The relationship between alcohol use and health is often misunderstood by physicians and patients because of prior research suggesting that low levels of alcohol consumption are associated with improved cardiovascular health outcomes. However, more recent evidence suggests that a dose response occurs between alcohol use and negative health outcomes, specifically with increasing risk for all-cause mortality and cancer incidence.1 Consequently, the U.S. Preventive Services Task Force recently reaffirmed its previous grade B recommendation to screen adults 18 years or older for unhealthy alcohol use and to provide brief behavioral counseling interventions to those who screen positive.2 We have identified the ways in which family physicians can implement this screening recommendation and then intervene when a patient has a positive screen.
How Do I Screen for Unhealthy Alcohol Use in a Busy Primary Care Practice?
The National Institute on Alcohol Abuse and Alcoholism recommends asking a single screening question: How many times in the past year have you had five (four for women) or more drinks in a day? This question has good sensitivity (between 73% and 88%) and specificity (between 74% and 100%) for detecting unhealthy alcohol use in U.S. primary care settings.3 If the patient's response is one or more, a more detailed instrument such as the Alcohol Use Disorders Identification Test (AUDIT; http://auditscreen.org/) is recommended. The AUDIT is a validated 10-question tool developed by the World Health Organization to risk-stratify patients for targeted interventions.
What Is a Practical Way to Identify an Appropriate Intervention for Patients with Unhealthy Alcohol Use?
The AUDIT assesses consumption, drinking behaviors, and alcohol-related problems. Scores range from 0 to 40, with a higher score indicating higher-risk alcohol use. There is no universal consensus regarding cutoff scores for specific types of intervention; however, the World Health Organization recommends brief counseling (sometimes referred to as brief intervention) for patients who have scores between 8 and 15, with a goal of reducing consumption levels. Patients who have scores between 16 and 19 enter the next tier of risk; current recommendations are to engage the patient in counseling with continued monitoring. This level of intervention may be delivered by the primary care physician, a co-located behavioral health professional, or an outside treatment provider.4 Scores of 20 or more indicate that the patient may have a moderate to severe alcohol use disorder, and referral to alcohol use disorder treatment is appropriate, as is a conversation about initiation of medication for treatment of alcohol use disorder.
What Is a Brief Intervention for Unhealthy Alcohol Use?
Brief (five- to 10-minute) multicontact counseling interventions seem to have the best evidence of effectiveness. Counseling interventions typically include discussing the patient's alcohol use compared with national norms, patient-specific adverse alcohol effects, and mutual agreements to specific drinking amounts. This type of normative feedback can be used alone or in combination with motivational interviewing. A recent meta-analysis found that brief interventions reduced unhealthy alcohol use with a decrease of 1.6 drinks per week, as compared with those in control groups. Because the negative health outcomes related to unhealthy alcohol use have a dose response, any statistically significant reduction in alcohol use is viewed as a successful intervention. The same meta-analysis also found that the intervention groups had a reduction in the proportion who exceed recommended drinking limits and the proportion who report heavy-drinking episodes.3 The Substance Abuse and Mental Health Services Administration has published a handout that is helpful in guiding the intervention conversation (https://www.samhsa.gov/sites/default/files/alcohol-use-facts-resources-fact-sheet.pdf), and an FPM article contains a video showing a primary care example of discussing unhealthy alcohol use (https://www.aafp.org/fpm/2017/0500/p12.html).
How Do I Utilize Other Clinicians and Staff to Help Patients with Unhealthy Alcohol Use?
There is increasing evidence that team-based care is more effective when trying to help people change potentially harmful activities and habits such as unhealthy alcohol use.5 Clinicians who normally take vitals and prepare patients for the physician can also administer the alcohol screening questions and update electronic medical record documentation. The physician can then review the screening information and formulate a treatment plan. This could include spending several minutes talking to the patient about alcohol use, asking the patient to see someone else in the clinic who is trained in brief intervention and motivational interviewing, or referral to an addiction subspecialist or substance use disorder treatment center. Even a small clinic with two or three physicians may want to have a nurse or masters-level licensed counselor trained in motivational interviewing and cognitive behavior therapy to help support patients in behavior change.
How Do I Use Medications to Help Patients Reduce Alcohol Use?
