Original Article: Care of Incarcerated Patients
Issue Date: November 15, 2018
See additional reader comments at: https://www.aafp.org/afp/2018/1115/p577.html
To the Editor: Dr. Davis and colleagues are to be commended for compiling this comprehensive set of best practices for caring for incarcerated people. As the primary provider of gender-affirming telemedicine to transgender people incarcerated in California's 35 prisons, I find it immensely challenging to partner with on-site health care teams in this area.
Transgender people have a significantly higher lifetime rate of incarceration compared with the general population,1 and nearly 40% of incarcerated transgender people have reported sexual victimization.2 Rape and sexual violence are more likely to occur when incarcerated people are housed according to their sex assigned at birth, thereby placing transgender women in men's facilities.
The National Commission on Correctional Health Care notes that medical screening should include inquiries about an individual's sexual activity, sexual orientation, and gender identity.3 However, screening for these factors creates the illusion that transgender women, particularly, will engage in only consensual sex. Incarcerated people lack access to condoms (legal in only three state prison systems and rarely in local facilities despite World Health Organization recommendations) or medications for HIV preexposure prophylaxis (currently not available in any state).4 Because sex is nearly universally illegal while incarcerated, attempts to obtain limited available protection can lead to self-incrimination.
Most states do not require testing for sexually transmitted infections (STIs) at intake or during incarceration. Therefore, family physicians are well positioned to provide stigma-free preventive care for incarcerated transgender people, in part by adopting a universal approach that considers increased STI transmission risk in an environment with frequent sexual assault and criminalized consensual sex behaviors.
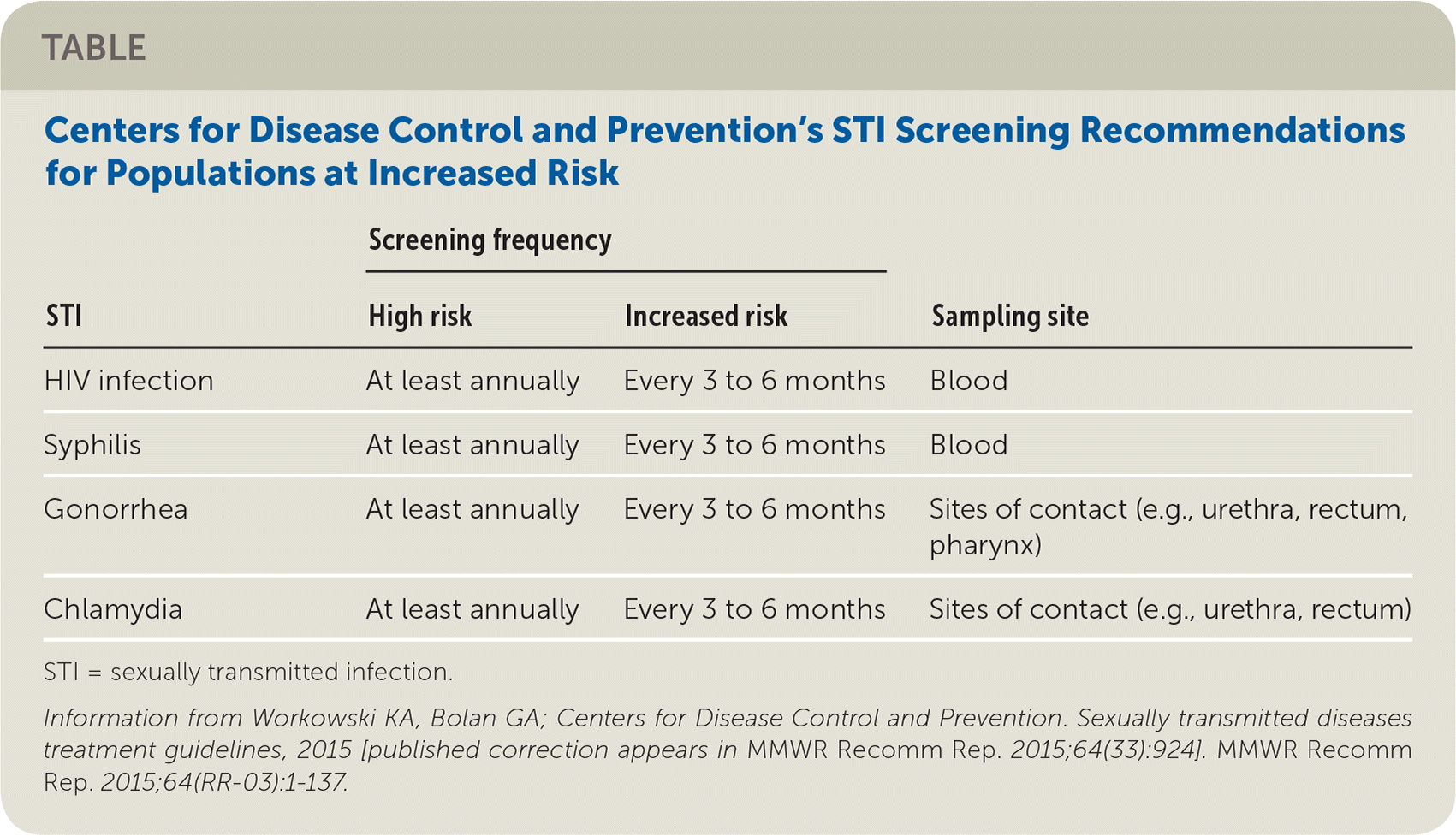
Routine approaches to screening based on the Centers for Disease Control and Prevention's recommendations for STI screening in high-risk populations are inadequate,5 leading to too-infrequent screening and often limiting testing to only the urethra. The accompanying table includes the schedule that should be used for STI screening in transgender women, whose risk is at least as high as that for men who have sex with men.5 Appropriately screening for and treating STIs is an essential public health issue that will improve care for incarcerated transgender people and their partners.
TABLE Centers for Disease Control and Prevention's STI Screening Recommendations for Populations at Increased Risk
| STI | Screening frequency | Sampling site | |
|---|---|---|---|
| High risk | Increased risk | ||
| HIV infection | At least annually | Every 3 to 6 months | Blood |
| Syphilis | At least annually | Every 3 to 6 months | Blood |
| Gonorrhea | At least annually | Every 3 to 6 months | Sites of contact (e.g., urethra, rectum, pharynx) |
| Chlamydia | At least annually | Every 3 to 6 months | Sites of contact (e.g., urethra, rectum) |
STI = sexually transmitted infection.
Information from Workowski KA, Bolan GA; Centers for Disease Control and Prevention. Sexually transmitted diseases treatment guidelines, 2015 [published correction appears in MMWR Recomm Rep. 2015;64(33):924]. MMWR Recomm Rep. 2015;64(RR-03):1–137.
In Reply: We appreciate Dr. Nass for highlighting some of the challenges correctional care clinicians face when caring for transgender people. Although transgender people represent only a small percentage of inmates, they are disproportionately likely to be incarcerated compared with the general population, and they are more likely to be sexually victimized in correctional settings.1 We agree that intake assessments should include inquiries about gender identity, biological sex, sexual orientation, and sexual practices. This allows for selection of an appropriate sampling location for gonorrhea/chlamydia testing (e.g., urethra, rectum, pharynx). We also agree that incarcerated people should be provided access to condoms, and recognize that this is not routinely available.2,3 We encourage clinicians to discuss consensual and nonconsensual sexual activity with all incarcerated patients. Preventive care for transgender incarcerated people should include expanded STI screening based on current anatomy4,5 and may include additional laboratory monitoring if the inmate is receiving gender-affirming hormone therapy.4

