF found no studies on screening or interventions for IPV in men.
The USPSTF found inadequate evidence that screening or early detection of elder abuse or abuse of vulnerable adults reduces exposure to abuse, physical or mental harms, or mortality in older or vulnerable adults.
HARMS OF DETECTION AND EARLY INTERVENTION
The USPSTF found inadequate evidence to determine the harms of screening or interventions for IPV. Limited evidence showed no adverse effects of screening or interventions for IPV. The USPSTF determined that the magnitude of the overall harms of screening and interventions for IPV can be bounded as no greater than small. When direct evidence is limited, absent, or restricted to select populations or clinical scenarios, the USPSTF may place conceptual upper or lower bounds on the magnitude of benefit or harms.
The USPSTF found inadequate evidence on the harms of screening or interventions for elder abuse or abuse of vulnerable adults.
Clinical Considerations
PATIENT POPULATION UNDER CONSIDERATION
This recommendation applies to women of reproductive age and older or vulnerable adults without recognized signs and symptoms of abuse. The studies reviewed for IPV included adolescents to women in their 40s.
See below for suggestions for practice regarding men and older and vulnerable adults.
DEFINITIONS OF IPV AND ELDER ABUSE
The term intimate partner violence refers to physical violence, sexual violence, psychological aggression (including coercive tactics, such as limiting access to financial resources), or stalking by a romantic or sex partner, including spouses, boyfriends, girlfriends, dates, and casual “hookups.” Severe physical violence includes being hit with a fist or something hard, kicked, hurt by pulling hair, slammed against something, hurt by choking or suffocating, beaten, burned on purpose, or threatened with a knife or gun.1
The term elder abuse refers to acts whereby a trusted person (e.g., a caregiver) causes or creates risk of harm to an older adult.12 According to the Centers for Disease Control and Prevention, an older adult is considered to be 60 years or older.12 The legal definition of vulnerable adult varies by state but is generally defined as a person who is or may be mistreated and who, because of age, disability, or both, is unable to protect him or herself.3 Types of abuse that apply to older or vulnerable adults include physical abuse, sexual abuse, emotional or psychological abuse, neglect, abandonment, and financial or material exploitation.
ASSESSMENT OF RISK
Although all women of reproductive age are at potential risk for IPV and should be screened, a variety of factors increase risk of IPV, such as exposure to violence as a child, young age, unemployment, substance abuse, marital difficulties, and economic hardships.13 However, the USPSTF did not identify any risk assessment tools that predict greater likelihood of IPV in populations with these risk factors.
Risk factors for elder abuse include isolation and lack of social support, functional impairment, and poor physical health.14 For older adults, lower income and living in a shared living environment with a large number of household members (other than a spouse) are associated with an increased risk of financial and physical abuse.15
SCREENING TESTS
Several screening instruments can be used to screen women for IPV. The following instruments accurately detect IPV in the past year among adult women: Humiliation, Afraid, Rape, Kick (HARK); Hurt, Insult, Threaten, Scream (HITS); Extended–Hurt, Insult, Threaten, Scream (E-HITS); Partner Violence Screen (PVS); and Woman Abuse Screening Tool (WAST).
HARK includes 4 questions that assess emotional and physical IPV in the past year. HITS includes 4 items that assess the frequency of IPV, and E-HITS includes an additional question to assess the frequency of sexual violence. PVS includes 3 items that assess physical abuse and safety. WAST includes 8 items that assess physical and emotional IPV.
Most studies included only women who could be separated from their partners during screening, during the intervention, or both so that screening and the intervention could be delivered in private.
State and local reporting requirements vary from one jurisdiction to another, with differences in definitions, who and what should be reported, who should report, and to whom. Some states require clinicians (including primary care providers) to report abuse to legal authorities, and most require reporting of injuries resulting from guns, knives, or other weapons.16 For elder abuse, mandatory reporting laws and regulations also vary by state; however, most states require reporting.17
The USPSTF found no valid, reliable screening tools in the primary care setting to identify IPV in men without recognized signs and symptoms of abuse.
The USPSTF found no valid, reliable screening tools in the primary care setting to identify abuse of older or vulnerable adults without recognized signs and symptoms of abuse.
SCREENING INTERVAL
The USPSTF found no evidence on appropriate intervals for screening. Randomized clinical trials of screening and interventions for IPV often screen for current IPV or IPV in the past year.