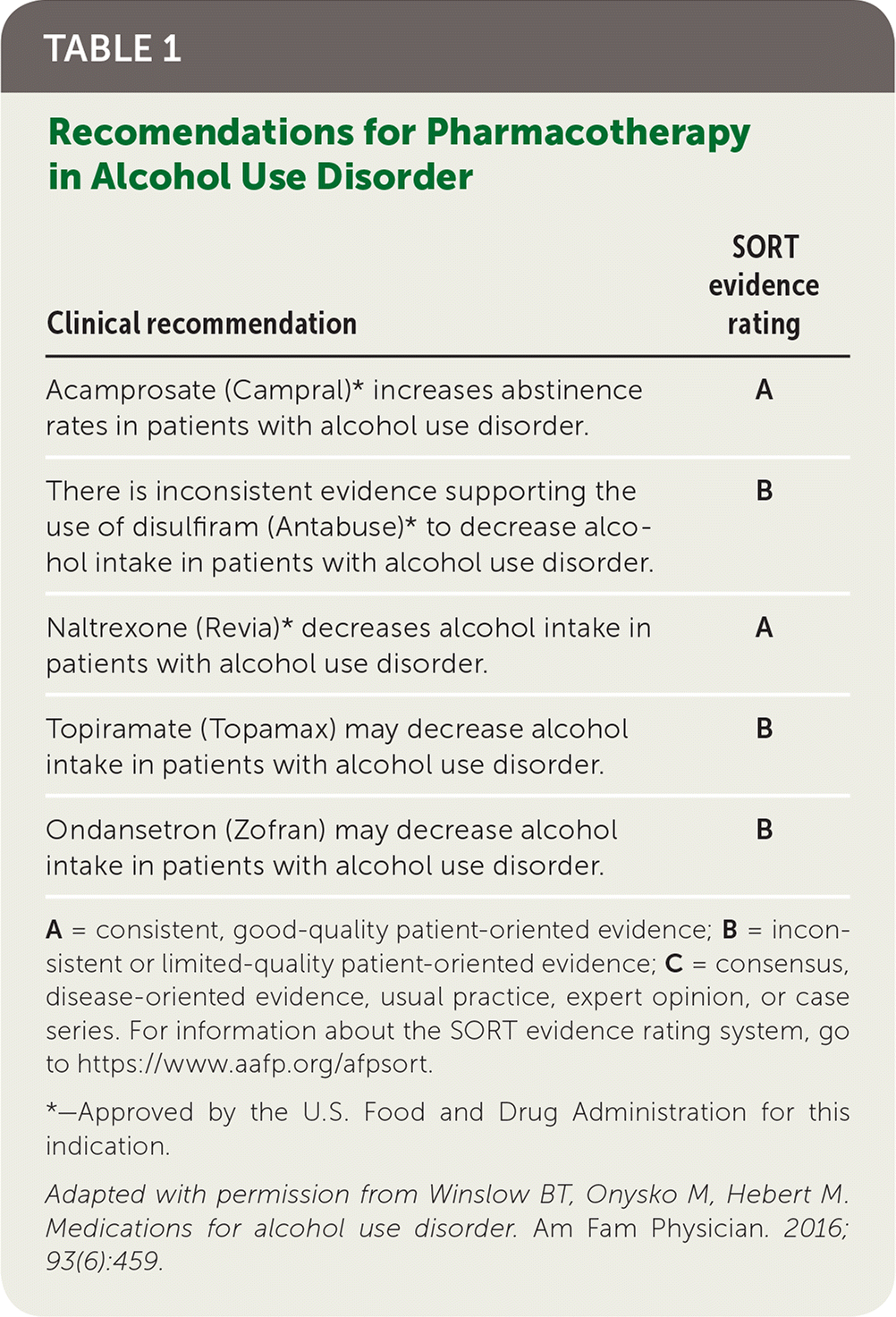
As few as 10% of people with alcohol use disorder receive pharmacotherapy.6 Medications that reduce alcohol craving are underused for multiple reasons, including costs, lack of physician training, negative physician perceptions or experiences, patient resistance, and societal biases.7 Medications for alcohol use disorder and their SORT evidence rating are shown in Table 1.8 An Amercian Family Physician article provides more information about medications used to treat alcohol use disorder (https://www.aafp.org/afp/2016/0315/p457.html).
TABLE 1 Recomendations for Pharmacotherapy in Alcohol Use Disorder
| Clinical recommendation | SORT evidence rating |
|---|---|
| Acamprosate (Campral)* increases abstinence rates in patients with alcohol use disorder. | A |
| There is inconsistent evidence supporting the use of disulfiram (Antabuse)* to decrease alcohol intake in patients with alcohol use disorder. | B |
| Naltrexone (Revia)* decreases alcohol intake in patients with alcohol use disorder. | A |
| Topiramate (Topamax) may decrease alcohol intake in patients with alcohol use disorder. | B |
| Ondansetron (Zofran) may decrease alcohol intake in patients with alcohol use disorder. | B |
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to https://www.aafp.org/afpsort.
*—Approved by the U.S. Food and Drug Administration for this indication.
Adapted with permission from Winslow BT, Onysko M, Hebert M. Medications for alcohol use disorder. Am Fam Physician. 2016;93(6):459.
Referring Patients for Specialized Alcohol Treatment
It may be helpful for family physicians to develop relationships with a physician or counselor in the community who specializes in treating unhealthy alcohol use so that patients can be referred directly, just as they would for any subspecialty care. Clinic staff can be trained to become familiar with local community resources by having them visit treatment centers and county-based programs. Some clinics have a list of local people in recovery who are available to provide peer support that may include taking the patient to a self-help meeting or to an addiction treatment facility intake appointment. Involving family members, friends, and work colleagues (with patient permission) in the referral process is also helpful. The Substance Abuse and Mental Health Services Administration and Health Resources and Services Administration Center for Integrated Health Solutions have many useful tools to assist primary care practices in developing referral systems (https://www.integration.samhsa.gov/clinical-practice/sbirt/referral-to-treatment).9 Physicians should reassure patients that a referral to an alcohol treatment center is no different from a referral to a cardiologist or pain subspecialist—the overall goal is to improve health, well-being, and quality of life.
Editor's Note: Dr. Salisbury-Afshar is a contributing editor for AFP.

