Am Fam Physician. 2019;99(12):773-774
Author disclosure: No relevant financial affiliations.
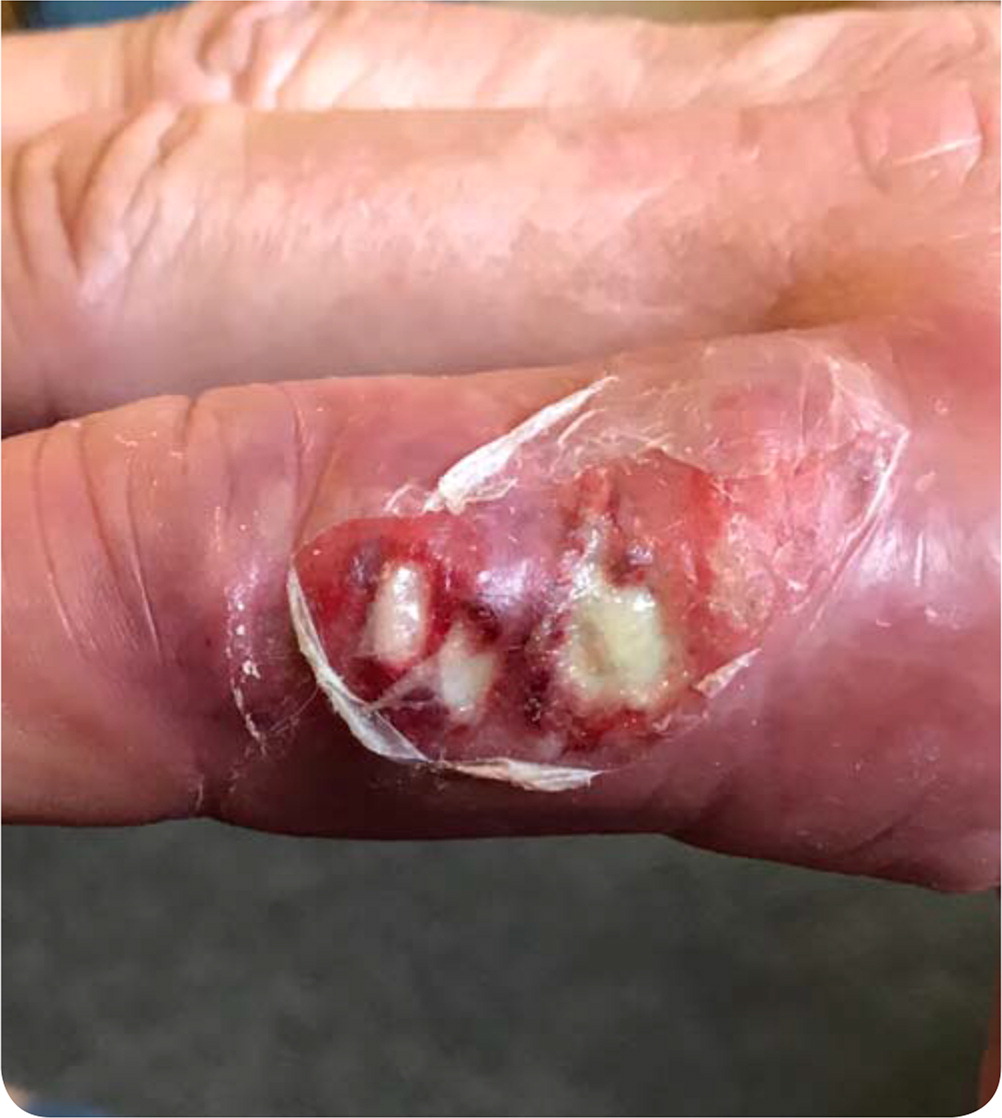
A 55-year-old man presented with an erythematous, swollen, painful lesion on his finger that had developed several weeks earlier. He otherwise felt well and had not been ill. His medical history was notable for treated hepatitis C with compensated cirrhosis. He wore gloves while working as a butcher and had no recent trauma to the hand.
Physical examination revealed swelling and erythema of the right index finger, with a central cluster of ulcerated lesions (Figure 1). Plain radiography showed soft tissue swelling of the finger with no bony abnormalities. The lesion did not resolve with seven days of trimethoprim/sulfamethoxazole followed by seven days of doxycycline.
Question
Discussion
The answer is B: erysipeloid. This skin lesion is the most common manifestation of infection with Erysipelothrix rhusiopathiae, a gram-positive bacterium found in a wide variety of domestic and wild animals. Humans are typically exposed to the organism through their occupation, with butchers at particular risk. Infection has also been reported with activities such as fishing and crabbing and following incidental contact with animals or animal products.1,2 The organism enters the skin via abrasions, scratches, or puncture wounds, commonly on the hands.
E. rhusiopathiae causes three forms of illness: localized cellulitis (most common); advancing skin infection; and systemic infection with bacteremia, which may be complicated by endocarditis.2 This patient had a focal cellulitis.
A painful, erythematous patch develops two to seven days after infection with E. rhusiopathiae. The pain is described as burning, itching, or throbbing.2 The lesion has a purplish discoloration, sometimes with central clearing and formation of vesicles. Systemic signs of illness, such as fever, are uncommon. The lesion resolves without treatment in three to four weeks, or earlier with antibiotics. Erysipelothrix is resistant to vancomycin and sulfa drugs, and tetracycline is not consistently effective. Penicillin and other beta-lactam antibiotics are the drugs of choice.2
Erysipelas is a superficial infection of the skin leading to clearly demarcated, bright red, swollen lesions that are tender to palpation.3 Group A streptococci infection is the most common etiology. Erysipelas often affects the face or lower extremities, and patients may be febrile.
