A 10-year-old girl was brought to the family medicine clinic by her mother with a painful lesion on the left upper gum. The lesion was first noted about two months before the visit, when it was approximately 3 mm in diameter. The lesion had gradually increased in size. There was no discharge, but the patient had noticed a change in sensation in her gum. She had no constitutional symptoms or history of injury to the permanent tooth. However, the mother recalled that one of her baby teeth was pulled in preparation for braces two years earlier.
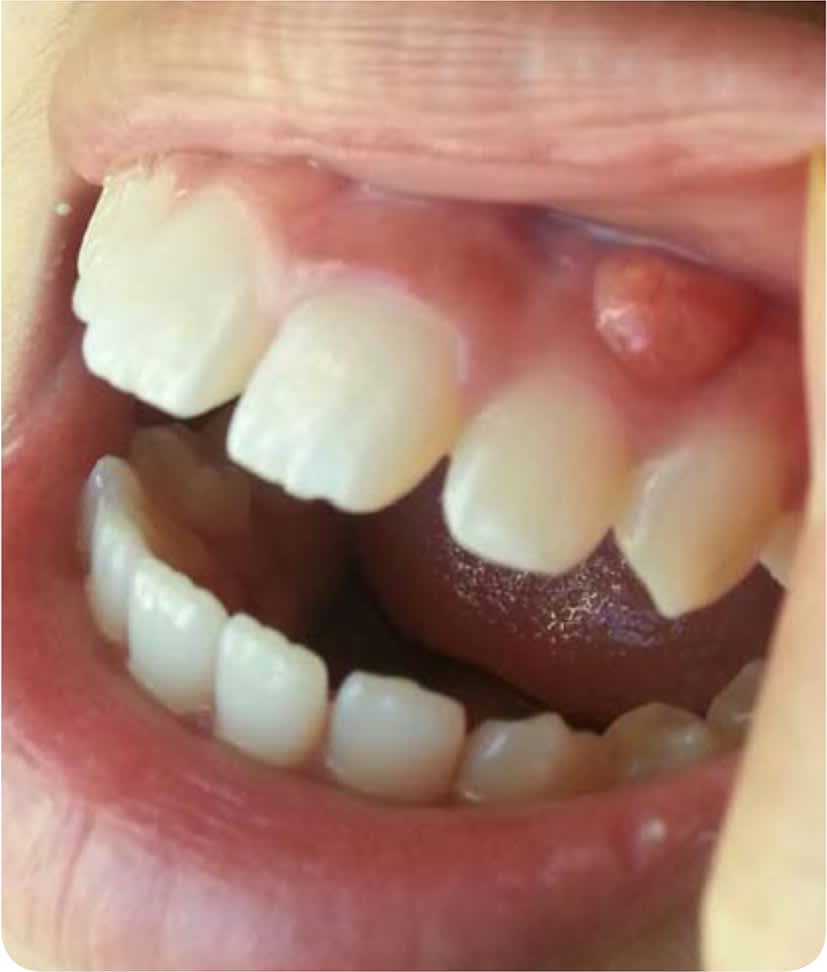
Physical examination revealed a lesion on the left upper anterior gingiva above the canine tooth (Figure 1). The round, erythematous lesion measured 8 mm in diameter. It was firm, nonpulsatile, and tender to palpation, and it did not bleed.
FIGURE 1
Question
Based on the patient's history and physical examination findings, which one of the following is the most likely diagnosis?
A. Dental abscess.
B. Langerhans cell histiocytosis.
C. Mucocele.
D. Pyogenic granuloma.
Discussion
The answer is A: dental abscess. Dental abscess is a subtype of odontogenic infection, which is one of the most common diseases of the oral and maxillofacial region.1 Classifications of dental abscess include periapical, periodontal, gingival, pericoronal, and combined periodontal-endodontic. Pain is one of the most common symptoms of dental abscess for which patients seek medical attention. The pain is usually moderate to severe and can be intermittent or persistent and sharp, throbbing, or shooting. Pain is absent in some acute cases. Swelling is almost always present, whether it is the acute or subacute phase. Patients sometimes describe a toothache with sensitivity to hot and cold and may have a history of a recent dental procedure.
Odontogenic infection is diagnosed with physical examination and imaging findings. The choice of imaging study varies with clinical setting. Computed tomography is particularly sensitive for osseous structures and is the modality of choice for most odontogenic infections.2 Fluid collection and tissue biopsies should be examined for evidence of acute or chronic inflammation and infection.
A spreading infection is more serious than localized swelling of gingival tissue, because the infection could spread outward from the root of the tooth throughout the bone and periosteum.3 Failure to recognize a systemic infection can lead to chronic infections or life-threatening complications, such as airway obstruction, mediastinitis, necrotizing fasciitis, cavernous sinus thrombosis, cerebral abscess, orbital abscess, and sepsis.4 Severe complications require intravenous antibiotics, incision and drainage, and probable removal of the source of infection.3 A localized infection is usually not urgent and can be managed in the outpatient setting.
Langerhans cell histiocytosis is a rare histiocytic disorder that most commonly affects children one to three years of age, although it can occur at any age. In young children, it is an acute disseminated multisystem disease.5 Bone and skin are most commonly affected. There is oral involvement in about 13% of cases,6 usually manifesting as an intraoral mass, gingivitis, mucosal ulcers, and loose teeth. Lesions of the bones or soft tissue are painful.7
Mucocele is an area of mucin drainage in soft tissue resulting from rupture of a salivary duct. Mucocele is most common in children and young adults who usually have multiple episodes of swelling lesions with periodic rupture. Long-standing lesions may develop fibrosis, which is nontender on palpation.8 Mucocele is most commonly located on the inside of the lower lip.9
Pyogenic granuloma is a rapidly growing lesion that develops in response to local irritations, such as poor hygiene, overhanging dental fillings, and trauma. The lesion can be from millimeters to centimeters in diameter. Pyogenic granulomas are erythematous, nonpainful, and smooth, and bleed easily when touched.8
SUMMARY TABLE

| Condition | Characteristics |
|---|---|
| Dental abscess | Moderate to severe pain, swelling, sensitivity to hot and cold; may have history of a recent dental procedure |
| Langerhans cell histiocytosis | Bone and skin are most commonly affected; oral involvement is possible, most often manifesting as an intraoral mass, gingivitis, mucosal ulcers, and loose teeth; most common in children one to three years of age |
| Mucocele | Multiple episodes of swelling with periodic rupture, nontender, often appears inside the lower lip, most common in young children |
| Pyogenic granuloma | Rapidly growing, erythematous, nonpainful, smooth lesions that bleed easily |

