A 24-year-old woman presented with several months of increasingly problematic foot odor. She noted that there were accompanying skin changes on the soles of her feet but no itching, redness, or discharge. She had no improvement with use of various deodorants, frequent washing, and frequent sock changes. When coworkers complained about the odor, she presented for evaluation.
Physical examination revealed small pits in the skin on her soles (Figure 1) along with the foot odor. There was a slight scale over the plantar surface of both feet. Wood light examination did not show fluorescence but showed that the pits were more extensive than what was apparent with room light (Figure 2).
FIGURE 1
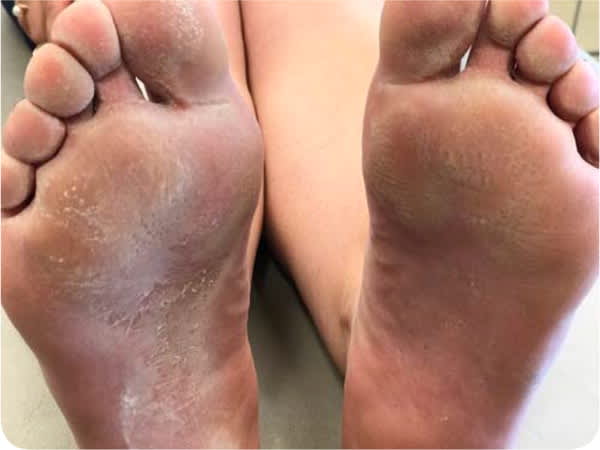
FIGURE 2
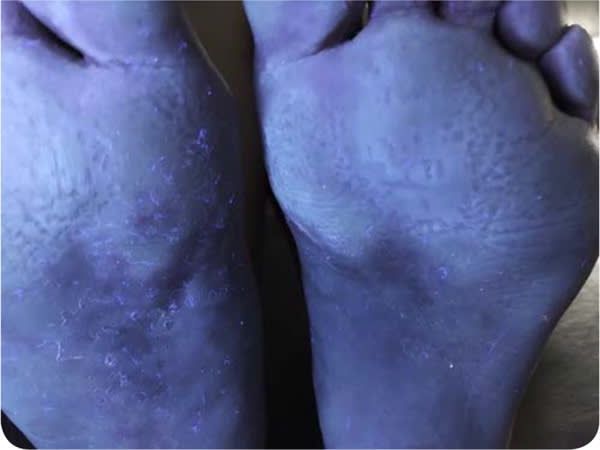
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Hyperhidrosis.
B. Palmoplantar hyperkeratosis.
C. Pitted keratolysis.
D. Tinea pedis.
Discussion
The answer is C: pitted keratolysis. The combination of pits on the weight-bearing areas of the feet and a very unpleasant foot odor is a hallmark of this condition. Pitted keratolysis most often occurs in individuals whose feet have excessive exposure to a damp environment, such as with hyperhidrosis (excessive sweating), frequent immersion in water, or occlusive footwear in a hot environment. The skin becomes macerated and develops bacterial overgrowth. Several bacterial species have been identified as causative agents. Some of these can cause fluorescence on Wood light examination if the feet have not been recently washed. The odor is thought to be due to the breaking of sulfhydryl bonds in the keratin layer.1
Treatment of pitted keratolysis is directed at the bacterial infection, as well as decreasing the risk factors for the condition. Wetness from hyperhidrosis should be treated with effective antiperspirants. Immersion of the feet into water should be limited if possible, and breathable shoes should be worn to promote drying. The bacterial infection usually responds to topical antibacterial agents. Clindamycin and erythromycin, alone and combined with benzoyl peroxide, have been successfully used.2 This patient was advised to discard her current footwear and get new shoes. She was successfully treated with aluminum chloride 20% topical solution (Drysol) plus topical clindamycin.
Hyperhidrosis is a condition of excessive sweating that is not related to heat or emotions. It occurs in up to 2% of the adult population.3 The chronic moisture can cause maceration and occasionally erythema. Hyperhidrosis can contribute to the risk of developing pitted keratolysis, but it does not include the bacterial growth seen with pitted keratolysis.
Palmoplantar hyperkeratosis refers to a group of conditions that cause thickened, often cracked skin on the palms and the soles. Several of these conditions are believed to be genetic. The thickened skin of the soles can have an odor; however, it is not as strong as with pitted keratolysis, and there is no pitting.
Tinea pedis is a fungal infection of the skin. It occurs in two patterns: a dry, scaly rash without erythema, often over the area covered by a shoe (moccasin tinea), or a more inflammatory pattern with itching, redness, and vesicles. Interdigital involvement by Candida species can lead to a “yeasty” smell, but the odor is much less strong than with pitted keratolysis, and there is no pitting.
SUMMARY TABLE
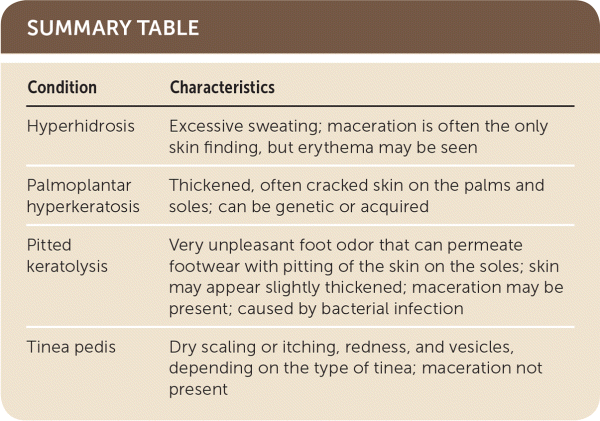
| Condition | Characteristics |
|---|---|
| Hyperhidrosis | Excessive sweating; maceration is often the only skin finding, but erythema may be seen |
| Palmoplantar hyperkeratosis | Thickened, often cracked skin on the palms and soles; can be genetic or acquired |
| Pitted keratolysis | Very unpleasant foot odor that can permeate footwear with pitting of the skin on the soles; skin may appear slightly thickened; maceration may be present; caused by bacterial infection |
| Tinea pedis | Dry scaling or itching, redness, and vesicles, depending on the type of tinea; maceration not present |