Herpetic whitlow is due to a primary infection with or reactivation of the herpes simplex virus. Following the development of redness and swelling, vesiculoulcerative lesions appear on the fingers.4 Herpetic whitlow is an occupational hazard for dentists and health care professionals. The lesions resolve in two weeks but may recur.
Impetigo is an acute superficial infection of the skin due to Staphylococcus aureus or Streptococcus pyogenes, manifesting as vesicles or pustules that crust or become bullous. The lesions are often found on the face of children, around the nose and mouth.5 Bullous impetigo, caused by S. aureus, may produce systemic signs of illness.
| Condition | Characteristics |
|---|---|
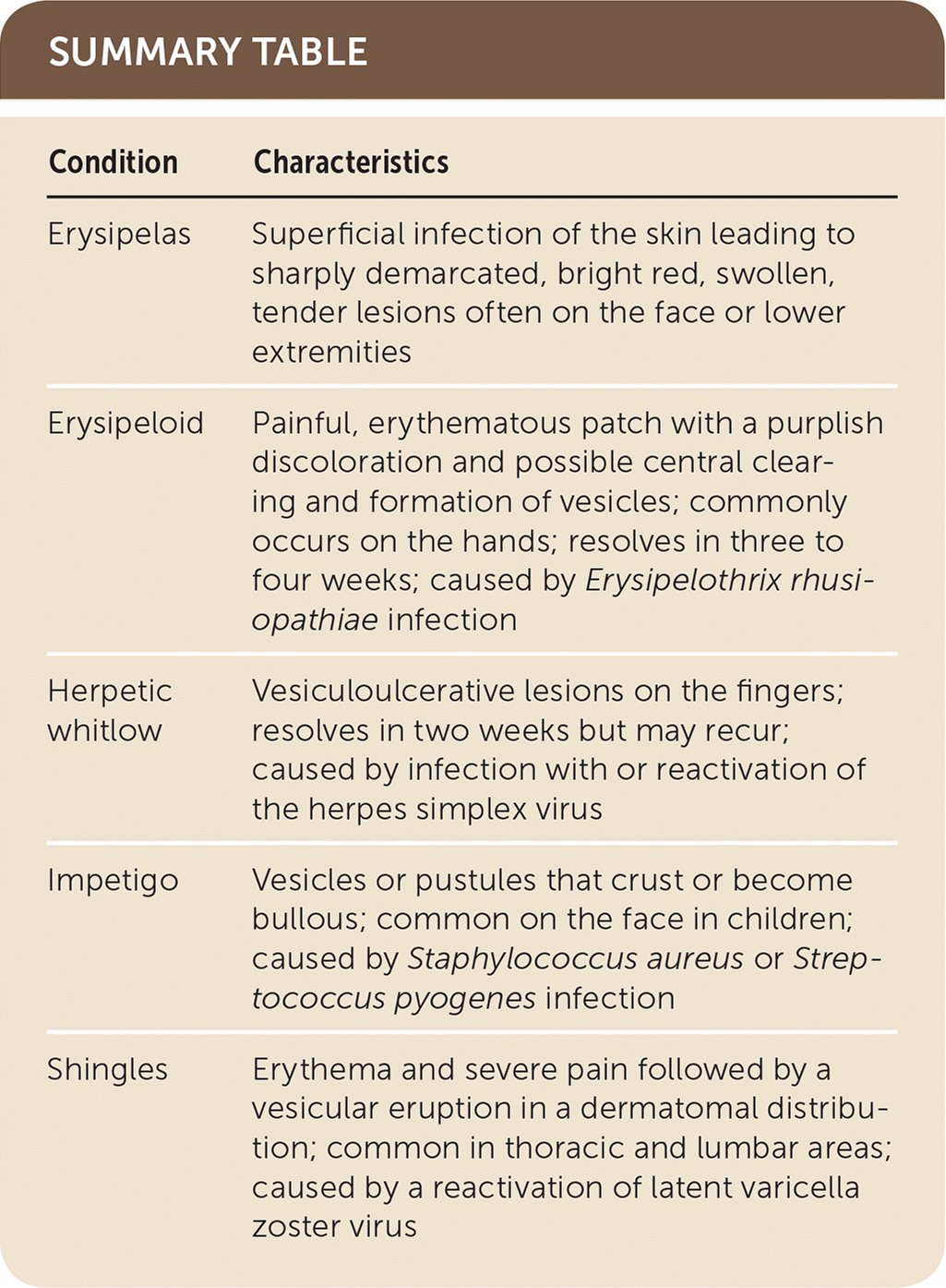
| Erysipelas | Superficial infection of the skin leading to sharply demarcated, bright red, swollen, tender lesions often on the face or lower extremities |
| Erysipeloid | Painful, erythematous patch with a purplish discoloration and possible central clearing and formation of vesicles; commonly occurs on the hands; resolves in three to four weeks; caused by Erysipelothrix rhusiopathiae infection |
| Herpetic whitlow | Vesiculoulcerative lesions on the fingers; resolves in two weeks but may recur; caused by infection with or reactivation of the herpes simplex virus |
| Impetigo | Vesicles or pustules that crust or become bullous; common on the face in children; caused by Staphylococcus aureus or Streptococcus pyogenes infection |
| Shingles | Erythema and severe pain followed by a vesicular eruption in a dermatomal distribution; common in thoracic and lumbar areas; caused by a reactivation of latent varicella zoster virus |