| Lead level (μg per dL [μmol per L]) | Evaluation | Education | Intervention | Follow-up |
|---|---|---|---|---|
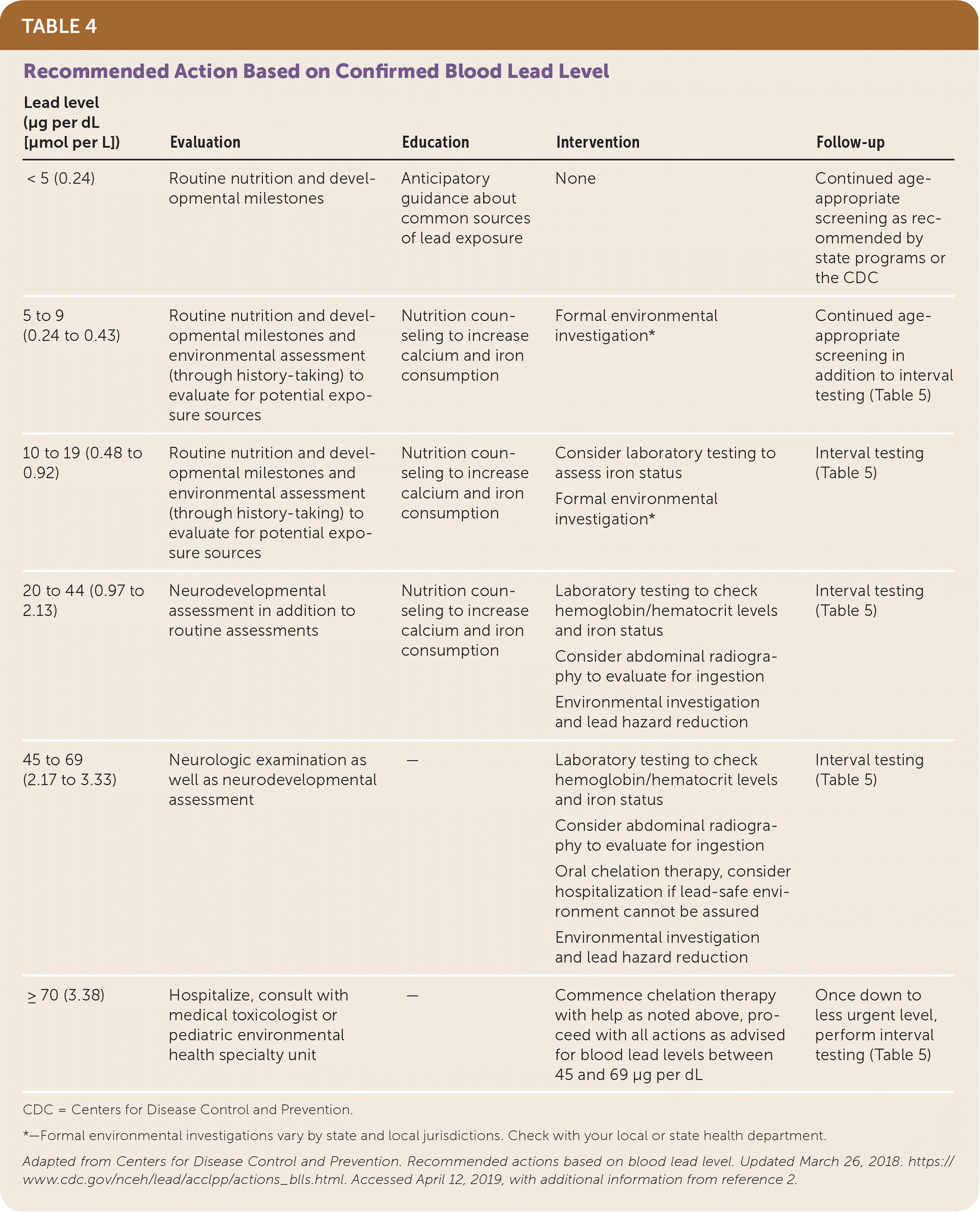
| < 5 (0.24) | Routine nutrition and developmental milestones | Anticipatory guidance about common sources of lead exposure | None | Continued age-appropriate screening as recommended by state programs or the CDC |
| 5 to 9 (0.24 to 0.43) | Routine nutrition and developmental milestones and environmental assessment (through history-taking) to evaluate for potential exposure sources | Nutrition counseling to increase calcium and iron consumption | Formal environmental investigation* | Continued age-appropriate screening in addition to interval testing (Table 5) |
| 10 to 19 (0.48 to 0.92) | Routine nutrition and developmental milestones and environmental assessment (through history-taking) to evaluate for potential exposure sources | Nutrition counseling to increase calcium and iron consumption | Consider laboratory testing to assess iron status Formal environmental investigation* | Interval testing (Table 5) |
| 20 to 44 (0.97 to 2.13) | Neurodevelopmental assessment in addition to routine assessments | Nutrition counseling to increase calcium and iron consumption | Laboratory testing to check hemoglobin/hematocrit levels and iron status Consider abdominal radiography to evaluate for ingestion Environmental investigation and lead hazard reduction | Interval testing (Table 5) |
| 45 to 69 (2.17 to 3.33) | Neurologic examination as well as neurodevelopmental assessment | — | Laboratory testing to check hemoglobin/hematocrit levels and iron status Consider abdominal radiography to evaluate for ingestion Oral chelation therapy, consider hospitalization if lead-safe environment cannot be assured Environmental investigation and lead hazard reduction | Interval testing (Table 5) |
| ≥ 70 (3.38) | Hospitalize, consult with medical toxicologist or pediatric environmental health specialty unit | — | Commence chelation therapy with help as noted above, proceed with all actions as advised for blood lead levels between 45 and 69 μg per dL | Once down to less urgent level, perform interval testing (Table 5) |