INTERVENTIONS
No studies definitively identified which intervention components resulted in positive outcomes. However, based on the evidence from 3 studies,18–20 effective interventions generally included ongoing support services that focused on counseling and home visits, addressed multiple risk factors (not just IPV), or included parenting support for new mothers. These studies were conducted in pregnant or postpartum women. Studies that included only brief interventions and provided information about referral options were generally ineffective.
SUGGESTIONS FOR PRACTICE REGARDING THE I STATEMENT AND OTHER POPULATIONS
Potential Preventable Burden: Older or Vulnerable Adults. Prevalence estimates of elder abuse and abuse of vulnerable adults vary. A 2008 nationwide survey of U.S. adults 60 years or older found that the prevalence of any abuse or potential neglect in the past year was 10%.21 Elder abuse has a number of long-term negative health effects, including death,9 higher risk of nursing home placement10 among those referred to APS, and adverse psychological consequences (distress, anxiety, and depression).11 A 2004 survey of APS agencies identified 40,848 substantiated reports of vulnerable adult abuse (in those aged 18 to 59 years) in 19 states.3
Potential Preventable Burden: Women Not of Reproductive Age. Based on the age categories reported by the Centers for Disease Control and Prevention, approximately 4% of women aged 45 to 54 years and more than 1% of women 55 years or older have experienced rape, physical violence, or stalking by an intimate partner in the past 12 months.22
Potential Preventable Burden: Men. More than 33% of men have experienced sexual violence, physical violence, or stalking by an intimate partner in their lifetime.1 Approximately 34% of men report any psychological aggression by an intimate partner in their lifetime. Among men who experience sexual violence, physical violence, or stalking, more than 10% experience at least 1 form of an IPV-related adverse effect, such as feeling fearful, feeling concerned for safety, injury, missing days of work or school, and needing medical care.1
POTENTIAL HARMS
Some potential harms of screening in older or vulnerable adults, women not of reproductive age, and men are shame, guilt, self-blame, retaliation or abandonment by perpetrators, partner violence, and the repercussions of false-positive results (e.g., labeling and stigma).
CURRENT PRACTICE
Older or Vulnerable Adults. Limited evidence suggests that screening is not commonly occurring in practice; 1 study found that more than 60% of clinicians have never asked their older adult patients about abuse.23
Women. While not specific to age, evidence suggests that screening for IPV is not commonly occurring in practice. A recent systematic review found that rates of routine screening vary and are typically low, ranging from 2% to 50% of clinicians reporting “always” or “almost always” routinely screening for IPV.24
Men. No data are available on current screening practice in men.
ADDITIONAL APPROACHES TO PREVENTION
The Health Resources and Services Administration (HRSA) Strategy to Address Intimate Partner Violence (2017 to 2020) identifies priorities for reducing IPV, including training the health care and public health workforce to address IPV.25 HRSA also developed a toolkit26 for clinicians and health centers to help implement screening and interventions for IPV. The National Hotline on Domestic Violence has information about local programs and resources across the country.27 The Administration for Children and Families has funded a compendium of state statutes and policies on domestic violence and health care.28
The Centers for Disease Control and Prevention,29 Substance Abuse and Mental Health Services Administration–HRSA Center for Integrated Health Solutions,30 U.S. Department of Veterans Affairs,31 Administration for Community Living,32 and the Administration on Aging's National Center for Elder Abuse33 also have additional resources available for clinicians.
USEFUL RESOURCES
The USPSTF has made recommendations on primary care interventions for child maltreatment34; screening for depression in adolescents,35 adults, and pregnant women36; screening for alcohol misuse37; and screening for drug misuse.38
This recommendation statement was first published in JAMA. 2018;320(16):1678-1687.
The “Other Considerations,” “Discussion,” “Update of Previous USPSTF Recommendation,” and “Recommendations of Others” sections of this recommendation statement are available at https://www.uspreventiveservicestaskforce.org/Page/Document/RecommendationStatementFinal/intimate-partner-violence-and-abuse-of-elderly-and- vulnerable-adults-screening1.
The USPSTF recommendations are independent of the U.S. government. They do not represent the views of the Agency for Healthcare Research and Quality, the U.S. Department of Health and Human Services, or the U.S. Public Health Service.
This summary is one in a series excerpted from the Recommendation Statements released by the USPSTF. These statements address preventive health services for use in primary care clinical settings, including screening tests, counseling, and preventive medications.
The complete version of this statement, including supporting scientific evidence, evidence tables, grading system, members of the USPSTF at the time this recommendation was finalized, and references, is available on the USPSTF website at https://www.uspreventiveservicestaskforce.org/.

